Search
-
What You Need To Know About Cold Water Drowning
Northern Nevada's stunning lakes, including Lake Tahoe, with its average summer water temperature of 50 degrees, present a potential risk of hypothermia. Unlike mild 50-degree air, water at the same temperature poses severe, life-threatening risks, including rapid-onset hypothermia and drowning. Awareness of the symptoms and taking proper precautions are crucial to prevent cold-water drowning. The 4 Phases of Cold-Water Drowning 1. Cold Shock Response: This response affects breathing and happens within the first minute. An automatic gasp reflex occurs in response to rapid skin cooling. If the head goes below water, water may be breathed into the lungs, resulting in drowning. A life jacket will help keep your head above water during this critical phase. Additionally, hyperventilation, like the gasp reflex, is a response to the cold and will subside. Panic will make this worse, so the key is to control breathing. 2. Cold Incapacitation: This response occurs within the first five to 15 minutes in cold water. In order to preserve core heat, vasoconstriction takes place decreasing blood flow to the extremities to protect the vital organs. The result is a loss of movement to hands, feet, arms and legs. Unless a life jacket is being worn, the ability to stay afloat is next to impossible. 3. Hypothermia: Important to note, it can take 30 minutes or more for most adults to become hypothermic. So there’s time to take action and survive. Keeping panic at bay is critical, as you have more survival time than you think. Symptoms include: Shivering Slow and shallow breathing Confusion Drowsiness or exhaustion Slurred speech Loss of coordination Weak pulse 4. Circum-rescue Collapse: This experience can happen just before rescue and is not well understood. Symptoms range anywhere from fainting to death. Some experts believe an abrupt drop in blood pressure may cause this final stage of cold water drowning, post-rescue. Additional Safety Tips and Helpful Resources Always wear a personal flotation device as well as a wetsuit or drysuit. Your personal flotation device is the most important piece of water safety gear. Try not to panic as the first phases will subside. Controlled breathing is to staying calm. Research suggests the body can withstand the cold longer than we think. The Heat Escape Lessening Posture (HELP) is a position which helps conserve energy if you’re wearing a personal flotation device. By hugging your knees to your chest, this posture helps maintain body heat for some time.
Read More About What You Need To Know About Cold Water Drowning
-
What is Dry Drowning?
Whether you're a parent, grandparent, caregiver, or sibling, it's vital to recognize that drowning is the second leading cause of death among children," states Dr. Leland Sullivan, of Northern Nevada Emergency Physicians. "While we diligently work to protect children from water-related accidents, there's a lesser-known threat that often goes unnoticed—dry drowning, also known as delayed drowning. Surprisingly, many people remain unaware of its existence and potential dangers. Dry drowning defined Dry drowning is a side-effect of a near-drowning experience and includes spasms of the vocal cords and larynx — known as a laryngospasm. This occurs when the body attempts to shut down the passage of any liquid into the lungs. Unfortunately, it can also shut down the passage of air into the lungs and force fluid into the stomach and lungs. Often the condition is not discovered until it's too late — severe cases can cause death within one to 24 hours after a water incident occurs. Who is susceptible? Novice or first-time swimmers are at increased risk, as are children with asthma and known breathing issues. In addition, children who have had pneumonia or experienced acute respiratory distress syndrome are also at greater risk. To reduce these factors, caregivers should be exceptionally watchful of inexperienced swimmers. According to Dr. Sullivan, children under the age of 5 are most susceptible to drowning and often drown in residential swimming pools. Infants less than 1-year-old most often drown in bathtubs. What are the signs of a dry drowning episode? If your child has a near-drowning incident, a few moments of coughing until they calm down is normal. However, you should know the more severe signs and symptoms to watch for during the 24 hours following the incident, including: Persistent coughing Difficulty breathing and/or shortness of breath Chest pains Extreme fatigue and/or lethargy Change in typical behavior Face becomes pale What is the treatment and prognosis for dry drowning? Dr. Sullivan recommends that all victims of near-drowning incidents seek medical attention, even if they have no symptoms. If caught early, dry drowning can be treated. If you think your child is experiencing a dry drowning episode, go to the nearest emergency room as quickly as possible — do not attempt treatment at home. Healthcare professionals will work to supply oxygen to your child's lungs to restore and regulate breathing.
