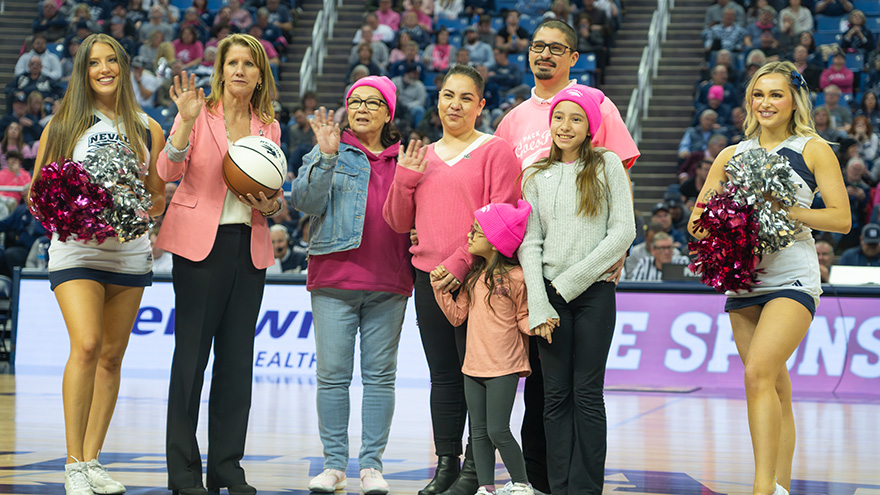Search
-
Why Childhood Immunizations Are So Important
Immunizations save thousands of lives each year by preventing serious illnesses, hospitalizations, and deaths. They also protect those who can't be vaccinated, like young children and the elderly, through herd immunity. Dr. Vanessa Slots highlights the crucial role of vaccines. Immunizations Your Child Needs (and when) Birth to 6 Months Hepatitis B: Shortly after birth, first vaccine dose Diphtheria, Tetanus, and Pertussis (DTaP), Polio, Haemophilus Influenza (HiB), Pneumonia, Hepatitis B and Rotavirus: Ages 2, 4 and 6 months, boosters and vaccines One Year to 18 Months MMR and Varicella (chickenpox) vaccine: Age 1, first vaccine dose Hepatitis A, HiB and Pneumonia: Age 1, booster DTaP: 15 months, fourth vaccine dose Hepatitis, second dose: 18 months Flu Vaccine: 6 months and older, annually* *In the year after receiving their first dose, an infant will need a booster one month later. Four Years Old MMRV, DTaP and Polio, final dose: Four years of age Pre-Teen and Beyond Tdap and Meningitis: Before starting middle school, children receive these vaccines. They are also old enough to start the HPV vaccine, an essential vaccine for all young adults to protect against cancer, genital warts and cervical dysplasia.
Read More About Why Childhood Immunizations Are So Important
-
When Care Can’t Wait: True Stories of Renown ER
Renown Health is home to three 24/7 Emergency Rooms (ERs) providing comprehensive emergency and trauma care, access to specialists and inpatient services backed by the area's most extensive health system. In 2023, Renown Health cared for 132,340 patients across three ER locations. Renown is also home to the region’s only level II trauma centers for both adult and pediatric patients. We spoke to three patients who sought immediate medical attention for various ailments and conditions to learn more about their emergency care experience and why they chose Renown ERs. Kamrin’s Story: From Worrisome to Critical In the spring of 2021, Danielle and her 13-year-old son Kamrin visited his primary care doctor for unexplained vomiting and were promptly referred to Renown Children's ER via ambulance for further evaluation and seen by board-certified emergency physician, Dr. Lisa Nelson. What initially began as an unassuming doctor's visit quickly turned into something much more severe after several tests confirmed a devastating abdominal tumor and a stage-four cancer diagnosis, unbeknownst to the family. Kamrin was immediately admitted to the Pediatric Intensive Care Unit (PICU) and referred to a Pediatric Oncologist at Renown Children’s Hospital to begin his plan of care with expert pediatric hematology and oncology specialists. Regarding the board-certified physician, who delivered the results to the family, Danielle said, “She was so calming to us, even as the diagnosis haunted us. She led us by guiding our family through the unknowns. She felt like a family member to us in that moment, letting all the unknowns be well known.” “The love, empathy, support and guidance these employees gave us carried us. The care team quickly and easily became a source of relief, knowing we were their priority and in the best hands. We are forever grateful for the team at Renown Children's Hospital and Renown Children’s ER; they truly saved our son's life and continue to be our guiding light whenever it's needed in our son’s health journey,” Danielle said. Today, Kamrin is in remission and navigating the aftereffects of chemotherapy, including an immune system deficiency. However, his family chooses to navigate each day by embracing the positive side of things, such as the life-saving impact of his