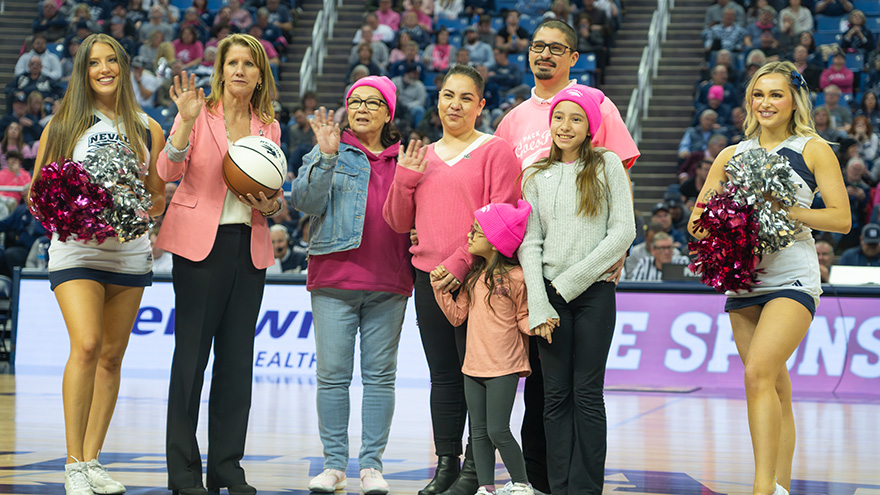Search
-
Dr. Carilyn Hoffman's Guide to Menopause Medication & Relief
Women undergo multiple hormonal changes throughout their lives, leading to different physical and emotional experiences. Dr. Carilyn Hoffman, at Renown Women's Health, explains these confusing life stages and helps decode menopause. Perimenopause: Transitioning Towards Menopause Defined as the time "around menopause," perimenopausal symptoms are caused by hormonal fluctuations that occur as the ovarian function declines. Levels of estrogen and progesterone decrease, and follicle stimulating hormone increases. These hormonal fluctuations may cause a range of symptoms including: Irregular or abnormal periods: Initially cycles intervals vary in length by greater than 7 days, then in later stages the interval increases to greater than 60 days between cycles Hot flashes and night sweats: This is the most common symptom and 50-82% of women will have vasomotor symptoms Mood swings and memory problems Anxiety or insomnia Heart palpitations Decreased libido and vaginal dryness Weight gain and thinning hair Increased risk of urinary tract infections Decreased bone density Menopause Menopause is defined as year without a menstrual cycle and marks the timeframe when the ovaries stop making estrogen. This signifies the end of the reproductive years. The average age of menopause is 51; however, the menopausal transition can last about 8 years. This means that women in their late 30’s and 40’s may start to have symptoms of perimenopause. The worst vasomotor symptoms are typically experienced at the one-year mark since the last period. Unfortunately, some women experience symptoms throughout the entire menopausal transition. Postmenopausal After 12 months without a menstrual cycle, a woman is confirmed to be postmenopausal. This is sometimes difficult to define, as women may have had procedures that cause menstrual suppression such as a uterine ablation or hysterectomy or they may still be on contraception. Sometimes, lab work may be recommended to help determine menopausal status. However, due to the broad time period that the menopausal transition occurs and the variations in normal hormone levels throughout a cycle, lab work is not always helpful. Dr. Hoffman explains the importance of thorough counseling for patients seeking to "check their hormone levels." She emphasizes that menopause is diagnosed clinically, focusing more on the individual's symptoms rather than lab values. This approach ensures that patients understand the implications of the test results and the treatment strategy. Menopause Medical Management Medical management of symptoms should be tailored to the individual’s concerns. Abnormal Bleeding: There are a range of medications, IUDs and procedures available if the main concern is irregular or prolonged menstrual bleeding during perimenopause. Hot Flashes and Night Sweats: Hormone Replacement Therapy (HRT): HRT is currently the most effective method for relieving vasomotor symptoms. However, it's important to discuss potential risks with a healthcare provider, as HRT can increase your risk of blood clots and breast cancer. If improperly prescribed, it can also increase the risk of uterine cancer. The American College of Obstetricians and Gynecologists recommends the lowest dose for the shortest duration. Low-dose antidepressants: SSRIs/SSNIs may mitigate hot flashes and mood disorders for those who are not candidates or prefer to avoid HRT. Currently, only Paroxetine is FDA-approved for this use. Fezolinetant: This is a newly FDA-approved non-hormonal medication that works at the brain's level to treat vasomotor symptoms. Gabapentin: This is an anticonvulsant medication that has been shown in several studies to be helpful for vasomotor symptoms, but it is not currently FDA-approved. Genitourinary Symptoms of Menopause: Vaginal estrogen: Vaginal dryness and pain with intercourse due to thinning vaginal tissue is a common symptom of menopause. Vaginal estrogen is highly effective at decreasing these symptoms and has fewer side effects than systemic HRT. Ospemifene: This is a selective estrogen receptor modulator that is a non-hormonal FDA-approved medication for severe vaginal dryness. Natural Symptom Relief Strategies: Nutrition: Incorporate calcium, vitamin D, and high-quality protein to support bone health and muscle maintenance. There are limited studies on phytoestrogens (found in soy and tofu) and vasomotor symptoms. While the data doesn’t necessarily support that these phytoestrogens relieve symptoms, no detrimental effects were found and these tend to be high quality and healthy proteins. Exercise: Regular physical activity can ease menopausal symptoms and support weight management. Data doesn’t support that this reduces vasomotor symptoms, but it can be helpful in weight management and sleep quality. Beverage choices: Limiting alcohol and caffeine can help decrease the frequency of vasomotor symptoms and may also improve sleep quality. Alternative remedies: One study shows that Chinese herbal medicine and acupuncture are effective at relieving vasomotor symptoms. There is not enough evidence to recommend Black Cohosh, and it is associated with liver toxicity in high doses. Studies don’t show that St. John’s Wart or Gingko Balboa are any better than placebo. Always mention your alternative medical therapies to your provider as some do interact with other prescribed medications. By understanding and recognizing that the symptoms of menopause are real and treatable, women are empowered to manage this transition better and can maintain their well-being and quality of life. Please schedule an appointment with Renown Women’s Health if you’d like to discuss your menopause symptoms with a provider.
Read More About Dr. Carilyn Hoffman's Guide to Menopause Medication & Relief
-
Are You Using the Right Sunscreen?
Seeking protection for yourself and your loved ones from the intense sun rays at northern Nevada's elevated altitudes? With so many choices available, selecting the ideal sunscreen can be daunting. To guide you through this, we consulted Dr. Angela Walker, a dermatologist from Renown Medical Group, for her expert insights. Sunscreen Application Dermatologists recommend a broad-spectrum sunscreen with a minimum SPF of 30, but keep in mind that no sunscreen protects against 100 percent of UV radiation and that reapplication is necessary. “No matter the SPF, sunscreen must be applied adequately and frequently, meaning a quarter-sized amount to cover the face and neck and a full shot glass amount for the body when wearing a bathing suit,” said Walker. “Reapplication should be every 80 minutes.” Why not use a high SPF, such as 70 or 100? According to the Skin Cancer Foundation, they don’t offer significantly more protection than SPF 30 and mislead people into thinking they have a higher level of protection. Here’s the breakdown: SPF 15 blocks 93 percent of UVB rays SPF 30 blocks 97 percent of UVB rays SPF 50 blocks 98 percent of UVB rays SPF 100 blocks 99 percent of UVB rays Do specific populations require a higher SPF? Walker explains that infants, seniors, and those with a history of skin cancer must take precautions against UV radiation, as their skin is vulnerable. Sunscreen should be an absolute priority before spending time outdoors and avoiding prolonged sun exposure, wearing a hat with wide brim (recommended 4-inch brim) and UPF (ultraviolet protection factor) clothing. Due to the sensitive nature of an infant’s skin, babies under six months should not spend time in the direct sun. For infants and toddlers six months and older, whose skin is thinner than adults, a sunscreen that contains zinc oxide or titanium dioxide (physical protectors) should be applied. Zinc and titanium are less likely to irritate because they do not penetrate the skin and instead sit on the surface and deflect UV radiation. Zinc oxide and titanium dioxide are vital ingredients to seek out in sunscreen due to their strong ability to deflect UV radiation. Sunscreen Terms Explained UVA = Long wave ultraviolet light. Penetrates deep into the dermis, the skin’s thickest layer, causing tissue damage that wrinkles and photo-aging and contributes to developing skin cancer. UVB = Short wave ultraviolet light. The biggest contributor to the development of skin cancer and are more prevalent during mid-day. SPF = Sun protection factor. Calculated by comparing the amount of time needed to burn sunscreen-protected skin vs. unprotected skin. So, SPF 15 means you can stay in the sun 15 times longer than you could without protection.
-
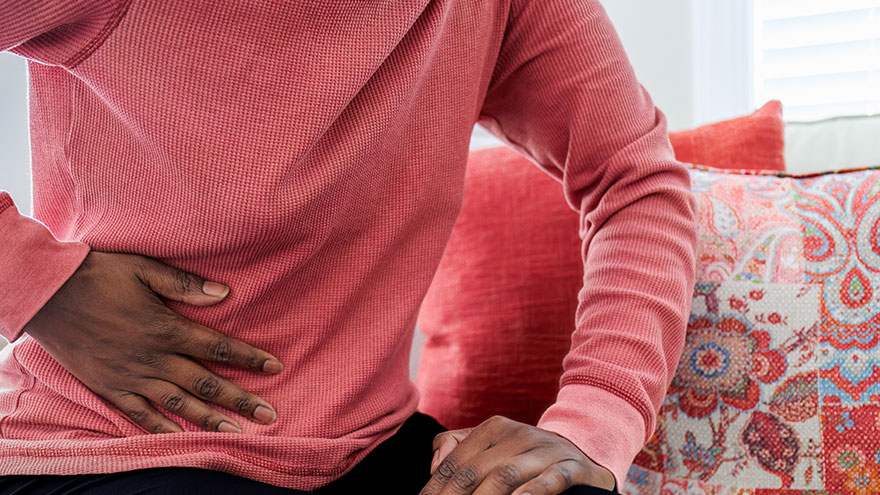
What is an Ovarian Cyst, and How is it Treated?
Abdominal pain is one of the most common reasons for an Emergency Room visit. The abdomen is an area that encompasses multiple organs and functions. So how would you know when the pain you are feeling is an ovarian cyst or something else, and when should you seek medical attention? Dr. Carilyn Hoffman, at Renown Women's Health, explains. Ovarian Function Defined Located on each side of the uterus, the ovaries are part of the female reproductive organs and produce eggs (ova), released during the menstrual cycle, allowing for fertilization and pregnancy. They also produce hormones such as estrogen and progesterone, which play an important role in female traits, bone health, cardiovascular health and pregnancy. Symptoms of an Ovarian Cyst Cysts are solid or fluid-filled masses. Ovarian cysts can be in the ovary or on its surface. When cysts are enlarged or rupture, they can create a dull ache or sharp pain below the belly button. Besides discomfort and pain, other symptoms of ovarian cysts may include bloating, fullness, pressure or heaviness. "Ovarian cysts are common; most are physiologic and will go away on their own. They are frequently found incidentally on ultrasound and are present in the middle of the menstrual cycle," says Dr. Hoffman. "However, if a woman experiences sudden and severe pelvic pain they should seek immediate medical attention. Sometimes ovarian cysts can become large and twist on themselves. This is called ovarian torsion and is a surgical emergency. Other times, cysts can rupture and bleed. This is called a hemorrhagic cyst and can also be a surgical emergency." Diagnosis and Treatment If an ovarian cyst is suspected, your doctor will perform a pelvic exam and order an ultrasound. There are certain ultrasound findings that suggest that the cyst is benign. There are other ultrasound findings that are concerning for cancer. Small simple cysts often resolve on their own, whereas solid or very large cysts may require surgery.
Read More About What is an Ovarian Cyst, and How is it Treated?
-
The Expanded Role of OBGYNs in Women's Healthcare
Obstetrician-gynecologists (OBGYNs) see patients from menses (the monthly menstrual cycle that occurs as a part of the female reproductive system), pregnancy and childbirth through menopause and play a pivotal role in managing reproductive health and overall wellness. Dr. James Alexander with Renown Women's Health explains. "As experts in women's health, we are uniquely positioned to recognize subtle changes or symptoms that might indicate broader health issues. This comprehensive approach allows us to serve as a valuable first touchpoint for various health concerns." Preventive Screenings: A Proactive Approach One key aspect is an OBGYN's ability to recommend preventive screenings based on your symptoms, age, lifestyle and medical history. For instance, lipid screenings are critical for monitoring cholesterol levels, which can be a significant factor in women’s heart disease. An OBGYN keeps up with the current guidelines for routine screening as well as in women with risk factors such as high blood pressure, diabetes, or a family history of heart disease during your visit. By identifying risks and abnormal screening early, they can collaborate with you to implement lifestyle changes or treatments to reduce your risk of heart conditions. Schedule Your Screening Appointment Make an Appointment by Phone: 775-982-5000
Read More About The Expanded Role of OBGYNs in Women's Healthcare
-
Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
Raquel was 33 when she was diagnosed with breast cancer. It was April 2023, when she found a lump in her breast and was referred to the William N. Pennington Cancer Institute. After comprehensive imaging, she was diagnosed with invasive lobular carcinoma, which is a type of breast cancer that begins in the milk-producing glands of the breast. Between June 2023 and January 2024, she received a total mastectomy, chemotherapy and radiation at Renown Health. “Breast cancer is uncommon in women under 40, but any woman with a mass or lump in her breast should have an exam by a physician and imaging at any age,” said Dr. Lee Schwartzberg. In fact, according to the Centers for Disease Control and Prevention (CDC), only 9% of all new cases of breast cancer in the U.S. are found in women younger than 45. “It was a pretty scary diagnosis, but I’ve been led by great people through the process,” she said. “They were so helpful and there for me throughout the chemo and radiation.” Raquel's journey through breast cancer treatment at the William N. Pennington Cancer Institute was marked by the exceptional care provided by the Renown Health team, including nurses, nurse navigators, therapists, support teams and providers. Among the dedicated professionals, Dr. Michelle Chu and Dr. Lee Schwartzberg played pivotal roles in Raquel's diagnosis and subsequent treatment plan. Their expertise, compassion and commitment to patient care left an indelible impact on Raquel's experience. Their thorough examination and comprehensive approach ensured that Racquel received the best possible care for her invasive lobular carcinoma. In addition to the care provided at Renown, Raquel greatly benefitted from being connected with a mentor by Dr. Chu. This mentor, Kayla, had undergone a similar diagnosis and treatment plan, and at the same age Raquel. They texted and called each other throughout Raquel’s treatment, providing additional support through a challenging time. As of January 2024, Raquel is done with her treatment and continues to see her care team for follow-up appointments. “I’m through the worst and ready to rebuild my life,” Raquel said. To help celebrate this milestone, Nevada Athletics invited Raquel to receive the game ball at a Nevada Men’s Basketball game. She was joined on the basketball court for this special recognition by her husband, Raul; mother, Arlene; and two daughters, Ryleigh and Rhiannon. Racquel's journey is not only a testament to her resilience but also a tribute to the invaluable contributions of Dr. Chu and Dr. Schwartzberg in guiding her towards triumph over breast cancer.
Read More About Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
-
Most Common Reasons Women Visit the ER
If you or someone you know is experiencing a medical emergency, it's essential to seek immediate attention by calling 9-1-1 or visiting the ER for a thorough evaluation by a trained medical professional and timely intervention. Access to a convenient and trusted emergency room (ER) is critical to any person’s healthcare needs, including medical emergencies related to women’s health. We explored some common scenarios and warning signs prompting women to seek immediate medical attention with Aiden Gould, Board-Certified Emergency Physician at Renown Health. When your medical emergency can’t wait, Renown ER is here to provide you with the region’s leading emergency care to diagnose and treat your condition or illness. Understanding Common Reasons Women Visit the Emergency Room Gynecological Emergencies: One of the most common reasons women may seek emergency care is due to gynecological emergencies such as severe pelvic pain, abnormal bleeding or complications related to pregnancy. These issues can be alarming and warrant immediate medical attention if the issue persists or is out of the ordinary for you. Emotional and Physical Well-Being: For those facing diverse medical or mental health emergencies, seeking prompt assistance is crucial for a thorough assessment and safe, timely intervention. Renown ER teams are equipped with trained professionals who provide compassionate care for individuals seeking help in the following situations: Suicide risk assessment and intervention Substance abuse assessment Assault and trauma care Crisis support and intervention Resources for ongoing care and well-being support Severe Abdominal Pain: Unexplained and severe abdominal pain that is substantially different than what is normal for you is a symptom you should never ignore as it can indicate underlying issues. Warning signs of an acute medical situation include fever, vomiting or a rapid change in motor function and inability to move due to pain. Respiratory Distress: Difficulty breathing, persistent coughing and other respiratory issues can be especially concerning. Women with pre-existing respiratory conditions like asthma or those experiencing sudden respiratory distress should seek immediate care from a medical professional. Warning signs of respiratory distress may include a significant change in one’s breathing rate, changing of the skin color to blue, gray or paleness due to lack of oxygen, nose flaring and chest retractions. Cardiovascular Emergencies: Heart-related issues are not exclusive to men. Women can also experience cardiovascular emergencies that often go undiagnosed because symptoms differ from men. Symptoms like chest pain, extreme fatigue, vomiting or pain in the abdomen, shortness of breath or palpitations should be evaluated by an emergency medical professional as timely intervention is critical in such cases. Renown leads the region in cardiology care with our technological expertise and patient-centered approach. Our comprehensive team diagnoses heart disease and other cardiac conditions, offering personalized treatment plans. Neurological Symptoms: Sudden and severe headaches, seizures or other neurological symptoms may prompt women to visit the ER if symptoms are extremely disorientating or debilitating. These symptoms could be indicative of various conditions from mild to severe, including strokes or neurological disorders that require prompt evaluation. Renown Regional Medical Center is a Comprehensive Stroke Center, providing primary stroke care including evaluation, treatment and education to patients who arrive at a Renown facility with the signs and symptoms of a stroke. Compassionate Care in Times of Need At Renown Health, we understand that your time is valuable, especially in emergency situations. That's why we strive to provide patients with exceptional care, compassion and respect. Plan ahead and make informed decisions about seeking medical care by viewing your estimated triage wait time at a Renown ER.
-
Understanding the Reasons Behind Heavy Menstrual Cycles
While menstrual cycles can be an annoying inconvenience for many women, heavy bleeding (menorrhagia) is not normal and can disrupt your life. A few days of heavy flow at the start of your period is usually nothing to worry about. However, if you’re frequently experiencing very heavy periods, you should discuss it with your gynecologist or primary care provider. Dr. Megan Fish, an OB-GYN with Renown Women’s Health, discusses various reasons, evaluation and treatment methods when it comes to heavy menstrual cycles. What is classified as heavy menstrual bleeding? The American College of Obstetricians and Gynecologists considers heavy bleeding to be any of the following signs: Bleeding that lasts more than 7 days. Bleeding that soaks through one or more tampons or pads every hour for several hours in a row. Needing to wear more than one pad at a time to control menstrual flow. Needing to change pads or tampons during the night. Menstrual flow with blood clots that are as big as a quarter or larger. What are the most common reasons for heavier periods? A variety of reasons why someone might have heavy periods. Fortunately, most of these problems are treatable. Because each woman's period is unique, only a doctor can definitively determine the cause of your heavy periods. Some of the most common issues that cause heavy periods include: Hormone imbalances such as anovulation, thyroid disease and Polycystic Ovary Syndrome (PCOS). Structural abnormalities in your uterus such as polyps or fibroids. Precancer and cancer such as uterine, cervical, vaginal, ovarian or endometrial hyperplasia. Infections such as chlamydia, gonorrhea, endometritis or vaginitis. Other medical conditions such as liver disease, kidney disease or Pelvic Inflammatory Disease. Medications such as blood thinners and aspirin, hormone replacement therapy, Intrauterine devices (IUDs), birth control pills and injectables. Pregnancy-related problems such as a miscarriage or ectopic pregnancy.
Read More About Understanding the Reasons Behind Heavy Menstrual Cycles
-
What is Polycystic Ovary Syndrome (PCOS)?
Dr. Carilyn Hoffman with Renown's Women's Health explains the symptoms, causes and treatments of Polycystic Ovary Syndrome (PCOS) (also referred to as Polycystic Ovarian Disease (PCOD)), a prevalent condition among women of reproductive age that influences hormonal balance, metabolism and fertility. Make an appointment with Renown Women's Health Click here to schedule Call to schedule: 775-982-5000 PCOS Defined PCOS is a constellation of symptoms characterized by two of the three criteria: multiple small cysts on the ovaries visible via ultrasound, irregular periods and signs of hyperandrogenism. Other symptoms include infertility, insulin resistance, and increased risk of cardiovascular disease. Symptoms of PCOS The symptoms of PCOS can vary from woman to woman, but some of the most common include: Irregular menstrual cycles: This is often one of the first signs of PCOS. Women may experience fewer than nine periods a year, more than 35 days between periods, frequent spotting, and/or abnormally heavy periods. Excess androgen levels: High levels of male hormones may result in physical signs such as excess facial and body hair (hirsutism), severe acne and male-pattern baldness. Polycystic ovaries: Enlarged ovaries containing numerous small cysts can be detected via ultrasound. Causes and Risk Factors The exact cause of PCOS is unknown, but several factors may play a role: Genetic predisposition: A family history of PCOS increases the risk. Insulin resistance: High insulin levels might increase androgen production, causing difficulty with ovulation. Obesity: Women with elevated BMI’s are more likely to have PCOS, although 20% of women with PCOS are not obese. Diagnosis and Treatment Dr. Hoffman outlines that diagnosing PCOS requires a medical history review, a physical exam, blood work and an ultrasound to evaluate the ovaries. Treatment options can range from lifestyle modifications, like diet and exercise and weight loss, to medications for menstrual regulation, fertility assistance, and rarely surgery. Lifestyle Changes A healthy lifestyle is a cornerstone of managing PCOS. Regular exercise, a nutritious diet, and weight management can help reduce symptoms and the risk of long-term health issues. In overweight patients, weight loss as little as 5% has been shown to improve symptoms of PCOS. Medication Medications may include hormonal contraceptives to regulate menstrual cycles, anti-androgens to reduce hair growth and acne, and Metformin to address insulin resistance. Fertility Treatment For women with PCOS who are trying to conceive, ovulation induction with clomiphene or letrozole is sometimes necessary. Sometimes a referral to a reproductive endocrinologist and infertility specialist is needed for more advanced technologies like IVF. Health Implications PCOS is not just about cystic ovaries or irregular periods; it can have profound implications on a woman's overall health. Women with PCOS are at an increased risk for several conditions, including type 2 diabetes, high blood pressure, heart disease, and endometrial cancer.
-
How Regular Cervical Cancer Screenings Can Save Lives
According to the American Cancer Society, approximately 13,820 new cases of invasive cervical cancer will be diagnosed, and 4,360 women will die from cervical cancer. However, cervical cancer is preventable with regular screening tests and the HPV vaccine. It’s important to note that medical advances have allowed progress in diagnosing and treating cervical cancer. While it used to be one of the most common causes of cancer death for American women, the incidence of death has significantly declined. What to Know About the HPV Vaccine HPV vaccination is the best way to prevent cervical cancer and is recommended for all youth starting as early as age 9, or for teens and adults up to age 45 who didn’t start or finish the series. In Nevada, only 50.1% of teens ages 13-17 have been vaccinated for HPV. There are 13 types of HPV, and the vaccine Gardasil 9 protects against 9 of those HPV strains, greatly reducing the incidence of cervical cancer among vaccinated individuals. What to Know About Cervical Cancer Screenings The CDC says the most important thing you can do to help prevent cervical cancer is to have regular screening tests starting at age 21. And there are two common tests that can detect early stages of cervical cancer (or precancer) and improve health outcomes. The pap test (or pap smear). This screening looks for precancers. Women should begin getting pap smears when they’re 21. The human papillomavirus (HPV) test looks for the virus that can cause these cell changes. Cervical Cancer Screening Schedule The American Cancer Society offers the following guidelines for screenings: All women should begin cervical cancer screening at 21. Women between 21 and 29 should have a pap test every three years. Beginning at 30, the preferred way to screen is with a pap test combined with an HPV test every five years. This is called co-testing and should continue until age 65. A pap test (or pap smear) is performed during a regular screening appointment to look for precancers, cell changes on the cervix that might become cervical cancer if they are not evaluated or appropriately treated. Typically outpatient procedures can reduce the risk of long-term health impacts that prevent pre-cancerous cells from becoming cancer cells. Women over 65 who have had regular screenings in the previous ten years should stop cervical cancer screening as long as they haven’t had any severe precancers found in the last 20 years. How to Get Screened Request an appointment with your primary care physician or OBGYN to schedule a screening.
Read More About How Regular Cervical Cancer Screenings Can Save Lives
-
Winter Skin Care: 5 Must-Know Pro Tips
As the seasons shift, so do the demands of our skin. We sat down with Heidi Nicol, a seasoned aesthetician at Renown Dermatology, Laser & Skin Care, to uncover the secrets of pampering your skin during the winter onset. The aftermath of summer often leaves us with dry, dull skin and unexpected breakouts. However, a few tweaks to your skincare regimen can make this seasonal transition smoother. 1. Re-evaluate Your Cleanser Now might be the opportune moment to transition to a non-drying cleanser. The one that worked wonders in the summer might be aggressive for the colder months. Nicol suggests opting for a "gentle" cleanser that effectively cleanses and exfoliates without including abrasive ingredients. 2. Amp Up the Hydration With the dip in temperature, your skin craves a richer moisturizer. Seek out products enriched with Hyaluronic Acid. This powerhouse ingredient amplifies your skin's ability to retain moisture, ensuring it stays supple throughout the day. 3. Introduce Retinol If retinol isn't a staple in your skincare arsenal yet, consider introducing it now. Its prowess in diminishing sun-induced brown spots and fine lines is unparalleled.
-
Why Is My Hair Falling Out? Alopecia Explained
Hair is often considered a symbol of identity and self-expression, from scalps and eyebrows to beards and bodies. But what happens when this symbol starts to fall out? The 6.7 million people across the country living with alopecia know this feeling all too well. Alopecia, or hair loss, is a medical condition with variable causes, presentations and treatments. Experts at Renown Health dive into the world of alopecia, its causes and how to address it – especially as we embrace National Alopecia Awareness Month this September. Types of Alopecia The term “alopecia” is a broad umbrella term that encompasses many different forms of hair loss that can present itself at any age, no matter your gender or ethnicity. The most common types include: Alopecia Areata: An autoimmune disorder where the immune system targets hair follicles, typically resulting in patches of hair loss on the scalp and/or other body parts. More severe forms of alopecia areata also exist, such as alopecia totalis and alopecia universalis. Androgenetic (or Androgenic) Alopecia: A disorder also known as male or female pattern baldness that causes gradual hair thinning and loss often around the temples and crown. Unlike alopecia areata, this form of alopecia is usually hereditary. Telogen Effluvium: A condition resulting in hair shedding, typically after high-stress or infectious events, such as after giving birth or after a COVID-19 infection. This usually resolves itself within a few months to a year. Traction Alopecia: Hair loss resulting from the effects of tight braiding or styling of the hair, which can cause permanent loss over time. Scarring and Inflammation-Mediated Hair Loss: Patterns of hair loss related to lupus, lichen planus or other autoimmune conditions that can unfortunately be permanent and progressive. Options to Treat Alopecia While there isn’t a cure for most types of alopecia, some treatments are available to help minimize the effects of the condition and promote hair growth. Treatment varies depending on the type of alopecia. Potential options can include: Topical Minoxidil: An FDA-approved over-the-counter medication available in foam or liquid form and applied directly to the scalp, which helps stimulate hair growth by increasing blood flow to hair follicles. Hormone Therapies: A hormone regimen that can help minimize the resulting hair thinning and balding. Corticosteroids: A topical cream or ointment – or an injection for severe cases – that help reduce inflammation and re-grow hair. Low-Level Laser Therapy: A therapeutic, non-invasive intervention involving wearing special caps or combs that release painless, low-level lasers to stimulate hair follicles. Healthy Diets and Nutritional Supplements: A diet rich in vitamins and minerals essential for hair health, such as biotin and collagen, can aid in recovery. Vitamin D and iron are also important hair growth nutrients. Stress Management: Stress can impact the speed and frequency of hair loss. Managing your stress can help mitigate the effects of alopecia. Treatment for alopecia is not a one-size-fits-all approach. A scalp skin biopsy may help determine a cause for hair loss and help guide the best management strategies with your provider. Addressing the Emotional Impacts Even though alopecia isn’t life-threatening, the impacts of the condition can affect your self-esteem and self-image. The most powerful tool to help you manage alopecia is knowledge. Keeping yourself educated about your condition, and encouraging your loved ones to do the same, can help arm yourself with the acceptance and self-compassion you need and help combat misconceptions. With the rise in awareness in the mainstream media for alopecia and other hair conditions, beauty standards and fashion are shifting to become more inclusive for those experiencing hair loss. Celebrating the many diverse hairstyles and fashion statements can help you regain your confidence. There are many options you can advantage of to help style your hair and protect your scalp: Hairpieces: Wigs, extensions and other hairpieces can help cover up balding or thinning patches and add volume to your hair. Hairpieces have come a long way in the past few decades, and many use real human hair. Hats: Hats serve a dual purpose – a fun fashion accessory to help boost your confidence and a method of protecting your scalp from the sun. As someone with alopecia, your scalp is more exposed, and hats can provide that extra layer of protection you need. Scalp Sunscreens: While regular body sunscreens can provide good scalp sun protection, they can result in oily scalp and hair appearance. Sunscreens that are specifically designed for the scalp are available at most beauty stores or online. Remember, patience is fundamental, as many treatments require consistent use over time to see noticeable results. Stay resilient, and don’t give up – you are not alone in your alopecia journey.
Read More About Why Is My Hair Falling Out? Alopecia Explained
-
How to Get Vitamin D on Cloudy Days, and Every Day
Vitamin D, also known as the sunshine vitamin, is considered a pro-hormone and is synthesized by our bodies when skin is exposed to sunlight. It helps our bodies absorb calcium, build strong bones and teeth, can help ward off osteoporosis and can help reduce the risk of developing type 2 diabetes by 15%. However, getting the vitamin D you need isn’t quite as simple as soaking up the rays. Vitamin D breaks down quickly, and in the winter – especially in northern latitudes – the sun never gets high enough for UVB rays to penetrate the atmosphere and reach your skin. So how do you get enough vitamin D? We asked Alexandra Westover, APRN for Renown Health, for more information on the topic. "Vitamin D deficiency is found to be linked to multiple health concerns; everything from cancer to depression," says Alexandra. “That said, rates of vitamin D deficiency are high in the U.S. due to various reasons, with the increasing rates of obesity being one factor." Another factor explaining why most Americans are low in vitamin D is that we get very little of our vitamin D from our diet, with most of our vitamin D being produced via exposure to sunlight. However, lounging in the sun for long hours without sunblock isn’t recommend either due to risk for skin cancer, thus, a supplement might not be a bad idea if your doctor is okay with it. "If your vitamin D levels are low, eating high vitamin D foods, such as fatty fish, mushrooms, dairy, eggs and fortified cereals and orange juice, can help, but it typically isn’t enough to correct a deficiency, nor are over-the-counter vitamin D supplements,” said Alexandra. “Most people require a prescription-dose level of vitamin D to correct deficiency." Top 5 Reasons Why You Need Vitamin D Maintains healthy bones and teeth Supports the health of the immune system, brain, and nervous system Regulates insulin levels and aids diabetes management Supports lung function and cardiovascular health Influences the expression of genes involved in cancer development Eating Foods That Are Rich in Vitamin D Fatty fish such as salmon, herring and tuna Fortified milk and orange juice Fortified cereals Eggs Mushrooms Cod Liver Oil
Read More About How to Get Vitamin D on Cloudy Days, and Every Day