Search
-
The Unmatched Health Benefits of Snowshoeing
Snowshoeing is an excellent winter workout that can help burn calories, strengthen muscles and boost cardiovascular health. Explore the top 8 snowshoeing spots and experience this ultimate workout adventure! Significant Health Benefits: Exceptional cardiovascular workout – burn up to 1,000 calories per hour! Low-impact muscle building Endurance building Balance strengthening and agility Improves your sense of well-being by connecting to nature Prepping for Your Adventure There are some crucial details to think about when it comes to snowshoeing, especially if you are a beginner. Make sure to pick the right kind of footwear to go on top of your snowshoes; a pair of comfortable waterproof boots are a great choice and remember to wear lots of layers. Several local places rent snowshoes if you aren’t sure about spending money on a pair. Check out Bobos Ski and Board Patio or our local REI Co-Op. Check out REI’s Beginner’s Guide to Snowshoeing for reference. 8 Cool Snowshoeing Spots 1. Galena Creek Park Close to Reno, this beautiful, low-altitude park offers several trails. You’ll find various creeks and streams under cover of pristine ponderosa pines. From beginner to advanced, the differing trail systems provide a challenge for everyone! Head west on State Route 431 (Mt. Rose Highway) for about seven miles until you see the park sign on the right side of the highway. 2. Tahoe Meadows – Chickadee Ridge This local favorite not only gives fantastic views of Lake Tahoe but the best part? – friendly little chickadees will eat seeds right out of your hand! Be sure to pack plenty of sunflower birdseed, as that seems to be their favorite. From the trailhead parking lot, head southeast into the open meadow. Then follow the ridgeline to your right (southwest). Continue southwest up toward the top of the ridgeline to the west, and you’ll get to Chickadee Ridge in just under two miles. 3. Spooner Lake Trail The easy 2.5-mile loop around Spooner Lake is excellent for all skill levels. This alpine lake is surrounded by aspen trees which house varied bird species, so bring your binoculars! Dogs are allowed on a leash, and all-day parking is $10. 4. Kirkwood Ski Resort You’ll need a trail pass, but this South Lake Tahoe resort has various routes from beginner to advanced, with roughly 50 miles of terrain. Nighttime snowshoe treks during the full moon are also available throughout the winter. Kirkwood is located on Highway 88, close to Carson Pass. 5. Camp Richardson Heading north, you can find this well-established and favorite local snowshoeing spot. If you’re up for an adventure, you can trek up to Fallen Leaf Lake. It’s located off Highway 89 and near Fallen Leaf Road. 6. Dry Pond Loop This moderate, 6.5-mile loop near Washoe Valley has impressive views of Carson Valley, Washoe Lake, and the Mt. Rose Wilderness. If you like the sound of rushing water, most of the trail meanders along White’s Creek. This area is dog-friendly and kid-friendly, which makes it a family favorite. 7. Royal Gorge Soda Springs is home to this resort, which is well known for its cross-country skiing trails. Enjoy extensive trails leading deep into the trees with spectacular views. Find Royal Gorge from the Soda Springs exit on West Interstate 80. 8. Ash Canyon Creek Tucked away in the Carson Valley, these trails are filled with mountain bikes in the spring and provide excellent snowshoeing trails in the winter. Find it from Interstate 580 by taking the Highway 395 Business exit to Winnie Lane.
Read More About The Unmatched Health Benefits of Snowshoeing
-
Strategies for Lasting Weight Loss
Managing weight is a complicated and often difficult journey for many individuals, and obesity stands as a common and serious chronic health condition. In fact, the Center for Disease Control and Prevention reports that the prevalence of obesity in the US is greater than 40% in adults and 20% in children, and those numbers are continuing to climb. In Nevada, according to the 2020 Behavioral Risk Factor Surveillance System, 28.7% of adults reported being obese. By 2030, almost 80% of American adults may be overweight and half of them will be obese. But obesity isn't just about the numbers on the scale; it's a multifaceted, lifelong, neurobehavioral disease triggered by a combination of factors. These include abnormal eating patterns, reduced physical activity levels, environmental stressors, genetics and various other contributors. Obesity extends far beyond appearance, often leading to the development of numerous medical conditions such as diabetes, heart disease, elevated blood pressure, stroke, sleep apnea, liver disease, various cancers and infertility. Join us as we delve into the complexities of obesity and explore strategies for effective weight management available right here in northern Nevada. Why Can Losing Weight be so Difficult? The challenge behind weight loss finds its roots in the Set-Point Theory of Obesity, a concept that says our bodies have a predetermined weight, or fat mass, within a defined set-point range. In other words, when an individual's weight deviates from this set point, the body initiates mechanisms to bring it back to the established range. So, if someone loses weight below their set point, the body may respond by increasing hunger and reducing metabolism, making it challenging to sustain weight loss. There Isn’t One Right Answer, But Renown is Here to Help Various weight management strategies can be utilized by patients struggling with obesity, which may lead to substantial weight loss, resolution of associated medical conditions and improved psychosocial health. In fact, the most successful strategy involves a multidisciplinary approach under the guidance of trained specialists that includes a combination of tactics, including: Behavioral adaptations Dietary modifications Physical exercise Anti-obesity medications Weight loss surgery
