Search
-
What You Need To Know About Cold Water Drowning
Northern Nevada's stunning lakes, including Lake Tahoe, with its average summer water temperature of 50 degrees, present a potential risk of hypothermia. Unlike mild 50-degree air, water at the same temperature poses severe, life-threatening risks, including rapid-onset hypothermia and drowning. Awareness of the symptoms and taking proper precautions are crucial to prevent cold-water drowning. The 4 Phases of Cold-Water Drowning 1. Cold Shock Response: This response affects breathing and happens within the first minute. An automatic gasp reflex occurs in response to rapid skin cooling. If the head goes below water, water may be breathed into the lungs, resulting in drowning. A life jacket will help keep your head above water during this critical phase. Additionally, hyperventilation, like the gasp reflex, is a response to the cold and will subside. Panic will make this worse, so the key is to control breathing. 2. Cold Incapacitation: This response occurs within the first five to 15 minutes in cold water. In order to preserve core heat, vasoconstriction takes place decreasing blood flow to the extremities to protect the vital organs. The result is a loss of movement to hands, feet, arms and legs. Unless a life jacket is being worn, the ability to stay afloat is next to impossible. 3. Hypothermia: Important to note, it can take 30 minutes or more for most adults to become hypothermic. So there’s time to take action and survive. Keeping panic at bay is critical, as you have more survival time than you think. Symptoms include: Shivering Slow and shallow breathing Confusion Drowsiness or exhaustion Slurred speech Loss of coordination Weak pulse 4. Circum-rescue Collapse: This experience can happen just before rescue and is not well understood. Symptoms range anywhere from fainting to death. Some experts believe an abrupt drop in blood pressure may cause this final stage of cold water drowning, post-rescue. Additional Safety Tips and Helpful Resources Always wear a personal flotation device as well as a wetsuit or drysuit. Your personal flotation device is the most important piece of water safety gear. Try not to panic as the first phases will subside. Controlled breathing is to staying calm. Research suggests the body can withstand the cold longer than we think. The Heat Escape Lessening Posture (HELP) is a position which helps conserve energy if you’re wearing a personal flotation device. By hugging your knees to your chest, this posture helps maintain body heat for some time.
Read More About What You Need To Know About Cold Water Drowning
-
Why I Give: Tami and Richard's Story
If you have the chance to meet Tami and Richard Dethmers, you will quickly discover a remarkable couple who embody a heartwarming spirit. Married for 44 years, they cherish family above all else. With five children and 10 grandchildren, their family is not just their priority—it's their whole world. It is this love and their steadfast faith that led Tami and Richard to make a transformative donation to Renown Children’s Hospital. The Heart of Giving In 2023, Tami toured the construction of the new Wilbur D. May Neonatal Intensive Care Unit and Pediatric Intensive Care Unit at Renown Children's Hospital. She was touched by the idea of creating a special place for sick children and their families. That night, she talked with Richard about how they could help. Together, they both agreed to make a generous donation that could help ease the pain for families with children in the hospital. A Comforting Consultation Room Their donation established a consultation room in the Wilbur D. May NICU and PICU at Renown Children's Hospital. Tami and Richard's motivation stems from personal experience, having seen their grandson endure four open-heart surgeries. "I remember challenging conversations with doctors, surrounded by other families in the open PICU. It was difficult,” said Tami. In this new consultation room, families have a private space to learn about the next steps in their journey, gaining insights into the illnesses affecting their children. It is a dedicated space where doctors can discuss treatment plans and medical information with families. Designed to be a supportive and calming environment, the room features art on the walls, and a window bathes the space in beautiful, natural light, offering comfort to families in need. Tami and Richard’s donation ensures that families in the NICU and PICU can navigate difficult conversations with doctors in a thoughtfully designed space. Because We Love You and We Care In the new consultation room, a powerful message is printed and framed: 'Because we love you and we care.' This phrase is an important part of Tami and Richard’s donation, reflecting words they spoke to their children while they were growing up. For them, it symbolizes love, care, and a commitment to offering support. A Legacy of Comfort Tami and Richard, along with their family, are dedicated to an ongoing legacy of giving. Together, they also donated blankets to patients and families who use the consultation room. “I hope they provide an added layer of comfort,” said Tami. Each blanket includes a custom tag repeating those same words 'Because we love you and we care.' Richard echoes Tami's sentiments. “We do what we can because we love children, and there is no greater pain than a child in distress,” Richard said, emphasizing their shared dedication to helping children in need. Together, with their children and grandchildren, they continue to make a difference, embodying the power of compassion and generosity in their family's legacy.
