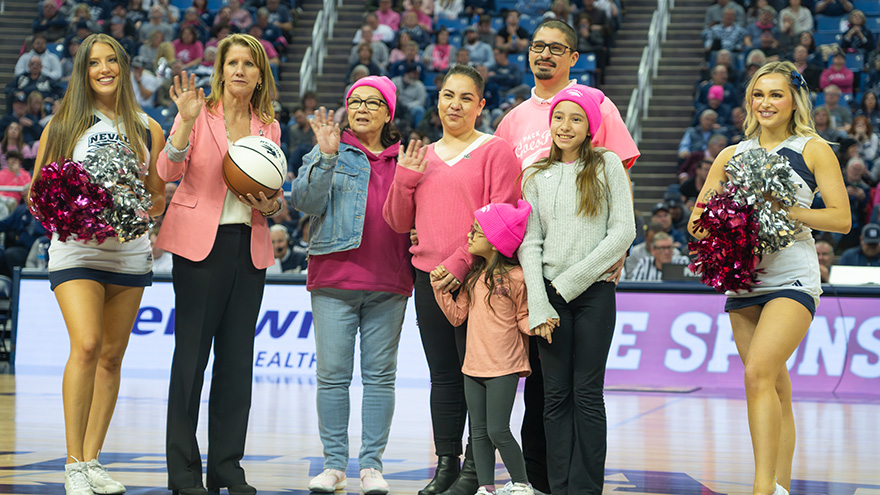Search
-
Department Spotlight: Pharmacy
When it comes to each patient’s healthcare journey, medication is often a key chapter. After all, medication is one of the most common treatment methods to help patients on the road back to health. In 2023, 4.83 billion prescriptions were filled in the U.S., and with this number only anticipated to rise annually, having an expert pharmacy team on your side to make certain you are prescribed the ideal dosage to treat your condition, prepare your prescriptions on time and help you manage your medications responsibly is important. Fortunately, at Renown Health, we have best-in-class inpatient and outpatient pharmacy teams to fill both prescriptions and promises for excellent care. Renown Pharmacy plays a vital role in helping us foster a health system that prioritizes patient well-being above all else. This department exemplifies the impact that a unified, expert pharmacy team can have on patient outcomes now and in the future. The Masters of Medication Spanning three hospitals plus ambulatory locations across the health system, Renown’s growing pharmacy team – full of dedicated pharmacists, pharmacy technicians and even medical assistants – manages medications in a wide variety of patient settings, touching nearly every aspect of the healthcare continuum: Outpatient Retail Pharmacies Renown Regional Medical Center – 75 Pringle Way The Healthcare Center – 21 Locust Street Renown South Meadows Medical Center – 10101 Double R Blvd Inpatient Pharmacies Renown Rehabilitation Hospital Renown Regional Medical Center (including Renown Children’s Hospital) Renown South Meadows Medical Center COMING SOON: Conrad Breast Center Pharmacy (in honor of Kristina Ferrari) in the Specialty Care Center at Renown South Meadows Ambulatory Pharmacies Anticoagulation Services – Institute for Heart & Vascular Health (IHVH) Pharmacotherapy Program – IHVH and Renown Medical Group Locations Congestive Heart Failure Pharmacotherapy Program – Center for Advanced Medicine B at Renown Regional Chronic Obstructive Pulmonary Disease (COPD) Pharmacotherapy Program – Renown South Meadows Endocrinology Pharmacotherapy Program – Renown South Meadows Clinical pharmacists at Renown bridge the gap between medicine and compassionate support, making sure each patient receives personalized care one prescription at a time. “There are various roles pharmacists play within Renown,” said Clarissa Munoz, Clinical Pharmacist in the Renown Regional Inpatient Pharmacy. “Staff pharmacists work diligently to ensure correct medications are dispensed, and if compounded, make sure they were prepared properly. They also work hard to answer medication messages and phone calls, help verify orders and make sure ode trays/RSI kits are appropriately stocked and ready when needed. Clinical pharmacists work from satellite pharmacies on the floor and focus on reviewing patient charts and aim to provide additional interventions to the providers to optimize treatment strategies. We also serve as a resource for nursing staff and help answer medication questions.” “My role in the pharmacy is pretty expansive,” added Chanelle Ajimura, Clinical Pharmacist in the Renown Regional Outpatient Pharmacy. “I maintain inventory to confirm patients can receive their medications in a timely manner both for our discharge and retail patients while balancing the Meds to Beds program, which offers medication delivery to the bedside and bedside medication counseling; collaborating with an interdisciplinary team to find the most affordable price for patients; and verifying that the dose, strength, indication, etc. is appropriate for the patient from start to finish.” “In the pharmacy, I make sure patients are receiving appropriate drug therapy by checking for major drug interactions and ensuring appropriate dosing,” added Courtney Church, Clinical Pharmacist in the Renown Regional Outpatient Pharmacy. “I also make recommendations to providers so patients can get cost-effective therapy.” Our pharmacy technicians work behind-the-scenes ensuring efficient medication management, making a difference in the lives of patients every day. “A pharmacy technician is responsible for making sure the patient gets their medications on time and at the lowest price possible,” said Nate Graham, Pharmacy Technician in the Renown Regional Outpatient Pharmacy. “This is done by working with patients, insurance companies and case workers. We fill prescriptions, enter prescriptions into our system, receive and send orders for medications and maintain a clean pharmacy with an accurate inventory.” “We do a variety of things; the task people probably know the most is counting out the medications and putting them in the amber vials,” added Rachel Vallin, Pharmacy Technician in the Renown Regional Outpatient Pharmacy. “We also help patients at the front of the pharmacy, ring out their prescriptions, answer some basic questions (deferring to a pharmacist as necessary) and billing insurance. Meds to Beds is my favorite part because I feel the most involved. I take medications to patients who are discharging up to their hospital rooms so they have it with them when they leave.” “As a technician, I confirm that all medications of new admissions