-
Meet Janelle Wood: Family, Hobbies & Everything In Between
Janelle Wood’s life has been filled with moves across several states, travel, different jobs, multiple hobbies and best of all – her big family. She is very close to and proud of her entire family, including her six children, six grandchildren and extended family members. New Chapters Janelle was born in 1950 in Fayetteville, Arkansas. She lived there her entire childhood and attended the University of Arkansas, Fayetteville where she received her Associate degree in Accounting. She then moved a few different times to various states including Louisiana and Arizona. In 1981, she and her family moved to Reno where she worked for a construction and mining supply company. In 1993, they relocated to a small town in southern Georgia called Thomasville, where Janelle worked for another mining and manufacturing company. “I was ready for a change of scenery and wanted to explore living in a new area,” said Janelle. “I was intrigued by moving to a smaller town to raise my children.” She and her family lived there for about 10 years when she eventually got transferred to Chicago for her job, to work at the company’s headquarters. “I was once again excited for another change and was happy to experience living in a big city,” said Janelle. “I loved my job and getting to travel as much as I did.” Janelle worked for the company in Chicago until 2014 when she decided to retire and move back to Reno to be closer to her son, daughter and grandchildren. Living to the Fullest Today, Janelle lives in Damonte Ranch in south Reno. She loves spending time outdoors, especially in the mountains and by the water. Her other hobbies include reading, cooking, doing puzzles, playing computer games antique shopping and something very unique – exploring old graveyards. “I love how they’re full of history and each one is different – I also enjoy reading what the headstones say, and the stories they tell,” said Janelle. “When I travel, I like to explore the old cemeteries that are nearby.” Janelle’s son even bought her a book called 129 Cemeteries to Visit Before You Die. She’s been to a few of them. As for traveling, Janelle’s favorite destination she’s been to is Catalina Island – she loves the history there. She also loves Chicago, Portland, Seattle, Canada and Mexico. “I’m always up for going someplace new,” said Janelle . Janelle Wood hiking to Rainbow Falls in Mammoth, CA When Christmas rolls around, Janelle loves to decorate. Her family finds it interesting just how crazy about Christmas she is. “I have 31 totes of Christmas décor and a dozen large decorations,” said Janelle. “My entire storage room is full of Christmas decorations. I start decorating the day after Thanksgiving and it takes me about 2 to 3 days to put everything up.” Janelle said Halloween is her second favorite holiday, which she also loves to decorate for. Family Values Above all else, Janelle’s favorite thing about being retired is having so much free time to spend with her children and grandchildren who live here in Reno. “I love helping my grandkids with their schoolwork and attending their sports and activities,” said Janelle. She has been volunteering at her grandchildren’s schools here in Reno ever since her now 14-year-old grandson started kindergarten. “Family is the highlight of my life,” said Janelle. She also makes sure to stay in contact and visit as often as possible with all of her family that lives out of state, including three of her children, one of her grandkids and some of her extended family. “One of my great nieces, Madison Marsh, was recently crowned Miss America, and another one of my great nieces, Madeline Bohlman, will be competing this summer for the title of Miss USA, as the current Miss Arkansas USA,” said Janelle. “I’m very proud of both of them for using their platforms to further such important issues; pancreatic cancer research and mental health, respectively.”
Read More About Meet Janelle Wood: Family, Hobbies & Everything In Between
-
Sterling Silver Club Shining Stars: Mark & Dana Combs
Dana and Mark Combs met through mutual friends and had a long friendship before they became a couple in 2009. They were married in 2011 in a private ceremony at a small Reno chapel, and a few months later had a big celebration with their family and friends. Encouraging Others to Succeed Over the years, the happy couple has spent much of their time volunteering and giving back to others in their community. Twenty-six years ago, Mark became a bilateral lower limb amputee. For the past 10 years, he has been a prosthetic consultant, helping other amputees learn how to cope with various challenges and encouraging them to keep living life to the fullest. “Mark is great with helping people,” said Dana. Dana also does a lot of rewarding work through a Philanthropic Educational Organization (P.E.O). She is an advocate for raising money to help women ages 18 and up gain an education. Dana also enjoys tutoring English as a second language. Enjoying Quality Time, Hobbies & Travel When Dana and Mark aren’t helping others, they are spending time with their family and friends, their dog Mia (a 3-year-old Maltipoo) or enjoying one of their many hobbies. Some of Mark’s favorite things to do include playing Solitaire and strumming on his guitar. “I love to garden and play crossword puzzles and word games,” said Dana. “I’m really looking forward to the springtime to spend more time in the garden.” She loves to work out and has a membership at the UFC gym in Reno through her Senior Care Plus gym benefit. Dana also has her own online Etsy store, where she sells homemade jam jars, candle holders and vintage dolls. “Last summer I sold my first edition Barbie that I got when I was 9 years old,” said Dana. “I made quite a profit on it.”
Read More About Sterling Silver Club Shining Stars: Mark & Dana Combs
-
Optimizing Mammogram Screenings: A Genetic Approach to a Personalized Screening Schedule
© Arthon Meekodong via Canva.com Breast cancer screening has long been a cornerstone of women's healthcare. With 1 in 8 women diagnosed with breast cancer in their lifetime1, the United States Preventive Services Task Force (USPSTF) has developed screening recommendations to help detect early-stage cancer. Notably in 2023, the USPSTF revised the recommended age for biennial mammogram screenings for women with average risk to start at age 40 instead of 502, estimated to result in 19% more lives being saved3 by starting screening earlier. While initiating screening at an earlier age offers advantages to a wide demographic, concerns about the potential of over-screening prompted research into the feasibility of identifying women with lower breast cancer risk who could safely delay mammograms. While guidelines address high-risk individuals, a notable gap exists in providing recommendations tailored to those at lower risk. To gain insight into a patient's risk level, physicians are able to utilize genetic testing to understand an individual's genetic makeup, providing precise insights into their predisposition to various health conditions, including breast cancer. Armed with this genetic information, healthcare providers could craft tailored screening strategies that align with an individual’s specific risk profile. This genetic risk-based approach underscores the value of genetics in individualizing the onset of screening to help avoid over-screening and its associated costs. Surprisingly, genetic information is not currently being widely utilized to identify women at risk of breast cancer or other diseases in clinical practice, despite its potential to make a significant positive impact for patients. A recent retrospective analysis of 25,591 women from the Healthy Nevada Project4 sheds light on the potential benefits of this genetic risk-based approach. The study classified 2,338 (9.1%) of these women as having a low genetic risk for breast cancer. What's remarkable is that these women exhibited a significantly lower and later onset of breast cancer compared to their average or high-risk counterparts. This finding suggests that it might be safe for low-risk women to delay mammogram screening by 5 to 10 years without compromising their health.
-
20 Years of Compassion and Dedication
When you meet Poeth Kilonzo, Director of Oncology Nursing at Renown Health, you are immediately greeted with a warm smile that puts your mind at ease. Within the William N. Pennington Cancer Institute, Poeth enjoys a strong reputation among her employees and patients as someone they can always rely on, no matter how rough the tides may flow. As an incredibly humble oncology professional, you may not realize that behind that smile is the power of a best-in-class nurse and leader holding a 20+ year career of diverse nursing experience and leadership excellence – dedicating the majority of her service to Renown Health. Join us as we dive into Poeth’s unique journey through Renown. Finding Her Passion Ever since she could remember, Poeth has been a “people person.” Above all else, she cared for people – and she cared a lot. What better place for her to be than healthcare? After moving to northern Nevada from Kenya, she began working in private patient care working with home health and dementia patients while taking classes at Truckee Meadows Community College (TMCC) in 2000. One day, a patient asked her a question that would change the course of her career journey: Did you ever think about becoming a nurse? Driven by not only the words of encouragement of her patients and supervisors in home health but also the rallying support from her family and friends, including her husband and high school friend, who both have decades of experience interacting with nurses in healthcare (with her husband spending many of those years at Renown), Poeth knew this was the path she was meant to take. “That was it; it was like a light switch had flipped,” said Poeth. “I switched to nursing overnight.” According to Poeth, TMCC’s nursing program offered her an incredibly supportive environment, which was especially important as she was a young mom at the time. Working in healthcare, going to nursing school and raising a family all at the same time is no easy task, but to Poeth, this was her calling. “Regardless of my path, I knew I wanted to be a nurse that was close to patients, sitting with them and holding their hand throughout their treatment,” said Poeth. During nursing school, Poeth completed clinicals at several hospitals in Reno – three of them were at Renown Health (known as Washoe Medical Center at the time). What immediately stood out to her was the passion of the pediatrics unit, especially in the neonatal intensive care unit (NICU). “While I knew that pediatrics wasn’t going to be my arena, some of the best times in my life were during my pediatrics clinical,” said Poeth. “It opened me up to how welcoming Renown is.” While doing her rotations, nursing leaders helped Poeth and her fellow classmates discover Renown’s Nurse Apprentice program, an apprenticeship designed exclusively for local northern Nevada nursing students. One of those leaders asked her, “have you considered doing a rotation in oncology?” And another light switch flipped. “Bingo. I am becoming an oncology nurse apprentice,” Poeth recalls. And that’s exactly what she did. After her four-month apprenticeship ended in February 2002, she walked into her interview with Joanna Gold, who would end up being her supervisor and one of her greatest mentors until she passed away in recent years. With her experience and enthusiastic spirit on her side, Poeth fervently expressed her passion and interest in working in oncology. And Joanna saw all of that and more. In June 2002, Poeth was presented with a two-year oncology RN contract, which she easily signed – however, she knew right then and there but she was not going anywhere. Renown was her home, and oncology ignited the fire within her. “The nurses in this unit are part of what kept me here,” Poeth remembers. “These nurses would really do anything for their patients. The commitment and love they all had for one another truly was like family. It inspired me to learn more and give even better care to my patients." To Poeth, it didn’t feel like she was coming to work just to do a job – she was following her dreams. “You don’t think about the work you do; you think about the service,” said Poeth. From there, Poeth spent three years on the floor as an oncology RN and became a night shift supervisor in 2005. She was thriving. But this part of her journey was only the beginning. When Opportunity Arises, Take It In March 2007, Poeth and her husband welcomed their third child – and for her, working a day shift position would serve her the best at her current stage of life. This revelation led her down to Renown South Meadows Medical Center, where she became a staff nurse in Medical Telemetry. It was in the telemetry unit where Poeth contributed to one of the largest digital transformations Renown would ever go through: transitioning from paper records to electronic records on EPIC. From there, Poeth was inspired to get back into leadership in 2012 as the Supervisor of Clinical Nursing overseeing nurses, clinical outcomes and payroll in the medical/telemetry unit and intensive care unit (ICU). The timing of her leadership role lined up perfectly with her decision to take her skills to the next level, achieving a bachelor’s degree from Nevada State College in 2016. The timing of her degree lined up perfectly with what was about to come; she embarked on her first leadership role at Renown This is where she would happily stay for 11 years, eventually becoming the Manager of Nursing in telemetry and the ICU, noting that Renown South Meadows felt like a second home to her. “I wore many hats at South Meadows,” Poeth recalls. “From piloting back coding and handling compliance work to being on the patient floor and heading up South Meadows’ first high school hospital volunteer program, I got very involved. We had seven years without having a single nurse traveler in our unit." It wasn’t long before Poeth was inspired to expand her education even further, and she graduated in January 2018 with a master’s degree in nursing clinical leadership from Western Governors University. Thanks to Renown’s educational assistance programs, our health system invested directly in Poeth’s education with tuition reimbursement and a $1,000 nursing scholarship. Soon after celebrating her achievement, Jennifer Allen Fleiner – who was the Director of Nursing at Renown South Meadows at the time – asked Poeth yet another question that would bring her to the precipice of another career detour: “Have you ever considered transferring from South Meadows to Renown Regional?” Moments later, Alicia Glassco, Director of Nursing for Renown Regional, asked her the same question, noting that the hospital’s neurosurgery unit needed the leadership of someone just like Poeth. “It took me a whole week to make a decision, because this was one of the toughest decisions I’ve ever made in my life,” said Poeth. “I truly loved South Meadows. After that week, my leader told me, ‘you know what, Poeth? You’ve reached your pinnacle. You need and deserve a new challenge. Learn from this new team and teach them something. I think you have a huge opportunity for growth.” So, Poeth decided to apply for the position and shadow the neurosurgery team, where unlike her unit, the majority of the team at the time were travelers. But this was a challenge Poeth was up to – so she was accepted into the role. “At the end of the day, these patients deserved consistent care,” Poeth emphasized. “I knew I had to take this position for the patients – they were the ones who sold me on this job. They are the reason why we are all here. It was important for me to be an advocate for them.” The big hills to climb didn’t slow down Poeth; in fact, the exact opposite happened. Within her first year in the neurosurgery unit, her team onboarded 18 new graduates and replaced travelers. “We were hiring like crazy,” said Poeth. “My standing agenda at all section meetings focused on hiring and our quality metrics. I started having a relationship with our doctors. Once we created a strong doctor/nurse collaboration, our nurses started staying with us longer.” Everything on the unit was going great. Then, COVID-19 hit. “Since we had private patient rooms, our unit became the first COVID unit at Renown Regional,” Poeth recalls. “My whole staff that I had built up had to be distributed elsewhere. I started caring for COVID patients. We relied on our Infection Prevention team a lot. And at the same time, I was worried about my family in Africa.” Despite the stressful nature that the pandemic brought upon health systems everywhere, according to Poeth, she knew she had to continue on. “The neurosurgery team ended up merging with orthopedic trauma, which was very difficult,” said Poeth. “We went from 28 beds to 58 beds. The key to success here was training. Nurses are very resilient, and through training, we were able to stabilize the unit.” Noticing the opportunity for virtual demonstrations that were previously offered only in-person, Poeth spearheaded online trainings for nursing, physical therapy, mobility, head injuries and more, allowing teams across Renown to upskill in safe spaces. These programs continued throughout the pandemic, and Poeth was proud to be a figurehead through it all, helping to stabilize the unit while creating strong relationships with the entire team, many of whom followed her from Renown South Meadows to Renown Regional. Then, she gets another visitor – her Chief Nursing Executive – in her office with yet another opportunity. Have You Considered... In September 2022, Chief Nursing Executive Melodie Osborn walked into Poeth’s office with those three words that Poeth has heard for decades: “Have you considered...” “Before Melodie could even finish, I thought, ‘I have considered A LOT in my career!’” said Poeth. Melodie told Poeth that the William N. Pennington Cancer Institute was looking for a Director of Oncology Nursing, noting that this could be yet another growth opportunity for her and a chance for her to go back to her roots. “I had just celebrated my twentieth year at Renown; I knew this was going to be a decision I really had to think about,” said Poeth. “Everyone believed in me. Alicia Glassco told me, ‘Poeth, you are ready for this. Go for it.’ Once I applied for the position and started getting my updated chemotherapy certifications, I thought, ‘they are right; I got this.’” At this point in her career, Poeth had been hyper-focused on inpatient care, and this role would be her first time caring for patients in the outpatient setting. After going through the interview process, however, Poeth knew that this was where she was meant to be yet again – and colleagues she hadn’t seen in years reaffirmed that commitment. “I felt the most excited about the job when I toured the facility,” Poeth recalls. “I’ll never forget what one of the infusion nurses told me on my tour. She told me, ‘I don’t know if you remember me, but I remember you; I came from Renown South Meadows, and you were so nice to me as I was precepting as a new nurse. Your kindness was unforgettable to me.’ The fact that people like her wanted me in the unit so badly inspired me to come back.” Soon enough, Poeth became the Director of Oncology Nursing, a position she still proudly holds to this day. Once she was hired, she immediately went into deep learning mode, mastering skills such as revenue integrity, credentialing and the insurance process. She attributes Supervisor of Infusion Kaitlin Hildebrand and Director of Radiation Oncology Services Susan Cox for helping her succeed. Shortly after assuming the position, Poeth noticed yet another opportunity for cross-training within the organization to combat short staffing – training nurses from the Float Pool to care for patients in Infusion Services. “Between May and July of this year, we trained six nurses from Float Pool to do infusion therapy services, which offered so much relief to my team; I am so thankful to Rendee Perry, the Manager of Nursing in our Float Pool unit, and her team for their support,” said Poeth. “My mission in outpatient oncology is to serve the staff and patient population and create those strong relationships." Poeth's efforts to circumvent nurse burnout go beyond cross-training – as a director, she is always there for her team members no matter what, leading with kindness every step of the way. “I never miss a 7:45 a.m. huddle unless I am in a ‘cannot miss’ commitment; I want my employees to always know that I am there for them and that they are cared for both on and off the job,” Poeth emphasizes. “I want them to feel like they are valued, their families are valued and their mental health is valued; after all, without my team, we cannot care for patients. It’s important for them to know that I am here to be a security blanket and that there is always something we can do to solve a problem." Today, Poeth enjoys a full team of core Renown staff members whom patients look forward to seeing – and the high patient satisfaction scores to prove it. “Our team is so established that patients feel comfort in knowing they are always going to know exactly who they are being treated by,” said Poeth. “We will always work to maintain that consistency.” Staying True to the Mission Renown’s mission of making a genuine difference in the health and well-being of our community resonates closely with Poeth. Before she arrives at the infusion unit every day, she asks herself: What can I do to make it easier for my team to deliver care? “It takes a village to deliver the care we do,” said Poeth. “Our nurses are priceless. You can’t place a monetary value on dealing with life and death every day. This is what inspires me. It’s all about helping each other out and keeping those relationships strong.” Maintaining those relationships on the floor, according to Poeth, requires one main ingredient: work-life balance. “I want my nurses to be able to balance sending their kids to kindergarten and giving their patients their first chemotherapy treatments,” Poeth emphasizes. “I genuinely care about their lives. It’s nice when you get to know your team’s children, grandkids, spouse and hobbies. I’m grateful that Renown has given us the autonomy to foster that flexible environment within our teams. It is so rewarding to have such a strong impact on these employees.” To Poeth, it’s all about doing and then duplicating. Luckily for her team and infusion patients in northern Nevada, a new infusion center at Renown South Meadows is planned to open in the coming years as part of our commitment to expanding care. Her team is excited to grow their expertise down to south Reno – Poeth's original home hospital. “I strongly believe that as nurses, we are meant to be where we are meant to be at the time,” said Poeth. “Be kind to yourself and remember your ‘why.’ Take advantage of the opportunity you have.” To all nurses (and future nurses) out there, Poeth wants you to know that you are welcomed and valued. You are saving lives every day, and to her, that is worth everything. “Always remain focused, even throughout all the challenges. Never forget why you got into nursing. And lastly, always stay true to your own mission,” closes Poeth.
-
11 Tips Caregivers Need to Know
Becoming a caregiver or playing a more active role in another’s healthcare is a big responsibility. At some point, almost all adults will support an aging parent or a loved one in need. Keeping track of their needs and wellbeing, while also prioritizing your own can become overwhelming. It’s important to know: you are not alone, and help is available. Read on for 11 tips to help you manage your time, your own wellbeing and your loved one’s care. Self-care comes first. When your main priority is the person in your life who needs care, it’s easy for your own needs to take the backseat. Give yourself time each day to focus on your personal wellbeing. It’s hard to give a loved one the care they need if your own needs are not met. Prioritize the Activities of Daily Living (ADL). Make a note of what ADLs your loved one can do alone, what they need help with and what activities require the most help. This will help you work through the day with them, as well as plan out how the day’s activities will go. Do a home safety audit. Do showers, bathtubs and steps have safety grab bars? Look around the house for additional tripping hazards, like rugs or electrical cords. If your loved one struggles with day-to-day navigation of the home, consider scheduling an occupational therapy appointment. This type of therapy helps a person develop or maintain the motions required to accomplish daily tasks. You might also qualify for a referral to in-home healthcare, such as Home Care. Have the hard conversation. The best time to discuss views about end of life care and to learn what choices are available is before a life-limiting illness or crisis occurs. With advance care planning, you can help reduce the doubt and anxiety related to decision making at the end of life. Completing an Advance Directive is a great tool to sort out all these decisions before they’re needed. Attend a free workshop to learn more and complete this important document. Identify when you need respite. Respite care involves receiving a short-term break from caregiving. Organizing in-home care for your loved one will allow you to step away and tend to your needs. By identifying what kind of respite care you are seeking, you can find the right person to provide you with that much-needed break. Don’t wait until you feel overwhelmed, plan ahead. Write down insurance contact information. Have a direct connection to the right insurance professional for support and advice. If your loved one is eligible Medicare, this is a good opportunity to review their current selections and if they would benefit from a Medicare Advantage Plan or Medicare Supplement Insurance. Seeking out expert advice or information on Medicare options is a great way to navigate this. Consider calling a broker, or attend a free educational seminar with Senior Care Plus. Gather legal and financial information. Make a list of all existing legal documents and financial accounts that your loved one has. These might include a will, advance directive, power of attorney, bank accounts or investment accounts. If you have questions about how to manage them, or need assistance in setting up additional framework, reach out to a lawyer, legal service, financial adviser or bank representative. Create an inventory of medical information. Identify where all of your loved one’s medical records are, as well as a list of providers or healthcare practices where they have received care. Consider if you should have your loved one give you Proxy Access in MyChart, which allows you to access all the features in MyChart on their behalf, including viewing upcoming appointments, viewing test results and emailing a doctor on their behalf. Make a list of what others can do. Think about all the little (and big) things that need to happen, and write down tasks that others could take care of you. When someone says “let me know what I can do” you’ll be ready with a pre-written list of items they may be able to assist with. Tasks could include tackling around-the-house repairs, scheduling lawn work, helping to walk the dog, taking a car for an oil change and cleaning. Find programs and events for social enjoyment. If and when possible, seek an activity outside of the home. Look for community centers that have programs for seniors, recreational activities or meals that you can patriciate in together. If leaving the home is not an option, arrange for visits or in-home activities, such as movie nights, card games or time to visit with family. Research long-term options. If you will be considering a nursing home or assisted living, make a list of amenities that you and the person you are caring for would like. Take this list with you when visiting potential locations to make sure you don’t forget to ask about each item.
-
Ladies! Get Screened for Breast Cancer
Early detection is a significant piece of the breast cancer puzzle. Susan Cox, Renown Health Director of Cancer Operations, discusses what you need to watch for and how the latest technology can help detect potential cancer sooner. When should women start getting breast exams? It depends on risk factors: Average-risk women: Most medical organizations recommend the first mammogram between 40 and 44. Higher-risk women: Dependent on their high risk, which will dictate when they start screening, but generally around the age of 30 and not before 25 years old.
-
5 Tips for Healthy Aging
September is National Healthy Aging Month, which is described by Healthy Aging Magazine as a “month designed to focus national attention on the positive aspects of growing older.” What does healthy aging mean to you? If you're like most people, you're looking forward to removing the negative from your life – negative energy, thoughts, people and activities that don't contribute to your best life. While we remain focused on ridding ourselves of the negatives, we can forget about ways to strengthen the positive parts of our lives. Dr. Shruti Basho, a family medicine physician at Renown Health’s senior-focused medical group, provides us with five positive behaviors to focus on to improve happiness and life satisfaction. Healthy Aging in 5 Easy Steps Connect – Humans are naturally social creatures! Build connections with friends, family, colleagues and neighbors. Strong interpersonal connections help enrich your life with new experiences and opportunities. Having a support system to call upon in both times of need and times of celebration is priceless, especially as you age. Forming these bonds helps you stay healthier and happier well into your aging journey. Joining the Sterling Silver Club is a great place to meet more people in the community who want to live a healthy, fulfilled life just like you. Be Active – Regular exercise, particularly as you grow older, is vital to increase and maintain your endurance, strength and balance. But exercise doesn’t have to be a chore! Pick a physical activity that you enjoy – whether it be enjoying a nature walk, taking a power weightlifting class or anything in between. Being active will also help you build strong connections with others. If you need a workout buddy in your neighborhood, Nextdoor is a great resource to find people who live right around the block from you and may be looking for their next exercise partner. Take Notice – Curiosity and mindfulness can be an impactful motivator in positive cognition and behavior as you age. Like a child, see the wonder and beauty of the world. Notice the things around you – the weather, the landscape, the mood and the feelings of people. According to Harvard Medical School, changes in the aging brain "enable us to become better at detecting relationships between diverse sources of information, capturing the big picture, and understanding the global implications of specific issues.” By taking notice, it’s easier to learn to appreciate the things that matter. Keep Learning – Engaging with lifelong learning is one of the best ways to keep your mind active. Keep trying something new! Challenges keep you on your toes and increase your confidence and excitement in your day. Don’t know where to start? EPIC (Educational Programs Inspiring the Community) offers a diverse personal enrichment and professional development curriculum at Truckee Meadows Community College ranging from art classes to accelerated training certificate courses. Give – Be generous with your time, your knowledge and your talents by giving to friends, family and the community when you have the capacity. Lending yourself to others doesn’t have to be taxing – saying thank you and even just giving someone a smile can change the course of someone’s day. If you’re looking for a hands-on way to give back, Nevada Volunteers is a great place to find volunteer opportunities near you. Renown Health is also always looking for volunteers who are passionate about making an unforgettable difference to the people and communities we serve. Practice these five tips to improve happiness and quality of life at any age.
-
Two Years We Won't Forget: COVID-19 at Renown Health
On March 19, 2020, Renown Regional admitted the first patient in need of care while sick with COVID-19. Our providers navigated two years of a pandemic and overcame many challenges while providing the best care for our patients and the community. Anicia Beckwith’s series “The Art of Healing” captured Renown Health during this time. Let's take a look back on the last two years. February 2020: Standing Up the Hospital Incident Command System (HICS) On February 25, 2020, leaders at Renown Health stood up Renown’s Hospital Incident Command System (HICS), a standardized system used to organize response personnel and resources and manage response operations during emergencies and crises. March 2020: Temporary Deployable Medical Structure Placed Outside Renown Regional Emergency Department On March 12, 2020, Renown set up a deployable medical facility to serve as a respiratory illness screening center for emergency room patients at Renown Regional. A similar tent was also set up outside the emergency room at South Meadows Medical Center. This proactive measure helped our teams care for community members with respiratory illness symptoms while protecting patients and staff in the emergency department and other areas of the hospital. Check out photos of the tent here. Read the Reno Gazette Journal Article about the tent here. April 2020: Alternate Care Site at Mill Street Parking Structure at Renown Regional Renown’s HICS team decided to create an Alternate Care Site (ACS) in the Renown Regional Medical Center Mill Street parking structure. The ACS served additional hospitalized patients and allowed caregivers to remain on campus and still have access to existing hospital infrastructure such as lab, pharmacy, imaging, food services and other critical services. After just 10 days of construction, the ACS was completed on April 3, 2020 with space to hold up to 1,400 patients. Check out photos of the ACS under construction here. On Nov. 12, 2020, Renown opened the ACS to serve additional hospitalized patients diagnosed with COVID-19 who were clinically stable or improving. Healthcare workers at Renown cared for hundreds of patients at this site. In early Jan. 2021, the remaining patients returned home. Check out the video of Connie, a patient who received care in the ACS. April and July 2020: The LOVE Sculpture Placed at Renown Regional On April 16, 2020, during a time of darkness and uncertainty, Artown loaned Renown the LOVE sculpture, a one-ton aluminum piece of art created by artist Laura Kimpton and fabricated by Jeff Schomberg. The structure, which originally debuted at Burning Man, was lit up Renown Regional's main entrance on Mill St. Watch a video about the LOVE sculpture’s debut at Renown Regional. On July 13, 2020, thanks to the support of former board chair and community supporter Blake Smith and the Keyser Foundation, the LOVE sculpture is now a permanent fixture at Renown Health. Throughout the pandemic, it has served as a source of inspiration, hope and positivity for our community and care providers. Check out a video of the LOVE is Here to Stay celebration. June 2020: Renown Offers In-House COVID Testing In June 2020, the Renown laboratory team sprang into action to help meet the growing demand for COVID-19 testing amongst Washoe County residents and businesses. Renown invested in expanded staffing and in-house testing capabilities that ensured our teams could swab and process up to 1,000 COVID-19 tests for patients each day. All with results returning within hours. November 2020: Renown Introduces “Hospital At Home” Remote Monitoring In November 2020, six patients at Renown Regional Medical Center and Renown South Meadows Medical Center diagnosed with COVID-19 were outfitted with a remote Hospital at Home monitoring system. Renown clinicians plan to continue using this system to monitor upwards of 1,000 hospitalized patients and lower acuity patients from their homes. December 2020: Renown Administers COVID-19 Vaccines to Health Care Employees On Dec. 17, 2020, Renown began to vaccinate its healthcare workers. Among those receiving the first vaccines was Luis Martinez, a technician on Renown’s Clinical Decision Unit who cared for patients recovering from COVID-19 in the Alternate Care Site field hospital. Read the Reno Gazette Journal article about the COVID-19 vaccine rollout at Renown. January 2021: Renown Administers COVID-19 Vaccines to Community After several weeks of successful employee and volunteer drive-thru vaccination events, Renown supported the Washoe County Health District and the state in vaccinating Washoe County community members. Click here for a playlist of videos featuring Renown Health employees and patients talking about the importance of the COVID-19 vaccine. February 2021: Local Widow Inspires Renown to Change Visitor Supporter Policy Darlene Randolph’s husband Dave spent 17 days hospitalized at Renown Regional Medical Center before losing his battle with COVID-19 on December 13, 2020. Darlene wrote a passionate letter to Renown Health asking for the visitor policy that allowed patients with COVID-19 to receive visitors. In February 2021, Renown hospitals were among the first in the country to lift visitor restrictions for patients with COVID-19 to encourage families to be at the patient's bedside. Read Darlene’s full story here. May 2021: Renown Celebrates Volunteers, Partners and Community Who Aided in Vaccine Efforts In May 2021, Renown administered the last dose of COVID-19 vaccines to community members in Renown’s drive-thru clinic. Between January and May 2021, over 80,000 doses were administered at the drive-thru. View drone footage of this effort here. Click here to see pictures of vaccine volunteers and employees. November 2021: Renown Offers Vaccine for Children Ages 5+ In November 2021, Renown vaccinated children in the Reno-Sparks community with the 2-dose series in a limited round of weekend clinics. The vaccine clinics featured therapy dogs, local mascots and donuts donated by Doughboy’s Donuts. Click here to see pictures of the children’s vaccine clinics and watch a video about the clinics here.
Read More About Two Years We Won't Forget: COVID-19 at Renown Health
-
Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide
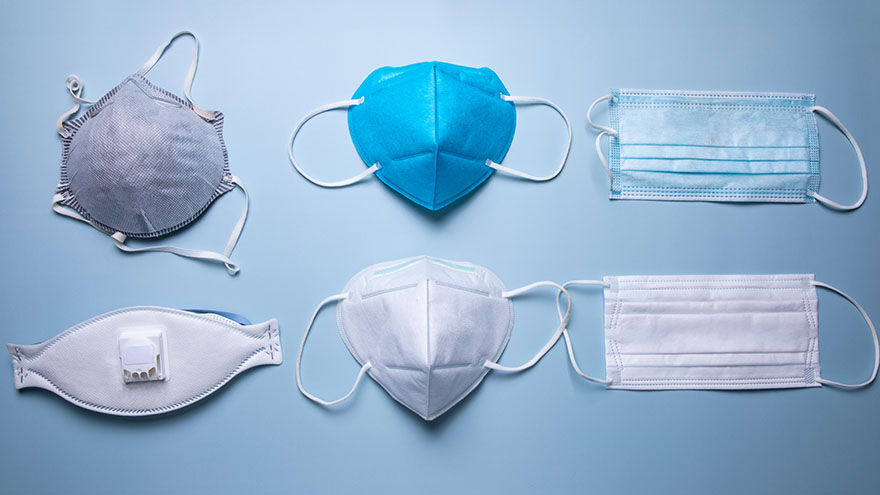
To better protect our patients, visitors and employees, cloth masks are no longer allowed at Renown facilities. Surgical masks, KN95 and N95 masks are allowed at Renown facilities. Appropriate face masks will be provided for visitors and patients who need one. With recent surges in the infectious COVID-19 omicron variant, many have sought to upgrade their face masks. But, let’s face it, shopping for face masks with adequate protection can be a challenge, especially considering the countless variations and the rise of counterfeit masks. Follow our straightforward guide below which includes some common red flags to help you discern between a high-quality face mask that provides proper protection and those that may be counterfeit. Types of Masks Qualities of a Real N95 Respirator Mask According to the National Institute for Occupational Safety and Health (NIOSH), N95 approved masks form a tight seal around your face and include a disposable respirator that removes particles including bacteria, viruses and dust as you breathe. N95 masks that are NIOSH approved undergo strict quality assurance and performance requirements to ensure mask respirators filter out up to 95% of hazardous particles. As a rule of thumb, N95 masks will not have ear loops, commonly used in cloth or surgical face masks. N95 respirators will contain two elastic bands or head straps that fasten behind the head, one securing the crown of the head and the other resting at the base of the neck, providing a snug fit and seal. Some other common signs that an N95 might be counterfeit include lack of all proper labeling, misspellings of NIOSH, decorative fabric and claiming to be approved for children. Currently, masks in adult sizes are the only masks to undergo NIOSH’s quality assurance and testing process. Respirators approved by NIOSH will include a testing certification (TC) approval number and will contain specific labeling on the facepiece of your mask. Find a full list of Center for Disease Control (CDC) and NIOSH requirements here. Identifying Real KN95 Respirator Masks Often preferred due to comfortability, the KN95 respirators were initially designed to meet Chinese standards for medical masks. Firstly, if a KN95 mask claims to be approved by the CDC, it is counterfeit as the CDC and NIOSH do not support any respiratory protective devices according to international standards. However, when KN95 masks are fitted and worn appropriately they do provide more protection than disposable masks. Legitimate KN95 masks will display a manufacturer number, GB2626-2019, ensuring accordance with current Chinese respirator standards for all masks made after July 1, 2021. Unlike N95 masks, it is important to note that KN95 masks are available in children's sizes. You might run into KN95 masks claiming to be “FDA (Food and Drug Administration) approved” or “FDA-registered,” but be aware that this does not mean much and is a misleading statement. What this indicates is that a mask maker has submitted paperwork to the FDA, but the product has not been thoroughly tested for proper filtration and protection. Surgical Masks Medical procedure masks often referred to as surgical or disposable masks vary in their protection according to a variety of factors including fit and filtration. The CDC defines medical procedure masks as “variably shaped, including flat pleated, cone-shaped, or duck-bill. Medical procedure masks are loose and are not expected to provide a reliable level of protection against airborne or aerosolized particles as N95 respirators regulated by the National Institute of for Occupational Safety and Health.” However, these types of masks provide more protection than cloth masks and are certainly better than wearing no mask at all. Often popular due to their level of comfort and cost-effectiveness, surgical masks can be knotted in the ear loop areas to provide a tighter seal and can be layered for additional filtration. Depending upon your budget and level of comfortability and protection, one variation of mask may suit you over another. Please remember to do your part in limiting the spread of COVID-19 and wear a surgical mask, KN95 or N95 mask when visiting Renown facilities.
Read More About Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide
-
COVID-19 Booster Shots, What You Need to Know
Getting the COVID-19 booster is the best way to protect yourself from severe illness or death due to COVID-19, and both the CDC and the FDA have approved booster shots for people ages 18 and older. So, with the holidays right around the corner and infection rates on the rise both in Nevada and nationally, the best thing you can do to prevent the continued spread of this deadly virus is to get boosted today. The Basics: Who: It is recommended that everyone 18 years or older get a COVID-19 booster shot. When: At least 6 months after completing your primary COVID-19 vaccination series. What: Any of the COVID-19 vaccines authorized in the United States. The CDC allows for mix and match dosing for booster shots. How: To make an appointment for your COVID-19 vaccine booster, please visit vaccines.gov today. Appointment Reminders: Don’t forget to bring your CDC vaccination record card to your appointment. Refresh yourself on the potential side effects and remember that these are normal signs your body is building up protection. Commonly Asked Questions: Q: Does anything change if I received the Johnson & Johnson as my first COVID-19 vaccine? A: If you received the Johnson & Johnson COVID-19 vaccine, you are elidable for a booster two months after completing your primary vaccine. Q: Is the formula the same for the boosters as it was for the primary vaccine? A: COVID-19 booster shots are the same formulation as the current COVID-19 vaccines. However, in the case of the Moderna COVID-19 vaccine booster shot, it is half the dose of the vaccine people get for their primary series. Q: Am I still considered “fully vaccinated” if I don’t receive a COVID-19 booster shot. A: Yes, everyone is still considered fully vaccinated two weeks after their second dose in a two-shot series, such as the Pfizer-BioNTech or Moderna vaccines, or two weeks after a single-dose vaccine, such as the J&J/Janssen vaccine. All information courtesy of the Center for Disease Control and Prevention. All information courtesy of the Center for Disease Control and Prevention
Read More About COVID-19 Booster Shots, What You Need to Know