-
The Expanded Role of OBGYNs in Women's Healthcare
Obstetrician-gynecologists (OBGYNs) see patients from menses (the monthly menstrual cycle that occurs as a part of the female reproductive system), pregnancy and childbirth through menopause and play a pivotal role in managing reproductive health and overall wellness. Dr. James Alexander with Renown Women's Health explains. "As experts in women's health, we are uniquely positioned to recognize subtle changes or symptoms that might indicate broader health issues. This comprehensive approach allows us to serve as a valuable first touchpoint for various health concerns." Preventive Screenings: A Proactive Approach One key aspect is an OBGYN's ability to recommend preventive screenings based on your symptoms, age, lifestyle and medical history. For instance, lipid screenings are critical for monitoring cholesterol levels, which can be a significant factor in women’s heart disease. An OBGYN keeps up with the current guidelines for routine screening as well as in women with risk factors such as high blood pressure, diabetes, or a family history of heart disease during your visit. By identifying risks and abnormal screening early, they can collaborate with you to implement lifestyle changes or treatments to reduce your risk of heart conditions. Schedule Your Screening Appointment Make an Appointment by Phone: 775-982-5000
Read More About The Expanded Role of OBGYNs in Women's Healthcare
-
Understanding the Reasons Behind Heavy Menstrual Cycles
While menstrual cycles can be an annoying inconvenience for many women, heavy bleeding (menorrhagia) is not normal and can disrupt your life. A few days of heavy flow at the start of your period is usually nothing to worry about. However, if you’re frequently experiencing very heavy periods, you should discuss it with your gynecologist or primary care provider. Dr. Megan Fish, an OB-GYN with Renown Women’s Health, discusses various reasons, evaluation and treatment methods when it comes to heavy menstrual cycles. What is classified as heavy menstrual bleeding? The American College of Obstetricians and Gynecologists considers heavy bleeding to be any of the following signs: Bleeding that lasts more than 7 days. Bleeding that soaks through one or more tampons or pads every hour for several hours in a row. Needing to wear more than one pad at a time to control menstrual flow. Needing to change pads or tampons during the night. Menstrual flow with blood clots that are as big as a quarter or larger. What are the most common reasons for heavier periods? A variety of reasons why someone might have heavy periods. Fortunately, most of these problems are treatable. Because each woman's period is unique, only a doctor can definitively determine the cause of your heavy periods. Some of the most common issues that cause heavy periods include: Hormone imbalances such as anovulation, thyroid disease and Polycystic Ovary Syndrome (PCOS). Structural abnormalities in your uterus such as polyps or fibroids. Precancer and cancer such as uterine, cervical, vaginal, ovarian or endometrial hyperplasia. Infections such as chlamydia, gonorrhea, endometritis or vaginitis. Other medical conditions such as liver disease, kidney disease or Pelvic Inflammatory Disease. Medications such as blood thinners and aspirin, hormone replacement therapy, Intrauterine devices (IUDs), birth control pills and injectables. Pregnancy-related problems such as a miscarriage or ectopic pregnancy.
Read More About Understanding the Reasons Behind Heavy Menstrual Cycles
-
Sterling Silver Club Shining Stars: Mark & Dana Combs
Dana and Mark Combs met through mutual friends and had a long friendship before they became a couple in 2009. They were married in 2011 in a private ceremony at a small Reno chapel, and a few months later had a big celebration with their family and friends. Encouraging Others to Succeed Over the years, the happy couple has spent much of their time volunteering and giving back to others in their community. Twenty-six years ago, Mark became a bilateral lower limb amputee. For the past 10 years, he has been a prosthetic consultant, helping other amputees learn how to cope with various challenges and encouraging them to keep living life to the fullest. “Mark is great with helping people,” said Dana. Dana also does a lot of rewarding work through a Philanthropic Educational Organization (P.E.O). She is an advocate for raising money to help women ages 18 and up gain an education. Dana also enjoys tutoring English as a second language. Enjoying Quality Time, Hobbies & Travel When Dana and Mark aren’t helping others, they are spending time with their family and friends, their dog Mia (a 3-year-old Maltipoo) or enjoying one of their many hobbies. Some of Mark’s favorite things to do include playing Solitaire and strumming on his guitar. “I love to garden and play crossword puzzles and word games,” said Dana. “I’m really looking forward to the springtime to spend more time in the garden.” She loves to work out and has a membership at the UFC gym in Reno through her Senior Care Plus gym benefit. Dana also has her own online Etsy store, where she sells homemade jam jars, candle holders and vintage dolls. “Last summer I sold my first edition Barbie that I got when I was 9 years old,” said Dana. “I made quite a profit on it.”