are available in our machines prior to admitting and then maintain stock during each patient’s stay,” added Tammara Axtman, Pharmacy Technician at Renown Rehabilitation Hospital. "I also assist our nurses when needed in regard to any of their questions with both EPIC and Omnicell.” Our pharmacy team is also on the move all across our health system, thanks to our Ambulatory Pharmacy programs. For patients experiencing a serious heart, lung, or endocrine condition that requires ongoing drug therapy maintenance and guidance, our ambulatory pharmacies step in to carefully monitor how their medications impact their health and well-being. “Our role as pharmacists in this department is non-traditional because we actually see patients in the exam rooms face-to-face,” said Cory Lankford, Ambulatory Care Clinical Pharmacist for Renown’s Anticoagulation Services. “We modify their medication regimens and drug recommendations under collaborative practice agreements.” “Because our role is so unique, we have a lot of opportunities to make a positive impact on patients,” added Janeen Abe, Ambulatory Care Clinical Pharmacist for Renown’s Anticoagulation Services. “We do a lot of direct patient interaction, including counseling patients on their medications and helping them navigate through their disease state.” “As a medical assistant in this department, we’re called the patient ‘liaisons’ to orchestrate who they should go to whether it’s a nurse, a provider or a pharmacist,” added Kiara Scruggs, Medical Assistant for Renown’s Anticoagulation Services. “We look at each patient’s medications and help with the Warfarin blood thinner monitor. We get to do a lot with patients." No matter the diagnosis, having Renown Pharmacy as an integral part of your healthcare team is a win-win situation for both you and them: you receive access to medication to help you heal, delivered to you with precision and care, and the pharmacy team has the opportunity to care for you and make a positive impact, a role they take seriously.
-
Dr. Carilyn Hoffman's Guide to Menopause Medication & Relief
Women undergo multiple hormonal changes throughout their lives, leading to different physical and emotional experiences. Dr. Carilyn Hoffman, at Renown Women's Health, explains these confusing life stages and helps decode menopause. Perimenopause: Transitioning Towards Menopause Defined as the time "around menopause," perimenopausal symptoms are caused by hormonal fluctuations that occur as the ovarian function declines. Levels of estrogen and progesterone decrease, and follicle stimulating hormone increases. These hormonal fluctuations may cause a range of symptoms including: Irregular or abnormal periods: Initially cycles intervals vary in length by greater than 7 days, then in later stages the interval increases to greater than 60 days between cycles Hot flashes and night sweats: This is the most common symptom and 50-82% of women will have vasomotor symptoms Mood swings and memory problems Anxiety or insomnia Heart palpitations Decreased libido and vaginal dryness Weight gain and thinning hair Increased risk of urinary tract infections Decreased bone density Menopause Menopause is defined as year without a menstrual cycle and marks the timeframe when the ovaries stop making estrogen. This signifies the end of the reproductive years. The average age of menopause is 51; however, the menopausal transition can last about 8 years. This means that women in their late 30’s and 40’s may start to have symptoms of perimenopause. The worst vasomotor symptoms are typically experienced at the one-year mark since the last period. Unfortunately, some women experience symptoms throughout the entire menopausal transition. Postmenopausal After 12 months without a menstrual cycle, a woman is confirmed to be postmenopausal. This is sometimes difficult to define, as women may have had procedures that cause menstrual suppression such as a uterine ablation or hysterectomy or they may still be on contraception. Sometimes, lab work may be recommended to help determine menopausal status. However, due to the broad time period that the menopausal transition occurs and the variations in normal hormone levels throughout a cycle, lab work is not always helpful. Dr. Hoffman explains the importance of thorough counseling for patients seeking to "check their hormone levels." She emphasizes that menopause is diagnosed clinically, focusing more on the individual's symptoms rather than lab values. This approach ensures that patients understand the implications of the test results and the treatment strategy. Menopause Medical Management Medical management of symptoms should be tailored to the individual’s concerns. Abnormal Bleeding: There are a range of medications, IUDs and procedures available if the main concern is irregular or prolonged menstrual bleeding during perimenopause. Hot Flashes and Night Sweats: Hormone Replacement Therapy (HRT): HRT is currently the most effective method for relieving vasomotor symptoms. However, it's important to discuss potential risks with a healthcare provider, as HRT can increase your risk of blood clots and breast cancer. If improperly prescribed, it can also increase the risk of uterine cancer. The American College of Obstetricians and