Search
-
Department Spotlight: Surgery & Procedure Scheduling
When it comes to intimidating procedures such as surgery, cardiac catheterization (Cath) or interventional radiology (IR), there can be a lot of unknowns. What can I expect on the big day? What will happen after I’m all done? Will I have to worry about my orders not being in the system? Who can I call if I have any last-minute questions? It’s easy for your thoughts to race as you approach your procedure date, but luckily, there is a team who puts your mind at ease. With Renown Health’s Surgery & Procedure Scheduling department, patients can breathe a sigh of relief knowing that all the nitty-gritty is taken care of before they step foot in the procedure room. This team operates in the mindset of a complex Tetris board – fitting in all the pieces to make sure every patient is set on the path for surgery success. Consistent Contact Our Surgery & Procedure Scheduling team has a unique history. Initially operating as two separate teams, over the last year, our leaders skillfully combined the two teams together under one umbrella. That allows the now singular team to have line of sight across every surgery and Cath or IR procedure plan and be better stewards of the resources they have at their fingertips to provide streamlined, more-connected care for patients. As one might imagine, with the merger of the two teams, the day-in-the-life of each team member is full of a variety of crucial checklist items to cross off – all supporting constant communication from patients to providers. On the surgery scheduling front, these team members are resource rockstars. From working with referring providers to get patients scheduled appropriately to ensuring rooms and equipment are available for every patient, this team makes sure everything and everyone is in place when the time comes to help create a successful procedure and the best possible patient experience. “In surgery scheduling, we handle inbound calls for the outside offices to get time scheduled for each patient in the operating room (OR),” said Lydia Sharkey, Senior Scheduler. “We make sure there are plenty of anesthesia resources and equipment for every surgery, including any important information that we need to schedule patients appropriately and adding all documents to the OR board. If we need to swap rooms or move patients around, we handle that process too.” Over on the IR/Cath scheduling side of things, this team is on the frontlines of patient communication. They are experts in helping patients navigate their procedure from start (seeing their provider and obtaining the proper referrals) to finish (the day of the procedure and post-procedure process). “My day is a little different than the hospital schedulers; our part of the team handles the outpatient aspect,” said Adrienne White, Senior Scheduler. “We are in constant contact with patients and the IR and Cath departments. We help them navigate their procedure, including what to expect during and after the procedure. We get them through the process as easily as possible and ease their minds, so they know what is going to happen every step of the way. It’s all about communication, communication, communication!” This department has a significant overarching role: make sure all documents and ancillary information is set up for all our clinical teams that help with surgeries and procedures. This critical work means that every process is followed, and no important details are left out. “No one wakes up and says, ‘I want to have surgery;” our team goes above and beyond to make sure every single detail is taken care of so that when patients arrive, everything is in place,” said Trisha White. “Our team works hard to ensure everything runs as efficiently as possible because we want to use our resources in the best way possible to serve our patients without delays. We make sure we receive all the orders, codes and insurance and that the teams that follow after us – including our pre-admit team and nurses – have all the information they need to do their job seamlessly." With all the work they accomplish daily – not to mention how they wholeheartedly support each other through it all – it’s no question that the entire team has a lot to be proud of. Besides helping make patient care possible, the team puts their departmental merger and the move to fully remote work at the top of the list. “We’re most proud of merging the surgery scheduling and procedure scheduling teams together and therefore more cohesive,” said Mary Gray, Senior Scheduler. “The merger has made our team blossom and be able to connect with and rely on one another even more. We aren’t afraid to speak up and say something. At the end of the day, we’re here to take care of the patient, but we also help each other out. Our morale has gone up, and everybody is happier. Even though we all work remotely, we are more connected and have a great work-life balance.” “Along with transitioning the two teams into one big team, the move to being fully remote was huge," added Patricia Cruz-Hernandez, Surgical RN Scheduling Coordinator. “We worked through all the glitches, and it was a seamless transition to move into a remote setting. What’s great is that it did not affect patients at all; everything still gets done exactly as it should.” No matter how busy the days may get, Renown’s surgery and procedure schedulers always remember one thing: they are incredibly grateful for their fellow team members. “We have a very efficient and hard-working team of women,” said Pam Chapa Valencia, Senior Scheduler. “I could not have handpicked better people for our team,” added Trisha White. “I feel so lucky to