Search
-
What You Need To Know About Cold Water Drowning
Northern Nevada's stunning lakes, including Lake Tahoe, with its average summer water temperature of 50 degrees, present a potential risk of hypothermia. Unlike mild 50-degree air, water at the same temperature poses severe, life-threatening risks, including rapid-onset hypothermia and drowning. Awareness of the symptoms and taking proper precautions are crucial to prevent cold-water drowning. The 4 Phases of Cold-Water Drowning 1. Cold Shock Response: This response affects breathing and happens within the first minute. An automatic gasp reflex occurs in response to rapid skin cooling. If the head goes below water, water may be breathed into the lungs, resulting in drowning. A life jacket will help keep your head above water during this critical phase. Additionally, hyperventilation, like the gasp reflex, is a response to the cold and will subside. Panic will make this worse, so the key is to control breathing. 2. Cold Incapacitation: This response occurs within the first five to 15 minutes in cold water. In order to preserve core heat, vasoconstriction takes place decreasing blood flow to the extremities to protect the vital organs. The result is a loss of movement to hands, feet, arms and legs. Unless a life jacket is being worn, the ability to stay afloat is next to impossible. 3. Hypothermia: Important to note, it can take 30 minutes or more for most adults to become hypothermic. So there’s time to take action and survive. Keeping panic at bay is critical, as you have more survival time than you think. Symptoms include: Shivering Slow and shallow breathing Confusion Drowsiness or exhaustion Slurred speech Loss of coordination Weak pulse 4. Circum-rescue Collapse: This experience can happen just before rescue and is not well understood. Symptoms range anywhere from fainting to death. Some experts believe an abrupt drop in blood pressure may cause this final stage of cold water drowning, post-rescue. Additional Safety Tips and Helpful Resources Always wear a personal flotation device as well as a wetsuit or drysuit. Your personal flotation device is the most important piece of water safety gear. Try not to panic as the first phases will subside. Controlled breathing is to staying calm. Research suggests the body can withstand the cold longer than we think. The Heat Escape Lessening Posture (HELP) is a position which helps conserve energy if you’re wearing a personal flotation device. By hugging your knees to your chest, this posture helps maintain body heat for some time.
Read More About What You Need To Know About Cold Water Drowning
-
What is Dry Drowning?
Whether you're a parent, grandparent, caregiver, or sibling, it's vital to recognize that drowning is the second leading cause of death among children," states Dr. Leland Sullivan, of Northern Nevada Emergency Physicians. "While we diligently work to protect children from water-related accidents, there's a lesser-known threat that often goes unnoticed—dry drowning, also known as delayed drowning. Surprisingly, many people remain unaware of its existence and potential dangers. Dry drowning defined Dry drowning is a side-effect of a near-drowning experience and includes spasms of the vocal cords and larynx — known as a laryngospasm. This occurs when the body attempts to shut down the passage of any liquid into the lungs. Unfortunately, it can also shut down the passage of air into the lungs and force fluid into the stomach and lungs. Often the condition is not discovered until it's too late — severe cases can cause death within one to 24 hours after a water incident occurs. Who is susceptible? Novice or first-time swimmers are at increased risk, as are children with asthma and known breathing issues. In addition, children who have had pneumonia or experienced acute respiratory distress syndrome are also at greater risk. To reduce these factors, caregivers should be exceptionally watchful of inexperienced swimmers. According to Dr. Sullivan, children under the age of 5 are most susceptible to drowning and often drown in residential swimming pools. Infants less than 1-year-old most often drown in bathtubs. What are the signs of a dry drowning episode? If your child has a near-drowning incident, a few moments of coughing until they calm down is normal. However, you should know the more severe signs and symptoms to watch for during the 24 hours following the incident, including: Persistent coughing Difficulty breathing and/or shortness of breath Chest pains Extreme fatigue and/or lethargy Change in typical behavior Face becomes pale What is the treatment and prognosis for dry drowning? Dr. Sullivan recommends that all victims of near-drowning incidents seek medical attention, even if they have no symptoms. If caught early, dry drowning can be treated. If you think your child is experiencing a dry drowning episode, go to the nearest emergency room as quickly as possible — do not attempt treatment at home. Healthcare professionals will work to supply oxygen to your child's lungs to restore and regulate breathing.