Gynecologists recommends the lowest dose for the shortest duration. Low-dose antidepressants: SSRIs/SSNIs may mitigate hot flashes and mood disorders for those who are not candidates or prefer to avoid HRT. Currently, only Paroxetine is FDA-approved for this use. Fezolinetant: This is a newly FDA-approved non-hormonal medication that works at the brain's level to treat vasomotor symptoms. Gabapentin: This is an anticonvulsant medication that has been shown in several studies to be helpful for vasomotor symptoms, but it is not currently FDA-approved. Genitourinary Symptoms of Menopause: Vaginal estrogen: Vaginal dryness and pain with intercourse due to thinning vaginal tissue is a common symptom of menopause. Vaginal estrogen is highly effective at decreasing these symptoms and has fewer side effects than systemic HRT. Ospemifene: This is a selective estrogen receptor modulator that is a non-hormonal FDA-approved medication for severe vaginal dryness. Natural Symptom Relief Strategies: Nutrition: Incorporate calcium, vitamin D, and high-quality protein to support bone health and muscle maintenance. There are limited studies on phytoestrogens (found in soy and tofu) and vasomotor symptoms. While the data doesn’t necessarily support that these phytoestrogens relieve symptoms, no detrimental effects were found and these tend to be high quality and healthy proteins. Exercise: Regular physical activity can ease menopausal symptoms and support weight management. Data doesn’t support that this reduces vasomotor symptoms, but it can be helpful in weight management and sleep quality. Beverage choices: Limiting alcohol and caffeine can help decrease the frequency of vasomotor symptoms and may also improve sleep quality. Alternative remedies: One study shows that Chinese herbal medicine and acupuncture are effective at relieving vasomotor symptoms. There is not enough evidence to recommend Black Cohosh, and it is associated with liver toxicity in high doses. Studies don’t show that St. John’s Wart or Gingko Balboa are any better than placebo. Always mention your alternative medical therapies to your provider as some do interact with other prescribed medications. By understanding and recognizing that the symptoms of menopause are real and treatable, women are empowered to manage this transition better and can maintain their well-being and quality of life. Please schedule an appointment with Renown Women’s Health if you’d like to discuss your menopause symptoms with a provider.
Read More About Dr. Carilyn Hoffman's Guide to Menopause Medication & Relief
-
Healthy Potato Salad A Creamy Dreamy and Light Picnic Favorite
Potato salad is the superstar of summer picnics, a delightful sidekick at backyard BBQs, and a tasty everyday treat! Our friends at Renown's Health Improvement Programs whipped up a fabulous, health-conscious version that doesn't skimp on the creamy dreaminess we crave. This salad features purple potatoes for a dash of delightful color. It's also easy to make, with protein-rich Greek yogurt and egg whites. This simple but classic dish will indeed become your circle's new favorite—talk about a tasty transformation!
Read More About Healthy Potato Salad A Creamy Dreamy and Light Picnic Favorite
-
Pediatric Sepsis: Causes, Symptoms and Treatment
Sepsis happens when a person's body reacts too strongly to an infection. Usually, our bodies fight infections with help from our immune system. But with sepsis, the body fights too hard, and that can be dangerous. Dr. Julianne Wilke, Pediatrics and Critical Care Medicine, examines pediatric sepsis's causes, symptoms and treatments and provides tips on preventing this potentially fatal condition. Most Common Causes Pediatric sepsis is a particularly concerning form of sepsis that can occur in children and infants. Therefore, it is vital for parents and caregivers to be aware of the indications of pediatric sepsis and to understand the causes. Bacterial infections are the most common cause of pediatric sepsis, accounting for over 80% of cases. Common Bacterial Causes: Staphylococcus infections (including Methicillin Resistant Staphylococcus Aureas - MRSA) Streptococcal infections (including those causing pneumonia and group B strep) Escherichia coli, or more commonly; E. coli Klebsiella and Pseudomonas infections Viral Infection Causes: Respiratory syncytial virus (RSV) Influenza Parainfluenza Adenovirus Human metapneumovirus Coronaviruses (including COVID-19) Other Causes: Fungal infections (but are relatively rare) Parasites, such as Giardia lamblia Pediatric Sepsis Symptoms Parents and caregivers need to be observant of sepsis symptoms in children and can include: Fever Extremely fast heart rate Rapid breathing Lethargy Pale or discolored skin Low blood pressure Confusion Slurred speech Abdominal pain Diarrhea & Vomiting Decreased urination Difficulty breathing Use the acronym SEPSIS: S – Slurred speech and confusion E – Extreme shivering or muscle pain/fever P – Passing no urine all day S – Severe breathlessness I – “I feel like I might die.” S – Skin mottled or discolored If any of these symptoms are present, seeking immediate medical attention is imperative.
Read More About Pediatric Sepsis: Causes, Symptoms and Treatment
-
Are You Using the Right Sunscreen?