treatment. Did you know? Renown Children's Pediatric Hematology and Oncology is located within Renown Regional Medical Center and offers expert pediatric specialists dedicated to providing comprehensive treatment for pediatric hematology and oncology, including chemotherapy, radiation therapy and infusion services. Taylor’s Story: From Crisis to Recovery Promptly after cosmetic surgery performed by a medical professional not associated with Renown, Taylor Salas (Chacon) began to lose consciousness and notice her post-surgery drainage systems, also known as Jackson-Pratt drains, fill with blood. She was transported to Renown Regional ER via ambulance and immediately seen by ER staff and board-certified emergency physician Thea Berning, MD, for medical assessment. Taylor drifted in and out of consciousness as the ER team began blood transfusions and a CT scan to determine her plan of care. Dr. Berning began facilitating communication with a community plastic surgeon with privileges at Renown Health and emergency surgery was performed to stop Taylor’s internal bleeding. Taylor was placed on a ventilator due to respiratory distress and trauma from the event, then transferred to Renown’s Intensive Care Unit (ICU) to continue her care. Thankfully, Taylor listened to her gut when something didn’t feel right after her surgery and sought immediate medical attention. The ER team's quick response, communication and collaboration with a plastic surgeon saved Taylor from severe internal bleeding. “I was informed every step of the way about what was happening and why. I felt comfort in this,” she said. Did you know? Because of Renown Regional Medical Center’s Level II Trauma Center distinction, you have immediate access to an extensive list of specialists and physicians trained in a wide array of specialties, in the event of a traumatic injury or accident. This is one of the many benefits of Renown Regional’s Level II Trauma status. Ted’s Story: The Unsuspected Threat Bothered by symptoms of heartburn, fatigue, neck pressure and arm discomfort, Ted was in the middle of a busy workweek in June 2023 when he began to suspect something was wrong. Knowing the importance of addressing early heart attack symptoms immediately, Ted and his wife headed to Renown Regional ER because of proximity and some familiarity with Renown’s leading cardiology care and technological expertise. After prompt assessment by the Renown ER team, including blood work, imaging tests and the administration of medication, Ted was admitted to the hospital to treat the blockage and narrowing of his coronary artery. On June 8, Ted was admitted for treatment, where he successfully underwent a single bypass surgery and recovered in the Cardiac Intensive Care Unit (CICU), before being discharged and following up with the Intensive Cardiac Rehab (ICR) program at Renown. The ICR program at Renown played a pivotal role in Ted's 55-pound weight loss and overall health improvement, empowering him to embrace a healthier lifestyle and find ways to use his newfound energy and strength today. “Overall, I believe I had the best care possible because of the collective group of people at Renown caring for this community, who we could see in the grocery store, at the ball game and in the shopping malls. This community feeling is something you might not get in a big city hospital,” Ted said. Did you know? Intensive Cardiac Rehab at Renown Health is a medically supervised program designed to improve cardiovascular health after a significant heart condition or procedure. Since its inception in 2016, this program has been a pioneer in the region for cardiac rehabilitation focusing on three key pillars including exercise, nutrition and stress management.
