Search
-
Department Spotlight: Medical Oncology
The month of September recognizes several cancer-related health observances. Join us in celebrating our Medical Oncology team at Renown! No person ever wants to hear the words, “You have cancer.” Those three short yet impactful words immediately change the course of someone’s life. As these patients Fight the Good Fight against cancer, there are a lot of intimidating unknowns that can take over their minds. What happens next? What will my treatment be like? What is my prognosis? How will I be able to handle this physically and emotionally? What will it take for me to beat this? Who is better to be by their side than the devoted team members at the William N. Pennington Cancer Institute at Renown Health? From helping patients manage the process of complex paperwork and referrals to delivering personalized oncology and hematology treatment options tailored to each individual diagnosis, those fighting virtually any type of cancer are never alone, thanks to this team. The William N. Pennington Cancer Institute always lives up to that promise, guiding patients through the daunting journey of cancer treatment ahead, one step at a time. Courageous Against Cancer Our exceptional Medical Oncology department inherently understands that each moment in life is precious, especially for patients battling cancer. This team is dedicated to orchestrating the most comprehensive plan for each patient, seamlessly weaving together diagnoses and treatments, oral chemotherapy, medication management, clinical trials, radiation oncology and more. With the many patients they impact, there’s no question that there is never a dull moment in the day of the life of a healing hero like those in this department. “No day is the same in Medical Oncology,” said Hollyann Dehm, Registered Nurse. “As a nurse, we wear many hats in the clinic. Our role is to educate patients on their treatment plans and specific drugs they are receiving, triage symptom calls from patients, refill medications and implement our oral chemotherapy program. We help provide direct patient care by accessing ports, drawing labs and giving IV hydration when needed. We also help fill out family and medical leave (FMLA)/disability paperwork, help with physician orders, help obtain prior authorizations for prescribed medications and treatments.” “We do our best to let our patients know that they will not be going through this alone,” added Danielle Say, Physician Scheduling Coordinator. "We will be here for them every step of the way, guiding them and making sure their treatment is as smooth as possible and making ourselves available to them as much as we can. We end up getting to know many of our patients on a very close, personal level, and this helps to build that trust.” “Our day-to-day activities include seeing patients and helping to manage their therapies as well as their toxicities,” added Dr. Harry Menon, DO, Oncology Physician. “We work closely with our infusion room staff and have a robust team to help us deal with these complex patients. We also work very closely with our surgical and radiation oncology colleagues in a multidisciplinary fashion to provide comprehensive care for our patients.” The Medical Oncology team excels not only in providing cutting-edge cancer care but also in their compassionate approach to helping patients reduce the anxieties they understandably feel. Recognizing that a cancer diagnosis can be an emotionally overwhelming experience, this dedicated team combines medical expertise with unwavering support to create a healing environment. “When patients are referred to our department, a lot of them have many fears and questions,” said Heather Cortez, Medical Assistant. “A majority of what our team does is focused on the mental support that our patients require to help them have the most successful outcomes. One thing I have learned about cancer care is that positivity in the face of adversity is everything. Just being there to listen to our patient’s concerns can make all the difference. Helping them to navigate their many appointments and taking the time to explain things in a patient and compassionate way, is part of how our team serves this vulnerable population.” “The uncertainty is one of my patients' biggest fears: How far has my cancer progressed? How long will I have left? Is treatment even an option?” added Mary Wilson, Senior Medical Assistant. “The best advice that I can give my patients is that they are not alone. While this battle is going to be one of the hardest parts of their lives, they are surrounded by constant support to try and help with any burdens they may be facing. I also tell my patients that we have to take the little wins no matter how small they may be, because while cancer treatment is a physical battle, it is also a large mental battle." “While we don’t have answers to all the questions patients and their family members may have, we do our best to listen to their questions and concerns regarding their cancer diagnosis and treatment and guide them through their cancer journey," added Hollyann Dehm. “We provide emotional support and education on their type of cancer, managing their pain and side effects of their treatment. We also connect them to nurse navigators and our social worker who also help identify barriers to care and provide the patient with resources.” Whether it's explaining treatment options in understandable terms or offering emotional support through difficult moments, this department is committed to empowering patients on their journey toward healing. Their holistic approach not only treats the disease but also nurtures the spirit, all while being a strong advocate on each patient’s behalf. “Getting a cancer diagnosis can be the worst news that a person can hear; what we try to do is focus on improving quality life and focus on goals that help to promote quality of life,” said Dr. Harry Menon. “If the option for a cure is on the table, we try and focus on that goal in concert with promoting quality life. I try and have our patients focus on what they can control, with the understanding that even if some things are out of our control, the way we approach and manage those things, including our mindset, is still within our control.” “In our clinic, we truly value our patients and how they are cared for,” added Mary Wilson. “The amount of compassion our team shows is incredible. Patients constantly commend our team on how much they feel like the provider's care. Our providers and staff are not afraid to advocate for patients and that truly is an accomplishment in and of itself.” “We know patients are only hearing a small amount of the immense volume of information we provide them, so we encourage them to ask questions until it makes sense because the timeframe is different for every patient,” said Lillian Morton, APRN of Medical Oncology. “Cancer is an anxiety inducing lack of control whirlwind – if we can help by being responsive to patient calls and messages, we do so.” With their harmonious and integrated approach, each patient’s treatment journey progresses uninterrupted, bringing them closer to a brighter and healthier future.