Seeking protection for yourself and your loved ones from the intense sun rays at northern Nevada's elevated altitudes? With so many choices available, selecting the ideal sunscreen can be daunting. To guide you through this, we consulted Dr. Angela Walker, a dermatologist from Renown Medical Group, for her expert insights. Sunscreen Application Dermatologists recommend a broad-spectrum sunscreen with a minimum SPF of 30, but keep in mind that no sunscreen protects against 100 percent of UV radiation and that reapplication is necessary. “No matter the SPF, sunscreen must be applied adequately and frequently, meaning a quarter-sized amount to cover the face and neck and a full shot glass amount for the body when wearing a bathing suit,” said Walker. “Reapplication should be every 80 minutes.” Why not use a high SPF, such as 70 or 100? According to the Skin Cancer Foundation, they don’t offer significantly more protection than SPF 30 and mislead people into thinking they have a higher level of protection. Here’s the breakdown: SPF 15 blocks 93 percent of UVB rays SPF 30 blocks 97 percent of UVB rays SPF 50 blocks 98 percent of UVB rays SPF 100 blocks 99 percent of UVB rays Do specific populations require a higher SPF? Walker explains that infants, seniors, and those with a history of skin cancer must take precautions against UV radiation, as their skin is vulnerable. Sunscreen should be an absolute priority before spending time outdoors and avoiding prolonged sun exposure, wearing a hat with wide brim (recommended 4-inch brim) and UPF (ultraviolet protection factor) clothing. Due to the sensitive nature of an infant’s skin, babies under six months should not spend time in the direct sun. For infants and toddlers six months and older, whose skin is thinner than adults, a sunscreen that contains zinc oxide or titanium dioxide (physical protectors) should be applied. Zinc and titanium are less likely to irritate because they do not penetrate the skin and instead sit on the surface and deflect UV radiation. Zinc oxide and titanium dioxide are vital ingredients to seek out in sunscreen due to their strong ability to deflect UV radiation. Sunscreen Terms Explained UVA = Long wave ultraviolet light. Penetrates deep into the dermis, the skin’s thickest layer, causing tissue damage that wrinkles and photo-aging and contributes to developing skin cancer. UVB = Short wave ultraviolet light. The biggest contributor to the development of skin cancer and are more prevalent during mid-day. SPF = Sun protection factor. Calculated by comparing the amount of time needed to burn sunscreen-protected skin vs. unprotected skin. So, SPF 15 means you can stay in the sun 15 times longer than you could without protection.
-
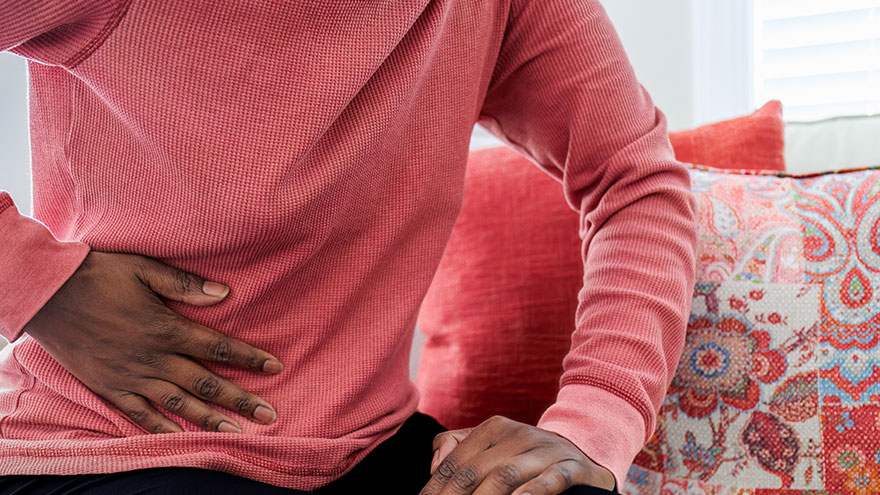
Know when to visit an ER: Top 5 concerns
When a sudden illness or injury occurs, the emergency room (ER) provides immediate medical attention to those in need. Understanding the top reasons for visiting the ER can help people make informed decisions about seeking emergency care. Here are the five most common reasons people in Nevada visited an ER in 2023. 1. Abdominal pain One of the top reasons people visit the ER is abdominal pain. The abdomen has many organs, including the stomach, liver, small and large intestines, gallbladder and pancreas. Significant pain in this area can be a cause of concern. Warning signs of a serious problem include abdominal pain with fever, vomiting, and not being able to move or perform everyday tasks due to pain. Seeking medical attention when experiencing these symptoms is essential. Emergency physicians can perform abdominal exams, assess the condition and rule out significant threats. 2. Fever High fevers that do not get better with medicine and are accompanied by other symptoms can cause concern. This can indicate that the body is fighting off an infection or illness. Fever with symptoms like vomiting, pain, altered mental status, shortness of breath or inability to perform daily functions are warning signs to watch out for. Adults and children should visit an ER, where the team can assess the causes of the fever. 3. Chest pain and shortness of breath Chest pain and discomfort, or pain in the upper body can suggest warning signs of a heart attack. If a person is experiencing signs of a heart attack, call 911 immediately to ensure timely treatment or assessment by a medical professional. Heart attack symptoms include: Chest pain, including pain that can be described as chest pressure, heaviness or squeezing Discomfort in the chest, arms, back, neck, shoulders and jaw Difficulty breathing Sweating with any of the above symptoms When visiting a Renown ER for chest pain, a trained medical professional will promptly perform an Electrocardiogram (EKG) in an area where preliminary assessments, also known as triage, take place. Individuals experiencing shortness of breath or trouble breathing, whether from a respiratory infection, asthma complications or other pre-existing conditions should not ignore symptoms as these can signify more serious issues. Warning signs of respiratory