Read More About When Care Can’t Wait: True Stories of Renown ER
-
Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
Raquel was 33 when she was diagnosed with breast cancer. It was April 2023, when she found a lump in her breast and was referred to the William N. Pennington Cancer Institute. After comprehensive imaging, she was diagnosed with invasive lobular carcinoma, which is a type of breast cancer that begins in the milk-producing glands of the breast. Between June 2023 and January 2024, she received a total mastectomy, chemotherapy and radiation at Renown Health. “Breast cancer is uncommon in women under 40, but any woman with a mass or lump in her breast should have an exam by a physician and imaging at any age,” said Dr. Lee Schwartzberg. In fact, according to the Centers for Disease Control and Prevention (CDC), only 9% of all new cases of breast cancer in the U.S. are found in women younger than 45. “It was a pretty scary diagnosis, but I’ve been led by great people through the process,” she said. “They were so helpful and there for me throughout the chemo and radiation.” Raquel's journey through breast cancer treatment at the William N. Pennington Cancer Institute was marked by the exceptional care provided by the Renown Health team, including nurses, nurse navigators, therapists, support teams and providers. Among the dedicated professionals, Dr. Michelle Chu and Dr. Lee Schwartzberg played pivotal roles in Raquel's diagnosis and subsequent treatment plan. Their expertise, compassion and commitment to patient care left an indelible impact on Raquel's experience. Their thorough examination and comprehensive approach ensured that Racquel received the best possible care for her invasive lobular carcinoma. In addition to the care provided at Renown, Raquel greatly benefitted from being connected with a mentor by Dr. Chu. This mentor, Kayla, had undergone a similar diagnosis and treatment plan, and at the same age Raquel. They texted and called each other throughout Raquel’s treatment, providing additional support through a challenging time. As of January 2024, Raquel is done with her treatment and continues to see her care team for follow-up appointments. “I’m through the worst and ready to rebuild my life,” Raquel said. To help celebrate this milestone, Nevada Athletics invited Raquel to receive the game ball at a Nevada Men’s Basketball game. She was joined on the basketball court for this special recognition by her husband, Raul; mother, Arlene; and two daughters, Ryleigh and Rhiannon. Racquel's journey is not only a testament to her resilience but also a tribute to the invaluable contributions of Dr. Chu and Dr. Schwartzberg in guiding her towards triumph over breast cancer.
Read More About Celebrating Resilience: Raquel's Remarkable Journey Through Breast Cancer Treatment
-
A Transformative Journey: Mary's Bariatric Surgery Story at Renown Health
Embarking on the path to bariatric surgery is a unique and deeply personal journey. Individuals like Mary Escobar choose this life-changing route for reasons ranging from improved cardiovascular health to managing diabetes or finding relief from various health complications. In Mary's case, her two-decade-long healthcare journey not only underscores the challenges she faced but also highlights the support and expertise that ultimately led to her successful transformation through bariatric surgery. Mary's Resilience: December 2002 through February 2003 More than two decades ago, Mary experienced unforeseen health complications just days after giving birth via c-section. Septic shock, hemolytic uremic syndrome, thrombocytopenia, renal failure and a blood clot in her lung plunged her into a critical state. Intensive care, plasma exchange and a long recovery followed. After being discharged with compromised kidney function, Mary faced complete renal failure two years later, leading to dialysis and a spot on the donor list. Mary's brother, a perfect match, selflessly donated his kidney on Dec. 14, 2007, marking a turning point in Mary's health. However, the post-transplant period brought new challenges, including diabetes, high blood pressure and a significant weight gain, reaching 230 pounds. Determined to regain control, Mary explored various diets without success until she consulted with a bariatric doctor. Journey to Bariatric Surgery: November 2009 - April 2021 In November 2009, Mary opted for a gastric band, shedding 40 pounds within a year. Despite initial success, issues with the gastric band arose, prompting a consultation with Dr. John Ganser at Renown Health in April 2021. Together, they decided to transition to a gastric sleeve, with comprehensive education provided to ensure long-term success.
Read More About A Transformative Journey: Mary's Bariatric Surgery Story at Renown Health
-
Department Spotlight: Special Procedures
Chronic pain can be one of the most distressing feelings someone may encounter – and more likely than not, you know someone who is managing their pain as a part of their healthcare journey. In fact, according to the Centers for Disease Control and Prevention, about 1 in 5 U.S. adults have experienced chronic pain in recent years. One of the most common methods of treating pain is through prescription pain medications; however, with the rise of the opioid epidemic across the country, leveraging other interventions to help patients manage their chronic pain has become increasingly more important. What if there was a way to treat pain directly without the automatic need for pain medication? Luckily for patients in northern Nevada, our Special Procedures department at Renown Rehabilitation Hospital specializes in exactly that: interventional pain mitigation sans painkillers. With nearly 95% of their patients who come in with pain-related mobility issues being able to physically walk out of the hospital after their treatment, much-needed relief is clearly in store. Tight-knit and forever-caring, the Special Procedures team knows how to transform the purpose of pain management. A Penchant for Pain Alleviation Renown's Special Procedures team offers a wide variety of pain management solutions that are uniquely tailored to each individual patient’s needs. With the help of a team of 14 attentive nurses, interventional radiology technologists and a surgical technician – plus a dedicated patient access representative ensuring everything goes smoothly behind-the-scenes – these lifechanging interventions include: Epidurals (including steroid epidurals) Nerve blocks Ablations Tenotomies Spinal cord stimulator trials Peripheral nerve stimulator trials The nurses on this specialized team guide patients before, during and after their procedures, making sure they are at ease throughout the entire process. Each nurse emulates both expertise and empathy to help light the path towards healing. “Before each procedure, we get the patient’s vitals, health history and work with the doctor to answer any questions they may have about what is going to happen in the procedure room,” said Michon Edgington, RN. “After they’re all done, they come back to me, and I make sure they are ready to go home by educating them on their discharge. Our goal is to get them back to their families very quickly.” “In the actual procedure room, we perform safety checks, do charting, prepare the sterile tray for the doctor and give medication for conscious sedations, all while consistently monitoring the patient and helping the doctor out along the way to help the procedure go well,” added Shannon Boelow, RN. This team’s dedicated imaging professionals harness expertise that goes beyond capturing images. Their skillful utilization of X-ray technology serves as a guide for doctors administering treatments for pain – and according to our own physicians, our imaging technologists are some of the best in the business. “Our X-ray skills here are specialized,” said Julie Smith, Imaging Lead. “Visually, the doctor needs to see what’s going on inside the body so they can accurately place needles and steroids. We all work together collectively and work with each doctor to accommodate their preferences, helping the treatments go much faster and minimizing the patient’s exposure to radiation.” Serving as the ideal representation of both precision and support, the surgical technician on this team is an important collaborator in the procedure room, helping to ensure the success of every interventional procedure with a meticulous eye for detail. “As the Special Procedures surgical technician, I get the room ready with all the necessary instruments, including making sure everything is sterile,” said Carrie Crow, Surgical Technician. “I enjoy keeping the team organized.” Overseeing it all are the physicians, who are eternally grateful for the team for the life-changing interventions they offer every day. “Our physicians are so phenomenal,” said Brittney Summerfield, Manager of Nursing. “They are very supportive and collaborative, and they always do the right thing. They have total confidence in us.” Seeing patients walk out of the hospital happy and healthy is a driving motivator for this team. Whether they had significant experience in pain management or were ready for a completely new challenge, each team member comes to work every day inspired to move mountains. “I had worked in pain management in other facilities, and I was extremely excited to come here and solely focus on pain,” said Jodi Eldridge, Supervisor of Special Procedures. “I enjoy seeing the patients so happy when they leave no longer in pain. I feel immediate gratification, because you truly feel like you’re doing something big for the patient. It’s very rewarding.” “I decided to come work here because I worked in the inpatient setting for a long time, and I was ready to see a different side of healthcare and provide a different type of care to our community; plus, my coworkers are the best,” added Lisa Dunnivant, RN. There’s no question that the realm of pain management is a delicate one – and there is no team better suited to take on that challenge than Special Procedures, working harmoniously to bring relief and a renewed sense of livelihood for every patient they serve. “Some people believe pain management is just all about pills, and that is simply not true,” said Carrie Crow. “Our procedures are yet another way to help them manage their pain and find relief.”
-
What You Need to Know About RSV
Respiratory syncytial virus, also known as RSV, is a common respiratory virus that impacts the lungs and breathing pathways. The virus can be dangerous for infants and young children and is also concerning for older adults. While most older kids and adults only experience cold-like systems and recover in a week or two, an estimated 58,000-80,000 children younger than 5 years old are hospitalized due to RSV each year, and in 2022 healthcare organizations across the country are experiencing higher infection rates than in years past. "We are experiencing a strong RSV season and do not expect it to go away anytime soon," said Dr. Kris Wilson, Division Chief of Renown Children's Primary Care. "Infants who are infected with RSV almost always show symptoms of runny noses and cough. Call your healthcare provider immediately if your child is having difficulty breathing, is not drinking enough fluids, or is experiencing any worsening of these symptoms.” Symptoms of RSV: Runny nose Decrease in appetite/inability to drink Dry diapers, an indication of dehydration Cough, which may progress to wheezing or difficulty breathing Irritability (most common in very young infants) Decreased activity (most common in very young infants) Decreased appetite (most common in very young infants) Apnea, pauses in breathing for more than 10 seconds (most common in very young infants) What to do if you think your child has RSV: Call your pediatrician! If you suspect your child might have RSV, consulting their healthcare provider is the best first line of defense. From here they will help you build an appropriate treatment plan for child. Keep in mind that many pediatrician offices offer 24/7 call lines. If your child is experiencing retracted breathing (when the area between the ribs and in the neck sinks in when a person attempts to inhale), dehydration (not drinking and decrease in wet diapers) or apnea (pauses in breathing for more than 10 seconds) please call 911 or go to the closest emergency room.
-
COPD Explained: Protecting Your Lungs and Managing Symptoms
COPD (chronic obstructive pulmonary disease) is a progressive lung condition often mistaken for typical aging signs, like shortness of breath and coughing. While smoking and pollution can contribute to its development, lifestyle changes and medications can help manage its progression. Diagnosis typically involves lung function tests, chest X-rays, or CT scans, with treatments available through a pulmonologist or primary care provider. Renown’s Pulmonary Rehabilitation Program offers insights into living with COPD. What is COPD? According to the COPD Foundation, it is an umbrella term used to describe progressive lung diseases including: Emphysema: Damage to the small air sacs in the lungs (alveoli). Chronic Bronchitis: Irritation and swelling of bronchial tubes, causing shortness of breath and coughing for long periods of time. Asthma (non-reversible): When asthma medications cannot reduce swelling in the airways. COPD Risk Factors Smoking is the most significant COPD risk factor, and the American Lung Association (ALA) says it accounts for nearly 90 percent of cases. If you are a smoker, it is essential to seek help and quit. Other COPD risk factors include: Air pollution Genetics Second-hand smoke Chemical, fumes or dust in the workplace How Can You Protect Yourself? Stop smoking Renown Health provides support offering 4-week Smoking Cessation Virtual Classes, free of charge! Sign up today. Use natural cleaning products Many household chemicals, especially those containing bleach, can irritate the lungs – a condition called, chemical pneumonitis. Stay away from all types of smoke This includes smoke from fireplaces. Likewise, plan to stay indoors when it is smoky outside, or air quality is poor. Get active Of course, it’s never too late to start an exercise program. When exercising your heart pumps, circulating your blood and sending oxygen to every part of your body. Notably it strengthens your lungs, making it easier to breath. Talk to your doctor to see if you are healthy enough to begin exercising. Eat a healthy diet Surprisingly what you eat can affect your breathing. The American Lung Association encourages those with COPD to watch their sodium intake, eat smaller, more frequent meals (instead of three large ones), limit high fat foods and drink plenty of water. Avoid scented products Perfumes, aerosol sprays and plug-in air fresheners can trigger flare-ups. Get a flu shot Did you know chronic lung conditions, as well as, heart disease, cancer and diabetes, can be made even worse by the flu? Now is the time to get your flu shot for the season if you haven’t already. Renown’s Pulmonary Rehab staff is certified through the American Association for Cardiovascular and Pulmonary Rehabilitation (AACVPR). Recently, Renown Regional Medical Center successfully completed a disease specific COPD certification survey by The Joint Commission. For two accreditation cycles in a row, the COPD Program has had zero findings during the rigorous survey.
Read More About COPD Explained: Protecting Your Lungs and Managing Symptoms
-
Why I Give: Dan’s Story
In the fall of 2020, Dan's world was suddenly shaken when he received a distressing call: his son, Jeremy, was admitted to Renown with complications from spinal meningitis. Without a second thought, Dan rushed from Southern California to be by Jeremy's side. For an agonizing 10 days, Dan remained in the ICU. He was overwhelmed with worry and helplessness as Jeremy fought for his life on a ventilator. During this time, Dan, an esteemed artist and professor, found comfort in the collection of artworks adorning the walls at Renown. With more than 2,000 pieces of original art, Renown has meticulously curated hospital rooms, hallways and various spaces to support those in need. Dan, who talks about art's magic every day as a professor, experienced its power in a new light.
-
Celebrating World Lung Day in Northern Nevada
In the United States, electronic cigarettes are the most popular form of tobacco product used among high school students. Approximately 21% of Washoe County area high schoolers report current use of e-cigarettes, higher than the national average of 14% reported in the most recent national data. While often viewed as a safer alternative to traditional cigarette use, e-cigarette use, commonly referred to as vaping, exposes users to nicotine and harmful chemicals that stunt brain development, results in lung damage and harms overall health. In partnership with Reno area school principals and nurses, the Renown Health – UNR Med Clinical Research Office was able to provide this year’s World Lung Day Anti-Vaping Program to Galena High School, Robert McQueen High School and Sage Ridge School, reaching hundreds of high school students.
Read More About Celebrating World Lung Day in Northern Nevada
-
6 Healthcare Action Items for the LGBTQIA+ Community
© Niyazz via Canva.com Every patient, regardless of how they may identify, greatly benefits from preventive healthcare and early detection. Members of the LGBTQIA+ community face unique considerations when it comes to their health, and a proactive approach to preventive screenings and vaccines is important in order to address their individual health needs. Dr. Karen Thiele, Family Medicine Physician with University Health and Assistant Professor of Family and Community Medicine at the University of Nevada, Reno School of Medicine, breaks down key steps that LGBTQIA+ patients should take to safeguard their health. PrEP and PEP Pre-exposure prophylaxis (PrEP) is a strategy to prevent human immunodeficiency virus (HIV) infection. It is an important measure for those who are HIV-negative but may be at risk of contracting it. The highest risk sexual practice is receptive anal intercourse, due to the relative fragility of rectal tissue. This medication can stop HIV from spreading in the body and help patients maintain their HIV-negative status. PrEP is available in both pill form, which is taken every day, and injection form, of which the first two injections are initiated one month after another while all other injections are initiated every two months. Post-exposure prophylaxis (PEP) is an antiretroviral drug regimen taken after potential HIV exposure to prevent an HIV-negative individual from converting to HIV-positive status. PEP is only for emergency situations and must be started within 72 hours of exposure – sooner is always better than later – and must be taken for 28 days. PrEP and PEP are available in many ways, including visiting your primary care provider (PCP) or an urgent care location. HPV Immunization All genders and identities can protect themselves against human papillomavirus (HPV), a sexually transmitted infection (STI) that can lead to the risk of cervical, mouth, head, neck, throat, anal, vaginal, penile and vulvar cancers. HPV is so common that nearly all sexually active people, regardless of sexual orientation and practices, will be exposed at some point in their lifetime. The HPV vaccine (common brands include Gardasil and Cervarix) is a safe and effective method to prevent HPV, according to the Centers for Disease Control and Prevention (CDC). This vaccine protects against infections that can lead to HPV-related cancers and precancers, as well as genital warts. While patients should start receiving the vaccine at 9 years old years old, unvaccinated adults up to the age of 45 can also receive the vaccine through their PCP – better late than never! STI Testing Sexually-transmitted infections form from bacteria, viruses or parasites that can be transmitted by person-to-person sexual contact through semen, vaginal, blood and other bodily fluids. According to the U.S. Department of Health and Human Services, there are more than 20 million estimated new STI cases across the nation each year. Luckily, most STIs are preventable. Annual STI testing for HIV, gonorrhea, chlamydia and syphilis is important to stay on top of your sexual health. Because these STIs may sometimes have no symptoms, screening is recommended regularly and with any change in sexual partners. Depending on the specific condition, tests for these infections include urine, swab and blood tests. Speak with your primary care provider on a screening schedule that works best for you. Prostate Exams Prostate exams look for early signs of prostate cancer in patients who still have a prostate. The CDC recommends those who are at least 55 years old get regular prostate screenings; however, for patients with a family history of prostate cancer, screenings may be recommended as early as 45 years old. These exams are done via two common methods – a prostate specific antigen (PSA) blood test and a digital rectal examination (DRE). Your provider can help you determine your risk and when you should start getting screened. Pap Tests and Pelvic Exams Patients of all genders who have a cervix, uterus, vagina and/or ovaries will benefit from regular pelvic exams and Pap screenings. A pelvic exam consists of a provider looking inside the vagina and at the cervix for anything unusual. A Pap test, also known as a Pap smear, involves your provider using a small, soft swab to collect cervical cells to check for early signs of cancer. Generally speaking, people with these organs should have a Pap test every three years starting at age 21 through the age of 30. After age 30, patients should receive a Pap test with HPV co-testing every five years until age 65. These recommendations are changing based on new research, so it is important to have a conversation with your PCP about the current guidelines so you can make an informed choice about what schedule you should follow. A gynecologist or your primary care provider can counsel you and perform these screenings. Mammograms and Breast Exams People with breast tissue, especially dense breast tissue, are at risk for breast cancer, and regular breast screenings are your best line of defense. At-home breast self-exams are the first step – you will want to check your breasts for any lumps, changes, fluid leaks, irregular tissue thickening or anything else that feels unusual. The Breast Cancer Risk Assessment tool, provided by the National Cancer Institute, is a good place to start to identify your risk. Talk with your primary care provider about the risks and benefits of starting screening at age 40 so you can make an informed decision about when to start. If you have any family history of breast or ovarian cancer, your PCP will offer you genetic testing for BRCA 1 and 2 mutations. Nevadans over the age of 18 can also get BRCA genetic test for free by enrolling in the Healthy Nevada Project. Mammograms are important screening tools, but for a significant portion of people with breast tissue, density of the breast tissue may make mammograms less helpful in detecting cancer. Your primary care provider can help you decide what additional imaging (such as breast ultrasound) might be best for you.
Read More About 6 Healthcare Action Items for the LGBTQIA+ Community
-
How to Treat a Sprain or Strain
Injuries happen to everyone. They are caused by participating in sports, recreational activities like hiking, and even by accidentally stepping off a curb wrong. If you experience a sprain or strain, the first few days are often the most painful. Renown Sports Medicine physicians Luis Palacio, MD and Brandon Hockenberry, MD walked us through what to do after an injury. Listen to Your Body See a medical professional right away if: You know or suspect that a bone is broken You are having difficulties putting full weight on a joint of the leg Pain or swelling is severe There is a sign of an infection, such as redness and warmth in the joint The First 24-72 Hours Joint sprains tend to swell more than muscle strains. You can use ice as needed for comfort and to relieve any pain, but do not use ice for more than 15-20 minutes at a time. Ice and NSAIDs (such as ibuprofen) can help prevent excessive swelling and mask the pain, but they do not speed recovery. Some research shows that overuse of ice actually delays recovery. During the first 24-72 hours, your injury will go through an inflammation phase. Inflammation is your body’s natural way to dispose of dead tissue cells, build new healthy structures, and hopefully heal even stronger than before.
-
Living with COPD? How to Maximize Your Summer Experience
June offers an official welcome to summer and the height of outdoor activities in northern Nevada such as hiking, camping, days spent at the lake and embracing long days and warm evenings with friends and family. Enjoying all that the summer season has to offer may not be as easy for those living with chronic obstructive pulmonary disease, or COPD, which effects more than 15 million Americans. What is COPD? COPD is a group of lung diseases including emphysema and chronic bronchitis that result in airflow blockages from the lungs. People may experience frequent coughing and shortness of breath among other symptoms. COPD typically impacts adults ages 65 and older and is becoming increasingly more common among women. Although smoking plays a key role in the development of COPD, air pollution and indoor air quality, and respiratory infection also contribute to disease development. While there is no cure for COPD, limiting progression of disease and managing symptoms can be achieved through lifestyle changes, therapy, and medications. Tips for Living with COPD This Summer, and Always Stay Hydrated: Staying hydrated is extremely important for people with COPD, especially during the summer. Not drinking enough water can make breathing more difficult because it increases respiratory symptoms. Make sure to always keep a water bottle with you and aim to drink 8-10 glasses of water daily. Be Mindful of Temperature: COPD symptoms can be exacerbated by hot weather. It is best to participate in outdoor activities during the cooler times of day, like the morning or evening. Check Air Quality Before You Go: Before engaging in outdoor activities, be sure to check the air quality index and plan your activities accordingly. Pace Yourself: Exercising can be difficult for people who have COPD. To make the most of your summer, try not to push yourself too hard and take breaks when you need them. If you start to feel out of breath or tired, take a break in a cool, shaded area until you feel better. Take Matters Into Your Own Hands To address the needs of community members living with COPD, the Renown Health Research Office has teamed up with Pulmonary Medicine to provide patients who are former or current smokers and have a history of frequent exacerbations with an option to participate in the ARNASA study. "COPD exacerbations have a huge negative impact on patient’s lung function” states Dr. Farah Madhani-Lovely, Chief of Pulmonary Medicine at Renown Health and Assistant Dean of Clinical Research at the University of Nevada, Reno School of Medicine. “We have had inhalers and prednisone for decades but patients are still having exacerbations. Now we have a new pathway we think will prevent exacerbations which is what this clinical trial is designed to prove.” This study will evaluate the efficacy and safety of astegolimab compared with placebo in participants 40-80 years of age with COPD. “This study in particular is so exciting because of the enthusiasm from the sponsor’s end” says Katie Buckley, Lead Clinical Research Coordinator working on pulmonology studies at Renown’s Clinical Research Office. “Often times sites aren’t assigned particularly passionate or engaged personnel who aid in carrying out these studies, but you can tell Roche Genentech’s team truly cares about the success of the study, the safety of their participants, and proving the efficacy of the investigational agent. Working on a study like this takes a village, and when the individuals on all ends share similar mindsets and work towards success as a collective unit instead of as individual moving parts, it’s amazing to see everything we’re able to accomplish.” Renown’s team of expert pulmonologists and researchers are available to join patients with COPD in support of their healthcare journey. If you are interested in learning more about this clinical trial option at Renown Health, talk to your pulmonologist at your next appointment or contact us at 775-982-3646. At Renown Health, our goal is to make it easy for patients to access clinical research as a care opportunity where patients can access a variety of standard care treatment options for their health condition or choose to participate in a clinical trial. For more information about clinical trial opportunities available to you or to ask any questions, contact the Renown Research Office at Renown-CRD@renown.org or 775-982-3646.
Read More About Living with COPD? How to Maximize Your Summer Experience