-
Why I Give: Tami and Richard's Story
If you have the chance to meet Tami and Richard Dethmers, you will quickly discover a remarkable couple who embody a heartwarming spirit. Married for 44 years, they cherish family above all else. With five children and 10 grandchildren, their family is not just their priority—it's their whole world. It is this love and their steadfast faith that led Tami and Richard to make a transformative donation to Renown Children’s Hospital. The Heart of Giving In 2023, Tami toured the construction of the new Wilbur D. May Neonatal Intensive Care Unit and Pediatric Intensive Care Unit at Renown Children's Hospital. She was touched by the idea of creating a special place for sick children and their families. That night, she talked with Richard about how they could help. Together, they both agreed to make a generous donation that could help ease the pain for families with children in the hospital. A Comforting Consultation Room Their donation established a consultation room in the Wilbur D. May NICU and PICU at Renown Children's Hospital. Tami and Richard's motivation stems from personal experience, having seen their grandson endure four open-heart surgeries. "I remember challenging conversations with doctors, surrounded by other families in the open PICU. It was difficult,” said Tami. In this new consultation room, families have a private space to learn about the next steps in their journey, gaining insights into the illnesses affecting their children. It is a dedicated space where doctors can discuss treatment plans and medical information with families. Designed to be a supportive and calming environment, the room features art on the walls, and a window bathes the space in beautiful, natural light, offering comfort to families in need. Tami and Richard’s donation ensures that families in the NICU and PICU can navigate difficult conversations with doctors in a thoughtfully designed space. Because We Love You and We Care In the new consultation room, a powerful message is printed and framed: 'Because we love you and we care.' This phrase is an important part of Tami and Richard’s donation, reflecting words they spoke to their children while they were growing up. For them, it symbolizes love, care, and a commitment to offering support. A Legacy of Comfort Tami and Richard, along with their family, are dedicated to an ongoing legacy of giving. Together, they also donated blankets to patients and families who use the consultation room. “I hope they provide an added layer of comfort,” said Tami. Each blanket includes a custom tag repeating those same words 'Because we love you and we care.' Richard echoes Tami's sentiments. “We do what we can because we love children, and there is no greater pain than a child in distress,” Richard said, emphasizing their shared dedication to helping children in need. Together, with their children and grandchildren, they continue to make a difference, embodying the power of compassion and generosity in their family's legacy.
-
When Care Can’t Wait: True Stories of Renown ER
Renown Health is home to three 24/7 Emergency Rooms (ERs) providing comprehensive emergency and trauma care, access to specialists and inpatient services backed by the area's most extensive health system. In 2023, Renown Health cared for 132,340 patients across three ER locations. Renown is also home to the region’s only level II trauma centers for both adult and pediatric patients. We spoke to three patients who sought immediate medical attention for various ailments and conditions to learn more about their emergency care experience and why they chose Renown ERs. Kamrin’s Story: From Worrisome to Critical In the spring of 2021, Danielle and her 13-year-old son Kamrin visited his primary care doctor for unexplained vomiting and were promptly referred to Renown Children's ER via ambulance for further evaluation and seen by board-certified emergency physician, Dr. Lisa Nelson. What initially began as an unassuming doctor's visit quickly turned into something much more severe after several tests confirmed a devastating abdominal tumor and a stage-four cancer diagnosis, unbeknownst to the family. Kamrin was immediately admitted to the Pediatric Intensive Care Unit (PICU) and referred to a Pediatric Oncologist at Renown Children’s Hospital to begin his plan of care with expert pediatric hematology and oncology specialists. Regarding the board-certified physician, who delivered the results to the family, Danielle said, “She was so calming to us, even as the diagnosis haunted us. She led us by guiding our family through the unknowns. She felt like a family member to us in that moment, letting all the unknowns be well known.” “The love, empathy, support and guidance these employees gave us carried us. The care team quickly and easily became a source of relief, knowing we were their priority and in the best hands. We are forever grateful for the team at Renown Children's Hospital and Renown Children’s ER; they truly saved our son's life and continue to be our guiding light whenever it's needed in our son’s health journey,” Danielle said. Today, Kamrin is in remission and navigating the aftereffects of chemotherapy, including an immune system deficiency. However, his family chooses to navigate each day by embracing the positive side of things, such as the life-saving impact of his treatment. Did you know? Renown Children's Pediatric Hematology and Oncology is located within Renown Regional Medical Center and offers expert pediatric specialists dedicated to providing comprehensive treatment for pediatric hematology and oncology, including chemotherapy, radiation therapy and infusion services. Taylor’s Story: From Crisis to Recovery Promptly after cosmetic surgery performed by a medical professional not associated with Renown, Taylor Salas (Chacon) began to lose consciousness and notice her post-surgery drainage systems, also known as Jackson-Pratt drains, fill with blood. She was transported to Renown Regional ER via ambulance and immediately seen by ER staff and board-certified emergency physician Thea Berning, MD, for medical assessment. Taylor drifted in and