distress may include: A significant change in breathing rate A significant change in the amount of energy used to inhale or exhale when breathing Changing of the skin color to blue, gray or paleness, which can indicate a lack of oxygen Nasal flaring Chest retractions, which can suggest difficulty bringing air into the lungs What this looks like: the chest sinking in just below the neck, breastbone or rib cage while breathing 4. Neurological symptoms Sudden and severe headaches or seizures may prompt individuals to visit the ER if symptoms are extremely disorientating or debilitating. These symptoms could be indicative of various conditions, including strokes or neurological disorders that require prompt evaluation. If a person is experiencing signs of stroke, call 911 immediately to ensure timely treatment. Stroke symptoms include: Numbness, weakness or loss of movement in the face, leg or arm, especially on one side Confusion, including trouble speaking or understanding Trouble with vision or loss of balance When choosing emergency care for signs and symptoms of stroke, a Comprehensive Stroke Center can provide patients with immediate intervention, including evaluation, treatment and education. 5. Cough/flu-like symptoms Emergency departments are staffed by medical professionals trained to prioritize and treat emergency and trauma situations. Receiving care at an ER should be reserved for severe symptoms and life-threatening conditions. It’s best to schedule a visit with a primary care physician for mild cold and flu symptoms. Most urgent care locations are equipped with rapid testing options, including RSV, COVID-19, influenza, mononucleosis, urinary issues and strep throat. It is critical to distinguish between common respiratory infections and more severe cases, such as pneumonia or complications from the flu. Symptoms that may warrant a visit to the ER include: Rapid decline in the ability to perform regular daily activities Coughing or throwing up blood Severe dehydration and inability to drink fluids High fever not responsive to medication Understanding top ER visits in Nevada While these ER complaints are common reasons for emergency room visits in Nevada, it's important to remember that emergency care is available for all immediate medical needs. Do not hesitate to seek help at an emergency room if someone experiences a sudden or severe health concern. Quick and appropriate action can make a significant difference in keeping you and your loved ones healthy. Renown Health is the largest locally governed, not-for-profit healthcare network in northern Nevada, providing leading emergency and trauma care by board-certified emergency physicians 24/7 at three locations, including the region’s only pediatric emergency department. Renown Health emergency rooms prioritize swift assessments, advanced diagnostic tools and compassionate care, providing leading emergency and trauma care. Trust Renown ER for not just emergency care but exceptional care. Learn more at renown.org/ER.
-
What is an Ovarian Cyst, and How is it Treated?
Abdominal pain is one of the most common reasons for an Emergency Room visit. The abdomen is an area that encompasses multiple organs and functions. So how would you know when the pain you are feeling is an ovarian cyst or something else, and when should you seek medical attention? Dr. Carilyn Hoffman, at Renown Women's Health, explains. Ovarian Function Defined Located on each side of the uterus, the ovaries are part of the female reproductive organs and produce eggs (ova), released during the menstrual cycle, allowing for fertilization and pregnancy. They also produce hormones such as estrogen and progesterone, which play an important role in female traits, bone health, cardiovascular health and pregnancy. Symptoms of an Ovarian Cyst Cysts are solid or fluid-filled masses. Ovarian cysts can be in the ovary or on its surface. When cysts are enlarged or rupture, they can create a dull ache or sharp pain below the belly button. Besides discomfort and pain, other symptoms of ovarian cysts may include bloating, fullness, pressure or heaviness. "Ovarian cysts are common; most are physiologic and will go away on their own. They are frequently found incidentally on ultrasound and are present in the middle of the menstrual cycle," says Dr. Hoffman. "However, if a woman experiences sudden and severe pelvic pain they should seek immediate medical attention. Sometimes ovarian cysts can become large and twist on themselves. This is called ovarian torsion and is a surgical emergency. Other times, cysts can rupture and bleed. This is called a hemorrhagic cyst and can also be a surgical emergency." Diagnosis and Treatment If an ovarian cyst is suspected, your doctor will perform a pelvic exam and order an ultrasound. There are certain ultrasound findings that suggest that the cyst is benign. There are other ultrasound findings that are concerning for cancer. Small simple cysts often resolve on their own, whereas solid or very large cysts may require surgery.
Read More About What is an Ovarian Cyst, and How is it Treated?