have the team that we have.” A Renown “Why” Our Surgery and Procedure Scheduling team members all have diverse stories to tell about their road to Renown and why they’ve stayed in the department for as long as they have. Whether they’ve been with us for two years or two decades, they all share the same strong calling to care for their community. “I always wanted to help people, and my grandma was a nurse,” said Pam Chapa Valencia, Senior Scheduler. “I loved hearing her stories, and it made me want to be involved in patient care.” “I have a caring nature, and a hospital nature seemed like the right fit – I've been here for 25 years,” added Mary Gray. Several of our schedulers recognized the influence Renown has within our community and the ability to grow professionally and personally, both of which were a driving factor in their decision to make our health system their long-term career. “I’m originally from southern California, and I moved here about eight years ago; my husband always talked so positively about Renown, especially with how big it is and how it has the only level II trauma center in northern Nevada, so my goal was always to get a job here,” said Lydia Sharkey. “It’s been a great environment to be a part of.” “I’ve been with Renown for 17 years, and I chose to come here because of the reputation of the services Renown provided and care they gave,” added Trisha White. “I also knew what opportunities there were for me professionally, and in doing so, we are taking care of our community. I’ve had the chance to grow within my own professional skills and leadership skillset.” A profound feeling of ‘home’ is a common theme among this department. These team members appreciate the sense of community Renown has, the strides we’ve made in expanding our reach and how our health system gives healthcare professionals who are new to the field a chance to succeed. “At the time, Renown was the only hospital that would train nurses, and as a brand-new nurse, I had no experience – Renown took a chance on me,” said Patricia Cruz-Hernandez. “I feel like this is home. Our health system is so community-based and people-first minded, keeping ‘mission over margin.’ We’re growing, we’re expanding, we’re everywhere!” “I was a part of a transition as the cardiology private practice I worked with became a Renown practice, and it was great,” added Adrienne White. “This transition enabled us to provide more services and better care to patients. I stay here because I see the leaps and bounds we’ve been able to make in terms of procedures, accessibility and patient experience.” As true advocates for both patients and each other, the team is proud to have found their niche – and the ultimate beneficiaries? Everyone undergoing a surgery or procedure at Renown. A Culture of Kindness and Gratitude When you meet the Surgery & Procedure Scheduling team, you are greeted with warm smiles and an enthusiastic “Nice to meet you!” You can’t help but smile back and feel the infectious kindness they exude. Renown operates with a People-First mindset, a vision that this department especially takes to heart. They emulate the exact definition of our “Collaboration” cultural commitment. “We’ve built very good relationships and rapport with the OR managers and board runners,” said Lydia Sharkey. “The communication that we have at all three locations is very solid.” “The OR leadership is always so willing to help out whenever they can, and the resources they’ve provided have been huge for us,” added Adrienne White. “All the teams that see the patients after us – especially the surgical pre-admit team and the case managers, are fantastic about collaborating with us and reaching out to solve any issues they may have,” added Trisha White. “We all work so well together, especially since we all impact patient care.” In any organization, strong and compassionate leadership is key to a thriving team. Luckily for our surgery and procedure schedulers, they have Trisha White on their side. They attribute a lot of their success to having a supportive leader who “gets it.” “Trisha has been a scheduler like us, so she completely understands when we’re having an issue, because she’s struggled with the same thing and knows where we are coming from,” said Mary Gray. “It makes us feel like we are not alone – I can always reach out to her, or any of my other coworkers, to ask questions and figure out a solution together.” Despite being a remote-only team that meets in-person only one or two times a month, this group never misses an opportunity to reconnect both online and offline. They frequently shout out their Culture Ambassadors, schedulers Pam Chapa Valencia and Roxanne Abundis, for their team’s high morale. “Even though we all primarily work remotely, our in-person days are some of my favorite days of the month,” said Trisha White. “We feel so uplifted, we laugh and we have fun. We love being with each other. Pam and Roxanne are our Culture Ambassadors, and they both have been amazing at planning fun things for our teams. They go above and beyond to make our team feel cohesive and included.” “Pam and Roxanne have been leaders in creating a fun environment and supportive culture for us,” added Lydia Sharkey. “Whether it’s creating care packages or making sure we all have a good time when we see each other in person, they deserve a lot of credit.” As this team excels in their roles and foster a culture rooted in kindness and gratitude, we can trust that Renown’s surgeries and procedures will continue to thrive, and patients will continue to benefit from their diligent efforts and commitment to efficiency. “We make the magic happen!” closes Mary Gray.