-
Department Spotlight: Respiratory Care
This Department Spotlight is dedicated to Jason Simpson, Manager of Respiratory Services at Renown Children’s Hospital. Take a moment to breathe deeply. Inhale in, exhale out. We rely on our lungs to provide us with the air we need to live a healthy life – and this essential bodily function is something that many of us don’t think twice about since it comes easily for us. Now, imagine yourself as someone who is living with severe asthma, chronic obstructive pulmonary disease (COPD) or someone who was recently diagnosed with a frightening respiratory condition like COVID-19 or pneumonia. The simple act of breathing can prove to be an intimidating venture requiring the care of a professional. Who are the people that take on the challenge? Meet Renown Health’s Respiratory Care Services department. Serving patients across 13 service lines, three acute facilities, outpatient locations and telehealth, our respiratory specialists – including respiratory therapists, respiratory care aides, inpatient COPD respiratory therapy navigators and educators and more – use their expertise to help restore the vitality of all their patients with every inhale and exhale, shaping a healthier livelihood one lung at a time. The Guardians of Respiratory Wellness Whether they are managing lifelong respiratory conditions or offering crucial support in emergencies, the Respiratory Care team strives to enhance the quality of life for every patient. As an indispensable member of the clinical team at Renown, our respiratory therapists work collaboratively with doctors and nurses to tackle a wide range of tasks, tailoring care for each patient’s unique needs. “Respiratory care is involved with all stages of life, from beginning to end,” said Sarah Kurtz, Respiratory Therapist. “We work closely with nurses and doctors and perform arterial punctures, breathing treatments, weaning maneuvers for patients on life support, intubations and much more. We assess patients constantly to see if their care needs to be upgraded or if they can be weaned to get them back home with their families.” “You start your morning researching your assigned patients,” added Tim Start, Respiratory Specialist. “We go over lab values and chest radiographs and decide the best plan of care for each patient. Our objective is to improve their respiratory status by giving them medications and doing breathing exercises. We participate in other forms of care with nurses, such as activities of daily living (ADLs) and mobilization. We work as a team, and that enables us to provide great patient care.” For patients living with COPD, enjoying all that life has to offer comes with a separate set of obstacles. According to the Centers for Disease Control and Prevention (CDC), over 200,000 people across the Silver State are living with this chronic condition. Luckily for them, Renown has a specialized team to help these patients optimize their life and manage their condition with individualized treatment and education. “We run a report every morning to identify all the patients currently admitted who have a history of COPD, take respiratory medications or smoke,” said Amber Beck, Inpatient COPD RT Navigator. “After looking through their charts, we visit with the patient (and possibly their family) at the bedside to help them better understand how to manage their breathing issues.” As a vital part of the Respiratory Care team, Renown’s respiratory care aides help ensure the seamless operation of our respiratory care services. These dedicated professionals provide essential support to respiratory therapists not only during intricate procedures but also outside of face-to-face patient care by transporting equipment, restocking supplies, assisting in the mobilization of patients and more. “We are responsible for the maintenance of unit supplies and making decisions regarding levels of stock to be maintained,” said Dia Ramos, Respiratory Care Aide. “We also transport equipment, refill the oxygen tanks on the floors and intensive care units (ICUs), order and stock respiratory care supplies, mobilize patients and assist the respiratory therapists during bronchoscopies in the ICUs. In addition, we clean respiratory equipment like mechanical ventilators, continuous positive airway pressure (CPAP) and bilateral positive airway pressure (BiPAP) machines, high flows and aerosol poles.” Once the COVID-19 pandemic hit, a special spotlight shined upon respiratory care teams across the country for the heroic care they provided patients in respiratory distress. While their roles in health systems have gained a better understanding nationwide, this team understands it is vital for them to educate the community about the important jobs they hold for our patients. “Respiratory care can be under the radar,” said Pam Umek, Respiratory Specialist. “Once, when I told someone that I am a Respiratory Therapist, they said, ‘Oh, like a yoga breathing instructor?’ I then explained all the things we do: intubation, extubation, bronchoscopies, transports, traumas, codes, rapid responses, pediatrics/NICU, breathing medications/therapies, open heart rapid ventilator weaning … needless to say, that individual walked away with a better understanding of not just Respiratory Care Services but also the enormous effort it takes to care for our community.” The accolades and achievements continue to pour in, from national awards and certifications to implementing different jobs in care units to optimize the patient care experience. “We have earned and continue to maintain the Joint Commission Disease-Specific Certification for COPD,” said Amber Beck. “We are well below national averages for 30-day readmissions, lengths of stay and mortality due to COPD. Sandy, one of our COPD Coordinators, was a recipient of a patient advocacy award from the American Association of Respiratory Care and FACES Foundation.” “We