Search
-
Department Spotlight: Wound Care
For the average person, wounds aren’t an everyday worry. However, for at least eight million Americans, chronic wounds can pose a serious threat to health and well-being. From a person with diabetes experiencing painful neuropathy to a patient healing from a significant burn, caring for advanced wounds is a major part of their healthcare journey. Who do they go to get the care and guidance they need? The answer: Renown Wound Care. Serving patients in both the inpatient and outpatient settings, this department provides comprehensive, best-in-class treatments for severe and chronic wound healing and ostomy care. Our Wound Care team members have mastered the art of harnessing cutting-edge technologies and a patient-centric approach to redefine the standards of healing. Advanced Care for the Best Repair At Renown Health, we are fortunate to have a team full of nurses, physicians and more caring for patients with wounds caused by a wide variety of conditions. Those include: Burns Trauma Vascular diseases Radiation therapy Pressure ulcers Diabetes and diabetic neuropathy Adding to the expert-level continuum of care, Renown is the only health system offering complete ostomy services in the entire region. The Wound Care team helps ostomy patients with the fitting of their medical bags, treatment of any skin conditions that may arise after ostomy bag placement, care coordination and much more. With a multidisciplinary network of experts tailoring personalized treatment plans, there is never a dull moment on the floor. On the outpatient side, the team expects 50-60 patients in one day alone. “As a clinician, wound care is a lot of ‘arts and crafts,’ so we get to use our creative and critical thinking skills to provide the best possible care,” said Samantha Moore, Advanced Wound Care Specialist RN for Outpatient Wound Care. “Each patient has an individualized plan of care – we greet them as they come into the clinic, escort them back to their treatment rooms and get their latest health updates and life situations before providing wound or ostomy care. We prepare each morning doing chart reviews to determine patient needs, wound progression and referral needs.” “We are a highly specialized, dedicated group of professionals with a passion to treat and heal our patients’ wounds,” added Lori Conner, Advanced Wound Care Specialist RN for Outpatient Wound Care. “When a patient comes to our clinic for evaluation, they are given a dedicated appointment to thoroughly go over their medical and surgical history, medications and nature of the wound.” Switching over to the inpatient care team, they operate like a well-oiled assembly line, navigating different daily assignments with precision and flexibility. “On the inpatient side, our day starts in our office with triaging our consult list; after the triage process is completed, we get our assignments, which can consist of wound vacuum-assisted closure (VAC) patients, follow-up patients, ostomy education patients and new wound consults,” said Megan Uy, Advanced Wound Care Specialist RN for Inpatient Wound Care. “In the case of patients requiring wound VAC changes, we consider what kind of pre-medication for pain that they need. Although some patients may be seen on a time schedule, the day ends up flexible as patients are being seen by other specialties. This flexibility also benefits the patients, making them feel more empowered with their care.” “Each day in the inpatient setting, we get to our office and sort through all the new consults that came in overnight, and the charge nurse makes the assignment for the day,” added Madison Arlin, Advanced Wound Care Specialist RN for Inpatient Wound Care. “After the assignment is completed, each nurse is responsible for researching their patients and organizing their day, typically by priority – wound VACs and ostomies usually take top priority.” Now, how do these treatments actually work? This specialized field handles advanced methods of treating each condition, including: Biological skin substitutes Surgical debridement Advanced wound dressings Negative pressure therapy Pre-ostomy markings and education Offloading techniques, such as padding or dressing “Before starting treatments, we communicate with our nurses and providers to make sure that the patient is comfortable prior to wound care,” said Dianna Seo, Advanced Wound Care Specialist RN for Inpatient Wound Care. “After we see the patient, if there is a need for escalated care, we contact the provider for additional testing or consults. We continue to follow-up on patients that have severe wounds, wound VACs and ostomies.” In the hands of the Wound Care team, patients exit our hospital walls not only restored but also empowered, set on a trajectory for long-term healing. Your Expert Care Guides No matter the case or the severity of the wound or condition, patient care, comfort and communication always come first – before, during and after treatment. “Many of our patients have chronic needs, so we end up seeing them for several months, if not years in some cases; we stay up to date with their specific psychosocial needs and help remove barriers that would prevent their wounds from healing,” said Samantha Moore. “I enjoy knowing that my positive attitude can improve our patients’ days,” added Maddie Pauley, Patient Access Representative for Outpatient Wound Care. “When they’re routinely coming to appointments they might not enjoy, hearing them praise our team and give their thanks is one of the most rewarding feelings.” As a wound care patient, there can be a lot of unknowns when beginning their care journey. However, these team members carefully walk each patient through every step from beginning to end. “When we go to see a wound care patient, our team is very consistent about explaining to the patients what our role is and what we plan to do with their wound, and then we continue to actively communicate throughout wound care each step that we are doing as we are doing it,” said Madison Arlin. “We also encourage some of our patients to listen to music that they enjoy during the wound care, or we will cover their eyes with a cloth if they request so that they don't have to see their wound. Sometimes, we will ask the family to stay at the bedside to hold their family member's hand.” Education is crucial to ensuring each patient knows what to expect in order to care for their wound and understanding the stages of healing. Fortunately, this team is well-versed in the world of wound wisdom. “A lot of education is provided on the type of dressing we are applying, and if the patient is going to be performing their own dressing changes, we will go over the entire change with them and provide supplies for discharge,” said Megan Uy. “Additionally, there will be written instructions in their discharge paperwork. In the cases of wound VAC dressing changes, each step is explained to the patient before doing it, and we also go over discharge options and expectations.” “As a clinician who sees a lot of patients prior to having their ostomy placed (pre-surgical marking), one of the most important things we do is first sit with the patient and/or