-
Patty Warren A Woman of Strength and Resilience
Meet and get to know Patty Warren, our featured Sterling Silver Club member this fall. You may recognize her from the latest Senior Care Plus commercial on television, where she joins a coffee chat discussing the many benefits of being a Senior Care Plus member. She’s one of the kindest souls you’ll ever meet – and has a positive outlook on life that we should all strive for. Patty's Story Patty was born and raised in a small Kansas town called Baxter Springs, where she grew up with an older brother, an older sister and two younger sisters. She and her siblings all enjoyed playing sports like softball and basketball, in addition to playing instruments. Patty developed a love and passion for music at a young age that carried into her adulthood. “I wanted to be an opera singer,” said Patty. “I decided to go to college at Pittsburg State University in Kansas where I majored in vocal performance.” After college, Patty moved to Manhattan in New York City to audition to be an opera singer, but she soon realized it wasn’t what she wanted to do after all. She eventually decided to work in the brokerage industry. After living and working in New York for three years, Patty moved back to Kansas where she later met the love of her life, Michael. “In 1992, I had put a dating ad in the local newspaper,” said Patty. “I received over 30 responses, and I went out on quite a few dates.” Then she had her first date with Michael, and the two of them quickly realized how much they liked each other. He asked her to marry him on Valentine’s Day in 1993, and they went on to get married in front of the Justice of the Peace on May 3, just a few months later. “We had a small wedding so that we could move into our first home together,” said Patty. A few years later in 1999, Patty and Michael moved to Arizona, where they lived for 22 years. Patty worked at Edward Jones Investments for 18 of those 22 years and loved her job and the people that she worked with. She retired in January 2021 during the pandemic, and three days later she and Michael moved to Sparks, Nevada.
Read More About Patty Warren A Woman of Strength and Resilience
-
Sepsis: Causes & Symptoms
According to the Global Sepsis Alliance, 1 in 5 deaths worldwide are associated with sepsis. If not recognized early and treated promptly, sepsis is the final common pathway to death from most infectious diseases worldwide, including viruses such as COVID-19. We spoke with Jeremy Gonda, MD, a critical care physician from Renown Health’s Sepsis Committee to increase public awareness of this preventable medical emergency. What is sepsis? Sepsis is a response to infection—bacterial, viral or fungal—and can start anywhere in the body and spread into the bloodstream. The body is trying so hard to fight an infection that it begins releasing chemicals into the bloodstream that cause inflammation and the shutdown of multiple organ systems. “It carries a very poor prognosis in general unless you catch and treat it very early,” said Dr. Gonda. “Any infection can lead to sepsis. Typically your immune system takes care of the infection. It doesn’t progress, but in cases where the infection becomes severe, or the immune system doesn’t function properly, people can certainly die. So there’s, unfortunately, a very high mortality rate associated with sepsis.” According to the Centers for Disease Control and Prevention, each year at least 1.7 million adults in America develop sepsis. While you can recover from sepsis if caught early, many sepsis survivors suffer from long-term physical and psychological effects. What are the signs of sepsis? One way to spot sepsis is to use the acronym SEPSIS: S – Slurred speech and confusion E – Extreme shivering or muscle pain/fever P – Passing no urine all day S – Severe breathlessness I – “I feel like I might die” S – Skin mottled or discolored Keep in mind that sepsis symptoms can vary depending on where the infection starts. “Patients may experience urinary burning if they have a urinary tract infection or a cough and shortness of breath if they have pneumonia first,” said Dr. Gonda. “However, often symptoms are more generalized or subtle such as fevers, confusion and malaise.” How do you develop sepsis? When germs enter your body, they can cause an infection. If you don’t stop that infection, it can cause sepsis. Areas of infection that more commonly result in sepsis include: Lungs, such as pneumonia Kidney, bladder and other parts of the urinary system Digestive system Bloodstream (bacteremia) Catheter sites Wounds or burns Who is most at risk? People with compromised immune systems are at greater risk for sepsis, such as “The very young, the elderly and any people who may have conditions that suppress your immune system,” said Dr. Gonda. “For instance, if you have diabetes or if you’re an organ transplant patient who is on immunosuppressant therapy, you’re at somewhat higher risk.” Sepsis is often considered a hospital-acquired infection, but a study in The Journal of American Medical Association found that 80% of sepsis cases occur outside of a hospital. That’s why it’s especially important to remember any infection can lead to sepsis, and anyone can develop sepsis from an infection. What do I do? Timing is critical in the case of sepsis and septic shock. According to a study on septic shock patients, there is a 7.6 percent decrease in survival for each hour treatment is delayed. On the other end, if treatment is given within an hour of the first drop in blood pressure, the survival rate is 80 percent. Because sepsis can be so deadly, it’s important to seek medical attention as soon as possible. “If you’re not getting any better, if you think symptoms are progressively worsening – you should definitely be evaluated by a doctor,” said Dr. Gonda. You can help #StopSepsis by getting involved at worldsepsisday.org.
-
Department Spotlight: Renown Transfer and Operations Center
Stepping into the Renown Transfer and Operations Center (RTOC) means stepping into a transformative hub of excellence where lives are saved and healthcare is reimagined. As a cornerstone of Renown Health's commitment to exceptional patient care, the RTOC serves as a dynamic nerve center that seamlessly coordinates medical resources, ambulance rides, hospital bed space, remote home systems, hospital transfers and emergency preparedness. In this best-in-class facility, the boundaries of what is possible in healthcare are constantly pushed, and new horizons of patient care are discovered. Staffed with a dedicated team of skilled professionals, the RTOC harnesses the power of advanced technology and compassionate expertise to ensure that patients receive the highest level of care and support, no matter where they are. Through a synchronized network of communication, coordination, and compassionate care, the RTOC team ensures that patients receive the critical support they need when it matters most, working tirelessly to redefine what it means to deliver world-class healthcare. A National Standard Charged with the goal of overseeing the placement and transportation for every patient, the RTOC officially launched in 2021 as northern Nevada’s first and only transfer center of its kind and a nationally celebrated facility. As Renown’s highly coordinated care logistics system, this team uses the cutting-edge technology at their fingertips to customize healthcare to the needs of every patient, manage patient flow and drive healthcare innovation. “Compared to where we’ve started to where we are now, it’s a 180-degree difference,” said Kelli McDonnell, Manager of RTOC. “When we first started building our facility right before the pandemic happened, we took what was six conference rooms and classrooms and turned it into a command center that organizations across the country admire and come to Reno to see what we do. Mel Morris, the Director of RTOC, was recruited exclusively to build our facility with her history of building successful hospital command centers. Many people didn’t realize what a transfer center was or that Renown was the only center in the region – and we only continue to grow.” This best-in-class facility, and the masterful team behind it, handles: Coordinating all incoming patients transferred from neighboring hospitals and 27 counties across northern Nevada, Lake Tahoe, northeast California and neighboring states. Matching patients to the most appropriate bed placement using diagnostic, triage and Epic electronic medical record clinical information in conjunction with medical staff expertise to outline a plan of care that determines the best bed assignment given the patient’s needs. Coordinating video-enabled Telehealth monitoring capabilities for Renown’s four Intensive Care Units (ICUs), as well as Renown patient Telehealth and virtual visits. Monitoring Remote Home systems with Masimo during the COVID-19 pandemic, where some patients received hospital-level care in the comfort of their own homes while Renown clinicians monitored and evaluated their data and plan of care. Serving emergency and disaster management for area hospitals, first-responders and the community with local, regional and statewide emergency and disaster management for sudden-onset emergencies. The RTOC is home to many different critical roles for our health system, including Transfer Center Nurses, Ride Line Coordinators, RTOC Coordinators and more, many duties of which each team member cross-trains on to be able to fill in whenever needed. While their roles may differ, their commitment to their patients remains the same – and they all work together to achieve the same outcome: delivering the right care, at the right time and place. “As an RTOC Coordinator, we do a variety of different things,” said Anna Schaffer, RTOC Coordinator. “We do triage coordination to help our nurses and hospitalists get patients in the emergency department admitted, and we also do bed control to find patients appropriate bed placement. Communication is important, so we always make sure to stay closely connected with the charge nurses on those floors.” “We start with a basic ‘need to know’ and place patients accordingly,” added Karly Brown, RTOC Coordinator. “We get surgery numbers, ICU capacity and discharges and find beds for all patients as quickly as possible. We have the advantage of being able to see the entire hospital.” “I primarily schedule transportation for patients at the hospital who are either going home or going to a skilled nursing facility,” said Sarah Clark, Ride Line Coordinator. “I get requests from case managers to schedule rides, and I work with REMSA and other ambulance services to schedule them. It relies a lot on appropriate and efficient communication and critical thinking.” Patients in facilities across northern Nevada and northeastern California, especially the rural communities, look to the RTOC to help guide ambulances, bed coordinators and hospital staff in finding care for our rural patients. “As a transfer center nurse, I facilitate incoming patients from rural facilities in Nevada and surrounding areas in California,” added Meg Myles, Transfer Center Nurse Specialist. “There are days we may take up to 30 direct admissions from these areas.” “We are the point of contact for inter-facility transfers, whether we are sending patients out or bringing them into Renown,” said Lisa Lac, Transfer Center Nurse Specialist. “We take phone calls from those rural areas, identify what services are needed, connect them to the appropriate provider and coordinate any transfers.” “Simply put, we are the bed wizards,” said Addison Rittenhouse, RTOC Coordinator. The RTOC team continues to break barriers and push the boundaries of medical excellence through leveraging the technology at their fingertips and their unwavering dedication to the health of our community. Inspiring a new era of medical possibilities, these team members have achieved a multitude of accomplishments for both their department and their patients since the birth of the center. “We have significantly reduced the time it takes to get patient admit orders in, thanks in part to the new Triage Coordinator role, and we provide easier access for patients to transfer to us from other facilities,” said Beth Rios, RTOC Coordinator. “We have taken a bigger role in helping the smaller hospitals in our area in caring for patients and improve patient throughput.” “As a team, we’ve done a lot of work in creating an engaging and positive environment, and our internal morale committee has been a huge help with that,” said Kelli McDonnell. “We’ve been working tremendously over the last year and taking all the feedback that we received from the Employee Engagement Survey to make improvements. We had 100 percent survey participation within five days, which is incredible.” “I am so proud of our escalation and problem-solving skills,” said Becca Dietrich, RTOC Coordinator. “When an issue is raised to us, we will always find a timely solution on our end so our care teams can focus on the issue in front of them. We are the eyes in the sky, seeing movement everywhere.” Each day in the life of our RTOC team members is a testament to their commitment, resilience and timework, making a profound impact on countless lives.
Read More About Department Spotlight: Renown Transfer and Operations Center
-
What Does a Doula Do?
If you’re expecting a new baby, you may have been given the advice to hire a doula. You may have seen statistics of improved outcomes among those who’ve had a doula attend their birth. Perhaps you’ve heard that the etymology is from the Greek word meaning “to serve.” But how does a doula serve their clients? A doula is a non-medical birth professional who will guide you through labor, birth, postpartum and beyond. Your doula can discuss your options with you so you can make informed decisions, as well as provide emotional and physical support to ease your experience. While each doula offers their own style, there are certain services that most doulas will provide for their clients. Typically, a birth doula will provide at least one prenatal visit, one postpartum visit and continuous support during active labor. A postpartum doula usually provides support during the 12 weeks immediately following birth, sometimes referred to as the “fourth trimester,” but some will continue care after that as well. Simply put, a doula provides informational, physical and emotional support during the childbearing year(s). Let’s take a closer look at these three ways a doula can support you. The Basics If you don’t know your options, you don’t have any. This is a common phrase in the world of birth work. When you’re in labor, you’re exhausted, in pain and there’s often urgency inherent or implied in any choices you make. So, when an intervention is offered, many birthing people accept it without question. One method that can help the decision-making process is to check your BRAIN: Benefits: What are the benefits of the proposed intervention? Risks: What are the risks of the proposed intervention? Alternatives: What are the alternative options? Intuition: What does your intuition tell you? Nothing: What if we do nothing? What if we wait? When you’re in active labor, you might have difficulty remembering this acronym; that’s where your doula comes in. At your prenatal visits, you can ask your doula for guidance in preparing your birth plan, which can include contingencies for certain potential interventions. And as choices arise during labor, your doula can guide you through the benefits and risks and can provide you with alternative options you might not otherwise be aware of that are available to you. Your doula can remind you to check in with your intuition and can help you quiet your mind so you can listen to your instincts. The Body Although we tend to see depictions of people giving birth on their backs with their feet in stirrups, this is only one of many ways to give birth. Walking and dancing can speed up early labor. Side-lying or hands-and-knees can prevent tearing during the pushing stage. Sometimes labor stalls, and a change of position is often helpful to get things moving again. Your doula can suggest positions depending on your stage of labor. Some labor positions might require the support of another person – your doula could fill this role or assist your partner in doing so. Some doulas also provide massage or even acupressure, and most will do the “hip squeeze” that so many laboring people swear by. If your baby is presenting posterior, or “sunny side up,” your doula can apply counter pressure to alleviate back pain during labor. Some postpartum doulas will do light housework while you rest and bond with your newborn. Others might care for your baby through the night so you can catch up on sleep. Many doulas have also gone through additional training to offer breastfeeding support and may be able to assist you with latch issues and nursing positions. The Mind Pregnancy, birth and postpartum periods can be some of the most emotional times in a person’s life. A doula will hold space for you and help you process your emotions before and after birth. It’s normal to feel apprehensive, or even fearful, about labor and birth, and discussing these feelings is the first step. A doula can help you navigate your concerns in a safe space so you can be prepared emotionally for your upcoming labor. Many doulas will also guide you through writing your birth plan, which can lessen anxiety about the unknown. If you have a history of trauma, your doula can assist in communicating this, so you don’t have to relive the experience every time you meet a new medical provider. Most people will experience some form of what’s often called the Baby Blues in the immediate postpartum period. The third day after birth tends to hit hard, as hormones attempt to regulate, but the Baby Blues can continue for weeks for some new parents. A postpartum doula’s support can be incredibly valuable during this time. When the baby blues last longer than a few weeks, it could considered a mood disorder. Most doulas will recognize signs of postpartum mood disorders and will have resources available for additional support. Choosing the Best Doula for You With so many wonderful doulas in northern Nevada, you might wonder how you could ever choose just one to attend your birth. Some expectant parents are unfortunately restricted by cost. With so many expenses related to a new baby, it can be difficult to budget doula services as well. Thankfully, Nevada Medicaid now covers doula care, and some commercial insurances are following suit. Check with your insurance company to find out if they might cover part of the cost for hiring a doula. If your insurance doesn’t cover doula services, some doulas offer a sliding scale based on income. You may want to interview multiple doulas to find the right one for you. If you’re the kind of person who wants all the information you can get, a more detail-oriented doula might be the best choice. But if you tend to feel overwhelmed by too many options, you might prefer a doula who only offers additional information as the situation calls for it. If you want massage or acupressure during labor, you might want to hire a doula with those certifications. Or maybe informational and physical support are not as important to you as emotional support, in which case your best choice could be a doula who has experience with postpartum mood disorders or trauma support. Regardless of who you hire, be sure to clearly communicate your desires and expectations – not just for your birth, but also for your doula. The most important thing when choosing your doula is trusting your gut. You need to feel comfortable with your doula, as they’ll be tending to you at one of the most vulnerable times in your life. When you find a doula that you click with, who listens to you and supports your choices, you have found the best doula for you.
-
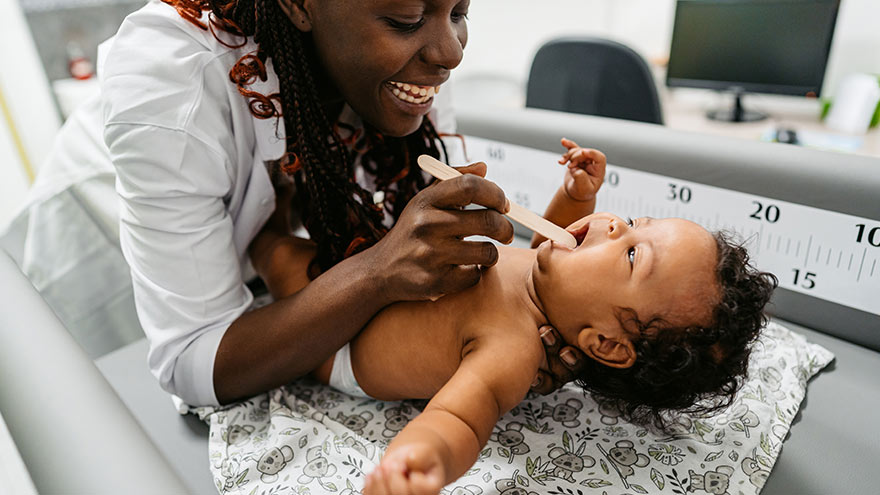
What to Expect at a Well Child Checkup
A well-child checkup is a great opportunity to monitor your child’s growth and development, and it's also a chance to establish a trusting relationship with your child’s pediatrician and have your questions answered. What to Expect at Each Checkup At every checkup, a comprehensive physical examination will be conducted to assess your child's growth parameters, including height, weight and head circumference. A developmental assessment will evaluate the progress of your infant or young child in achieving age-appropriate milestones, encompassing language skills, motor development, problem-solving abilities and psycho-social skills. In addition, your pediatrician will address common concerns such as feeding, sleep patterns, oral health and general infant care. Unless there are specific needs or concerns for your baby, routine laboratory tests are typically unnecessary. Your pediatrician will provide guidance on immunization schedules, post-vaccination expectations and when to seek medical attention. Furthermore, during each visit, you will receive age-specific guidance to help you anticipate your child's expected growth and development, along with essential safety precautions and illness prevention measures. Your pediatrician will discuss various topics, such as placing your baby to sleep on their back, utilizing rear-facing infant car seats until around age two, maintaining home water thermostats below 120 degrees Fahrenheit, ensuring dangerous objects and poisonous substances are out of sight and reach, emphasizing dental health and promoting the use of bike helmets, among other things. Preparing for Your Visit It is recommended that, as a parent, you write down any questions beforehand, so you don’t forget them in the moment. Most importantly, feel comfortable asking your pediatrician about anything that might seem unusual, as you are the parent, and you know best! Before leaving the pediatrician’s office, be sure that you fully understand any instructions given to you and ask for clarification if needed. From your child’s birth through young adulthood, you will be visiting your pediatrician regularly. The American Academy of Pediatrics provides what a regular schedule might look like. Well-Child Checkup Schedule Two to three days after birth and at one month Two months Four months Six months Nine months One year 15 months 18 months 24 months 30 months Three years, and yearly after
-
10 Essential Questions to Ask at Your Child's Pediatrician Visit
Taking a few minutes to prepare for your child's pediatrician visit helps ensure that all your child's medical needs are met. Knowing the right questions to ask your provider can help you get the most out of your visit and ensure you and your child feel comfortable and informed. It is essential to base your questions on your child's specific health needs, but the ten options below are a great place to start. How is my child's overall health and development progressing? Is my child meeting their developmental milestones, and are there any areas where they may need extra support? What vaccinations does my child need, and are they up to date on all required immunizations? Are there any nutritional recommendations or concerns for my child's age and stage of development? What are some strategies for promoting healthy habits and physical activity for my child? Are there any warning signs I should look out for regarding my child's health or behavior? What can I do to help prevent common childhood illnesses like colds, flu strains or ear infections? What should I do if my child gets sick, and when should I seek medical attention? Are there any changes to my child's medication or dosage that I should be aware of? Is there anything else I should know or be aware of regarding my child's health or development?
Read More About 10 Essential Questions to Ask at Your Child's Pediatrician Visit
-
Senior Care Plus Loves Pickleball
Senior Care Plus is pleased to announce we are now a proud sponsor of Jam On It Pickleball, open to the community seven days a week at the Reno Sparks Convention Center. We’re excited to help promote this fun activity to our members, employees and the public. Pickleball has many wonderful health benefits – particularly for seniors. It’s a low-impact game that raises the heart rate, improves hand-eye coordination and increases mobility. In addition to the obvious physical benefits, pickleball is a great social activity. Getting out of the house and playing a fun, easy-to-learn game with others is a great way to make new friends while improving your physical and mental health! Ralph Barbato, a Senior Care Plus member from Reno, is a huge fan of pickleball and all it has to offer. “Pickleball has made such a positive impact on my life. I love the physical and mental health benefits along with the social aspect – it’s a great way to meet new people and I’m excited to have it in our community,” said Ralph.
-
Your Top 5 Questions about TAVR Answered
Your heart is the muscle in charge of pumping blood to your entire body. This vital organ is made up of chambers, valves and blood vessels. Your heart valves work similarly to a one-way door: they open and close, controlling blood flow in the correct direction through the heart chambers. For patients who have been diagnosed with a heart-related condition like aortic valve stenosis (narrowing), it is important to know treatment options. Most might think open-heart surgery is the only way to treat a heart valve, but many hospitals, including Renown, also offer a minimally invasive procedure called a Transcatheter Aortic Valve Replacement (TAVR). Dr. Abhilash Akinapelli of Renown Institute for Heart & Vascular Health shares his answers to the top five TAVR questions: 1. What causes aortic valve stenosis? Aortic valve stenosis can be caused by a variety of factors. The main reasons being wear and tear of the valve due to aging; genetically abnormal heart valve (bicuspid aortic valve); long-standing high blood pressure; and other reasons like radiation exposure. 2. Am I a candidate for TAVR? Renown’s heart care teams are made up of your primary care provider, cardiologist and cardio thoracic surgeon. They will evaluate if patients are a good candidate for the TAVR procedure by performing a variety of screenings and tests. Some of these include: Echocardiogram Electrocardiogram (ECG or EKG) Chest X-ray Exercise tests or stress tests Cardiac computerized tomography (CT) scan Cardiac catheterization 3. What are the advantages of the TAVR procedure? The Transcatheter Aortic Valve Replacement (TAVR) procedure is much less invasive than open heart surgery, otherwise known as a Surgical Aortic Valve Replacement (SAVR). Patients can typically return to their normal lifestyles within a week after leaving the hospital. During the TAVR procedure, a stent valve mounted on a balloon is advanced to the heart through the blood vessels in the groin without any incision. Once in position, the balloon will be inflated to firmly expand the new valve inside the diseased old valve, pushing it away to the sides. Once the new valve is in place, it begins working immediately and the deflated balloon is removed. The surgical procedure is approximately one hour long. Patients can get up and walk after four hours and will be discharged the following day if no complications arise. Compared to a SAVR, recovery time is much shorter and less risky for patients above the age of 75. A big advantage for anyone who fits under the criteria for a TAVR. 4. Is the procedure painful? The TAVR procedure is not surgery, but you will still be asleep during the procedure. Since no incision is made, it is essentially a painless procedure. Patients may experience slight discomfort such as aches and pains at the entry site of the catheter. 5. Can I have an MRI and X-rays done after having a TAVR valve? Yes, patients can have MRI scans and X-rays after TAVR. For further questions and information about the TAVR procedure, please consult with your Renown heart care team at 775-982-2452 or through MyChart.
-
Department Spotlight: Surgical Preadmission
Heading into surgery of any kind can bring along feelings of intimidation. With a best-in-class surgery team at Renown Health, patients rest assured that they are in the most capable hands for their entire procedure from start to finish – and while the physical preparation is vital, mental and emotional preparation is equally as important to ensure each patient has a smooth and comfortable experience. The Surgical Preadmission department (a.k.a. “preadmit”) at Renown Regional Medical Center and Renown South Meadows Medical Center is a dynamic and compassionate group of nurses, case managers, chart managers and more who are dedicated to guiding each patient through the surgical process. With extensive knowledge and expertise under their belt, the teams are equipped to make a genuine difference in the health and well-being of all patients, for all surgeries, at all times of the year. Surgery Starting Ground The Surgical Preadmission teams are crucial aspects in the successful outcome of every surgical procedure. Comprised of skilled healthcare professionals, this department is dedicated to providing comprehensive support and care before heading into the pre-operating room. “Our job is to prepare every patient for surgery, make sure all their pre-surgery testing is done, ensure they understand their fasting and medication instructions, have had their questions answered, have a ride home and know what to expect during surgery and after so their recovery can go smoothly and without complications,” said Debra Bennett, RN, Supervisor of Surgical Preadmission at Renown Regional. “Each patient is unique, so each experience is different.” Our preadmit nurses are the masters of communication, directing thorough assessments – including medications, tests and clearances – and addressing any questions or concerns patients may have, never missing the opportunity to inform them of exactly what they will expect in surgery. “I do a complete history on every patient while giving them detailed pre-operating instructions and helping them answer any questions to the best of my ability,” said Nancy Hilts, Surgical Preadmission RN at Renown Regional. “I am proud to be able to help allay their fears and concerns using my 30 years of pre-op experience. I offer an avenue for them to feel comfortable opening up to me.” “We always tell patients that they have great surgeons and a fantastic team that will be watching over them and taking care of them every step of the way,” added Jon Capallupo, Surgical Preadmission RN at Renown South Meadows. “We also give them plenty of educational handouts and video content, in addition to verbal instruction, to ensure they are as prepared as possible.” The nurses then pass the reigns onto the chart managers, who prepare the charts for surgery and ensure all documentation is up-to-date before sending them to the pre-operative team. The expert surgical case managers also step in to prepare a thorough discharge plan, along with reviewing pre-operation orders for status, consent, codes and more. The team does several of these initial visits virtually, and they are looking forward to soon phasing all preadmit case manager preliminary visits into a virtual model. From assisting the pre-op and post-anesthesia care unit (PACU) teams with discharge planning concerns to helping on the outpatient side with anything from oxygen equipment and catheters to transportation issues and those experiencing homelessness, our pre-admit case managers are always up to the challenge. "We are true patient advocates, alleviating concerns and fears along the way,” said Mary Carl, RN, Case Manager at Renown Regional. “Just to name a few things we do on a daily basis, we see our total joint and non-weight bearing patients during their preadmission appointment, so they are aware of the medical equipment they need and if it is covered by insurance; provide education for Aspira catheters and gastrostomy tubes; advocate to ensure tube feeding and dressing changes are set up for hospice and home health patients; and escalate concerns of patient safety to ensure a safe discharge.” In the midst of it all, there is never a dull moment in the preadmit teams. At Renown Regional alone, the preadmit professionals see more than 1,600 patients a month – and each one has a hyper-personalized experience with their very own preadmit team. “Many times, we are the first impression a patient has on our organization; after all, we touch more than 97 percent of patients that are scheduled for surgery, cardiac catheterization lab procedures or interventional radiology,” said Amy Schler, Surgical Preadmission RN at Renown Regional. “We also collaborate with many other departments in the hospital as well, from surgeons and anesthesiologists to case managers and nurse navigators. Our work in preadmit impacts the entire surgical process.” Holding a diverse array of experiences, our preadmit department plays an integral role in our commitment to providing the highest quality of care to every patient. Knowledge is Power Heading into surgery feeling fearful and worried is normal for any patient. However, how would you feel knowing that each individual member on your preadmit team has, on average, 23-25 years of experience in the field? This is the reality for our Surgical Preadmission department – and they put that vast knowledge to great use to bring a sense of calm to patients. “Our team members have worked in various departments within our organization, and they bring a wealth of knowledge that we share with each other, and most importantly, with our patients,” said Amy Schler, RN. “If you have hundreds of years of nursing experience, you can speak not only as a nurse but also as a patient. It allows you to give a more personal perspective on what patients can expect in their recovery. Being able to assess their emotions and provide feedback to our pre-op and PACU teams help the patient have a better experience.” “Many of our nurses have close to 40 years of experience each, and they have an extremely large knowledge base since we see patients from newborn to geriatric and from easy procedures to complex surgeries,” added Debra Bennett, RN. “Another great aspect of our team is the varied nursing backgrounds we all hold – surgery, pre- and post-op, labor and delivery, pediatric intensive care, cardiology, gastroenterology, urology, cardiac cath lab, home health and everything in between. Communication between departments is so important!” All members in this department, regardless of which clinical area they came from, surgical or non-surgical, can easily translate their skills into the work they do in preadmit – and they only continue to grow. “As a surgical preadmission nurse, I have used my years of experience as a nurse in surgical services,” said Terri Delatorre, Surgical Preadmission RN at Renown Regional. “I started as a floor nurse with orthopedics for 12 years, and then I worked with the PACU for 11 years. This has helped me give great understanding and care to our surgical patients.” “Because we have staff with such a vast knowledge base, we can rely on our years of working within our organization to help alleviate fears that the patient may have,” added Amy Schler, RN. We can prepare them for what to expect in pre-op and PACU and educate them on what to expect post-op, including any barriers they may face. For example, mastectomy patients may not realize they will not be able to raise their arms for 7-10 days post-op, and total knee patients have to navigate stairs and housing access. Helping patients think about barriers at home that they may not have thought about helps them prepare prior to surgery, enhances their healing and provides a better surgical experience.” The preadmit team works closely with our best-in-class surgeons and anesthesiologists, continuing to grow their expertise along the way while learning alongside our talented providers. For instance, when it comes to our Renown South Meadows preadmit department, anesthesiologist Nariman Rahimzadeh, MD provides excellent guidance for the entire team on state-of-the-art anesthesiology practices. “I am very proud of the work we do with Dr. Rahimzadeh,” said Lisa Closson, Surgical Preadmission RN at Renown South Meadows. “Together, we ensure patients are safe for both surgery and anesthesia.” Despite the challenges that come their way – whether it be changes to process and workflow to navigating support for patients after they leave the surgery floor – the preadmit team cleverly uses their collective wealth of knowledge to bring hope and comfort to all patients. “Our nurses are such warm, caring and compassionate humans that do their best to ease any fears and anxieties patients may have,” said Debra Bennett, RN. The Pride of Preadmission The pride of our preadmit team lies in their ability to make a positive impact on all patients they serve. To them, their work is not just a job – it's a calling. And they do it all while working together to elevate their team and performance. “Our team is most proud of the quality of care we provide to our patients and our abilities to troubleshoot difficult situations to ensure they have a great surgical experience here at Renown,” said Mary Carl, RN. The entire department supports each other by working collaboratively and relying on each other’s expertise to provide the best possible care for patients. They understand that their success as a team depends on their abilities to support and help each other. “Our team is awesome here at South Meadows,” said Jon Capallupo, RN. “We can turn to each other for support, and we all work very well with each other. I am glad to be a part of this team.” “I am proud of how well all of us in preadmit works with each other every day,” added Lisa Closson, RN. “We try to make patients feel comfortable from the moment they arrive to the time they leave the department.” The pride that our preadmit team expends goes beyond their departmental limits – these team members are also trusted teachers. They work closely with cancer nurse navigators to teach weekly classes for patients who have been newly diagnosed with breast cancer, coupled with lymphedema prevention and education classes. The team also encourages participation in Renown’s free smoking cessation programs to help their patients learn the risks and benefits of quitting smoking. When not serving patients or teaching classes, you can find many of these team members taking charge of multidisciplinary committees within our health system, including breast leadership, gastroenterology leadership, shared governance, infection control and recruitment and retention. On top of it all, this team certainly knows how to celebrate, with several of their members being a part of their own department-wide Celebration Committee, where they gather for retirement parties, baby showers and team get-togethers. Always active and never passing up a challenge, our preadmit department are shining examples of Renown’s Culture Commitments, especially Caring and Collaboration, and the pride in the vital work they do every day is limitless. “I am so happy my position in preadmit opened up for me at a time when I was really feeling challenged in my career,” said Nancy Hilts, RN. “The team that we have here is amazing. I am so grateful and thankful every day for the opportunity. It is an amazing place to work!”
-
Building a Better Birth Team
Giving birth expends as much energy as running a marathon. And just like you would only run a marathon with training beforehand, there are exercises you can do to prepare for birth. But instead of a coach, you'll have your birth team. Your birth team exists to help you navigate pregnancy and labor and support your choices. Let's say you've never put together a birth team before and are wondering where to start. Today we'll go over the three main positions to fill for your birth team's starting lineup. Birthing Person The birthing person is the leader of the team. After all, you can't have a birth team without someone giving birth. This person could be the baby's mother, gestational surrogate, birth parent before adoption, a transgender father or a non-binary parent. If you are not the birthing person, don't presume to know what the ideal labor and birth circumstances should be. And if you are the birthing person, don't allow anyone else to tell you what you want. This is your body and your birth; you are the boss in the birth room. Doula No birth team is complete without a doula, and although doulas have increased in popularity lately, many people still don't know what a doula is. Simply put, a doula is a birth professional – not a medical provider – who offers emotional, physical and informational support during pregnancy, labor and beyond. Most doulas' services include at least one prenatal visit and one postpartum visit, as well as continuous care throughout active labor. Some doulas provide more than one prenatal/postpartum visit, so be sure to ask what is included in their fee. Even if you have a partner who will support you during labor, studies have shown that a doula can significantly increase your likelihood of a positive birth outcome. Even the most supportive partner needs to rest, and a doula can ensure that you still get the care you need while your partner gets a break. Midwife or Obstetrician Finally, you'll want to choose the medical professional who will attend your birth. Many folks choose to give birth with the OB/GYN who does their annual check-ups, but there are many reasons someone might choose a different provider for their birth. The first step to finding the best attending provider for your birth is to decide which model of care aligns closest to your values and goals: the Midwifery Model of Care or the Medical Model of Care. .tg {border-collapse:collapse;border-spacing:0;} .tg td{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; overflow:hidden;padding:10px 5px;word-break:normal;} .tg th{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; font-weight:normal;overflow:hidden;padding:10px 5px;word-break:normal;} .tg .tg-gqvw{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-weight:bold; text-align:left;vertical-align:top} .tg .tg-8vim{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-size:18px; font-weight:bold;text-align:left;vertical-align:top} .tg .tg-qm8j{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;text-align:left; vertical-align:top} .tg {border-collapse:collapse;border-spacing:0;} .tg td{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; overflow:hidden;padding:10px 5px;word-break:normal;} .tg th{border-color:black;border-style:solid;border-width:1px;font-family:Arial, sans-serif;font-size:14px; font-weight:normal;overflow:hidden;padding:10px 5px;word-break:normal;} .tg .tg-gqvw{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-weight:bold; text-align:left;vertical-align:top} .tg .tg-8vim{background-color:#ffffff;color:#56266d;font-family:Arial, Helvetica, sans-serif !important;font-size:18px; font-weight:bold;text-align:left;vertical-align:top} .tg .tg-2rvk{background-color:#ffffff;color:#000000;font-family:Arial, Helvetica, sans-serif !important;text-align:left; vertical-align:top} Midwifery Model of Care Medical Model of Care Philosophy Birth is physiological. Birth is potentially pathological. Interventions Medical interventions can cause more complications, and therefore are only used as needed. Medical interventions should be used, even in non-emergency situations and sometimes as preventative measures. Decisions Birthing person is the key decision maker. Medical professional is the key decision maker. Provider’s Role Providers monitor labor and will intervene or transfer to hospital if needed. Providers assess and control the birthing process.