out of consciousness as the ER team began blood transfusions and a CT scan to determine her plan of care. Dr. Berning began facilitating communication with a community plastic surgeon with privileges at Renown Health and emergency surgery was performed to stop Taylor’s internal bleeding. Taylor was placed on a ventilator due to respiratory distress and trauma from the event, then transferred to Renown’s Intensive Care Unit (ICU) to continue her care. Thankfully, Taylor listened to her gut when something didn’t feel right after her surgery and sought immediate medical attention. The ER team's quick response, communication and collaboration with a plastic surgeon saved Taylor from severe internal bleeding. “I was informed every step of the way about what was happening and why. I felt comfort in this,” she said. Did you know? Because of Renown Regional Medical Center’s Level II Trauma Center distinction, you have immediate access to an extensive list of specialists and physicians trained in a wide array of specialties, in the event of a traumatic injury or accident. This is one of the many benefits of Renown Regional’s Level II Trauma status. Ted’s Story: The Unsuspected Threat Bothered by symptoms of heartburn, fatigue, neck pressure and arm discomfort, Ted was in the middle of a busy workweek in June 2023 when he began to suspect something was wrong. Knowing the importance of addressing early heart attack symptoms immediately, Ted and his wife headed to Renown Regional ER because of proximity and some familiarity with Renown’s leading cardiology care and technological expertise. After prompt assessment by the Renown ER team, including blood work, imaging tests and the administration of medication, Ted was admitted to the hospital to treat the blockage and narrowing of his coronary artery. On June 8, Ted was admitted for treatment, where he successfully underwent a single bypass surgery and recovered in the Cardiac Intensive Care Unit (CICU), before being discharged and following up with the Intensive Cardiac Rehab (ICR) program at Renown. The ICR program at Renown played a pivotal role in Ted's 55-pound weight loss and overall health improvement, empowering him to embrace a healthier lifestyle and find ways to use his newfound energy and strength today. “Overall, I believe I had the best care possible because of the collective group of people at Renown caring for this community, who we could see in the grocery store, at the ball game and in the shopping malls. This community feeling is something you might not get in a big city hospital,” Ted said. Did you know? Intensive Cardiac Rehab at Renown Health is a medically supervised program designed to improve cardiovascular health after a significant heart condition or procedure. Since its inception in 2016, this program has been a pioneer in the region for cardiac rehabilitation focusing on three key pillars including exercise, nutrition and stress management.
Read More About When Care Can’t Wait: True Stories of Renown ER
-
Department Spotlight: Facilities Engineering
When an appliance or fixture stops working at home, who do you contact? If your lights stop working, you call an electrician. Is your air conditioning unit out of order? Reach out to an HVAC (heating, ventilation and air conditioning) technician. What about if your sewer drains start backing up? Time to contact a plumber. And if your fire safety equipment needs servicing? Better call a fire safety technician. Regular maintenance and repairs on the inner workings of your household are always important, and when something goes wrong, it can be distressing and inconvenient to you and everyone living with you. You feel the need to get the issue resolved as quickly as possible, right? Now imagine that those needs are magnified – to the tune of hundreds of thousands of people every year. Who could potentially take on such a monumental task? Enter: Facilities Engineering at Renown Health. Crucial to ensuring our health system performs at its peak, these team members step in to make sure every patient, team member and visitor who walks through any of our doors are able to access the facilities they need and make their time with us as comfortable – and as successful – as possible. The Silent Heroes As our care teams move heroic mountains to save lives, another set of heroes emerge behind-the-scenes. As a strong backbone of our health system, the Facilities Engineering department plays a key role in maintaining the infrastructure that supports patient care, from ensuring the HVAC systems are functioning optimally to maintaining the plumbing and electrical systems that keep the lights on and the equipment running smoothly. Renown is fortunate to have some of the most dedicated journeymen in the business. This team boasts many experts, including: Plumbers Fire Safety Technicians Craftsmen HVAC Journeymen Electricians Boiler Operators Facilities Technicians As one can imagine, every day brings on a new challenge for our Facilities team members. “Each workday is always different; it could be water, power or HVAC issues or anything in between,” said Nhil Dado, Supervisor of Facilities Services. “We are proud of the services we provide for the needs of patients and employees.” “Every day, we have a variety of equipment to work on,” added Alfred Santos, HVAC Journeyman. “Whether it’s facility upkeep, plumbing, HVAC or electrical, we want to help,” added Brian McCarty, Facilities Technician. This department works around the clock to ensure that every aspect of our hospitals and outpatient care locations meets the highest standards of safety and efficiency, from routine maintenance and equipment improvements to emergency repairs. These are huge responsibilities – all of which they perform with pride. “As an HVAC journeyman, we are responsible for making sure the air circulating in the hospital is clean,” said Christopher Bobis, HVAC Journeyman. “It is also our job to make sure the air is positive and negative in isolation rooms and ensure patients are satisfied with the temperature in their rooms.” “In addition to performing regular maintenance tasks like changing air and water