Read More About Department Spotlight: Surgery & Procedure Scheduling
-
Make Your Own Trail Mix: 4 Quick and Easy Recipes
Craving a crunchy, sweet, and nutritious snack? Try making your own trail mix! Perfect blends of nuts, dried fruits, and a touch of chocolate can be whipped up using bulk bin ingredients or pantry staples. Enjoy this delicious, healthy snack on a hike, at the office, or on your next road trip through Nevada's scenic deserts.
Read More About Make Your Own Trail Mix: 4 Quick and Easy Recipes
-
Healthy Potato Salad A Creamy Dreamy and Light Picnic Favorite
Potato salad is the superstar of summer picnics, a delightful sidekick at backyard BBQs, and a tasty everyday treat! Our friends at Renown's Health Improvement Programs whipped up a fabulous, health-conscious version that doesn't skimp on the creamy dreaminess we crave. This salad features purple potatoes for a dash of delightful color. It's also easy to make, with protein-rich Greek yogurt and egg whites. This simple but classic dish will indeed become your circle's new favorite—talk about a tasty transformation!
Read More About Healthy Potato Salad A Creamy Dreamy and Light Picnic Favorite
-
What is Polycystic Ovary Syndrome (PCOS)?
Dr. Carilyn Hoffman with Renown's Women's Health explains the symptoms, causes and treatments of Polycystic Ovary Syndrome (PCOS) (also referred to as Polycystic Ovarian Disease (PCOD)), a prevalent condition among women of reproductive age that influences hormonal balance, metabolism and fertility. Make an appointment with Renown Women's Health Click here to schedule Call to schedule: 775-982-5000 PCOS Defined PCOS is a constellation of symptoms characterized by two of the three criteria: multiple small cysts on the ovaries visible via ultrasound, irregular periods and signs of hyperandrogenism. Other symptoms include infertility, insulin resistance, and increased risk of cardiovascular disease. Symptoms of PCOS The symptoms of PCOS can vary from woman to woman, but some of the most common include: Irregular menstrual cycles: This is often one of the first signs of PCOS. Women may experience fewer than nine periods a year, more than 35 days between periods, frequent spotting, and/or abnormally heavy periods. Excess androgen levels: High levels of male hormones may result in physical signs such as excess facial and body hair (hirsutism), severe acne and male-pattern baldness. Polycystic ovaries: Enlarged ovaries containing numerous small cysts can be detected via ultrasound. Causes and Risk Factors The exact cause of PCOS is unknown, but several factors may play a role: Genetic predisposition: A family history of PCOS increases the risk. Insulin resistance: High insulin levels might increase androgen production, causing difficulty with ovulation. Obesity: Women with elevated BMI’s are more likely to have PCOS, although 20% of women with PCOS are not obese. Diagnosis and Treatment Dr. Hoffman outlines that diagnosing PCOS requires a medical history review, a physical exam, blood work and an ultrasound to evaluate the ovaries. Treatment options can range from lifestyle modifications, like diet and exercise and weight loss, to medications for menstrual regulation, fertility assistance, and rarely surgery. Lifestyle Changes A healthy lifestyle is a cornerstone of managing PCOS. Regular exercise, a nutritious diet, and weight management can help reduce symptoms and the risk of long-term health issues. In overweight patients, weight loss as little as 5% has been shown to improve symptoms of PCOS. Medication Medications may include hormonal contraceptives to regulate menstrual cycles, anti-androgens to reduce hair growth and acne, and Metformin to address insulin resistance. Fertility Treatment For women with PCOS who are trying to conceive, ovulation induction with clomiphene or letrozole is sometimes necessary. Sometimes a referral to a reproductive endocrinologist and infertility specialist is needed for more advanced technologies like IVF. Health Implications PCOS is not just about cystic ovaries or irregular periods; it can have profound implications on a woman's overall health. Women with PCOS are at an increased risk for several conditions, including type 2 diabetes, high blood pressure, heart disease, and endometrial cancer.
-
Perfect Peanut Butter and Pumpkin Puppy Treats
This holiday season, sprinkle some extra joy for your favorite furry pals by whipping up these easy, AKC-approved dog treats. With simple ingredients and quick baking times, they're the perfect last-minute surprise to show your pet some love. Turn it into a delightful gift by snagging some adorable, budget-friendly canisters (easily found at dollar or thrift stores) and fill them to the brim with these homemade goodies. It's a merry, tail-wagging gift that's sure to make this season the most pet-friendly one yet! 🎄🐾🍪
Read More About Perfect Peanut Butter and Pumpkin Puppy Treats
-
Strategies for Lasting Weight Loss
Managing weight is a complicated and often difficult journey for many individuals, and obesity stands as a common and serious chronic health condition. In fact, the Center for Disease Control and Prevention reports that the prevalence of obesity in the US is greater than 40% in adults and 20% in children, and those numbers are continuing to climb. In Nevada, according to the 2020 Behavioral Risk Factor Surveillance System, 28.7% of adults reported being obese. By 2030, almost 80% of American adults may be overweight and half of them will be obese. But obesity isn't just about the numbers on the scale; it's a multifaceted, lifelong, neurobehavioral disease triggered by a combination of factors. These include abnormal eating patterns, reduced physical activity levels, environmental stressors, genetics and various other contributors. Obesity extends far beyond appearance, often leading to the development of numerous medical conditions such as diabetes, heart disease, elevated blood pressure, stroke, sleep apnea, liver disease, various cancers and infertility. Join us as we delve into the complexities of obesity and explore strategies for effective weight management available right here in northern Nevada. Why Can Losing Weight be so Difficult? The challenge behind weight loss finds its roots in the Set-Point Theory of Obesity, a concept that says our bodies have a predetermined weight, or fat mass, within a defined set-point range. In other words, when an individual's weight deviates from this set point, the body initiates mechanisms to bring it back to the established range. So, if someone loses weight below their set point, the body may respond by increasing hunger and reducing metabolism, making it challenging to sustain weight loss. There Isn’t One Right Answer, But Renown is Here to Help Various weight management strategies can be utilized by patients struggling with obesity, which may lead to substantial weight loss, resolution of associated medical conditions and improved psychosocial health. In fact, the most successful strategy involves a multidisciplinary approach under the guidance of trained specialists that includes a combination of tactics, including: Behavioral adaptations Dietary modifications Physical exercise Anti-obesity medications Weight loss surgery
-
Cranberry-Jalapeño Cream Cheese Dip
Add a dash of holiday cheer to your gatherings with this vibrant Cranberry-Jalapeño Cream Cheese Dip. Its festive red and green hues perfectly capture the spirit of the season, while the delightful blend of sweet, spicy, tart, and creamy flavors is sure to delight and tantalize your guests' palates. Simple to prepare, this appetizer is an irresistible addition to any holiday feast!
-
Mysterious Mummy Hot Dogs
This easy, kid-friendly recipe just might be the perfect pre-trick-or-treating meal that will vanish before your eyes! Serve with veggie sticks and mustard and ketchup for dipping. Several healthy hot dog options, such as vegan, turkey and chicken, are available in most grocery or health food stores.
-
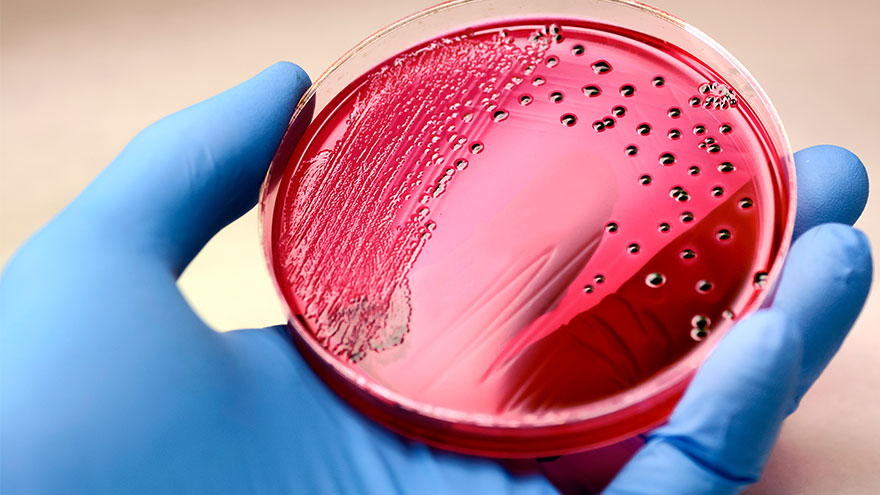
Sepsis: Causes & Symptoms
According to the Global Sepsis Alliance, 1 in 5 deaths worldwide are associated with sepsis. If not recognized early and treated promptly, sepsis is the final common pathway to death from most infectious diseases worldwide, including viruses such as COVID-19. We spoke with Jeremy Gonda, MD, a critical care physician from Renown Health’s Sepsis Committee to increase public awareness of this preventable medical emergency. What is sepsis? Sepsis is a response to infection—bacterial, viral or fungal—and can start anywhere in the body and spread into the bloodstream. The body is trying so hard to fight an infection that it begins releasing chemicals into the bloodstream that cause inflammation and the shutdown of multiple organ systems. “It carries a very poor prognosis in general unless you catch and treat it very early,” said Dr. Gonda. “Any infection can lead to sepsis. Typically your immune system takes care of the infection. It doesn’t progress, but in cases where the infection becomes severe, or the immune system doesn’t function properly, people can certainly die. So there’s, unfortunately, a very high mortality rate associated with sepsis.” According to the Centers for Disease Control and Prevention, each year at least 1.7 million adults in America develop sepsis. While you can recover from sepsis if caught early, many sepsis survivors suffer from long-term physical and psychological effects. What are the signs of sepsis? One way to spot sepsis is to use the acronym SEPSIS: S – Slurred speech and confusion E – Extreme shivering or muscle pain/fever P – Passing no urine all day S – Severe breathlessness I – “I feel like I might die” S – Skin mottled or discolored Keep in mind that sepsis symptoms can vary depending on where the infection starts. “Patients may experience urinary burning if they have a urinary tract infection or a cough and shortness of breath if they have pneumonia first,” said Dr. Gonda. “However, often symptoms are more generalized or subtle such as fevers, confusion and malaise.” How do you develop sepsis? When germs enter your body, they can cause an infection. If you don’t stop that infection, it can cause sepsis. Areas of infection that more commonly result in sepsis include: Lungs, such as pneumonia Kidney, bladder and other parts of the urinary system Digestive system Bloodstream (bacteremia) Catheter sites Wounds or burns Who is most at risk? People with compromised immune systems are at greater risk for sepsis, such as “The very young, the elderly and any people who may have conditions that suppress your immune system,” said Dr. Gonda. “For instance, if you have diabetes or if you’re an organ transplant patient who is on immunosuppressant therapy, you’re at somewhat higher risk.” Sepsis is often considered a hospital-acquired infection, but a study in The Journal of American Medical Association found that 80% of sepsis cases occur outside of a hospital. That’s why it’s especially important to remember any infection can lead to sepsis, and anyone can develop sepsis from an infection. What do I do? Timing is critical in the case of sepsis and septic shock. According to a study on septic shock patients, there is a 7.6 percent decrease in survival for each hour treatment is delayed. On the other end, if treatment is given within an hour of the first drop in blood pressure, the survival rate is 80 percent. Because sepsis can be so deadly, it’s important to seek medical attention as soon as possible. “If you’re not getting any better, if you think symptoms are progressively worsening – you should definitely be evaluated by a doctor,” said Dr. Gonda. You can help #StopSepsis by getting involved at worldsepsisday.org.
-
Importance of Safe Sleep
In today's fast-paced society, it is understandable for parents to want to take shortcuts in caring for their little ones. A s a result, It is tempting to leave a sleeping infant in a car seat or swing after a long day of errands or when you need a moment to catch your breath. But, as convenient as these devices may be, they pose a serious risk to your child's safety. Why Car Seats and Swings Pose Risks for Infant Sleep Car seats, swings, and bouncers are quick and convenient ways to feed, hold, and sleep an infant. Not out of malice or discontent, but again from the need for quick and easy access to baby care in an already busy lifestyle. However, the risks outweigh the benefits. The American Academy of Pediatrics (AAP) states that “infants should be moved to a crib, bassinet, or play yard for sleeping as soon as is practical.” If a parent must use a car seat or other sitting device, they should only do so for a short period of time and never as a substitute for a proper sleeping environment. Leaving a sleeping infant in a sitting device, such as a car seat or swing, can create unsafe sleeping conditions. The American Academy of Pediatrics (AAP) warns that doing so increases the risk of sudden infant death syndrome (SIDS) and positional asphyxia. This is because infants can easily slump over or become entangled in the straps, blocking their airway, and causing suffocation. Car seats, swings, and bouncers are quick and convenient ways to feed, hold, and sleep an infant. Not out of malice or discontent, but again from the need for quick and easy access to baby care in an already busy lifestyle. However, the risks outweigh the benefits. The AAP states: Infants should be moved to a crib, bassinet, or play yard for sleeping as soon as is practical. If a parent must use a car seat or other sitting device, they should only do so for a short period and never as a substitute for a proper sleeping environment. Leaving a sleeping infant in a sitting device, such as a car seat or swing, can create unsafe sleeping conditions. The AAP warns that doing so increases the risk of sudden infant death syndrome (SIDS) and positional asphyxia. In addition, infants can easily slump over or become entangled in the straps, blocking their airways and causing suffocation.
-
What Does a Doula Do?
If you’re expecting a new baby, you may have been given the advice to hire a doula. You may have seen statistics of improved outcomes among those who’ve had a doula attend their birth. Perhaps you’ve heard that the etymology is from the Greek word meaning “to serve.” But how does a doula serve their clients? A doula is a non-medical birth professional who will guide you through labor, birth, postpartum and beyond. Your doula can discuss your options with you so you can make informed decisions, as well as provide emotional and physical support to ease your experience. While each doula offers their own style, there are certain services that most doulas will provide for their clients. Typically, a birth doula will provide at least one prenatal visit, one postpartum visit and continuous support during active labor. A postpartum doula usually provides support during the 12 weeks immediately following birth, sometimes referred to as the “fourth trimester,” but some will continue care after that as well. Simply put, a doula provides informational, physical and emotional support during the childbearing year(s). Let’s take a closer look at these three ways a doula can support you. The Basics If you don’t know your options, you don’t have any. This is a common phrase in the world of birth work. When you’re in labor, you’re exhausted, in pain and there’s often urgency inherent or implied in any choices you make. So, when an intervention is offered, many birthing people accept it without question. One method that can help the decision-making process is to check your BRAIN: Benefits: What are the benefits of the proposed intervention? Risks: What are the risks of the proposed intervention? Alternatives: What are the alternative options? Intuition: What does your intuition tell you? Nothing: What if we do nothing? What if we wait? When you’re in active labor, you might have difficulty remembering this acronym; that’s where your doula comes in. At your prenatal visits, you can ask your doula for guidance in preparing your birth plan, which can include contingencies for certain potential interventions. And as choices arise during labor, your doula can guide you through the benefits and risks and can provide you with alternative options you might not otherwise be aware of that are available to you. Your doula can remind you to check in with your intuition and can help you quiet your mind so you can listen to your instincts. The Body Although we tend to see depictions of people giving birth on their backs with their feet in stirrups, this is only one of many ways to give birth. Walking and dancing can speed up early labor. Side-lying or hands-and-knees can prevent tearing during the pushing stage. Sometimes labor stalls, and a change of position is often helpful to get things moving again. Your doula can suggest positions depending on your stage of labor. Some labor positions might require the support of another person – your doula could fill this role or assist your partner in doing so. Some doulas also provide massage or even acupressure, and most will do the “hip squeeze” that so many laboring people swear by. If your baby is presenting posterior, or “sunny side up,” your doula can apply counter pressure to alleviate back pain during labor. Some postpartum doulas will do light housework while you rest and bond with your newborn. Others might care for your baby through the night so you can catch up on sleep. Many doulas have also gone through additional training to offer breastfeeding support and may be able to assist you with latch issues and nursing positions. The Mind Pregnancy, birth and postpartum periods can be some of the most emotional times in a person’s life. A doula will hold space for you and help you process your emotions before and after birth. It’s normal to feel apprehensive, or even fearful, about labor and birth, and discussing these feelings is the first step. A doula can help you navigate your concerns in a safe space so you can be prepared emotionally for your upcoming labor. Many doulas will also guide you through writing your birth plan, which can lessen anxiety about the unknown. If you have a history of trauma, your doula can assist in communicating this, so you don’t have to relive the experience every time you meet a new medical provider. Most people will experience some form of what’s often called the Baby Blues in the immediate postpartum period. The third day after birth tends to hit hard, as hormones attempt to regulate, but the Baby Blues can continue for weeks for some new parents. A postpartum doula’s support can be incredibly valuable during this time. When the baby blues last longer than a few weeks, it could considered a mood disorder. Most doulas will recognize signs of postpartum mood disorders and will have resources available for additional support. Choosing the Best Doula for You With so many wonderful doulas in northern Nevada, you might wonder how you could ever choose just one to attend your birth. Some expectant parents are unfortunately restricted by cost. With so many expenses related to a new baby, it can be difficult to budget doula services as well. Thankfully, Nevada Medicaid now covers doula care, and some commercial insurances are following suit. Check with your insurance company to find out if they might cover part of the cost for hiring a doula. If your insurance doesn’t cover doula services, some doulas offer a sliding scale based on income. You may want to interview multiple doulas to find the right one for you. If you’re the kind of person who wants all the information you can get, a more detail-oriented doula might be the best choice. But if you tend to feel overwhelmed by too many options, you might prefer a doula who only offers additional information as the situation calls for it. If you want massage or acupressure during labor, you might want to hire a doula with those certifications. Or maybe informational and physical support are not as important to you as emotional support, in which case your best choice could be a doula who has experience with postpartum mood disorders or trauma support. Regardless of who you hire, be sure to clearly communicate your desires and expectations – not just for your birth, but also for your doula. The most important thing when choosing your doula is trusting your gut. You need to feel comfortable with your doula, as they’ll be tending to you at one of the most vulnerable times in your life. When you find a doula that you click with, who listens to you and supports your choices, you have found the best doula for you.
-
A Fighting Chance at 24 Weeks Sloans Story
Most babies weigh just one pound and are roughly the size of an eggplant when they reach 24 weeks of development inside the womb. It is a crucial stage when internal organs begin functioning, and the babies' respiratory and central nervous systems are still developing. So, in November 2021 when Kallie Johnson experienced a premature rupture of amniotic fluid around this point in her pregnancy, her care team in Winnemucca decided to transport her via Care Flight to Renown Regional Medical Center. The team at Renown Children’s Hospital immediately began discussing the risks of delivering at 24 weeks with the Johnson family. Moving Forward with Hope Knowing the stakes, Kallie remembers never feeling rushed to decide about delivering her baby preterm. “I felt educated and supported by my care team at Renown throughout our entire stay, starting with the education they provided about what it meant to deliver my baby early,” Kallie said. “The team really helped me make the best decision for myself and my family.” Together, Renown employees and the Johnson family moved forward with a healthy set of nerves and a powerful feeling of hope. Weighing in at one pound 11 ounces, Sloan entered the world on Nov. 19, 2021, via emergency Cesarean section. Her birth was classified as a micro preemie because she was born before week 26 of pregnancy and so small that she fit inside the palm of her father Sterling’s hand. A full-term pregnancy is classified as reaching 39 weeks. A Fighting Chance Called a fighter by many Renown Children’s Hospital care team members, Sloan spent over five months in the neonatal intensive care unit (NICU). She was placed on a ventilator, fed through a feeding tube and monitored 24/7, overcoming daily challenges with the Renown team and her family. As a result of being born prematurely, Sloan developed a grade one brain bleed and a congenital heart defect called patent ductus arteriosus, a persistent opening between two major blood vessels, causing too much blood to flow to the lungs and heart. To meet the oxygen needs of her tiny lungs, Sloan was intubated and developed a severe oral aversion and high-arched palate as a result. The effects would lead to difficult developmental and physical challenges that she still conquers today. Yet, with the help of her care team – including physical, occupational and speech therapists, dieticians and doctors – Sloan continues to make progress every day.