-
Department Spotlight: Radiation Oncology
Up to half of all men and one-third of all women will face a cancer diagnosis in their lifetime, according to the Nevada Cancer Coalition. Chances are, you or someone you care about has been affected by cancer and has witnessed the ultimate fight for life. More than likely, your loved one’s cancer journey involved radiation therapy – and in fact, more than half of cancer diagnoses are treated in whole or in part with radiation. At first glance, this treatment plan can sound scary to any person. With a cancer care journey, it takes a village, and at Renown Health, we have top-notch leaders of the village roads that lead to radiation. Meet our Radiation Oncology team at the William N. Pennington Cancer Institute. From intake to inpatient, this department of passionate physicians, radiation therapists, registered nurses, medical assistants, intake coordinators, schedulers and more are here to help every patient dealing with the intimidating diagnosis of cancer. Any patient that needs radiation as a part of their treatment is in the best of hands with this team, who will stop at nothing to ensure each patient under their care knows that they have a village Fighting the Good Fight right alongside them. Teamwork in Tackling Tumors One of the most common forms of cancer treatment, radiation therapy uses high-energy X-rays to minimize cancerous cells. But with Renown’s Radiation Oncology department, the impressive cancer care doesn’t stop there – this team leverages advanced technology right at their fingertips. In fact, our cancer institute has the most state-of-the-art radiation therapy system of its kind – the ultra-precise Varian TrueBeam radiation therapy system – and is the very first program holding American College of Radiology accreditation in the entire region. Given the advanced nature of their jobs and the high standard of care their patients expect them to uphold, it’s no question that the days-in-the-life of each team member is complex and can continually change every day. “There are many moving parts in radiation oncology on any given day,” said Sandra Bailey, Manager of Radiation Oncology Services. “The radiation oncologists consult newly diagnosed patients, follow up with previously treated patients and oversee daily treatments for patients actively receiving treatments. Nurses and medical assistants move around the clinic to support the physicians with patients and provide education and other supportive care.” The physics and dosimetry teams work diligently alongside the physicians to design the most beneficial treatment plan for each patient. Once a patient begins their treatments, the radiation therapists administer the daily treatments with the utmost precision. Intake coordinators, schedulers and patient access representatives make surethe patients have their insurance authorization and are processed through the system appropriately. Like any well-oiled machine, each part is necessary for the other to function at peak performance to ensure our patients receive the quality care they deserve and expect. Like many other clinical departments at Renown, teamwork coupled with education is crucial to best serve radiation therapy patients. Our nurses on this team are experts at exactly that, serving as a reminder of the transformative power of care in the face of a daunting disease. “Radiation oncology is a unique world,” said Kristen Reed, Registered Nurse. “We have many different team members that play a role in how we function as a department. We all work together in some aspect to provide care for our patients. As a nurse, I provide patient education to all my patients before starting treatment to go over potential side effects and expectations on their treatment. Daily, we see new patients and follow-ups, plan simulations to start patients for radiation treatments and provide radiation treatments, among many other daily tasks.” The unique role of our radiation therapists, the team members who are on the frontlines of giving radiation treatments, helps this department stand out from the rest with their tireless dedication to fighting against cancer with compassion and expertise. Not only are they armed with technology, but they are also armed with hands that deliver healing rays of radiation. “As a radiation therapist, our daily tasks can vary pretty widely,” said Casey Johnson, Radiation Therapist. “We rotate between three radiation treatment machines called linear accelerators – one of which we use for stereotactic radiosurgery, a minimally invasive form of surgical intervention. We also staff the CT simulation room where we construct all the patients' treatment devices and perform their ‘mapping’ scan. We then coordinate with the dosimetrists and physicians to determine the specifics of the patients’ course of treatment. The most important parts of our job are patient care and education. Even though our job is very technical and requires tremendous attention to detail, the critical part is remembering that our average workday could be a monumental day for a new patient.” “Our day-in-the-life in Radiation Oncology is centered around patient care,” added Haley Longfield, Radiation Therapist. “Although we do not spend a ton of time with our patients, we see them every day. We are able to build a wonderful rapport with our patients that is top-notch. We set up the room with their treatment devices, get them set up appropriately and administer their radiation treatment. On average, our patients are here for about 15 minutes.” The bottom line: our Radiation Oncology team’s unified commitment to both excellence and innovation promises a brighter future for those battling cancer. No one is ever alone in their fight, and this team makes sure of that, no matter what. Radiating Excellence in Cancer Care The Pennington Cancer Institute boasts a stellar reputation in our community for offering best-in-class, evidence-based care and cutting-edge research, improving outcomes for patients battling cancer. This fact is what inspired many Radiation Oncology team members to take their talents to this department in the first place. “I chose to work at the Cancer Institute because I believe we offer the best patient care experience, along with the most advanced radiation treatments in the area,” said Casey Johnson. "I am a fifth generation Reno resident, and I am part of this community through and through,” added Haley Longfield. “I always knew that I wanted to work here.” The success of our cancer institute starts with our people – and many members of the Radiation Oncology team