filters, we complete any random work order that may come up,” added Brett Courtney, Facilities Technician. “We also recently switched out our lighting at Renown South Meadows to LED lights, which helps with energy savings.” “I overlook the boiler house equipment and coordinate the fixing of maintenance issues reported by hospital staff,” added Arnt Utnes, Boiler Operator. “We also respond to every single alarm." It’s difficult for us to imagine what our health system would be like without the Facilities team providing us with the comfortable and safe environment our patients need and deserve. Luckily, we’re never alone in our efforts to keep us running, and this department expertly leads that charge. “Along with writing down the PSI readings in the gas rooms and answering calls from dispatch and the boiler rooms, I go through all the daily work orders and complete them,” said Ken Carrillo, Facilities Technician. “It always feels good to see when we complete all the work orders for the day, especially as the next shift arrives.” “We fix, replace and dispose of pieces that are no longer in service – bottom line, we help keep the building up and running,” added Alejandro Cardenas, Craftsman. But it doesn’t stop there – Facilities Engineering is currently in the midst of creating a whole new fleet vehicle program to improve the operations of our many on-site vehicles, including trucks, forklifts and more. “I am the point of contact for all things fleet,” said Michelle Bay, Administrative Assistant. “We are building a new fleet program and working closely with leadership to move the program forward. I am involved with setting up new fleet fuel cards and can set up the program in the best interest of our internal customers while looking to the future for growth.” It’s clear that the Facilities team is indispensable to Renown. Through their expertise, professionalism and commitment to quality, they stop at nothing to keep our health system functioning at its highest level.
Read More About Department Spotlight: Facilities Engineering
-
The Expanded Role of OBGYNs in Women's Healthcare
Obstetrician-gynecologists (OBGYNs) see patients from menses (the monthly menstrual cycle that occurs as a part of the female reproductive system), pregnancy and childbirth through menopause and play a pivotal role in managing reproductive health and overall wellness. Dr. James Alexander with Renown Women's Health explains. "As experts in women's health, we are uniquely positioned to recognize subtle changes or symptoms that might indicate broader health issues. This comprehensive approach allows us to serve as a valuable first touchpoint for various health concerns." Preventive Screenings: A Proactive Approach One key aspect is an OBGYN's ability to recommend preventive screenings based on your symptoms, age, lifestyle and medical history. For instance, lipid screenings are critical for monitoring cholesterol levels, which can be a significant factor in women’s heart disease. An OBGYN keeps up with the current guidelines for routine screening as well as in women with risk factors such as high blood pressure, diabetes, or a family history of heart disease during your visit. By identifying risks and abnormal screening early, they can collaborate with you to implement lifestyle changes or treatments to reduce your risk of heart conditions. Schedule Your Screening Appointment Make an Appointment by Phone: 775-982-5000
Read More About The Expanded Role of OBGYNs in Women's Healthcare
-
Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
Raquel was 33 when she was diagnosed with breast cancer. It was April 2023, when she found a lump in her breast and was referred to the William N. Pennington Cancer Institute. After comprehensive imaging, she was diagnosed with invasive lobular carcinoma, which is a type of breast cancer that begins in the milk-producing glands of the breast. Between June 2023 and January 2024, she received a total mastectomy, chemotherapy and radiation at Renown Health. “Breast cancer is uncommon in women under 40, but any woman with a mass or lump in her breast should have an exam by a physician and imaging at any age,” said Dr. Lee Schwartzberg. In fact, according to the Centers for Disease Control and Prevention (CDC), only 9% of all new cases of breast cancer in the U.S. are found in women younger than 45. “It was a pretty scary diagnosis, but I’ve been led by great people through the process,” she said. “They were so helpful and there for me throughout the chemo and radiation.” Raquel's journey through breast cancer treatment at the William N. Pennington Cancer Institute was marked by the exceptional care provided by the Renown Health team, including nurses, nurse navigators, therapists, support teams and providers. Among the dedicated professionals, Dr. Michelle Chu and Dr. Lee Schwartzberg played pivotal roles in Raquel's diagnosis and subsequent treatment plan. Their expertise, compassion and commitment to patient care left an indelible impact on Raquel's experience. Their thorough examination and comprehensive approach ensured that Racquel received the best possible care for her invasive lobular carcinoma. In addition to the care provided at Renown, Raquel greatly benefitted from being connected with a mentor by Dr. Chu. This mentor, Kayla, had undergone a similar diagnosis and treatment plan, and at the same age Raquel. They texted and called each other throughout Raquel’s treatment, providing additional support through a challenging time. As of January 2024, Raquel is done with her treatment and continues to see her care team for follow-up appointments. “I’m through the worst and ready to rebuild my life,” Raquel said. To help celebrate this milestone, Nevada Athletics invited Raquel to receive the game ball at a Nevada Men’s Basketball game. She was joined on the basketball court for this special recognition by her husband, Raul; mother, Arlene; and two daughters, Ryleigh and Rhiannon. Racquel's journey is not only a testament to her resilience but also a tribute to the invaluable contributions of Dr. Chu and Dr. Schwartzberg in guiding her towards triumph over breast cancer.