caregivers and talk about their fears, concerns, questions and goals,” said Samantha Moore. “We provide a lot of emotional support and education, helping identify community resources. For our wound patients, we spend a lot of time educating our patients/caregivers about how and why their wounds occurred. We try to connect with them on a personal level and help them identify ways to help their wounds heal.” To see a patient’s care journey from the second they enter through our doors to the moment they return home is one of the most rewarding feelings for the Wound Care teams. In fact, they’ve had the pleasure of treating patients for years and seeing their wounds almost completely heal. The team collectively values the successful healing journeys of their patients as their proudest achievement. “One of our team's greatest accomplishments was being able to see one of our long-term patients discharged with nearly resolved wounds,” said Megan Uy. “This patient had been in our care on-and-off for the past year with many hospitalizations and had complicated high-output enterocutaneous fistulas within his wound bed. These were incredibly hard to keep a dressing on successfully, and he often had issues with the dressing leaking. Eventually, we got a dressing that could remain intact until his next scheduled dressing change, and he was able to get surgery that fixed his fistulas. Being able to see him recover and heal his wounds was a very large accomplishment for us.” The admiration and compassion this team has for their patients also extends to each other. The cohesive way they work together only further benefits their patients, offering the best-possible collaborative care. “We have extremely skilled clinicians in our group that are not only incredible in the work that they do and the patient care that they provide but are also enjoyable to work with as well,” said Geane Weaver, Advanced Wound Care Specialist RN for Inpatient Wound Care. “There is something to be admired in each and every one of my coworkers.” “Our team is very close and supportive of each other at all times,” added Madison Arlin. “I feel very lucky to work with such an amazing group of people. Our team is very proud of the work we do.” Fervently Fighting the Good Fight So, with the highly specialized nature of advanced wound care, how did these team members get inspired to join the Wound Care team in the first place? Well, for many of these devoted employees, their first exposure to caring for wounds took place on different units – sparking their interest in making wound care their full-time career. “Renown was the most welcoming towards me as a student nurse, and I liked that it was a teaching hospital,” said Madison Arlin. “I started in the General Surgical Unit (GSU) immediately after graduating nursing school and worked there for two years before transferring to wound care. I decided to apply to the wound team after watching the wound nurses do wound VACs and ostomy changes on the floor. I would ask them if I could watch, and I was always very fascinated by the wound healing process.” “Prior to joining the inpatient wound team, like Madison, I was also a bedside nurse in GSU,” added Geane Weaver. “Working on that floor, I was already exposed to a lot of patients that were requiring some kind of advanced wound care in one way or another. Working in the GSU, I also cared for a lot of patients that had wound VACs and ostomies. These patients make up a huge group of the individuals that our team sees on a regular basis, and they've always been intriguing for me, so naturally, wound care has always been on my radar.” For other team members, wound care has always been a point of curiosity throughout their education and career. From their very first exposure to this care area, they were hooked. “I was always curious about wound care even through my nursing school experience,” said Dianna Seo. “When I was working on the floor, I would trade to do wound care for patients. When I had time, I would follow wound care and help when I could. I joined the skin team which drove me to be increasingly involved with wound care. As soon as there was a job opening, I applied for the position. I worked in outpatient wound care for approximately four years and now inpatient for another four years. I have enjoyed all aspects of wound care and patient care.” “I had great clinical experience at Renown when I was in nursing school; I also was very interested in caring for trauma patients, and Renown being a Level II trauma center aligned with my interests,” added Megan Uy. “I began my nursing career in the GSU, but my dream job was always Wound Care. During my nursing school clinicals, I had the opportunity to watch some members of the wound team do wound VAC changes and thought it was incredibly intriguing and a great combination of utilizing the knowledge of anatomy and physiology while being creative with handicraft. A position opened on the team around the time I met the prerequisites to be eligible for the position, and luckily, I got it.” Our Wound Care team has achieved significant employee and departmental milestones over the past year, reflecting their dedication to enhancing patient care and overall process improvement. “We have had many accomplishments within the last year and are currently working on more to improve the hospital,” said Dianna Seo. “Madison Arlin won the DAISY Award for her great work with our patients. Megan Uy won Top Talent of the Quarter for helping a stranger. Ande Ferriera has worked tirelessly to improve our process improvement. Allie Saunders, as our leader, has worked to improve patient skin by getting new beds for Renown Regional. All our patients that have healed or are on their way to healing under our care is our greatest achievement that we as wound team is most proud of.” “We are constantly updating protocols, notes and orders for bedside nursing so that it is a more straightforward and seamless charting process,” added Madison Arlin. “We have representatives of different supply companies come and present new products that we think may benefit our patients better. Our wonderful tech has even updated our department site on Inside Renown so that the nurses always have references available.” Renown’s strong influence in the region – and the opportunity to give back to their community – was, and continues to be, a major draw for this team. “Since I can remember, Renown has always been the most prevalent healthcare name for my family and has always taken the most amazing, thorough care of my loved ones,” said Maddie Pauley. “I have always wanted to work somewhere I could help people, and starting at Renown has really opened my eyes into how much of a difference each one of us can make.” Our Wound Care department’s success stories and proactive approach not only reflect their passion for healing but also inspire a ripple effect of positive change throughout our health system. They proudly exemplify a shared commitment to enhancing the well-being of all patients under their care. “Being part of Renown and part of this team has been my blessing; I get to do a job I love with people that love it too,” closed Dianna Seo.