witnessed this firsthand upon their arrival in this department. “I was initially inspired to move across the country to work in the Cancer Institute by the vision of the senior leaders and the future growth plans for the entire institute; once I arrived, I quickly realized what a great team I am now leading,” said Sandra Bailey. “The compassion and care the Radiation Oncology team provides our patients is second to none. Medical errors are rare in our department, and this can be attributed to not only the processes in place to prevent them, but everyone working together to deliver radiation treatments safely. Each day I witness a patient relationship being nurtured and developed. I am truly honored to be part of this team.” Inspired by Renown's integral role in the northern Nevada community, several team members were drawn to this department because of the opportunity to make a meaningful impact on patients' lives in a quiet healing environment. “As a student nurse, I had clinical and practicum on the cancer nursing unit here at Renown; I noticed the quiet, healing environment and a patient population enduring some of life’s most challenging hurdles,” said Rachel Bales, Registered Nurse. “It is in these moments that you can really make a difference as a nurse. After pursuing critical care as a new grad and working in Interventional Radiology with cancer patients, I knew that I had to find my way back to oncology. I applied to Radiation Oncology, and I am working towards my third year in this department. I have always known that I enjoy helping others, and the fulfillment that comes from working with this patient population is unmatched.” “Renown is a huge part of the community in northern Nevada, and I knew while I was in nursing school that I wanted to have a career here,” added Kristen Reed. “I ended up joining the Cancer Institute about two years ago. My patients are a huge part of why I stay. We really get to know these patients and their families well, especially because they come in from Monday through Friday for up to six weeks for treatments. Building connections and being able to support these patients during a difficult time in their life makes my job fulfilling.” From the initial consultation to the administration of therapy, the staff's commitment to personalized care remains strong. Patients and their families develop profound connections with these team members as they navigate through the challenges of treatment. “We have knowledgeable and caring staff that help guide our patients through treatment,” said Kristen Reed. “This starts on the day of their consultation and continues even after completion of treatment. The patients and families get to know the staff through their treatment, and having a familiar face can be reassuring to them. We also take time every week to see how they are doing physically and mentally while undergoing treatment and we give them a chance to check in with their doctor. Taking this time helps reassure patients and allows them to ask questions, and in turn, reduce some anxiety and worry.”
-
The Unmatched Health Benefits of Snowshoeing
Snowshoeing is an excellent winter workout that can help burn calories, strengthen muscles and boost cardiovascular health. Explore the top 8 snowshoeing spots and experience this ultimate workout adventure! Significant Health Benefits: Exceptional cardiovascular workout – burn up to 1,000 calories per hour! Low-impact muscle building Endurance building Balance strengthening and agility Improves your sense of well-being by connecting to nature Prepping for Your Adventure There are some crucial details to think about when it comes to snowshoeing, especially if you are a beginner. Make sure to pick the right kind of footwear to go on top of your snowshoes; a pair of comfortable waterproof boots are a great choice and remember to wear lots of layers. Several local places rent snowshoes if you aren’t sure about spending money on a pair. Check out Bobos Ski and Board Patio or our local REI Co-Op. Check out REI’s Beginner’s Guide to Snowshoeing for reference. 8 Cool Snowshoeing Spots 1. Galena Creek Park Close to Reno, this beautiful, low-altitude park offers several trails. You’ll find various creeks and streams under cover of pristine ponderosa pines. From beginner to advanced, the differing trail systems provide a challenge for everyone! Head west on State Route 431 (Mt. Rose Highway) for about seven miles until you see the park sign on the right side of the highway. 2. Tahoe Meadows – Chickadee Ridge This local favorite not only gives fantastic views of Lake Tahoe but the best part? – friendly little chickadees will eat seeds right out of your hand! Be sure to pack plenty of sunflower birdseed, as that seems to be their favorite. From the trailhead parking lot, head southeast into the open meadow. Then follow the ridgeline to your right (southwest). Continue southwest up toward the top of the ridgeline to the west, and you’ll get to Chickadee Ridge in just under two miles. 3. Spooner Lake Trail The easy 2.5-mile loop around Spooner Lake is excellent for all skill levels. This alpine lake is surrounded by aspen trees which house varied bird species, so bring your binoculars! Dogs are allowed on a leash, and all-day parking is $10. 4. Kirkwood Ski Resort You’ll need a trail pass, but this South Lake Tahoe resort has various routes from beginner to advanced, with roughly 50 miles of terrain. Nighttime snowshoe treks during the full moon are also available throughout the winter. Kirkwood is located on Highway 88, close to Carson Pass. 5. Camp Richardson Heading north, you can find this well-established and favorite local snowshoeing spot. If you’re up for an adventure, you can trek up to Fallen Leaf Lake. It’s located off Highway 89 and near Fallen Leaf Road. 6. Dry Pond Loop This moderate, 6.5-mile loop near Washoe Valley has impressive views of Carson Valley, Washoe Lake, and the Mt. Rose Wilderness. If you like the sound of rushing water, most of the trail meanders along White’s Creek. This area is dog-friendly and kid-friendly, which makes it a family favorite. 7. Royal Gorge Soda Springs is home to this resort, which is well known for its cross-country skiing trails. Enjoy extensive trails leading deep into the trees with spectacular views. Find Royal Gorge from the Soda Springs exit on West Interstate 80. 8. Ash Canyon Creek Tucked away in the Carson Valley, these trails are filled with mountain bikes in the spring and provide excellent snowshoeing trails in the winter. Find it from Interstate 580 by taking the Highway 395 Business exit to Winnie Lane.