Read More About Sterling Silver Club Shining Stars: Mark & Dana Combs
-
The Impactful Role of Renown Health Foundation's Board of Directors
Above: Brian Cushard (left), Renown Health Foundation Board Chair, with his family At Renown Health Foundation, our mission is simple yet powerful – to raise funds that support Renown Health, the largest not-for-profit health system in northern Nevada. We are the driving force behind initiatives that bring state-of-the-art equipment, conduct groundbreaking research, enhance healthcare services, improve patient outcomes and contribute to the overall well-being of our community. Our Dedicated Board of Directors Our impactful work would not be possible without our Board of Directors – a fantastic team of 27 local volunteers. They bring diverse skills to the table, working together to create positive changes in healthcare for northern Nevada. Our board is at the core of our Foundation's success by guiding important decisions, sharing valuable insights and actively engaging in community relationships. Meet Brian Cushard – Renown Health Foundation’s Chair Brian Cushard took on the role of Foundation Board Chair at the beginning of 2024. Brian, who is the President of LP Insurance Services in Reno, will lead us for the next two years, bringing a wealth of experience and a deep commitment to community well-being. Since joining Renown Health Foundation’s Board in 2018, Brian has been instrumental in shaping our strategic direction. Brian’s Vision: Advocating for Renown Health’s Mission and Making a Difference We had the opportunity to sit down with Brian and explore his passion for healthcare philanthropy and the positive changes he envisions. Brian's 'why' is firmly rooted in the belief that a robust health system serves as the backbone of the community. His vision extends beyond fundraising; it's about inspiring the community by sharing remarkable stories of care and championing Renown's impactful contributions. Q: Why does Renown's mission matter to you, and how do you see your role making a difference? A: Renown's mission matters deeply to me because, without a highly functioning healthcare system, the economic structure of the community can be impacted. At LP Insurance, where I work, we see ourselves as guardians of our clients' hopes and dreams. This translates to my role on the Board as stewards for the health of others. Advocating for a highly functioning health system is crucial in supporting community members and clients alike. Surrounding ourselves with a solid network is essential. As advocates, our voices are integral in ensuring that everyone's voices are heard. Q: Can you share a moment that made you want to support healthcare causes? A: There are those stop-in-your-tracks healthcare moments that make you reassess life's priorities. I've had moments where life comes to a standstill, and what you once thought was important takes a backseat to the basics of life—getting better, one step at a time. In those vulnerable moments, you realize the importance of every person at the hospital. In desperate need, we rely on them. It's eye-opening and gives perspective on what's truly valuable in life. Q: Tell us about a time when you saw the positive impact of healthcare or philanthropy. How did that influence your decision to get involved? A: One impactful moment in philanthropy stands out — the Music and Miracles concert featuring the Beach Boys. LP Insurance was a major donor, contributing $100,000 to benefit Sophie’s Place, a music therapy room coming to Renown Children's Hospital. On the day of the event, my wife and I volunteered and saw the remarkable community support for Renown Children’s Hospital. The collective efforts that day raised over $1 million, specifically designated to establish Sophie’s Place. This experience inspired me to want to do more, as I recognized the profound positive impact that philanthropy can have on healthcare and the community. Note: Sophie’s Place, opening later this year, will offer vital care and healing experiences for young patients at Renown Children’s Hospital.
Read More About The Impactful Role of Renown Health Foundation's Board of Directors
-
Patty Warren A Woman of Strength and Resilience
Meet and get to know Patty Warren, our featured Sterling Silver Club member this fall. You may recognize her from the latest Senior Care Plus commercial on television, where she joins a coffee chat discussing the many benefits of being a Senior Care Plus member. She’s one of the kindest souls you’ll ever meet – and has a positive outlook on life that we should all strive for. Patty's Story Patty was born and raised in a small Kansas town called Baxter Springs, where she grew up with an older brother, an older sister and two younger sisters. She and her siblings all enjoyed playing sports like softball and basketball, in addition to playing instruments. Patty developed a love and passion for music at a young age that carried into her adulthood. “I wanted to be an opera singer,” said Patty. “I decided to go to college at Pittsburg State University in Kansas where I majored in vocal performance.” After college, Patty moved to Manhattan in New York City to audition to be an opera singer, but she soon realized it wasn’t what she wanted to do after all. She eventually decided to work in the brokerage industry. After living and working in New York for three years, Patty moved back to Kansas where she later met the love of her life, Michael. “In 1992, I had put a dating ad in the local newspaper,” said Patty. “I received over 30 responses, and I went out on quite a few dates.” Then she had her first date with Michael, and the two of them quickly realized how much they liked each other. He asked her to marry him on Valentine’s Day in 1993, and they went on to get married in front of the Justice of the Peace on May 3, just a few months later. “We had a small wedding so that we could move into our first home together,” said Patty. A few years later in 1999, Patty and Michael moved to Arizona, where they lived for 22 years. Patty worked at Edward Jones Investments for 18 of those 22 years and loved her job and the people that she worked with. She retired in January 2021 during the pandemic, and three days later she and Michael moved to Sparks, Nevada.
Read More About Patty Warren A Woman of Strength and Resilience
-
6 Healthcare Action Items for the LGBTQIA+ Community
Every patient, regardless of how they may identify, greatly benefits from preventive healthcare and early detection. Members of the LGBTQIA+ community face unique considerations when it comes to their health, and a proactive approach to preventive screenings and vaccines is important in order to address their individual health needs. Dr. Karen Thiele, Family Medicine Physician with University Health and Assistant Professor of Family and Community Medicine at the University of Nevada, Reno School of Medicine, breaks down key steps that LGBTQIA+ patients should take to safeguard their health. PrEP and PEP Pre-exposure prophylaxis (PrEP) is a strategy to prevent human immunodeficiency virus (HIV) infection. It is an important measure for those who are HIV-negative but may be at risk of contracting it. The highest risk sexual practice is receptive anal intercourse, due to the relative fragility of rectal tissue. This medication can stop HIV from spreading in the body and help patients maintain their HIV-negative status. PrEP is available in both pill form, which is taken every day, and injection form, of which the first two injections are initiated one month after another while all other injections are initiated every two months. Post-exposure prophylaxis (PEP) is an antiretroviral drug regimen taken after potential HIV exposure to prevent an HIV-negative individual from converting to HIV-positive status. PEP is only for emergency situations and must be started within 72 hours of exposure – sooner is always better than later – and must be taken for 28 days. PrEP and PEP are available in many ways, including visiting your primary care provider (PCP) or an urgent care location. HPV Immunization All genders and identities can protect themselves against human papillomavirus (HPV), a sexually transmitted infection (STI) that can lead to the risk of cervical, mouth, head, neck, throat, anal, vaginal, penile and vulvar cancers. HPV is so common that nearly all sexually active people, regardless of sexual orientation and practices, will be exposed at some point in their lifetime. The HPV vaccine (common brands include Gardasil and Cervarix) is a safe and effective method to prevent HPV, according to the Centers for Disease Control and Prevention (CDC). This vaccine protects against infections that can lead to HPV-related cancers and precancers, as well as genital warts. While patients should start receiving the vaccine at 9 years old years old, unvaccinated adults up to the age of 45 can also receive the vaccine through their PCP – better late than never! STI Testing Sexually-transmitted infections form from bacteria, viruses or parasites that can be transmitted by person-to-person sexual contact through semen, vaginal, blood and other bodily fluids. According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new STI cases across the nation each year. Luckily, most STIs are preventable. Annual STI testing for HIV, gonorrhea, chlamydia and syphilis is important to stay on top of your sexual health. Because these STIs may sometimes have no symptoms, screening is recommended regularly and with any change in sexual partners. Depending on the specific condition, tests for these infections include urine, swab and blood tests. Speak with your primary care provider on a screening schedule that works best for you. Prostate Exams Prostate exams look for early signs of prostate cancer in patients who still have a prostate. The CDC recommends those who are at least 55 years old get regular prostate screenings; however, for patients with a family history of prostate cancer, screenings may be recommended as early as 45 years old. These exams are done via two common methods – a prostate specific antigen (PSA) blood test and a digital rectal examination (DRE). Your provider can help you determine your risk and when you should start getting screened. Pap Tests and Pelvic Exams Patients of all genders who have a cervix, uterus, vagina and/or ovaries will benefit from regular pelvic exams and Pap screenings. A pelvic exam consists of a provider looking inside the vagina and at the cervix for anything unusual. A Pap test, also known as a Pap smear, involves your provider using a small, soft swab to collect cervical cells to check for early signs of cancer. Generally speaking, people with these organs should have a Pap test every three years starting at age 21 through the age of 30. After age 30, patients should receive a Pap test with HPV co-testing every five years until age 65. These recommendations are changing based on new research, so it is important to have a conversation with your PCP about the current guidelines so you can make an informed choice about what schedule you should follow. A gynecologist or your primary care provider can counsel you and perform these screenings. Mammograms and Breast Exams People with breast tissue, especially dense breast tissue, are at risk for breast cancer, and regular breast screenings are your best line of defense. At-home breast self-exams are the first step – you will want to check your breasts for any lumps, changes, fluid leaks, irregular tissue thickening or anything else that feels unusual. The Breast Cancer Risk Assessment tool, provided by the National Cancer Institute, is a good place to start to identify your risk. Talk with your primary care provider about the risks and benefits of starting screening at age 40 so you can make an informed decision about when to start. If you have any family history of breast or ovarian cancer, your PCP will offer you genetic testing for BRCA 1 and 2 mutations. Nevadans over the age of 18 can also get BRCA genetic test for free by enrolling in the Healthy Nevada Project. Mammograms are important screening tools, but for a significant portion of people with breast tissue, density of the breast tissue may make mammograms less helpful in detecting cancer. Your primary care provider can help you decide what additional imaging (such as breast ultrasound) might be best for you.
Read More About 6 Healthcare Action Items for the LGBTQIA+ Community
-
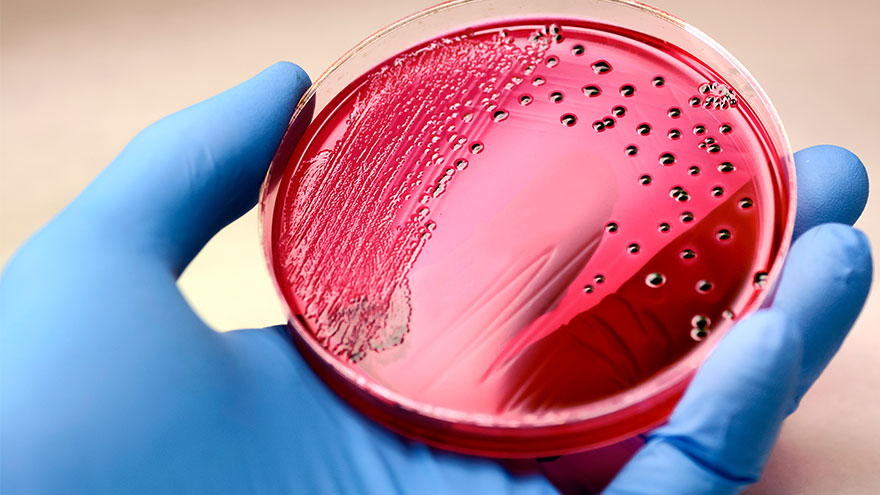
Sepsis: Causes & Symptoms
According to the Global Sepsis Alliance, 1 in 5 deaths worldwide are associated with sepsis. If not recognized early and treated promptly, sepsis is the final common pathway to death from most infectious diseases worldwide, including viruses such as COVID-19. We spoke with Jeremy Gonda, MD, a critical care physician from Renown Health’s Sepsis Committee to increase public awareness of this preventable medical emergency. What is sepsis? Sepsis is a response to infection—bacterial, viral or fungal—and can start anywhere in the body and spread into the bloodstream. The body is trying so hard to fight an infection that it begins releasing chemicals into the bloodstream that cause inflammation and the shutdown of multiple organ systems. “It carries a very poor prognosis in general unless you catch and treat it very early,” said Dr. Gonda. “Any infection can lead to sepsis. Typically your immune system takes care of the infection. It doesn’t progress, but in cases where the infection becomes severe, or the immune system doesn’t function properly, people can certainly die. So there’s, unfortunately, a very high mortality rate associated with sepsis.” According to the Centers for Disease Control and Prevention, each year at least 1.7 million adults in America develop sepsis. While you can recover from sepsis if caught early, many sepsis survivors suffer from long-term physical and psychological effects. What are the signs of sepsis? One way to spot sepsis is to use the acronym SEPSIS: S – Slurred speech and confusion E – Extreme shivering or muscle pain/fever P – Passing no urine all day S – Severe breathlessness I – “I feel like I might die” S – Skin mottled or discolored Keep in mind that sepsis symptoms can vary depending on where the infection starts. “Patients may experience urinary burning if they have a urinary tract infection or a cough and shortness of breath if they have pneumonia first,” said Dr. Gonda. “However, often symptoms are more generalized or subtle such as fevers, confusion and malaise.” How do you develop sepsis? When germs enter your body, they can cause an infection. If you don’t stop that infection, it can cause sepsis. Areas of infection that more commonly result in sepsis include: Lungs, such as pneumonia Kidney, bladder and other parts of the urinary system Digestive system Bloodstream (bacteremia) Catheter sites Wounds or burns Who is most at risk? People with compromised immune systems are at greater risk for sepsis, such as “The very young, the elderly and any people who may have conditions that suppress your immune system,” said Dr. Gonda. “For instance, if you have diabetes or if you’re an organ transplant patient who is on immunosuppressant therapy, you’re at somewhat higher risk.” Sepsis is often considered a hospital-acquired infection, but a study in The Journal of American Medical Association found that 80% of sepsis cases occur outside of a hospital. That’s why it’s especially important to remember any infection can lead to sepsis, and anyone can develop sepsis from an infection. What do I do? Timing is critical in the case of sepsis and septic shock. According to a study on septic shock patients, there is a 7.6 percent decrease in survival for each hour treatment is delayed. On the other end, if treatment is given within an hour of the first drop in blood pressure, the survival rate is 80 percent. Because sepsis can be so deadly, it’s important to seek medical attention as soon as possible. “If you’re not getting any better, if you think symptoms are progressively worsening – you should definitely be evaluated by a doctor,” said Dr. Gonda. You can help #StopSepsis by getting involved at worldsepsisday.org.
-
Department Spotlight: Renown Transfer and Operations Center
Stepping into the Renown Transfer and Operations Center (RTOC) means stepping into a transformative hub of excellence where lives are saved and healthcare is reimagined. As a cornerstone of Renown Health's commitment to exceptional patient care, the RTOC serves as a dynamic nerve center that seamlessly coordinates medical resources, ambulance rides, hospital bed space, remote home systems, hospital transfers and emergency preparedness. In this best-in-class facility, the boundaries of what is possible in healthcare are constantly pushed, and new horizons of patient care are discovered. Staffed with a dedicated team of skilled professionals, the RTOC harnesses the power of advanced technology and compassionate expertise to ensure that patients receive the highest level of care and support, no matter where they are. Through a synchronized network of communication, coordination, and compassionate care, the RTOC team ensures that patients receive the critical support they need when it matters most, working tirelessly to redefine what it means to deliver world-class healthcare. A National Standard Charged with the goal of overseeing the placement and transportation for every patient, the RTOC officially launched in 2021 as northern Nevada’s first and only transfer center of its kind and a nationally celebrated facility. As Renown’s highly coordinated care logistics system, this team uses the cutting-edge technology at their fingertips to customize healthcare to the needs of every patient, manage patient flow and drive healthcare innovation. “Compared to where we’ve started to where we are now, it’s a 180-degree difference,” said Kelli McDonnell, Manager of RTOC. “When we first started building our facility right before the pandemic happened, we took what was six conference rooms and classrooms and turned it into a command center that organizations across the country admire and come to Reno to see what we do. Mel Morris, the Director of RTOC, was recruited exclusively to build our facility with her history of building successful hospital command centers. Many people didn’t realize what a transfer center was or that Renown was the only center in the region – and we only continue to grow.” This best-in-class facility, and the masterful team behind it, handles: Coordinating all incoming patients transferred from neighboring hospitals and 27 counties across northern Nevada, Lake Tahoe, northeast California and neighboring states. Matching patients to the most appropriate bed placement using diagnostic, triage and Epic electronic medical record clinical information in conjunction with medical staff expertise to outline a plan of care that determines the best bed assignment given the patient’s needs. Coordinating video-enabled Telehealth monitoring capabilities for Renown’s four Intensive Care Units (ICUs), as well as Renown patient Telehealth and virtual visits. Monitoring Remote Home systems with Masimo during the COVID-19 pandemic, where some patients received hospital-level care in the comfort of their own homes while Renown clinicians monitored and evaluated their data and plan of care. Serving emergency and disaster management for area hospitals, first-responders and the community with local, regional and statewide emergency and disaster management for sudden-onset emergencies. The RTOC is home to many different critical roles for our health system, including Transfer Center Nurses, Ride Line Coordinators, RTOC Coordinators and more, many duties of which each team member cross-trains on to be able to fill in whenever needed. While their roles may differ, their commitment to their patients remains the same – and they all work together to achieve the same outcome: delivering the right care, at the right time and place. “As an RTOC Coordinator, we do a variety of different things,” said Anna Schaffer, RTOC Coordinator. “We do triage coordination to help our nurses and hospitalists get patients in the emergency department admitted, and we also do bed control to find patients appropriate bed placement. Communication is important, so we always make sure to stay closely connected with the charge nurses on those floors.” “We start with a basic ‘need to know’ and place patients accordingly,” added Karly Brown, RTOC Coordinator. “We get surgery numbers, ICU capacity and discharges and find beds for all patients as quickly as possible. We have the advantage of being able to see the entire hospital.” “I primarily schedule transportation for patients at the hospital who are either going home or going to a skilled nursing facility,” said Sarah Clark, Ride Line Coordinator. “I get requests from case managers to schedule rides, and I work with REMSA and other ambulance services to schedule them. It relies a lot on appropriate and efficient communication and critical thinking.” Patients in facilities across northern Nevada and northeastern California, especially the rural communities, look to the RTOC to help guide ambulances, bed coordinators and hospital staff in finding care for our rural patients. “As a transfer center nurse, I facilitate incoming patients from rural facilities in Nevada and surrounding areas in California,” added Meg Myles, Transfer Center Nurse Specialist. “There are days we may take up to 30 direct admissions from these areas.” “We are the point of contact for inter-facility transfers, whether we are sending patients out or bringing them into Renown,” said Lisa Lac, Transfer Center Nurse Specialist. “We take phone calls from those rural areas, identify what services are needed, connect them to the appropriate provider and coordinate any transfers.” “Simply put, we are the bed wizards,” said Addison Rittenhouse, RTOC Coordinator. The RTOC team continues to break barriers and push the boundaries of medical excellence through leveraging the technology at their fingertips and their unwavering dedication to the health of our community. Inspiring a new era of medical possibilities, these team members have achieved a multitude of accomplishments for both their department and their patients since the birth of the center. “We have significantly reduced the time it takes to get patient admit orders in, thanks in part to the new Triage Coordinator role, and we provide easier access for patients to transfer to us from other facilities,” said Beth Rios, RTOC Coordinator. “We have taken a bigger role in helping the smaller hospitals in our area in caring for patients and improve patient throughput.” “As a team, we’ve done a lot of work in creating an engaging and positive environment, and our internal morale committee has been a huge help with that,” said Kelli McDonnell. “We’ve been working tremendously over the last year and taking all the feedback that we received from the Employee Engagement Survey to make improvements. We had 100 percent survey participation within five days, which is incredible.” “I am so proud of our escalation and problem-solving skills,” said Becca Dietrich, RTOC Coordinator. “When an issue is raised to us, we will always find a timely solution on our end so our care teams can focus on the issue in front of them. We are the eyes in the sky, seeing movement everywhere.” Each day in the life of our RTOC team members is a testament to their commitment, resilience and timework, making a profound impact on countless lives.
Read More About Department Spotlight: Renown Transfer and Operations Center
-
A Friend to Veterans, A Friend to Renown
Did you know that 218,000 veterans and their families call Nevada home? That is almost 7% of our total population who served this country and will require quality access to healthcare at some point in their lifetime. When faced with a daunting diagnosis or procedure, such as cancer or surgery, Renown rises to the occasion to provide veterans and their loved ones with the highest caliber of care possible to protect the lives that protected ours. Accessing that care, however, can be a challenge for some. As Renown serves veterans across 100,000 square miles, veterans living in rural communities often must travel long distances – with the costs of overnight lodging standing in the way, making healthcare access out-of-budget, and sometimes, nearly impossible. That’s where Veterans Guest House comes in. Veterans Guest House provides veterans and their families with temporary overnight accommodations while receiving medical treatment in the Reno/Sparks area. Founded in 1993 in response to the growing number of veterans sleeping in their cars to access healthcare, the nonprofit embraces veterans and their families who would otherwise not be able to obtain the medical care they need because of inabilities to pay for overnight lodging. A support system for veterans, especially veterans who are senior citizens, is vital to their overall health and well-being – and seniors at Veterans Guest House never have to feel alone in their care journey. Enter Dyana Parks, a senior care assistant working with Veterans Guest House. A friend to Renown Health and the William N. Pennington Cancer Institute, Dyana goes the extra mile for seniors staying at Veterans Guest House – she not only helps them navigate the logistics of their care, but she also is one of their biggest mental well-being champions. A Helping Hand for Guests in Need A proud member of a veteran family herself, senior and veteran in-home care is a family affair for Dyana. With a sister experiencing post-accident brain damage, elderly parents – one of whom facing dementia – and a son and daughter-in-law in the same field of work, Dyana has a unique passion for in-home and dementia care and holds several decades of hospice experience. As such, when she was assigned to help the clients at Veterans Guest House in September 2022, it was a natural fit for her, and she immediately jumped into action. Dyana takes special time during her work hours to transport seniors in need to their appointments at Renown (and keeps track of all of them), sits with them through chemotherapy and radiation treatments, ensures patients stay hydrated and nourished after major procedures, picks them up from surgery and always ensures everything goes well with each patient’s care. When patients coming from Veterans Guest House need extra emotional support, Dyana is always there to make sure they are okay and push them to keep going. “I always say to my seniors, ‘never give up,’” said Dyana. “If a need arises, I am there to help. I love getting to know my clients and helping them go home healthy.” As a ‘frequent flier’ at Renown and the William N. Pennington Cancer Institute, many of our team members are thrilled when they see Dyana walking through the doors with her clients, as they know that their patient is going home with one of their strongest advocates. To Dyana, Renown is akin to a family for both herself and her clients. “I love Renown,” said Dyana. “Everyone there makes my clients feel as though they are more than just a patient – they make them feel like family, especially when going through a scary diagnosis like cancer. As someone who has been going there with my own family forever and who now guides veteran seniors through the process, I will always recommend Renown to anyone.” Dyana emulates exactly what it means to make a genuine difference in the health and well-being of our community, all while raising awareness for both Renown and Veterans Guest House. “More people need to know about Veterans Guest House,” said Dyana. “When I came here, I was in awe. They do so much for every guest, making them feel comfortable at home while not having to worry about finances. Almost everyone that comes here, whether it be from the rural surrounding towns or all the way out to Alaska and even the Philippines, needs treatment of some kind, and I know Renown will always give them the best care.” To learn more about Veterans Guest House, visit veteransguesthouse.org.
-
Department Spotlight: Patient Access
Health systems across the country recently celebrated Patient Access Week from April 2-8. Join us in recognizing our Patient Access team at Renown! Fighting the Good Fight starts the moment a patient steps onto the grounds of our health system. When patients visit Renown on their healthcare journey, they look to the experts to not only help them navigate through the complexities of the process but also ensure their experience with us starts off on the right foot. Renown Health’s Patient Access Representatives (also referred to as “PARs”) are the faces of this entire process. As the key links between patients, providers and insurers, they strive to create a welcoming and respectful environment for everyone. PARs are committed to providing all of Renown’s patients access to the quality care when needed. After all, it’s in their name! A Friendly Face PARs are the front faces of almost all clinical areas at Renown. As the starting point for much of the patient experience, the day-in-the-life of PARs can vary. Checking patients in and out, getting demographic information, verifying insurance, answering phone calls, fostering communication between patients and their care teams, scheduling patients for follow-ups, explaining financial responsibilities and our financial aid programs, creating an overall positive experience and environment, the list goes on – but they all remain united under one goal: setting patients off on the right foot as they access care through our health system. “Each day, PARs are met with new patients who are seeking solutions to different concerns,” said Macy Betts, PAR for Renown Women’s Health. “We are the front doors to this department. We are not just checking patients in and out; we are the first step to the patients receiving the care they deserve.” “We take pride in our work,” added Tanya Quintanilla, Shari Longley and Nancy Arroyo Garcia, PARs for Renown Pediatrics. “Usually, we are the first point of contact within Renown, so we don’t take our role lightly. For example, when we see a newborn, we must ensure the registration has been verified, which consists of patient demographics, patient preferences and insurance verification. We need to be consistent and thorough because what we do affects every point of contact a patient may have within Renown.” “As my team’s senior PAR, my day begins with gathering the outpatient therapy work queue numbers and assigning the team to work them,” added Logan Johnson, Senior PAR in Pre-Registration at Renown. “Our goal is to contact and schedule patients for physical, occupational and/or speech therapy as soon as possible so that they have the maximum benefit and can get back to a normal life as quickly as possible. Our encounters can make or break the entire experience.” PARs never underestimate the power of good communication and compassion. Even during the busiest of times, our PARs work diligently to ensure all patients and their care teams fully understand the administrative side of whichever part of their journey they are about to embark on, lending a helping hand and a smile. “Whether you’re communicating with patients, leaders or coworkers, communication is key,” said Jonathan Figueroa, PAR for the Renown Institute for Heart & Vascular Health (IHVH). “We try and make sure that we do everything possible to make their visit go as smoothly as possible.” “Communication makes the world go round,” added Keith Madrona, Sherry Riley, Erika Rios and Andie Kilpatrick, PARs at Renown Urgent Care – Ryland. “Having a friendly attitude and demeanor is very important. “The PARs in Labor & Delivery do so much more than just registering patients – from escorting expectant parents to their rooms, welcoming newborn babies, processing pre-estimates and more – and the patience and excellent communication I receive from other teams is what keeps me going,” added Nanci Barash-Vietti, PAR for Renown Labor & Delivery (L&D). “This is critical to the success and effectiveness of the PARs in our department.” Shift changes for PARs mimic other teams at Renown, leveraging technology and both written and spoken communication to ensure the next shift begins successfully. "When I come in, the night shift will give me a report on what is going on and what the schedule looks like during the day; then I log in to my computer and get everything that I will need for that day up on the screen,” said Allie Boracchia, PAR for Renown L&D. “Usually around this time we have a 7-8 a.m. induction scheduled for the first patient, so I will grab the pre-made packet that the night shift put together, the unit clerk will call the nurse to get a room number, and I take the patient to the room and have them sign all the forms. After the patient has the baby, then we admit them and finish registration. This is continuous all day long.” Our PARs all agree that regardless of the setting, whether it be emergent or routine, every patient is looking for that advocate from the moment they enter through our doors. “Being friendly, patient and understanding is a must,” said Sheryl Lundgren, PAR for the William N. Pennington Institute for Cancer. “It is so nice being able to brighten the days of patients who are living with a cancer diagnosis.” “In the urgent care setting, a lot of the patients we see are not feeling their best, so it is important that we show them we care and are here to help make check in go smoothly,” added Sam Deithrich, PAR at the Renown Urgent Care – Los Altos. “Patients are relieved that they are speaking to a real person that will help set up appointments,” added Rick Jordan and Celeste Landry, PARs in Lab Services at Renown South Meadows. PARs embrace lifelong learning at Renown, especially as their roles differ day-to-day. They are always ready to jump in and assist on tasks that might be new for them, growing their skills on the job and never hesitating to say, “How can I help?” “As a PAR, you are always learning new things, even when it seems like you know just about everything,” said Liz Cardenas-Ramos, PAR for Renown Endocrinology. “It’s been such a positive experience.” “Giving yourself grace to learn and grow in Patient Access is the key,” said Maggie Savoie, PAR for Renown Primary Care – Fernley. “I find myself learning every day at Renown, and if you’re learning, you’re growing. Being able to take a breath and say, ‘this is a learning opportunity for me, and tomorrow I will be better a better PAR because I’ve gained this knowledge’ is an amazing way to stay positive in the position.” “In L&D, we are all multi-tasking, and every day I am learning something new about my department and patients, as well as how to excel in my position,” added Nanci Barash-Vietti. Renown PARs are the front lines to health care access, and they wear that badge with pride. Jeanette Flores, PAR in the Emergency Department at Renown South Meadows, sums up the role of Patient Access well: “Talk about first impressions!” “I am proud of our team and the excellent care we give our patients,” said Dawn Linker, PAR for the Renown IHVH. “We want them to have a good experience.” Impactful Accomplishments The role of our Patient Access team members goes beyond the desk. A patient’s healthcare journey begins, and sometimes even ends, with the helping hands of our PARs, leaving a lasting positive impression of Renown. "Our interactions with the patients make a difference before they see the provider, so we always demonstrate a welcoming and helpful atmosphere for the patients to feel like their needs are being met,” said Mary Dettling, PAR for Renown Endocrinology. “I love seeing the difference we make in peoples’ lives,” added Shannon Leone, PAR for the Stacie Mathewson Behavioral Health & Addiction Institute. “We can get patients at their toughest and worst times. Watching them overcome their fears, traumas and addictions has been very rewarding.” Our PARs don’t just make goals for themselves – time and time again, they surpass them, all in the name of patient experience and excellence. “We have not only met our monthly point-of-sale scores, but we also have exceeded our stretch goal for the last eight months and our scores have been in the 50th percentile or higher,” said Jeanette Flores. “Along with being the top point-of-sale collectors, we have also been known to be some of the sweetest and most helpful staff at South Meadows,” said Katie Morrill, PAR in the Emergency Department at Renown South Meadows. As their teams grow, so does their impact on our patients. PARs are dedicated to providing the best customer service possible, and with their expanding teams, that service goes even further, even throughout the pandemic. “A year ago, we only had one PAR; now, we have a full and amazing team,” said Alex Bucholz, PAR for Renown Advanced Wound Care. “We have come so far in a short amount of time.” "During the pandemic, we have maintained a core group of individuals who come in every day and help keep this office and all its parts moving smoothly,” added Shannon Leone. “We have maintained a full patient load the last three years and never had to close our office for any reason. We have even had the opportunity to start our Medicated Assisted Treatment and Transcranial Magnetic Stimulation programs.” "We successfully operated and maintained our pediatric COVID clinic, which is the only one within our five clinics,” added Tanya Quintanilla, Shari Longley and Nancy Arroyo Garcia. “We feel proud knowing our tiny humans are protected with the COVID vaccine.” Like many other teams at Renown, our PARs are masters at teamwork. Despite any obstacles that may happen along the way, they are always there for each other to ensure every patient gets the care and attention they deserve. “We call ourselves the ‘A-Team’ here in Pulmonary,” said Shannon Birnberg, PAR for Renown Pulmonary & Sleep Medicine. “We have persevered through changes, additions and departures. We are most proud of bringing different personalities to the team and being super strong and effective.” “I have noticed the team always steps up whenever needed,” added Brittany Hughes, PAR for the Renown IHVH. “Everyone has a great attitude and is very positive!” “While our team is fairly new, we are growing together, learning our strengths and weaknesses and always pushing for stronger unity,” added Angel Freer, PAR in the Emergency Department at Renown Regional. When our PARs find ways to simplify a process or make a workflow run more efficiently, they don’t waste any time in making that happen. They take any opportunity to enhance patient experience. “Our team came up with a solution on how to get patients registered faster,” said Jess Castillo-Marquez, PAR in Lab Services at Renown Regional. “We came up with modalities which assign each PAR their own procedure in which they will be registering for during their scheduled shift. It has been a great success, helping our productivity and keeping our patients satisfied with our service.” “We are proud of our successful implementation of our new therapy workflow,” added Logan Johnson. “Patients are now waiting much less to be contacted about their care.” Our PARs know that teamwork makes the dream work, and their commitment to the patients they serve – and the goals they continue to blow out of the water – continue to inspire them daily. “You are only as strong as your team,” said Aundie Yonker, PAR in the Emergency Department at Renown Regional.










.jpg?rev=ddb15541cee845129a2355ba27384fb5)