-
Sterling Silver Club Shining Stars: Mark & Dana Combs
Dana and Mark Combs met through mutual friends and had a long friendship before they became a couple in 2009. They were married in 2011 in a private ceremony at a small Reno chapel, and a few months later had a big celebration with their family and friends. Encouraging Others to Succeed Over the years, the happy couple has spent much of their time volunteering and giving back to others in their community. Twenty-six years ago, Mark became a bilateral lower limb amputee. For the past 10 years, he has been a prosthetic consultant, helping other amputees learn how to cope with various challenges and encouraging them to keep living life to the fullest. “Mark is great with helping people,” said Dana. Dana also does a lot of rewarding work through a Philanthropic Educational Organization (P.E.O). She is an advocate for raising money to help women ages 18 and up gain an education. Dana also enjoys tutoring English as a second language. Enjoying Quality Time, Hobbies & Travel When Dana and Mark aren’t helping others, they are spending time with their family and friends, their dog Mia (a 3-year-old Maltipoo) or enjoying one of their many hobbies. Some of Mark’s favorite things to do include playing Solitaire and strumming on his guitar. “I love to garden and play crossword puzzles and word games,” said Dana. “I’m really looking forward to the springtime to spend more time in the garden.” She loves to work out and has a membership at the UFC gym in Reno through her Senior Care Plus gym benefit. Dana also has her own online Etsy store, where she sells homemade jam jars, candle holders and vintage dolls. “Last summer I sold my first edition Barbie that I got when I was 9 years old,” said Dana. “I made quite a profit on it.”
Read More About Sterling Silver Club Shining Stars: Mark & Dana Combs
-
Celebrating Blood Sugar Balance This Holiday Season
As the holiday season draws near, we find more reasons to celebrate with loved ones. At Renown Health, we are kicking off the celebrations early this November with American Diabetes Month. Approximately 37 million Americans, including 270,000 Nevadans, have been diagnosed with diabetes with as many as 95% of those diagnosed living with type 2 diabetes mellitus (T2DM). What is Type 2 Diabetes? Type 2 diabetes is a chronic health condition that occurs because your body is not using insulin (a hormone made by the pancreas to help cells use the food we eat for energy) as well as it should, resulting in high blood sugar levels. It is important to obtain a diagnosis for T2DM and ensure it is well-controlled to prevent serious health complications. Those with diabetes are at higher risk for blindness, kidney failure, heart disease, stroke and amputation. Tips for Supporting Your Health with Type 2 Diabetes Know Your Blood Sugar Levels: Work with your healthcare provider to establish target blood sugar levels, and make sure to monitor your levels regularly as advised by your healthcare provider to prevent or delay health complications associated with T2DM. Focus on Your Plate: Eating foods such as fruits and vegetables, lean meats or plant-based proteins, healthy fats and whole grains supports diabetes management. If choosing healthy foods is difficult due to your busy schedule, cost or simply because you aren’t sure where to start, talk with your healthcare provider who may refer you to a registered dietitian. Registered dietitian nutritionists are certified nutrition specialists who can provide education and practical tips for eating to support your T2DM diagnosis with visits covered by many insurance plans. Prioritize Staying Active: Engaging in regular exercise is good for everyone, especially those living with T2DM. Exercise helps your cells become more sensitive to insulin and therefore supports healthy blood sugar levels. Always check with your healthcare provider prior to beginning a new exercise plan. Support Stress Reduction: Stress is unavoidable but can be managed through regular exercise, getting enough quality sleep (7-8 uninterrupted hours per night) and practicing meditation and other mindfulness techniques. Plan Ahead for Holiday Gatherings: There’s still room for celebration while focusing on blood sugar management. Consider bringing a healthy dish to your gathering, focus on filling your plate with vegetable sides and eating those first and incorporate a family walk after dinner. If traveling, pack nutritious snacks that support your health and keep you full. Lastly, enjoy the special dishes and desserts this season has to offer in single-serving portions.
Read More About Celebrating Blood Sugar Balance This Holiday Season
-
Importance of Safe Sleep
In today's fast-paced society, it is understandable for parents to want to take shortcuts in caring for their little ones. A s a result, It is tempting to leave a sleeping infant in a car seat or swing after a long day of errands or when you need a moment to catch your breath. But, as convenient as these devices may be, they pose a serious risk to your child's safety. Why Car Seats and Swings Pose Risks for Infant Sleep Car seats, swings, and bouncers are quick and convenient ways to feed, hold, and sleep an infant. Not out of malice or discontent, but again from the need for quick and easy access to baby care in an already busy lifestyle. However, the risks outweigh the benefits. The American Academy of Pediatrics (AAP) states that “infants should be moved to a crib, bassinet, or play yard for sleeping as soon as is practical.” If a parent must use a car seat or other sitting device, they should only do so for a short period of time and never as a substitute for a proper sleeping environment. Leaving a sleeping infant in a sitting device, such as a car seat or swing, can create unsafe sleeping conditions. The American Academy of Pediatrics (AAP) warns that doing so increases the risk of sudden infant death syndrome (SIDS) and positional asphyxia. This is because infants can easily slump over or become entangled in the straps, blocking their airway, and causing suffocation. Car seats, swings, and bouncers are quick and convenient ways to feed, hold, and sleep an infant. Not out of malice or discontent, but again from the need for quick and easy access to baby care in an already busy lifestyle. However, the risks outweigh the benefits. The AAP states: Infants should be moved to a crib, bassinet, or play yard for sleeping as soon as is practical. If a parent must use a car seat or other sitting device, they should only do so for a short period and never as a substitute for a proper sleeping environment. Leaving a sleeping infant in a sitting device, such as a car seat or swing, can create unsafe sleeping conditions. The AAP warns that doing so increases the risk of sudden infant death syndrome (SIDS) and positional asphyxia. In addition, infants can easily slump over or become entangled in the straps, blocking their airways and causing suffocation.
-
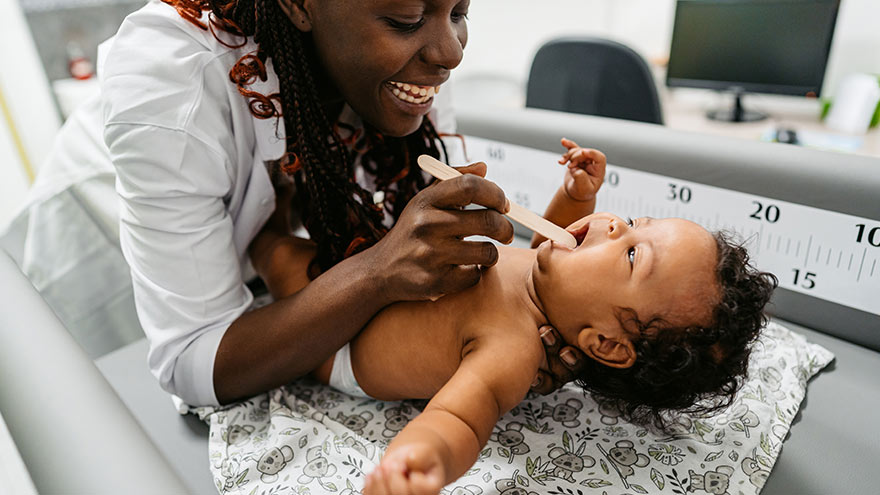
What to Expect at a Well Child Checkup
A well-child checkup is a great opportunity to monitor your child’s growth and development, and it's also a chance to establish a trusting relationship with your child’s pediatrician and have your questions answered. What to Expect at Each Checkup At every checkup, a comprehensive physical examination will be conducted to assess your child's growth parameters, including height, weight and head circumference. A developmental assessment will evaluate the progress of your infant or young child in achieving age-appropriate milestones, encompassing language skills, motor development, problem-solving abilities and psycho-social skills. In addition, your pediatrician will address common concerns such as feeding, sleep patterns, oral health and general infant care. Unless there are specific needs or concerns for your baby, routine laboratory tests are typically unnecessary. Your pediatrician will provide guidance on immunization schedules, post-vaccination expectations and when to seek medical attention. Furthermore, during each visit, you will receive age-specific guidance to help you anticipate your child's expected growth and development, along with essential safety precautions and illness prevention measures. Your pediatrician will discuss various topics, such as placing your baby to sleep on their back, utilizing rear-facing infant car seats until around age two, maintaining home water thermostats below 120 degrees Fahrenheit, ensuring dangerous objects and poisonous substances are out of sight and reach, emphasizing dental health and promoting the use of bike helmets, among other things. Preparing for Your Visit It is recommended that, as a parent, you write down any questions beforehand, so you don’t forget them in the moment. Most importantly, feel comfortable asking your pediatrician about anything that might seem unusual, as you are the parent, and you know best! Before leaving the pediatrician’s office, be sure that you fully understand any instructions given to you and ask for clarification if needed. From your child’s birth through young adulthood, you will be visiting your pediatrician regularly. The American Academy of Pediatrics provides what a regular schedule might look like. Well-Child Checkup Schedule Two to three days after birth and at one month Two months Four months Six months Nine months One year 15 months 18 months 24 months 30 months Three years, and yearly after
-
10 Essential Questions to Ask at Your Child's Pediatrician Visit
Taking a few minutes to prepare for your child's pediatrician visit helps ensure that all your child's medical needs are met. Knowing the right questions to ask your provider can help you get the most out of your visit and ensure you and your child feel comfortable and informed. It is essential to base your questions on your child's specific health needs, but the ten options below are a great place to start. How is my child's overall health and development progressing? Is my child meeting their developmental milestones, and are there any areas where they may need extra support? What vaccinations does my child need, and are they up to date on all required immunizations? Are there any nutritional recommendations or concerns for my child's age and stage of development? What are some strategies for promoting healthy habits and physical activity for my child? Are there any warning signs I should look out for regarding my child's health or behavior? What can I do to help prevent common childhood illnesses like colds, flu strains or ear infections? What should I do if my child gets sick, and when should I seek medical attention? Are there any changes to my child's medication or dosage that I should be aware of? Is there anything else I should know or be aware of regarding my child's health or development?
Read More About 10 Essential Questions to Ask at Your Child's Pediatrician Visit
-
11 Tips Caregivers Need to Know
Becoming a caregiver or playing a more active role in another’s healthcare is a big responsibility. At some point, almost all adults will support an aging parent or a loved one in need. Keeping track of their needs and wellbeing, while also prioritizing your own can become overwhelming. It’s important to know: you are not alone, and help is available. Read on for 11 tips to help you manage your time, your own wellbeing and your loved one’s care. Self-care comes first. When your main priority is the person in your life who needs care, it’s easy for your own needs to take the backseat. Give yourself time each day to focus on your personal wellbeing. It’s hard to give a loved one the care they need if your own needs are not met. Prioritize the Activities of Daily Living (ADL). Make a note of what ADLs your loved one can do alone, what they need help with and what activities require the most help. This will help you work through the day with them, as well as plan out how the day’s activities will go. Do a home safety audit. Do showers, bathtubs and steps have safety grab bars? Look around the house for additional tripping hazards, like rugs or electrical cords. If your loved one struggles with day-to-day navigation of the home, consider scheduling an occupational therapy appointment. This type of therapy helps a person develop or maintain the motions required to accomplish daily tasks. You might also qualify for a referral to in-home healthcare, such as Home Care. Have the hard conversation. The best time to discuss views about end of life care and to learn what choices are available is before a life-limiting illness or crisis occurs. With advance care planning, you can help reduce the doubt and anxiety related to decision making at the end of life. Completing an Advance Directive is a great tool to sort out all these decisions before they’re needed. Attend a free workshop to learn more and complete this important document. Identify when you need respite. Respite care involves receiving a short-term break from caregiving. Organizing in-home care for your loved one will allow you to step away and tend to your needs. By identifying what kind of respite care you are seeking, you can find the right person to provide you with that much-needed break. Don’t wait until you feel overwhelmed, plan ahead. Write down insurance contact information. Have a direct connection to the right insurance professional for support and advice. If your loved one is eligible Medicare, this is a good opportunity to review their current selections and if they would benefit from a Medicare Advantage Plan or Medicare Supplement Insurance. Seeking out expert advice or information on Medicare options is a great way to navigate this. Consider calling a broker, or attend a free educational seminar with Senior Care Plus. Gather legal and financial information. Make a list of all existing legal documents and financial accounts that your loved one has. These might include a will, advance directive, power of attorney, bank accounts or investment accounts. If you have questions about how to manage them, or need assistance in setting up additional framework, reach out to a lawyer, legal service, financial adviser or bank representative. Create an inventory of medical information. Identify where all of your loved one’s medical records are, as well as a list of providers or healthcare practices where they have received care. Consider if you should have your loved one give you Proxy Access in MyChart, which allows you to access all the features in MyChart on their behalf, including viewing upcoming appointments, viewing test results and emailing a doctor on their behalf. Make a list of what others can do. Think about all the little (and big) things that need to happen, and write down tasks that others could take care of you. When someone says “let me know what I can do” you’ll be ready with a pre-written list of items they may be able to assist with. Tasks could include tackling around-the-house repairs, scheduling lawn work, helping to walk the dog, taking a car for an oil change and cleaning. Find programs and events for social enjoyment. If and when possible, seek an activity outside of the home. Look for community centers that have programs for seniors, recreational activities or meals that you can patriciate in together. If leaving the home is not an option, arrange for visits or in-home activities, such as movie nights, card games or time to visit with family. Research long-term options. If you will be considering a nursing home or assisted living, make a list of amenities that you and the person you are caring for would like. Take this list with you when visiting potential locations to make sure you don’t forget to ask about each item.
-
Department Spotlight: NICU Transport
Bringing in new life is an exciting and beautiful occasion. The possibilities for the newest members of our world are endless – what will the child grow up to become? What will they achieve in their lifetime? Anyone will agree that a new life is precious and protecting that life by any means possible is a necessity. Sometimes, however, a baby’s journey into our world brings along obstacles. Prematurity, congenital defects and other complications can accompany a birth and the baby’s first few moments of life. But what happens when these complications happen outside of a fully-functioning Labor & Delivery unit, or if the complications need a special level of intervention with a health system capable of caring for their unique needs? Enter the NICU Transport team at Renown Health. As the only Neonatal Intensive Care Unit (NICU) Transport team in northern Nevada, these dedicated nurses, respiratory therapists and neonatal nurse practitioners – who have normal unit duties of their own at Renown Regional Medical Center – step up to the plate to take on this extra duty to support members of their community facing some of the scariest moments of their lives. To them, transporting babies in critical condition and giving them the best chance of life isn’t just a responsibility; it’s a calling. The NICU on Wheels When the Saint Mary’s maternity unit, which was Renown’s partner in NICU transport duties, made the decision to close, our dedicated NICU nurses and respiratory therapists diligently rose to the occasion to fill the demand. Dubbed the “NICU on Wheels,” Renown’s team went from taking on transport duties every other day to 365 days a year – and they are always ready to go at a moment’s notice, whether it’s by ambulance or by fixed-wing aircraft. “When we learned about the closure we knew it was our calling and knew we had to step up,” said Rachel D., Neonatal Transport RN at Renown. “We still have regular days on the floor, and we each switch off being on-call for transport. Once we get a distress call, we have 30 minutes to get to the hospital, grab our gear and go. We have to essentially put a whole room’s worth of portable equipment in one bag.” “I really enjoy being a part of the transport team and making a difference from northern Nevada to northern California,” added Sam V., Supervisor of Respiratory Care at Renown. “We are able to practice at the top of our skill level and use autonomy that not every practitioner gets to use.” Each NICU Transport unit works in teams of three when heading out into the field: one nurse (our bedside experts), one nurse practitioner (our education experts) and one respiratory therapist (our lung and breathing experts). With several years – and in many cases, decades – of experience in NICU nursing, NICU transport duties and respiratory therapy, this team is poised to provide state-of-the-art lifesaving care en route to the hospital. This diverse array of experiences among the team especially comes in handy as they continue to face the increased transport workload. “We are so thankful to have Saint Mary’s employees come over and work on our team after their maternity ward closed,” said Melyssa H., RN, NICU Transport Coordinator at Renown. “Helping the babies, as well as helping the scared families, will always be our top priority.” “I love the complexity that babies provide in the NICU,” added Jennifer J., Neonatal Transport RN at Renown. “Providing hands-on care right at the bedside along other members of the team is such a rewarding experience.” Education is also a crucial tool in NICU care, especially in the field. The nurse practitioners on this team make it their mission to outreach to the community, including our rural health partners, and help them build the tools and skills they need to care for our smallest and most critical patients. “I have been on a few transports where we went out and did not have to bring the baby over to the hospital, and we were able to provide lots of education instead,” said Shiela A., Respiratory Specialist at Renown. “For instance, I was called out to Fallon for a baby that was in respiratory distress. When we arrived, we saw the baby was awake and active although intubated. The tube came out, and we retaped it. While we stayed to observe the baby to make sure everything was okay, the nurse practitioner on the team provided educational tools to the family on what they can improve on regarding their baby’s tubing. Our nurses do such a great job with these teachings.” “When I started, I quickly noticed that more education was needed in the field,” added Jennifer J., RN. “Now I see the momentum we’ve had in these communities really take full force. Because of this education, and the confidence we instill in our patients’ families, each baby’s transition to our team has become so much easier. It has been awesome to watch this progress over the years.” With immense experience, education and a strong commitment to their community under their wing, the NICU on Wheels is only just getting started. Teamwork Makes the Dream Work Running a successful NICU Transport operation, especially as the sole health system participating, takes a village. With only three professionals out in the field, the team leans on their fellow nurses, physicians, surgeons and specialists to make the operation run as smoothly as possible. From REMSA and Care Flight helping load patients in and get them to the hospital safely, to Renown’s Clinical Engineering team who are first on the scene when machines need repairs and troubleshooting, everyone rises to the occasion to achieve the best-possible outcome for our youngest patients at some of the most challenging moments of the beginning of their lives – and they are fully trusted to move those mountains. “Being a part of the NICU Transport team has given us the opportunity to facilitate a deeper, meaningful relationship with providers and a patient’s entire care team,” said Rachel D., RN. “They entrust us with our assessment skills, opinions and skill levels. There is an equal layer of trust between us and them.” Despite the pressure they feel every day, the NICU Transport team never let it overtake them and instead let it empower them. “We are under a lot of pressure and stress regardless of the case, and yet, we all work so well together; the teamwork really is incredible,” said Lisa A., Respiratory Specialist at Renown. “I am very proud of how our team steps up and is very intricate, even down to organization. For example, team members like Shiela arrange all the respiratory bags and make sure they are laid out in a way that makes the procedure as simple as possible to ensure there are no complications.” The nurses and respiratory therapists also partner together on the NICU floor and are always ready to provide coverage when their transport colleagues get a call. Committed to collaboration and ready to jump into action, the NICU Transport team works together to elevate each other and the bottom line for each patient. “This is a full-time gig, and the group works together to make sure everyone is covered; we are all very collaborative,” said Sarah K., Respiratory Specialist at Renown. “We all think of our patients as extra special, and it’s nice to know that you can make a difference in the baby’s life and the lives of the family. We all have a sense of purpose in giving back to the community.” “I am just so thankful to be a part of this team,” added Marcia A., Neonatal Transport RN at Renown. “We really have developed a strong bond.” A Track Record of Success The life-saving measures that each member of the NICU Transport team take surpass hospital walls. The impact they have on each baby are remembered and celebrated for years, and they often develop lifelong relationships with patients and their families after their stay in the NICU. One prime example of this can be found in an impassioned letter from Tess, the mother of a young boy who was in the midst of respiratory distress and needed immediate intervention. Because of the valiant efforts of Renown’s NICU Transport team, her child, Warren, is a healthy and happy baby to this day. She recalls the experience: Warren had stopped breathing while getting routine blood work. He was resuscitated twice while at an area hospital. We made the decision to transfer him to Renown for him to be admitted into the NICU. Within an hour and a half of this decision, Renown had sent a team consisting of a respiratory therapist, nurse and nurse practitioner to come and get him. As soon as the team entered the room, we immediately felt safe and comforted. The team made sure we knew exactly what was going on and what was going to happen in the following hours, and they let us know they would do everything for Warren. He was resuscitated two more times by the respiratory therapist while getting ready for transport. At that time, the decision was made to intubate for a smoother ride to Renown. We knew you all had his best interest in mind, and of course, we trusted you with everything. The intubation went well, and he was packed up and ready to drive. Today, Warren is hitting all of his developmental milestones and is a normal, happy baby in everyone’s eyes. We can’t thank the NICU Transport team enough for taking such good care of Warren and helping him Fight the Good Fight. “This success wasn’t just due to our three-person unit – our manager, Jason, also jumped in and drove all the way to Carson City to stabilize the child,” said Shiela A. “This just goes to show that no matter our title, we are always here to help and make a huge difference in the lives of our patients.” Success stories of children like Warren describe the common mission of the NICU Transport team in detail, and while there are more of these stories to come, the team is always ready to make the necessary sacrifices for the greater good of their patients. “Sarah K. is like Warren’s guardian angel,” said Tess. “We call her ‘Auntie Sarah’ now. He wouldn’t be here if it weren’t for her and the entire NICU Transport team. It takes a special kind of person to work in the NICU. I can never repay this team for what they’ve done for Warren and our family.” “I am proud of this team, their flexibility and the sacrifices they have made to do transport 365 days a year,” added Melyssa H., RN.” The remarkable success of the NICU Transport team serves as proof of the unwavering and tireless commitment of each and every team member, bringing hope to families during their most difficult moments. “NICU Transport forces you to be confident in yourself and your abilities and to push yourself a step further,” said Rachel D., RN. “I am a better nurse because I joined the transport team.”
-
Building a Better Birth Team
Giving birth expends as much energy as running a marathon. And just like you would only run a marathon with training beforehand, there are exercises you can do to prepare for birth. But instead of a coach, you'll have your birth team. Your birth team exists to help you navigate pregnancy and labor and support your choices. Let's say you've never put together a birth team before and are wondering where to start. Today we'll go over the three main positions to fill for your birth team's starting lineup. Birthing Person The birthing person is the leader of the team. After all, you can't have a birth team without someone giving birth. This person could be the baby's mother, gestational surrogate, birth parent before adoption, a transgender father or a non-binary parent. If you are not the birthing person, don't presume to know what the ideal labor and birth circumstances should be. And if you are the birthing person, don't allow anyone else to tell you what you want. This is your body and your birth; you are the boss in the birth room. Doula No birth team is complete without a doula, and although doulas have increased in popularity lately, many people still don't know what a doula is. Simply put, a doula is a birth professional – not a medical provider – who offers emotional, physical and informational support during pregnancy, labor and beyond. Most doulas' services include at least one prenatal visit and one postpartum visit, as well as continuous care throughout active labor. Some doulas provide more than one prenatal/postpartum visit, so be sure to ask what is included in their fee. Even if you have a partner who will support you during labor, studies have shown that a doula can significantly increase your likelihood of a positive birth outcome. Even the most supportive partner needs to rest, and a doula can ensure that you still get the care you need while your partner gets a break. Midwife or Obstetrician Finally, you'll want to choose the medical professional who will attend your birth. Many folks choose to give birth with the OB/GYN who does their annual check-ups, but there are many reasons someone might choose a different provider for their birth. The first step to finding the best attending provider for your birth is to decide which model of care aligns closest to your values and goals: the Midwifery Model of Care or the Medical Model of Care. .tg {border-collapse:collapse;border-spacing:0;} .tg td{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; overflow:hidden;padding:10px 5px;word-break:normal;} .tg th{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; font-weight:normal;overflow:hidden;padding:10px 5px;word-break:normal;} .tg .tg-gqvw{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-weight:bold; text-align:left;vertical-align:top} .tg .tg-8vim{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-size:18px; font-weight:bold;text-align:left;vertical-align:top} .tg .tg-qm8j{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;text-align:left; vertical-align:top} .tg {border-collapse:collapse;border-spacing:0;} .tg td{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; overflow:hidden;padding:10px 5px;word-break:normal;} .tg th{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; font-weight:normal;overflow:hidden;padding:10px 5px;word-break:normal;} .tg .tg-gqvw{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-weight:bold; text-align:left;vertical-align:top} .tg .tg-8vim{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-size:18px; font-weight:bold;text-align:left;vertical-align:top} .tg .tg-2rvk{background-color:#ffffff;color:#000000;font-family:Arial, Helvetica, sans-serif !important;text-align:left; vertical-align:top} Midwifery Model of Care Medical Model of Care Philosophy Birth is physiological. Birth is potentially pathological. Interventions Medical interventions can cause more complications, and therefore are only used as needed. Medical interventions should be used, even in non-emergency situations and sometimes as preventative measures. Decisions Birthing person is the key decision maker. Medical professional is the key decision maker. Provider’s Role Providers monitor labor and will intervene or transfer to hospital if needed. Providers assess and control the birthing process.
-
Get Ready for Baby with Childbirth Classes
By taking our pregnancy and birth class, you will gain the tools necessary to have a safe and empowering birth experience for both you and your baby. Chris Marlo, Childbirth Educator at Renown Health explains why birth classes are important. For questions regarding classes or tours, contact Chris Marlo: chris.marlo@renown.org 775-982-4352 What is a Certified Childbirth Educator/Doula? If you are expecting a baby, Renown has a wide variety of classes to help prepare you for birth. Classes are taught by certified childbirth educators and doulas. A certified childbirth educator is a trusted resource who has a passion for educating expecting parents about childbirth, and will provide you with non-biased, evidence-based information. A doula is a professional labor assistant who provides physical and emotional support during pregnancy, childbirth and postpartum. As you prepare for birth, our certified educators will guide you each step of the way and ensure you receive the quality care you deserve.
-
Top Safe Sleep Tips for Your Baby
Becoming a parent for the first time means lots of new unknowns – from learning to breastfeed and swaddle to buckling your newborn into the car seat for the first time. But when it comes to putting them to bed safely, it’s important to remember it really can mean life or death. It’s something we’re taught before our little one is even here: the correct way to put your baby to bed safely. Sadly though, the number of infant deaths continues to climb. The main culprit of sleep-related infant death continues to be all the items parents leave in the crib with their babies. According to the Center for Disease Control and Prevention, there are about 3,500 sleep-related deaths among babies each year. “The best advice is ‘bare is best.’ Keep your infant’s sleep space clutter free – no blankets, bumpers, toys or pillows,” said Karen Wagner, Pediatric Nurse Practitioner. Follow the ABCs for Safe Sleep Remembering the ABCs is an easy way to remember how to put your little one to bed safely. A: Alone No blankets, toys or pillows. “We do recommend using a sleep sack as a blanket alternative,” said Karen. “It prevents the risk of suffocation and keeps your baby warm.” Keep in mind, the greatest risk for suffocation happens when babies are under 1 year of age, so it’s best to save the toys, blankets and pillows for their “big kid bed,” or around 18 months old. B: Back The slogan “back is best” is another good reminder. Keeping your baby on their back until they’re old enough to rollover helps reduce the risk of Sudden Infant Death Syndrome (SIDS). C: Crib It is best to have your baby sleep alone in their crib. While co-sleeping may be enticing, especially after a late-night feed, it increases the risks of possible suffocation. However, “having your child in your room, in their own crib or bassinet, is protective for SIDS,” Karen said. “In fact, we think co-rooming reduces SIDS risk by almost 50 percent.” Co-rooming allows parents to keep new babies in close reach and helps parents oversee their baby’s sleep, just in case something happens.
-
Remove the Guesswork with Renown’s Labor Assessment Area
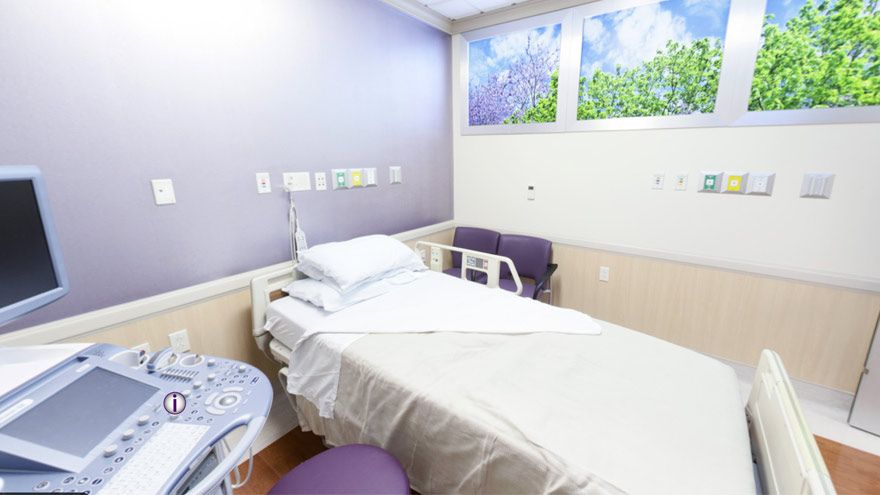
Pictured above: A section of Renown’s Labor Assessment Area. When patients expecting a new child are about to give birth, nerves can be especially heightened. Questions flood their minds: Is the baby actually on the way? What’s going to happen next? Are we ready to push? Lucky for them, at Renown Health, the guesswork can finally end with Renown’s Labor & Delivery unit Labor Assessment Area. This unique space is a triage area that helps make more precise labor diagnoses by determining exactly what stage expectant parents are at in the labor process. Funded by a state grant more than a decade ago, the six-bed Labor Assessment Area sees 500-600 patients per month – from patients entering the unit directly, unsure if they are in active labor, to patients who are sent over from elsewhere experiencing labor symptoms, such as high blood pressure and water breaking. The area also serves as a pre-operation space for patients getting ready for procedures such as C-sections. The six cubicles that are enclosed with doors and curtains ensure each patient gets the private, one-on-one care they need. Furthermore, rather than sitting in a waiting room, this area allows expectant parents a comfortable place to prepare for labor. “We are a unit that prides ourselves on getting patients into beds very quickly,” said Debbie Hawley, Associate Nurse Manager in Renown’s Labor & Delivery unit. “This area has allowed us to triage more effectively and allow more patients to collaborate with their provider in a quick manner.”
Read More About Remove the Guesswork with Renown’s Labor Assessment Area
.png?rev=5ac90884d83d45468d7e3a5389920ff1)