Read More About Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
-
A Transformative Journey: Mary's Bariatric Surgery Story at Renown Health
Embarking on the path to bariatric surgery is a unique and deeply personal journey. Individuals like Mary Escobar choose this life-changing route for reasons ranging from improved cardiovascular health to managing diabetes or finding relief from various health complications. In Mary's case, her two-decade-long healthcare journey not only underscores the challenges she faced but also highlights the support and expertise that ultimately led to her successful transformation through bariatric surgery. Mary's Resilience: December 2002 through February 2003 More than two decades ago, Mary experienced unforeseen health complications just days after giving birth via c-section. Septic shock, hemolytic uremic syndrome, thrombocytopenia, renal failure and a blood clot in her lung plunged her into a critical state. Intensive care, plasma exchange and a long recovery followed. After being discharged with compromised kidney function, Mary faced complete renal failure two years later, leading to dialysis and a spot on the donor list. Mary's brother, a perfect match, selflessly donated his kidney on Dec. 14, 2007, marking a turning point in Mary's health. However, the post-transplant period brought new challenges, including diabetes, high blood pressure and a significant weight gain, reaching 230 pounds. Determined to regain control, Mary explored various diets without success until she consulted with a bariatric doctor. Journey to Bariatric Surgery: November 2009 - April 2021 In November 2009, Mary opted for a gastric band, shedding 40 pounds within a year. Despite initial success, issues with the gastric band arose, prompting a consultation with Dr. John Ganser at Renown Health in April 2021. Together, they decided to transition to a gastric sleeve, with comprehensive education provided to ensure long-term success.
Read More About A Transformative Journey: Mary's Bariatric Surgery Story at Renown Health
-
The Impactful Role of Renown Health Foundation's Board of Directors
Above: Brian Cushard (left), Renown Health Foundation Board Chair, with his family At Renown Health Foundation, our mission is simple yet powerful – to raise funds that support Renown Health, the largest not-for-profit health system in northern Nevada. We are the driving force behind initiatives that bring state-of-the-art equipment, conduct groundbreaking research, enhance healthcare services, improve patient outcomes and contribute to the overall well-being of our community. Our Dedicated Board of Directors Our impactful work would not be possible without our Board of Directors – a fantastic team of 27 local volunteers. They bring diverse skills to the table, working together to create positive changes in healthcare for northern Nevada. Our board is at the core of our Foundation's success by guiding important decisions, sharing valuable insights and actively engaging in community relationships. Meet Brian Cushard – Renown Health Foundation’s Chair Brian Cushard took on the role of Foundation Board Chair at the beginning of 2024. Brian, who is the President of LP Insurance Services in Reno, will lead us for the next two years, bringing a wealth of experience and a deep commitment to community well-being. Since joining Renown Health Foundation’s Board in 2018, Brian has been instrumental in shaping our strategic direction. Brian’s Vision: Advocating for Renown Health’s Mission and Making a Difference We had the opportunity to sit down with Brian and explore his passion for healthcare philanthropy and the positive changes he envisions. Brian's 'why' is firmly rooted in the belief that a robust health system serves as the backbone of the community. His vision extends beyond fundraising; it's about inspiring the community by sharing remarkable stories of care and championing Renown's impactful contributions. Q: Why does Renown's mission matter to you, and how do you see your role making a difference? A: Renown's mission matters deeply to me because, without a highly functioning healthcare system, the economic structure of the community can be impacted. At LP Insurance, where I work, we see ourselves as guardians of our clients' hopes and dreams. This translates to my role on the Board as stewards for the health of others. Advocating for a highly functioning health system is crucial in supporting community members and clients alike. Surrounding ourselves with a solid network is essential. As advocates, our voices are integral in ensuring that everyone's voices are heard. Q: Can you share a moment that made you want to support healthcare causes? A: There are those stop-in-your-tracks healthcare moments that make you reassess life's priorities. I've had moments where life comes to a standstill, and what you once thought was important takes a backseat to the basics of life—getting better, one step at a time. In those vulnerable moments, you realize the importance of every person at the hospital. In desperate need, we rely on them. It's eye-opening and gives perspective on what's truly valuable in life. Q: Tell us about a time when you saw the positive impact of healthcare or philanthropy. How did that influence your decision to get involved? A: One impactful moment in philanthropy stands out — the Music and Miracles concert featuring the Beach Boys. LP Insurance was a major donor, contributing $100,000 to benefit Sophie’s Place, a music therapy room coming to Renown Children's Hospital. On the day of the event, my wife and I volunteered and saw the remarkable community support for Renown Children’s Hospital. The collective efforts that day raised over $1 million, specifically designated to establish Sophie’s Place. This experience inspired me to want to do more, as I recognized the profound positive impact that philanthropy can have on healthcare and the community. Note: Sophie’s Place, opening later this year, will offer vital care and healing experiences for young patients at Renown Children’s Hospital.