Read More About The Unmatched Health Benefits of Snowshoeing
-
Life after Lymphedema Diagnosis: What to Expect
Managing lymphedema effectively is essential for enhancing the quality of life for individuals affected by this condition. Katherine Bunker, a Physical Therapist and Certified Lymphedema Therapist (PT, DPT, CLT) at Renown, has expertise in this area and her insights offer valuable strategies for managing lymphedema. Lymphedema is a chronic condition characterized by swelling in one or more limbs due to a blockage in the lymphatic system. This condition can result from cancer treatments, surgery, infection, or can sometimes be congenital. While it can be challenging to live with lymphedema, understanding the condition and adopting specific lifestyle changes and strategies can significantly improve the quality of life. Understanding Lymphedema Educating yourself about lymphedema is crucial. Understanding the causes, symptoms, and potential complications can provide you with the tools to manage the condition proactively. Lymphedema can lead to discomfort, decreased mobility, and in severe cases, infections such as cellulitis. Therefore, recognizing the early signs and knowing when to seek medical advice is essential. Medical Management Consulting with healthcare professionals who specialize in lymphedema is critical. A physiotherapist or occupational therapist trained in lymphedema management can tailor a treatment plan for you that can include the following: Compression Therapy - Wearing prescribed compression garments can help move the lymph fluid and reduce swelling. It’s essential to get fitted by a professional and understand how to use these garments correctly. Manual Lymphatic Drainage (MLD) a gentle massage technique that encourages the movement of lymph fluid out of the affected limb. It’s typically performed by a trained therapist but ask about self-massage techniques you can do at home.
Read More About Life after Lymphedema Diagnosis: What to Expect
-
The Expanded Role of OBGYNs in Women's Healthcare
Obstetrician-gynecologists (OBGYNs) see patients from menses (the monthly menstrual cycle that occurs as a part of the female reproductive system), pregnancy and childbirth through menopause and play a pivotal role in managing reproductive health and overall wellness. Dr. James Alexander with Renown Women's Health explains. "As experts in women's health, we are uniquely positioned to recognize subtle changes or symptoms that might indicate broader health issues. This comprehensive approach allows us to serve as a valuable first touchpoint for various health concerns." Preventive Screenings: A Proactive Approach One key aspect is an OBGYN's ability to recommend preventive screenings based on your symptoms, age, lifestyle and medical history. For instance, lipid screenings are critical for monitoring cholesterol levels, which can be a significant factor in women’s heart disease. An OBGYN keeps up with the current guidelines for routine screening as well as in women with risk factors such as high blood pressure, diabetes, or a family history of heart disease during your visit. By identifying risks and abnormal screening early, they can collaborate with you to implement lifestyle changes or treatments to reduce your risk of heart conditions. Schedule Your Screening Appointment Make an Appointment by Phone: 775-982-5000
Read More About The Expanded Role of OBGYNs in Women's Healthcare
-
Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
Raquel was 33 when she was diagnosed with breast cancer. It was April 2023, when she found a lump in her breast and was referred to the William N. Pennington Cancer Institute. After comprehensive imaging, she was diagnosed with invasive lobular carcinoma, which is a type of breast cancer that begins in the milk-producing glands of the breast. Between June 2023 and January 2024, she received a total mastectomy, chemotherapy and radiation at Renown Health. “Breast cancer is uncommon in women under 40, but any woman with a mass or lump in her breast should have an exam by a physician and imaging at any age,” said Dr. Lee Schwartzberg. In fact, according to the Centers for Disease Control and Prevention (CDC), only 9% of all new cases of breast cancer in the U.S. are found in women younger than 45. “It was a pretty scary diagnosis, but I’ve been led by great people through the process,” she said. “They were so helpful and there for me throughout the chemo and radiation.” Raquel's journey through breast cancer treatment at the William N. Pennington Cancer Institute was marked by the exceptional care provided by the Renown Health team, including nurses, nurse navigators, therapists, support teams and providers. Among the dedicated professionals, Dr. Michelle Chu and Dr. Lee Schwartzberg played pivotal roles in Raquel's diagnosis and subsequent treatment plan. Their expertise, compassion and commitment to patient care left an indelible impact on Raquel's experience. Their thorough examination and comprehensive approach ensured that Racquel received the best possible care for her invasive lobular carcinoma. In addition to the care provided at Renown, Raquel greatly benefitted from being connected with a mentor by Dr. Chu. This mentor, Kayla, had undergone a similar diagnosis and treatment plan, and at the same age Raquel. They texted and called each other throughout Raquel’s treatment, providing additional support through a challenging time. As of January 2024, Raquel is done with her treatment and continues to see her care team for follow-up appointments. “I’m through the worst and ready to rebuild my life,” Raquel said. To help celebrate this milestone, Nevada Athletics invited Raquel to receive the game ball at a Nevada Men’s Basketball game. She was joined on the basketball court for this special recognition by her husband, Raul; mother, Arlene; and two daughters, Ryleigh and Rhiannon. Racquel's journey is not only a testament to her resilience but also a tribute to the invaluable contributions of Dr. Chu and Dr. Schwartzberg in guiding her towards triumph over breast cancer.
Read More About Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment