Search
Results for 'clinic'
Clear-
Understanding the Risks of Colon Cancer
Colorectal cancer is the second-deadliest cancer in the United States – largely because it goes undiagnosed. Dr. Christi Matteoni, Division Chief of Gastroenterology at Renown Health, discusses the symptoms and key screenings used to detect this type of cancer, along with risk factors and lifestyle changes that could affect the likelihood of getting the disease. What are some of the signs and symptoms of colorectal cancer? Many cases go undiagnosed because polyps can develop and become cancerous without any symptoms. Additionally, since colorectal cancer begins as small polyps, symptoms usually aren’t seen until later stages. This is why screenings are especially important. For those who do experience symptoms, the signs are often tied to your bowel habits. This can include changes such as constipation or diarrhea, narrow or dark stool, rectal bleeding, abdominal cramping, weakness and fatigue or unintended weight loss. What are some of the risk factors associated with this type of cancer? There are risk factors that can and cannot be controlled. Uncontrollable factors include age, race, personal and family histories as well as certain genetic syndromes that are important to discuss with your provider. This type of cancer is more common in people over the age of 50, African Americans and those of eastern European Jewish (Ashkenazi) descent. This type of cancer is also more common in those who have been diagnosed with polyps, Crohn’s disease, ulcerative colitis and long-term inflammatory bowel disease. important to discuss any of these risk factors with your provider. There are also lifestyle factors that can help reduce your risk. Factors include being overweight, having a diet high in red and processed meat, as well as smoking and consuming excess alcohol. Conversely, diets high in fruits and vegetables and a regular exercise routine can help lower your risk. If someone has some of these risk factors, what should they do? Do they need to get tested? If you are 45 or older and have any of these risk factors, we recommend you speak with your primary care provider about a formal colorectal risk assessment. The most common form of screening is colonoscopy. This screening lets your doctor examine the length of your colon, map out any potential problem areas and remove polyps. For most people, colonoscopies are recommended every 10 years starting at age 50. However, depending on your results and risk factors, you may need to begin screening sooner or get screened more frequently. What do diagnosis and treatment look like for this type of cancer? There are several diagnostic options for colorectal cancer, including endoscopic ultrasound; CT, MRI and PET scans; and biopsy and pathology reports. These technologies allow your doctor to get images of your colon and evaluate what treatment is needed, as well as how the treatment is progressing. Treatment varies for each individual working with their doctor. In the case of colorectal cancer treatment, the William N. Pennington Institute for Cancer offers chemotherapy, radiation therapy, surgery and clinical trials.
-
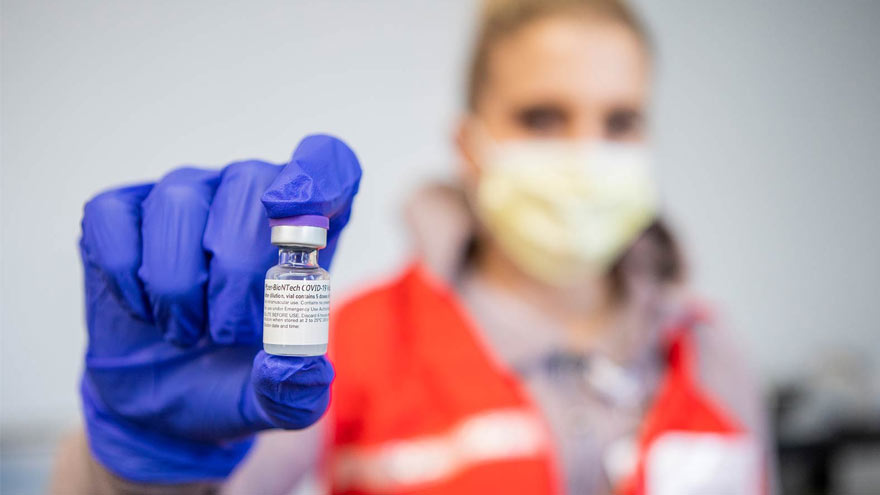
Pharmacists Answer Questions about the COVID-19 Vaccines
Vaccines that provide protection against the COVID-19 virus are bringing us closer to the end of this deadly pandemic. Two different COVID-19 vaccines are currently available in the U.S. today: one from Pfizer and the other from Moderna. Kate Ward, PharmD, BCPS, Director of Clinical Pharmacy at Renown Health and Adam Porath, PharmD, Vice President of Pharmacy at Renown, share what you need to know about these vaccines. When two COVID-19 vaccines were approved by the U.S. Food & Drug Administration (FDA) in December 2020, it was cause for celebration. Why? Because according to the CDC, the vaccines are 94 percent or more effective in providing protection against the COVID-19 virus! Many people are seeking information about the new Moderna and Pfizer vaccines. Below, our pharmacy leaders provide answers to some commonly asked questions. How do the COVID-19 Vaccines Work? The Pfizer and Moderna vaccines are both mRNA vaccines that help your immune system develop antibodies against the COVID-19 virus. The vaccines use messenger RNA, or mRNA, to show our bodies’ protein-making cells how to make the spike proteins of the COVID-19 virus. Our immune system reacts to these spike proteins by creating antibodies that can recognize and destroy them. So when a person is exposed to the virus in the future, they will be less likely to get sick. What are the Differences between the Pfizer and Moderna Vaccines? The Pfizer and Moderna COVID-19 vaccines are very similar, with just a few small differences worth noting. The main difference between the two vaccines is when you should receive your follow-up dose. Patients who receive a first dose of Pfizer should receive their second dose about three weeks later. Those who receive a first dose of Moderna should receive their follow-up vaccination roughly four weeks after their first dose. People 18 years and older can receive the Moderna vaccine while people 16 years and older can receive the Pfizer vaccine. Dosage for the Moderna vaccine is 0.5 ml (100 mcg). Dosage for the Pfizer vaccine is 0.3 ml (30 mcg).
Read More About Pharmacists Answer Questions about the COVID-19 Vaccines