Search
-
What is Polycystic Ovary Syndrome (PCOS)?
Dr. Carilyn Hoffman with Renown's Women's Health explains the symptoms, causes and treatments of Polycystic Ovary Syndrome (PCOS) (also referred to as Polycystic Ovarian Disease (PCOD)), a prevalent condition among women of reproductive age that influences hormonal balance, metabolism and fertility. Make an appointment with Renown Women's Health Click here to schedule Call to schedule: 775-982-5000 PCOS Defined PCOS is a constellation of symptoms characterized by two of the three criteria: multiple small cysts on the ovaries visible via ultrasound, irregular periods and signs of hyperandrogenism. Other symptoms include infertility, insulin resistance, and increased risk of cardiovascular disease. Symptoms of PCOS The symptoms of PCOS can vary from woman to woman, but some of the most common include: Irregular menstrual cycles: This is often one of the first signs of PCOS. Women may experience fewer than nine periods a year, more than 35 days between periods, frequent spotting, and/or abnormally heavy periods. Excess androgen levels: High levels of male hormones may result in physical signs such as excess facial and body hair (hirsutism), severe acne and male-pattern baldness. Polycystic ovaries: Enlarged ovaries containing numerous small cysts can be detected via ultrasound. Causes and Risk Factors The exact cause of PCOS is unknown, but several factors may play a role: Genetic predisposition: A family history of PCOS increases the risk. Insulin resistance: High insulin levels might increase androgen production, causing difficulty with ovulation. Obesity: Women with elevated BMI’s are more likely to have PCOS, although 20% of women with PCOS are not obese. Diagnosis and Treatment Dr. Hoffman outlines that diagnosing PCOS requires a medical history review, a physical exam, blood work and an ultrasound to evaluate the ovaries. Treatment options can range from lifestyle modifications, like diet and exercise and weight loss, to medications for menstrual regulation, fertility assistance, and rarely surgery. Lifestyle Changes A healthy lifestyle is a cornerstone of managing PCOS. Regular exercise, a nutritious diet, and weight management can help reduce symptoms and the risk of long-term health issues. In overweight patients, weight loss as little as 5% has been shown to improve symptoms of PCOS. Medication Medications may include hormonal contraceptives to regulate menstrual cycles, anti-androgens to reduce hair growth and acne, and Metformin to address insulin resistance. Fertility Treatment For women with PCOS who are trying to conceive, ovulation induction with clomiphene or letrozole is sometimes necessary. Sometimes a referral to a reproductive endocrinologist and infertility specialist is needed for more advanced technologies like IVF. Health Implications PCOS is not just about cystic ovaries or irregular periods; it can have profound implications on a woman's overall health. Women with PCOS are at an increased risk for several conditions, including type 2 diabetes, high blood pressure, heart disease, and endometrial cancer.
-
Importance of Safe Sleep
In today's fast-paced society, it is understandable for parents to want to take shortcuts in caring for their little ones. A s a result, It is tempting to leave a sleeping infant in a car seat or swing after a long day of errands or when you need a moment to catch your breath. But, as convenient as these devices may be, they pose a serious risk to your child's safety. Why Car Seats and Swings Pose Risks for Infant Sleep Car seats, swings, and bouncers are quick and convenient ways to feed, hold, and sleep an infant. Not out of malice or discontent, but again from the need for quick and easy access to baby care in an already busy lifestyle. However, the risks outweigh the benefits. The American Academy of Pediatrics (AAP) states that “infants should be moved to a crib, bassinet, or play yard for sleeping as soon as is practical.” If a parent must use a car seat or other sitting device, they should only do so for a short period of time and never as a substitute for a proper sleeping environment. Leaving a sleeping infant in a sitting device, such as a car seat or swing, can create unsafe sleeping conditions. The American Academy of Pediatrics (AAP) warns that doing so increases the risk of sudden infant death syndrome (SIDS) and positional asphyxia. This is because infants can easily slump over or become entangled in the straps, blocking their airway, and causing suffocation. Car seats, swings, and bouncers are quick and convenient ways to feed, hold, and sleep an infant. Not out of malice or discontent, but again from the need for quick and easy access to baby care in an already busy lifestyle. However, the risks outweigh the benefits. The AAP states: Infants should be moved to a crib, bassinet, or play yard for sleeping as soon as is practical. If a parent must use a car seat or other sitting device, they should only do so for a short period and never as a substitute for a proper sleeping environment. Leaving a sleeping infant in a sitting device, such as a car seat or swing, can create unsafe sleeping conditions. The AAP warns that doing so increases the risk of sudden infant death syndrome (SIDS) and positional asphyxia. In addition, infants can easily slump over or become entangled in the straps, blocking their airways and causing suffocation.
-
What Does a Doula Do?
If you’re expecting a new baby, you may have been given the advice to hire a doula. You may have seen statistics of improved outcomes among those who’ve had a doula attend their birth. Perhaps you’ve heard that the etymology is from the Greek word meaning “to serve.” But how does a doula serve their clients? A doula is a non-medical birth professional who will guide you through labor, birth, postpartum and beyond. Your doula can discuss your options with you so you can make informed decisions, as well as provide emotional and physical support to ease your experience. While each doula offers their own style, there are certain services that most doulas will provide for their clients. Typically, a birth doula will provide at least one prenatal visit, one postpartum visit and continuous support during active labor. A postpartum doula usually provides support during the 12 weeks immediately following birth, sometimes referred to as the “fourth trimester,” but some will continue care after that as well. Simply put, a doula provides informational, physical and emotional support during the childbearing year(s). Let’s take a closer look at these three ways a doula can support you. The Basics If you don’t know your options, you don’t have any. This is a common phrase in the world of birth work. When you’re in labor, you’re exhausted, in pain and there’s often urgency inherent or implied in any choices you make. So, when an intervention is offered, many birthing people accept it without question. One method that can help the decision-making process is to check your BRAIN: Benefits: What are the benefits of the proposed intervention? Risks: What are the risks of the proposed intervention? Alternatives: What are the alternative options? Intuition: What does your intuition tell you? Nothing: What if we do nothing? What if we wait? When you’re in active labor, you might have difficulty remembering this acronym; that’s where your doula comes in. At your prenatal visits, you can ask your doula for guidance in preparing your birth plan, which can include contingencies for certain potential interventions. And as choices arise during labor, your doula can guide you through the benefits and risks and can provide you with alternative options you might not otherwise be aware of that are available to you. Your doula can remind you to check in with your intuition and can help you quiet your mind so you can listen to your instincts. The Body Although we tend to see depictions of people giving birth on their backs with their feet in stirrups, this is only one of many ways to give birth. Walking and dancing can speed up early labor. Side-lying or hands-and-knees can prevent tearing during the pushing stage. Sometimes labor stalls, and a change of position is often helpful to get things moving again. Your doula can suggest positions depending on your stage of labor. Some labor positions might require the support of another person – your doula could fill this role or assist your partner in doing so. Some doulas also provide massage or even acupressure, and most will do the “hip squeeze” that so many laboring people swear by. If your baby is presenting posterior, or “sunny side up,” your doula can apply counter pressure to alleviate back pain during labor. Some postpartum doulas will do light housework while you rest and bond with your newborn. Others might care for your baby through the night so you can catch up on sleep. Many doulas have also gone through additional training to offer breastfeeding support and may be able to assist you with latch issues and nursing positions. The Mind Pregnancy, birth and postpartum periods can be some of the most emotional times in a person’s life. A doula will hold space for you and help you process your emotions before and after birth. It’s normal to feel apprehensive, or even fearful, about labor and birth, and discussing these feelings is the first step. A doula can help you navigate your concerns in a safe space so you can be prepared emotionally for your upcoming labor. Many doulas will also guide you through writing your birth plan, which can lessen anxiety about the unknown. If you have a history of trauma, your doula can assist in communicating this, so you don’t have to relive the experience every time you meet a new medical provider. Most people will experience some form of what’s often called the Baby Blues in the immediate postpartum period. The third day after birth tends to hit hard, as hormones attempt to regulate, but the Baby Blues can continue for weeks for some new parents. A postpartum doula’s support can be incredibly valuable during this time. When the baby blues last longer than a few weeks, it could considered a mood disorder. Most doulas will recognize signs of postpartum mood disorders and will have resources available for additional support. Choosing the Best Doula for You With so many wonderful doulas in northern Nevada, you might wonder how you could ever choose just one to attend your birth. Some expectant parents are unfortunately restricted by cost. With so many expenses related to a new baby, it can be difficult to budget doula services as well. Thankfully, Nevada Medicaid now covers doula care, and some commercial insurances are following suit. Check with your insurance company to find out if they might cover part of the cost for hiring a doula. If your insurance doesn’t cover doula services, some doulas offer a sliding scale based on income. You may want to interview multiple doulas to find the right one for you. If you’re the kind of person who wants all the information you can get, a more detail-oriented doula might be the best choice. But if you tend to feel overwhelmed by too many options, you might prefer a doula who only offers additional information as the situation calls for it. If you want massage or acupressure during labor, you might want to hire a doula with those certifications. Or maybe informational and physical support are not as important to you as emotional support, in which case your best choice could be a doula who has experience with postpartum mood disorders or trauma support. Regardless of who you hire, be sure to clearly communicate your desires and expectations – not just for your birth, but also for your doula. The most important thing when choosing your doula is trusting your gut. You need to feel comfortable with your doula, as they’ll be tending to you at one of the most vulnerable times in your life. When you find a doula that you click with, who listens to you and supports your choices, you have found the best doula for you.
-
A Fighting Chance at 24 Weeks Sloans Story
Most babies weigh just one pound and are roughly the size of an eggplant when they reach 24 weeks of development inside the womb. It is a crucial stage when internal organs begin functioning, and the babies' respiratory and central nervous systems are still developing. So, in November 2021 when Kallie Johnson experienced a premature rupture of amniotic fluid around this point in her pregnancy, her care team in Winnemucca decided to transport her via Care Flight to Renown Regional Medical Center. The team at Renown Children’s Hospital immediately began discussing the risks of delivering at 24 weeks with the Johnson family. Moving Forward with Hope Knowing the stakes, Kallie remembers never feeling rushed to decide about delivering her baby preterm. “I felt educated and supported by my care team at Renown throughout our entire stay, starting with the education they provided about what it meant to deliver my baby early,” Kallie said. “The team really helped me make the best decision for myself and my family.” Together, Renown employees and the Johnson family moved forward with a healthy set of nerves and a powerful feeling of hope. Weighing in at one pound 11 ounces, Sloan entered the world on Nov. 19, 2021, via emergency Cesarean section. Her birth was classified as a micro preemie because she was born before week 26 of pregnancy and so small that she fit inside the palm of her father Sterling’s hand. A full-term pregnancy is classified as reaching 39 weeks. A Fighting Chance Called a fighter by many Renown Children’s Hospital care team members, Sloan spent over five months in the neonatal intensive care unit (NICU). She was placed on a ventilator, fed through a feeding tube and monitored 24/7, overcoming daily challenges with the Renown team and her family. As a result of being born prematurely, Sloan developed a grade one brain bleed and a congenital heart defect called patent ductus arteriosus, a persistent opening between two major blood vessels, causing too much blood to flow to the lungs and heart. To meet the oxygen needs of her tiny lungs, Sloan was intubated and developed a severe oral aversion and high-arched palate as a result. The effects would lead to difficult developmental and physical challenges that she still conquers today. Yet, with the help of her care team – including physical, occupational and speech therapists, dieticians and doctors – Sloan continues to make progress every day.
-
11 Tips Caregivers Need to Know
Becoming a caregiver or playing a more active role in another’s healthcare is a big responsibility. At some point, almost all adults will support an aging parent or a loved one in need. Keeping track of their needs and wellbeing, while also prioritizing your own can become overwhelming. It’s important to know: you are not alone, and help is available. Read on for 11 tips to help you manage your time, your own wellbeing and your loved one’s care. Self-care comes first. When your main priority is the person in your life who needs care, it’s easy for your own needs to take the backseat. Give yourself time each day to focus on your personal wellbeing. It’s hard to give a loved one the care they need if your own needs are not met. Prioritize the Activities of Daily Living (ADL). Make a note of what ADLs your loved one can do alone, what they need help with and what activities require the most help. This will help you work through the day with them, as well as plan out how the day’s activities will go. Do a home safety audit. Do showers, bathtubs and steps have safety grab bars? Look around the house for additional tripping hazards, like rugs or electrical cords. If your loved one struggles with day-to-day navigation of the home, consider scheduling an occupational therapy appointment. This type of therapy helps a person develop or maintain the motions required to accomplish daily tasks. You might also qualify for a referral to in-home healthcare, such as Home Care. Have the hard conversation. The best time to discuss views about end of life care and to learn what choices are available is before a life-limiting illness or crisis occurs. With advance care planning, you can help reduce the doubt and anxiety related to decision making at the end of life. Completing an Advance Directive is a great tool to sort out all these decisions before they’re needed. Attend a free workshop to learn more and complete this important document. Identify when you need respite. Respite care involves receiving a short-term break from caregiving. Organizing in-home care for your loved one will allow you to step away and tend to your needs. By identifying what kind of respite care you are seeking, you can find the right person to provide you with that much-needed break. Don’t wait until you feel overwhelmed, plan ahead. Write down insurance contact information. Have a direct connection to the right insurance professional for support and advice. If your loved one is eligible Medicare, this is a good opportunity to review their current selections and if they would benefit from a Medicare Advantage Plan or Medicare Supplement Insurance. Seeking out expert advice or information on Medicare options is a great way to navigate this. Consider calling a broker, or attend a free educational seminar with Senior Care Plus. Gather legal and financial information. Make a list of all existing legal documents and financial accounts that your loved one has. These might include a will, advance directive, power of attorney, bank accounts or investment accounts. If you have questions about how to manage them, or need assistance in setting up additional framework, reach out to a lawyer, legal service, financial adviser or bank representative. Create an inventory of medical information. Identify where all of your loved one’s medical records are, as well as a list of providers or healthcare practices where they have received care. Consider if you should have your loved one give you Proxy Access in MyChart, which allows you to access all the features in MyChart on their behalf, including viewing upcoming appointments, viewing test results and emailing a doctor on their behalf. Make a list of what others can do. Think about all the little (and big) things that need to happen, and write down tasks that others could take care of you. When someone says “let me know what I can do” you’ll be ready with a pre-written list of items they may be able to assist with. Tasks could include tackling around-the-house repairs, scheduling lawn work, helping to walk the dog, taking a car for an oil change and cleaning. Find programs and events for social enjoyment. If and when possible, seek an activity outside of the home. Look for community centers that have programs for seniors, recreational activities or meals that you can patriciate in together. If leaving the home is not an option, arrange for visits or in-home activities, such as movie nights, card games or time to visit with family. Research long-term options. If you will be considering a nursing home or assisted living, make a list of amenities that you and the person you are caring for would like. Take this list with you when visiting potential locations to make sure you don’t forget to ask about each item.
-
Get Ready for Baby with Childbirth Classes
By taking our pregnancy and birth class, you will gain the tools necessary to have a safe and empowering birth experience for both you and your baby. Chris Marlo, Childbirth Educator at Renown Health explains why birth classes are important. For questions regarding classes or tours, contact Chris Marlo: chris.marlo@renown.org 775-982-4352 What is a Certified Childbirth Educator/Doula? If you are expecting a baby, Renown has a wide variety of classes to help prepare you for birth. Classes are taught by certified childbirth educators and doulas. A certified childbirth educator is a trusted resource who has a passion for educating expecting parents about childbirth, and will provide you with non-biased, evidence-based information. A doula is a professional labor assistant who provides physical and emotional support during pregnancy, childbirth and postpartum. As you prepare for birth, our certified educators will guide you each step of the way and ensure you receive the quality care you deserve.
-
Department Spotlight: Customer Engagement Center
Do it for the patient. That’s the motto that each employee in the Customer Engagement Center (CEC) lives by every single day. This team spins all the existing stereotypical thoughts about call centers on their side by empowering and partnering with patients to achieve their best health. Being transferred around several times just isn’t in this team’s DNA – being a one-stop-shop for patient scheduling, referrals, insurance matters and more is how they proudly operate. Through elevating the customer engagement experience, the CEC closes care gaps to ensure patients get the right care at the right time. From employees who work from our home base in Reno, all the way to the southeastern corner of Florida, this primarily remote team stays firmly connected and collaborative to make patient care possible for all Renown Health patients and Hometown Health and Senior Care Plus members. The “Make It Happen” Department Back-to-back phone calls about a wide variety of patient needs? They make it happen. Referrals that need to go directly to the provider? They make it happen. Complex insurance questions that need to be resolved? They make it happen. The CEC is the keeper of all things customer service and all things patient satisfaction, leveraging technology to improve engagement and accessibility – and they wear that badge with pride. “Patient care is our first priority,” said Cindy Arevalo, Supervisor of Customer Engagement. “Even though we aren’t face-to-face with them, we are always there to help them over the phone with whatever their needs are.” The CEC has a lot of different sub-departments under its umbrella: scheduling, referrals, insurance, patient outreach, personal assistants, MyChart customer service and more. Each team handles calls for a different section of our health system, including the hospitals, imaging, primary care and specialty care. While their individual teams may be different, one aspect of their jobs remains the same: they care. Deeply. “We advocate for the patient, especially when they can’t advocate for themselves,” said Amanda Ishii, Referral Specialist. “We are the first people that patients speak to, and we all have empathy to listen to them, help them solve their problems and take as much time as they need to care for their needs,” added Susana Arroyo Garcia, Supervisor of Customer Engagement. Customer loyalty is key to the CEC. Every CEC team member builds strong relationships with patients and members. Whether they manage patient outreach or manage back-to-back inbound calls, each employee feels a special connection to the helpful work they do to solve a variety of patient concerns. “As Senior Care Plus Personal Assistants, for instance, we help guide our members through complex situations, and we eliminate the process of transferring them to different departments, becoming a ‘one-stop-shop' for them,” said Stephanie Perez Campbell, Senior Care Plus (SCP) Health Coordinator. “While every day is different, we are constantly learning new things and helping members navigate through the health system." With the 4.5 million calls the CEC handles per year, the nature of their jobs is undoubtedly fast paced. However, this does not intimidate the CEC team members; instead, it inspires them to continue reaching new milestones, helping thousands of patients and members every year by handling all the scheduling and referral work on the backend so that they can receive the care needed. “I never find myself sitting around asking, ‘what should I do next,’” said Gina Briles, Supervisor of Customer Engagement. “We always support each other to stay on top of it all in order to take care of our patients.” By wearing a lot of hats and managing many different work queues all while staying engaged with each patient, the CEC is full of natural problem-solvers, helping our healthcare network run smoothly. “The Engagement Center is the front door for the community; serving as the voice of the customer, we ensure patients do not fall through the cracks of the complex healthcare system and are able to easily access the right care at the right time through an exceptional experience,” said Candace Dietrich, Director of Customer Engagement. Consistently Connected With thousands of referrals to process and millions of calls to field, the ways the CEC stays connected to patients and members as well as each other can be related closely to magic. No concern goes unnoticed, and no problem is too complicated. “The sheer volume of patients we engage with is incredible,” said Rene Jacinto, Manager of Customer Engagement. “We processed nearly 200,000 referrals and authorizations last year.” “We expect a steady increase of calls year-over-year. My team processed 1,259 referrals in one day alone recently,” added Arielle Gomes, Referral Specialist. A superpower that every CEC team member holds is the ability to listen. According to this department, active listening is key when problem-solving with every patient and member, as that skill helps them anticipate patient needs and resolve their issues quickly and efficiently. “I’ll always listen,” said Alex Gomez, Customer Engagement Representative. “I want them to know that they are in good hands, especially when they are feeling scared or frustrated.” Team members like Alex help carefully guide customers through the Hometown Health and Senior Care Plus enrollment process, increasing membership and engaging patients to find the perfect plan for them. One of the largest challenges the CEC faces is the departures and arrivals of providers. The ebbs and flows of all hospital systems include provider departures and shifting provider availabilities. Despite this challenge, the CEC staff work hard to ensure communication with all patients regarding provider changes is consistent and that all patients are scheduled in a slot that works for both their schedule and the provider’s schedule. “It’s important for us to be flexible, because things can change at a moment’s notice,” said Gina Briles. “This is more than just a job – we are here for our patients. What we are doing impacts everyone.” Throughout all times of transition, the CEC builds robust relationships with both patients and providers within our organization and community, a skill that this team emphasizes as “fundamentally important.” For example, SCP Personal Assistants like Stephanie Perez Campbell will coordinate care with community resources and offices, giving members one less call to make and one less hurdle to cross in order to get the care they need. On top of it all, even though this team has the ability to work from all 50 states (and many of them work outside of Nevada!), every employee feels connected to their colleagues and their work. “This is the best group of people I’ve ever worked with,” said Riley Petro, Manager of Customer Engagement – Imaging. “I am super lucky for this job and am so thankful for these people.” Proud and Powerful The proof is in the pudding – or rather, the proof is in the numbers. Within the 4.5 million calls they successfully field every year, approximately 1.6 million of those calls route through the private branch exchange (PBX) team – the team that oversees the main operator lines – under the guidance of Jess Nater, Supervisor of Customer Engagement. The CEC is also on track to handle nearly 300,000 referrals this year alone. Additionally, the Hometown Health CEC team was recognized nationally this year with a five-star rating from Medicare. “We all have the initiative to grow, and because of this, we are always learning something new,” said Cindy Arevalo. “Our leaders also support our growth, especially if we want to skill-build or advance in our careers.” The CEC is frequently the first stop on the career ladder for many employees as they start their journey in healthcare, and CEC leadership is committed to the growth and development of their teams to reach their career goals at Renown. The secret formula for all this success can be in part attributed to the pride each CEC employee has for their team, their work and Renown. “We have a very supportive team,” said Holly Coffey, Supervisor of Customer Engagement. “I’ve seen our leaders support their teams tremendously.” “We rely on each other,” added Ashleigh Carty, Customer Engagement Representative. "I love the relationships we create with one another.” Employees in the CEC come from many walks of life, choosing to work at Renown and Hometown Health for a variety of different reasons, many related to the positive power our health system holds. Team members in this department hold a myriad of different career backgrounds, including pharmacy technicians, medical assistants, population health professionals, community health workers and more. Some team members, like Nikki Clifford, Customer Engagement Representative Lead, heard wonderful things about Renown from her mother, who also works for Renown. According to Nikki, “seeing how happy my mom has been in her career made me want to join too. I’ve loved it here ever since.” Katie Lunau, Supervisor of Customer Engagement, also grew up in a family involved in healthcare, and she wanted to follow in their footsteps. Choosing Renown as the place to follow her family path was a simple one, because “Renown stood out as the company that was actively involved in the community helping others.” For other team members, like Susana Arroyo Garcia, Ashleigh Carty and Stephanie Perez Campbell, Renown and Hometown Health’s impact on the local healthcare landscape was their primary driver for choosing a career here and in the CEC specifically. “Renown is very well-known in the area,” said Stephanie Perez Campbell. “I went to school in Reno for public health, so Renown came up all the time in my schooling. I knew Renown had a lot of different opportunities available for career growth, and with the friendly environment I always experienced here, it was an easy decision.” “Once I went through the interview process and joined the team, I immediately realized that there are outstanding managers, support systems and communication skills here. People genuinely care,” added Ashleigh Carty. Ashleigh is exactly right. As emphasized by every team member, employees in the CEC care. Their heightened levels of care and empathy set the bar high for all at Renown and Hometown Health, and their impact will be felt for years to come.
Read More About Department Spotlight: Customer Engagement Center
-
Plan Early: Completing Your Advance Directive
We plan for the birth of a child, weddings and retirement, but rarely do we discuss how we want to be cared for at the end of our lives. Getting through this challenging conversation and completing an Advance Directive can give you peace of mind that your loved ones will not have to make difficult choices on your behalf. The best time to complete an Advance Directive is now – don’t wait until a life-limiting illness or crisis occurs to discuss your views about end-of-life care and to learn what choices are available. By preparing in advance, you can help reduce the doubt and anxiety related to decision-making for your family if you cannot speak for yourself. What are Advance Directives? An Advance Directive is a document that states your choices about medical treatment and names another person to make medical decisions on your behalf if you are unable to. This document allows you to make legally valid decisions about future medical care. “Completing your Advance Directive is a gift you give your family,” says Director of Palliative Care, Mary-Ann Brown RN, MSN. “The stress associated with these difficult decisions is decreased if everyone knows what is important to you and what you want at the end of life.”
Read More About Plan Early: Completing Your Advance Directive
-
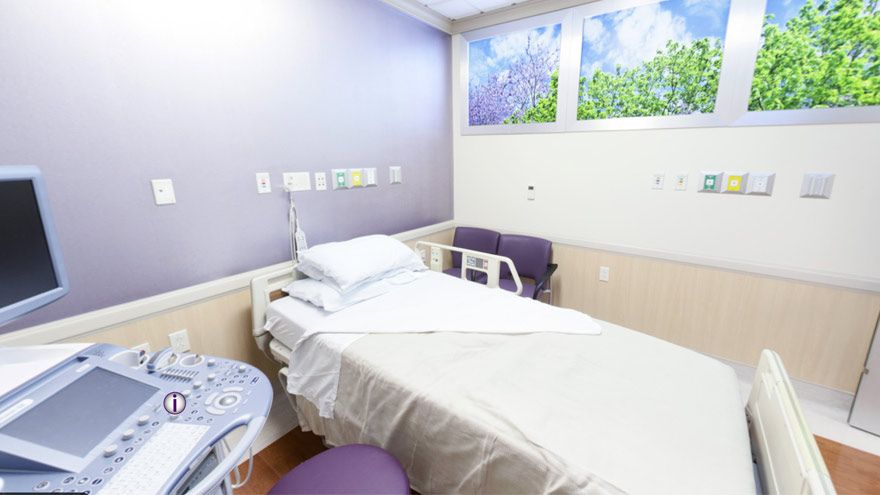
Remove the Guesswork with Renown’s Labor Assessment Area
Pictured above: A section of Renown’s Labor Assessment Area. When patients expecting a new child are about to give birth, nerves can be especially heightened. Questions flood their minds: Is the baby actually on the way? What’s going to happen next? Are we ready to push? Lucky for them, at Renown Health, the guesswork can finally end with Renown’s Labor & Delivery unit Labor Assessment Area. This unique space is a triage area that helps make more precise labor diagnoses by determining exactly what stage expectant parents are at in the labor process. Funded by a state grant more than a decade ago, the six-bed Labor Assessment Area sees 500-600 patients per month – from patients entering the unit directly, unsure if they are in active labor, to patients who are sent over from elsewhere experiencing labor symptoms, such as high blood pressure and water breaking. The area also serves as a pre-operation space for patients getting ready for procedures such as C-sections. The six cubicles that are enclosed with doors and curtains ensure each patient gets the private, one-on-one care they need. Furthermore, rather than sitting in a waiting room, this area allows expectant parents a comfortable place to prepare for labor. “We are a unit that prides ourselves on getting patients into beds very quickly,” said Debbie Hawley, Associate Nurse Manager in Renown’s Labor & Delivery unit. “This area has allowed us to triage more effectively and allow more patients to collaborate with their provider in a quick manner.”
Read More About Remove the Guesswork with Renown’s Labor Assessment Area
-
Estate Planning Mistakes to Avoid
August is National Make-a-Will month. We talked to Renown Health Foundation Planned Giving Officer, Abbey Stephenson, to learn more about wills, trusts, and estate plans and why you should feel motivated this month to get started. Did you know that 2/3 of Americans don't have a will or trust? If this is you, don’t worry, you’re not alone. Although there are laws in place to determine who inherits your assets if you die without a will or trust, having a will or trust ensures your assets go where you want them to go after you are gone. They can also help minimize disputes between family members and heirs about who gets what. In Nevada, the laws that govern who gets what if you die without a will or trust can be found in Chapter 134 of the Nevada Revised Statutes. There are other documents that people often prepare at the same time as their will or trust – like an advance health care directive and durable power of attorney for assets. These documents all together are called an estate plan. Although they have other purposes too (like nominating a guardian for a child, planning for disability or avoiding probate, which is a court process), wills and trusts are documents that say who will receive your assets after you are gone. The most common type of trust is often called a revocable living trust or a family trust. People who have a trust usually still have a will, although it is a shorter form of will called a pour-over will. It’s a good idea to talk to an estate planning attorney about whether or not a trust makes sense for your family or circumstances. Now that you’re ready to get started, here are some mistakes to avoid: 1. Failing to plan Not setting aside the time to plan may be the biggest mistake. Failing to prioritize preparing or updating your estate plan means your last wishes and desires may not be fulfilled. The right documents memorialize what you would like to happen upon your disability and death so that other people can know and follow your wishes with respect to your care and your assets. 2. Failing to coordinate beneficiary designations Certain types of assets like life insurance and retirement accounts are not covered by your will or trust and need to be addressed separately. These types of assets are referred to as non-probate assets because they transfer under contract principles and don’t require court supervision or probate to be distributed to the named beneficiaries. By completing beneficiary designation forms provided by the retirement account custodian, insurance company or financial institution, you can direct your assets to one or more beneficiaries. 3. Failing to title your assets properly Asset titling refers to how you own your asset – such as in your individual name, jointly with someone else, or in a trust or entity. For example, assets titled for two people with a “right of survivorship” will automatically go to the surviving owner. Review your asset titling and make changes, if needed, to ensure your property and assets are passed down the way you intend. 4. Failing to include charities meaningful to you In addition to providing for family members and other important people in your life, you many also choose to give to charities meaningful to you in your estate plan. When you include a charity in your estate plan, that gift is called a planned gift and many charitable organizations, including Renown, recognize such donations through their legacy giving societies. As you prepare to make your own will or a more comprehensive estate plan, we recommend you consult with a lawyer. Here are some free resources that may be helpful too: Renown Health Foundation is proud to sponsor the Family Estate Planning Series put on by PBS Reno and the Community Foundation of Northern Nevada. The free, 8-week course of 90-minute, in-depth workshops is a great place to learn much more and to help you get started in the planning process. The next course begins on September 7, 2022. More information can be found here. Renown Health offers periodic advance health care directive workshops where attendees can learn about, complete, and sign their directive. The next workshop is scheduled for September 14th. More information can be found here. The American College of Trust and Estate Counsel provides information on a number of commonly asked estate planning questions here. If you are interested in including a charitable gift to Renown in your estate plan, we would be happy to talk to you about how your gift will make a difference for our mission. Please contact Abbey Stephenson at abbey.stephenson@renown.org or visit renown.org/LegacyGiving to learn about Renown Health Foundation’s Legacy Giving Society and ways to give.
-
Meet Gabby, Renown Regional ER Nurse and Miss Rodeo Nevada
Renown Health is proud to embrace the Reno-Sparks culture that makes our community stand out, which is why we sponsor the Reno Rodeo, an early summer staple with roots in the community as deep as our own. One of our many ties with the Reno Rodeo includes Renown Regional’s own emergency room nurse and Miss Rodeo Nevada 2022, Gabby Szachara. A Reno native, Gabby developed a love for the Reno Rodeo at a very young age. “I loved watching the girls on the Reno Rodeo Flag Team when I was little and knew I wanted to be part of the Reno Rodeo someday,” said Gabby. “As I got older, I started to make connections and build relationships with some people in the rodeo scene, and they generously lent me their horses so I could participate in the Reno Rodeo Flag Team.” Gabby was on the flag team for three years before being crowned Miss Rodeo Nevada 2022 last year. Before joining the Reno Rodeo Flag Team, Gabby was a student at the University of Nevada, Reno, and a member of the women’s volleyball team. In December 2017, she graduated with a bachelor’s degree in public health. At first, Gabby was interested in a career in sports medicine – it made sense with her background in athletics. But, after working in the medical field as a certified nurse assistant and an emergency medical technician, she grew passionate about patient care and decided she wanted to become a nurse. “I’ve always loved teamwork and helping others,” said Gabby. “It’s important to me to be there for others, especially when it might be their worst day.” In December 2021, Gabby graduated from Truckee Meadows Community College with a nursing degree and joined Renown Health this February. “I love Renown for various reasons. Everyone here is so nice and welcoming, and there is a great team dynamic,” said Gabby. “And I love that Renown’s main color is purple because that is my favorite!” When Gabby isn’t in her scrubs and caring for patients, she is in western wear and carrying out her duties as Miss Rodeo Nevada. “I do a lot of traveling across the country to attend other rodeos,” said Gabby. “I enjoy meeting so many wonderful people and experiencing the culture of different states.” Gabby’s main goals as Miss Rodeo Nevada are to promote the western way of life, agriculture, rodeo and community benefit. In addition, she visits local schools to talk with kids about how they can get involved in these areas and inspires them to turn their dreams into reality. Gabby has a special place in her heart for the Reno Rodeo. “Reno is my home, and the Reno Rodeo is the heart and soul of summer in northern Nevada. Everyone comes together and dusts off their boots to have fun and also contribute money to important causes in our community,” said Gabby. “I love the comradery, the friendly and healthy competition and the great people.” If you’re going to the Reno Rodeo this weekend, watch for Gabby and her horse, “Torque.” And if you see Gabby in the halls at Renown Regional, give her a high-five for all her hard work as a nurse and Miss Rodeo Nevada!
Read More About Meet Gabby, Renown Regional ER Nurse and Miss Rodeo Nevada
-
Paola’s Story: Bringing Hope and Determination to Patient Care
You may recognize her from billboards around town or the cover of Renown's latest annual report, but what you might not know is the story behind the now-familiar face. Paola Espinoza-Patino is the oncology unit's associate nurse manager at Renown Regional, and she grounds her work in hope and determination daily. Meet Paola:
Read More About Paola’s Story: Bringing Hope and Determination to Patient Care