Read More About The Impactful Role of Renown Health Foundation's Board of Directors
-
How Regular Cervical Cancer Screenings Can Save Lives
According to the American Cancer Society, approximately 13,820 new cases of invasive cervical cancer will be diagnosed, and 4,360 women will die from cervical cancer. However, cervical cancer is preventable with regular screening tests and the HPV vaccine. It’s important to note that medical advances have allowed progress in diagnosing and treating cervical cancer. While it used to be one of the most common causes of cancer death for American women, the incidence of death has significantly declined. What to Know About the HPV Vaccine HPV vaccination is the best way to prevent cervical cancer and is recommended for all youth starting as early as age 9, or for teens and adults up to age 45 who didn’t start or finish the series. In Nevada, only 50.1% of teens ages 13-17 have been vaccinated for HPV. There are 13 types of HPV, and the vaccine Gardasil 9 protects against 9 of those HPV strains, greatly reducing the incidence of cervical cancer among vaccinated individuals. What to Know About Cervical Cancer Screenings The CDC says the most important thing you can do to help prevent cervical cancer is to have regular screening tests starting at age 21. And there are two common tests that can detect early stages of cervical cancer (or precancer) and improve health outcomes. The pap test (or pap smear). This screening looks for precancers. Women should begin getting pap smears when they’re 21. The human papillomavirus (HPV) test looks for the virus that can cause these cell changes. Cervical Cancer Screening Schedule The American Cancer Society offers the following guidelines for screenings: All women should begin cervical cancer screening at 21. Women between 21 and 29 should have a pap test every three years. Beginning at 30, the preferred way to screen is with a pap test combined with an HPV test every five years. This is called co-testing and should continue until age 65. A pap test (or pap smear) is performed during a regular screening appointment to look for precancers, cell changes on the cervix that might become cervical cancer if they are not evaluated or appropriately treated. Typically outpatient procedures can reduce the risk of long-term health impacts that prevent pre-cancerous cells from becoming cancer cells. Women over 65 who have had regular screenings in the previous ten years should stop cervical cancer screening as long as they haven’t had any severe precancers found in the last 20 years. How to Get Screened Request an appointment with your primary care physician or OBGYN to schedule a screening.
Read More About How Regular Cervical Cancer Screenings Can Save Lives
-
Department Spotlight: Float Pool
Ring in the New Year and the rest of the holiday season by celebrating Renown’s Float Pool team! After coming out of the COVID-19 pandemic, it's no mystery that healthcare across the country has shifted and adapted to the growing needs and new demands of our patient populations. Renown Health is no different. As the largest not-for-profit health system in the region, we are no stranger to change, even when change presents challenges. Who do we call on when a unit needs more team members in the eleventh hour? Who can help when our patient volume spikes up with seconds to spare? This is where the Float Pool at Renown comes to the rescue. Skilled in a wide variety of healthcare specialties, from acute care nursing and critical care to care aiding and patient safety, this is the team that can seamlessly step in to provide crucial patient care to the units that need it most, whether a team is understaffed for the day or needs extra all-hands-on-deck for a specific patient or procedure. Float Pool team members are equipped to work in virtually any clinical area at Renown, making a genuine difference with every patient they encounter. A Pool of Relief Teams across Renown can breathe a sigh of relief knowing that Float Pool has their back in times of need. As the backbone of our health system, these dedicated team members possess a wealth of clinical knowledge and the ability to navigate diverse medical environments. Their flexibility allows them to fill staffing gaps and provide essential support to many different units. “We fill in the gaps of staffing to make everyone's day better,” said Patti Crepps, Critical Care Float Pool RN. “A float nurse has to be flexible and able to adapt to different situations and places – basically, ‘go with the flow.’ Patient care is basically the same all over; we make patient care possible by being familiar with all the various specialties and providing the specific care needed depending on the population we are taking care of on that shift.” “Float Pool staff members are like healthcare chameleons, transitioning between different departments,” added Shelby Riach, Acute Float Pool RN. “We incorporate flexibility, teamwork and a commitment to ensuring patients receive the best care, regardless of the setting or circumstances.” This team thrives in uncertainty; in fact, no workday is the same in Float Pool – and that’s exactly the way they like it. Working with many different teams across a multitude of specialties, these Care Aides, RNs, Critical Care Techs, Patient Safety Assistants (PSAs), Certified Nurses Assistants (CNAs) and more enjoy facing change, while they all share a goal of providing the best patient care possible. “No day looks the same; since we are the Float Pool, we are assigned a different assignment on Smart Square every day, whether it be as a care aide, a patient safety assistant, a unit clerk or patient transport,” said Melina Castenada, Care Aide. “If we are assigned as a care aide on the floor, we help assist with call lights and help with whatever nurses and CNAs may need, including feeding, transporting, walking, helping patients use the restroom, etc. When we are assigned as a PSA ‘sitter,’ we sit for the patient to help keep them safe. If we are assigned as unit clerk, we help answer phones and direct patients appropriately, file paperwork, answer call lights if needed and assist with office work.” “I love that every day is a different floor with different tasks and a different atmosphere,” added Julia Chappell, Critical Care Technician. “I find out which floor that I will be on right before my shift starts and head to the floor to find out my assignment for the day. Depending on the specialty, such as the medical-surgical floor versus an intensive care unit (ICU), my daily job tasks can vary.” When it comes to high-risk patients, who require special attention, PSAs within Float Pool step in to help. “The PSA role within Float Pool largely consists of adverse event prevention for our high-risk patients, and being a Float Pool employee allows us to work wherever we are needed,” said Dimitri Macouin, Patient Safety Assistant. “Whether it be in the emergency department, neurology or pediatrics, the PSA will be the eyes and ears for the nurses working with this patient population.” “Great strides have been made to ensure that PSAs remain vigilant and are recognized as an integral part of the patients' care team rather than 'just a sitter,’” added Karla Phillips, Patient Safety Assistant. Float Pool also oversees our Discharge Lounge, which offers patients and their families a dedicated space to reconnect and prepare for their discharge from the hospital. “The increase in utilization of the Discharge Lounge is something we are very proud of,” said Kara Abshier, Care Aide. “We assist in discharging patients from all over the hospital to help the floor and get new patients into rooms.” Every day brings a new challenge for Float Pool. As these team members wake up with uncertainty, they are ready to embrace the diverse demands of caring for patients of all ages. “The fact that Float Pool exists is amazing,” said Hannah Luccshesi, Acute Float Pool RN. “We wake up with no clue as to whether we will be working with babies, children or adults and then fill in the needs of the hospital.”
-
6 Healthcare Action Items for the LGBTQIA+ Community
Every patient, regardless of how they may identify, greatly benefits from preventive healthcare and early detection. Members of the LGBTQIA+ community face unique considerations when it comes to their health, and a proactive approach to preventive screenings and vaccines is important in order to address their individual health needs. Dr. Karen Thiele, Family Medicine Physician with University Health and Assistant Professor of Family and Community Medicine at the University of Nevada, Reno School of Medicine, breaks down key steps that LGBTQIA+ patients should take to safeguard their health. PrEP and PEP Pre-exposure prophylaxis (PrEP) is a strategy to prevent human immunodeficiency virus (HIV) infection. It is an important measure for those who are HIV-negative but may be at risk of contracting it. The highest risk sexual practice is receptive anal intercourse, due to the relative fragility of rectal tissue. This medication can stop HIV from spreading in the body and help patients maintain their HIV-negative status. PrEP is available in both pill form, which is taken every day, and injection form, of which the first two injections are initiated one month after another while all other injections are initiated every two months. Post-exposure prophylaxis (PEP) is an antiretroviral drug regimen taken after potential HIV exposure to prevent an HIV-negative individual from converting to HIV-positive status. PEP is only for emergency situations and must be started within 72 hours of exposure – sooner is always better than later – and must be taken for 28 days. PrEP and PEP are available in many ways, including visiting your primary care provider (PCP) or an urgent care location. HPV Immunization All genders and identities can protect themselves against human papillomavirus (HPV), a sexually transmitted infection (STI) that can lead to the risk of cervical, mouth, head, neck, throat, anal, vaginal, penile and vulvar cancers. HPV is so common that nearly all sexually active people, regardless of sexual orientation and practices, will be exposed at some point in their lifetime. The HPV vaccine (common brands include Gardasil and Cervarix) is a safe and effective method to prevent HPV, according to the Centers for Disease Control and Prevention (CDC). This vaccine protects against infections that can lead to HPV-related cancers and precancers, as well as genital warts. While patients should start receiving the vaccine at 9 years old years old, unvaccinated adults up to the age of 45 can also receive the vaccine through their PCP – better late than never! STI Testing Sexually-transmitted infections form from bacteria, viruses or parasites that can be transmitted by person-to-person sexual contact through semen, vaginal, blood and other bodily fluids. According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new STI cases across the nation each year. Luckily, most STIs are preventable. Annual STI testing for HIV, gonorrhea, chlamydia and syphilis is important to stay on top of your sexual health. Because these STIs may sometimes have no symptoms, screening is recommended regularly and with any change in sexual partners. Depending on the specific condition, tests for these infections include urine, swab and blood tests. Speak with your primary care provider on a screening schedule that works best for you. Prostate Exams Prostate exams look for early signs of prostate cancer in patients who still have a prostate. The CDC recommends those who are at least 55 years old get regular prostate screenings; however, for patients with a family history of prostate cancer, screenings may be recommended as early as 45 years old. These exams are done via two common methods – a prostate specific antigen (PSA) blood test and a digital rectal examination (DRE). Your provider can help you determine your risk and when you should start getting screened. Pap Tests and Pelvic Exams Patients of all genders who have a cervix, uterus, vagina and/or ovaries will benefit from regular pelvic exams and Pap screenings. A pelvic exam consists of a provider looking inside the vagina and at the cervix for anything unusual. A Pap test, also known as a Pap smear, involves your provider using a small, soft swab to collect cervical cells to check for early signs of cancer. Generally speaking, people with these organs should have a Pap test every three years starting at age 21 through the age of 30. After age 30, patients should receive a Pap test with HPV co-testing every five years until age 65. These recommendations are changing based on new research, so it is important to have a conversation with your PCP about the current guidelines so you can make an informed choice about what schedule you should follow. A gynecologist or your primary care provider can counsel you and perform these screenings. Mammograms and Breast Exams People with breast tissue, especially dense breast tissue, are at risk for breast cancer, and regular breast screenings are your best line of defense. At-home breast self-exams are the first step – you will want to check your breasts for any lumps, changes, fluid leaks, irregular tissue thickening or anything else that feels unusual. The Breast Cancer Risk Assessment tool, provided by the National Cancer Institute, is a good place to start to identify your risk. Talk with your primary care provider about the risks and benefits of starting screening at age 40 so you can make an informed decision about when to start. If you have any family history of breast or ovarian cancer, your PCP will offer you genetic testing for BRCA 1 and 2 mutations. Nevadans over the age of 18 can also get BRCA genetic test for free by enrolling in the Healthy Nevada Project. Mammograms are important screening tools, but for a significant portion of people with breast tissue, density of the breast tissue may make mammograms less helpful in detecting cancer. Your primary care provider can help you decide what additional imaging (such as breast ultrasound) might be best for you.
Read More About 6 Healthcare Action Items for the LGBTQIA+ Community






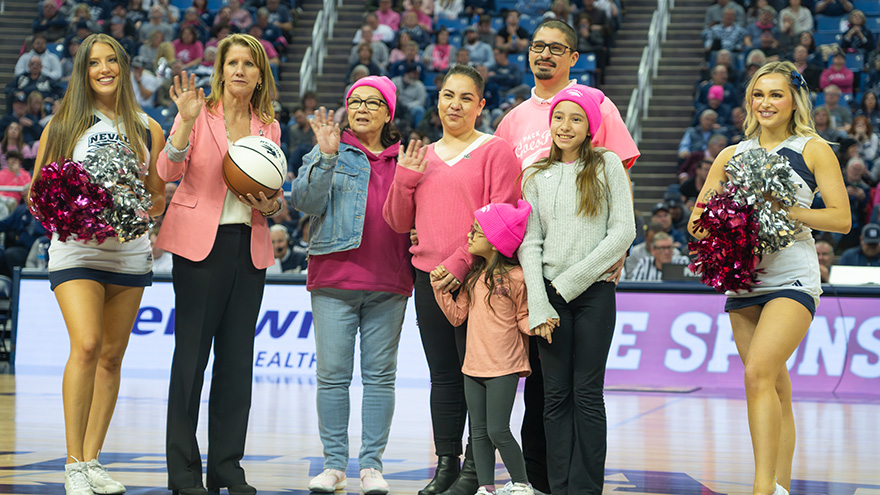



.png?rev=fcd27802b7604a96bf1056b050ef90c5)