have started implementing Respiratory Care Aides in the critical units, starting with the Cardiac ICU,” added Dia Ramos. “We work as one team and are always helping each other with their tasks.” Education and mentorship are at the core of Renown’s mission to make a genuine difference in the health and well-being of every patient. Nurturing the next generation of medical professionals – including respiratory care professionals – is a task that the Respiratory Care team takes seriously. “It has been great being able to help educate students in different disciplines,” added Pam Umek. “We have been able to offer shadow shifts to students in emergency medical services (EMS), nursing and medical school. These opportunities help students entering the medical field have a better understanding of the many ways we can help care for our respiratory patients.” From the moment of birth to the final stages of life, Renown is fortunate to have a Respiratory Care team that tirelessly ensures every breath counts, safeguarding their role as a trusted partner within our health system. A Tribute to Jason Simpson, Healthcare Hero
-
Living with COPD? How to Maximize Your Summer Experience
June offers an official welcome to summer and the height of outdoor activities in northern Nevada such as hiking, camping, days spent at the lake and embracing long days and warm evenings with friends and family. Enjoying all that the summer season has to offer may not be as easy for those living with chronic obstructive pulmonary disease, or COPD, which effects more than 15 million Americans. What is COPD? COPD is a group of lung diseases including emphysema and chronic bronchitis that result in airflow blockages from the lungs. People may experience frequent coughing and shortness of breath among other symptoms. COPD typically impacts adults ages 65 and older and is becoming increasingly more common among women. Although smoking plays a key role in the development of COPD, air pollution and indoor air quality, and respiratory infection also contribute to disease development. While there is no cure for COPD, limiting progression of disease and managing symptoms can be achieved through lifestyle changes, therapy, and medications. Tips for Living with COPD This Summer, and Always Stay Hydrated: Staying hydrated is extremely important for people with COPD, especially during the summer. Not drinking enough water can make breathing more difficult because it increases respiratory symptoms. Make sure to always keep a water bottle with you and aim to drink 8-10 glasses of water daily. Be Mindful of Temperature: COPD symptoms can be exacerbated by hot weather. It is best to participate in outdoor activities during the cooler times of day, like the morning or evening. Check Air Quality Before You Go: Before engaging in outdoor activities, be sure to check the air quality index and plan your activities accordingly. Pace Yourself: Exercising can be difficult for people who have COPD. To make the most of your summer, try not to push yourself too hard and take breaks when you need them. If you start to feel out of breath or tired, take a break in a cool, shaded area until you feel better. Take Matters Into Your Own Hands To address the needs of community members living with COPD, the Renown Health Research Office has teamed up with Pulmonary Medicine to provide patients who are former or current smokers and have a history of frequent exacerbations with an option to participate in the ARNASA study. "COPD exacerbations have a huge negative impact on patient’s lung function” states Dr. Farah Madhani-Lovely, Chief of Pulmonary Medicine at Renown Health and Assistant Dean of Clinical Research at the University of Nevada, Reno School of Medicine. “We have had inhalers and prednisone for decades but patients are still having exacerbations. Now we have a new pathway we think will prevent exacerbations which is what this clinical trial is designed to prove.” This study will evaluate the efficacy and safety of astegolimab compared with placebo in participants 40-80 years of age with COPD. “This study in particular is so exciting because of the enthusiasm from the sponsor’s end” says Katie Buckley, Lead Clinical Research Coordinator working on pulmonology studies at Renown’s Clinical Research Office. “Often times sites aren’t assigned particularly passionate or engaged personnel who aid in carrying out these studies, but you can tell Roche Genentech’s team truly cares about the success of the study, the safety of their participants, and proving the efficacy of the investigational agent. Working on a study like this takes a village, and when the individuals on all ends share similar mindsets and work towards success as a collective unit instead of as individual moving parts, it’s amazing to see everything we’re able to accomplish.” Renown’s team of expert pulmonologists and researchers are available to join patients with COPD in support of their healthcare journey. If you are interested in learning more about this clinical trial option at Renown Health, talk to your pulmonologist at your next appointment or contact us at 775-982-3646. At Renown Health, our goal is to make it easy for patients to access clinical research as a care opportunity where patients can access a variety of standard care treatment options for their health condition or choose to participate in a clinical trial. For more information about clinical trial opportunities available to you or to ask any questions, contact the Renown Research Office at Renown-CRD@renown.org or 775-982-3646.
Read More About Living with COPD? How to Maximize Your Summer Experience
-
Your Ultimate Cold and Flu Survival Guide
While viruses can attack year-round, colds, flus and other respiratory illnesses are typically more prevalent during fall and winter. People spend more time indoors, which allows viruses to pass more easily from one person to another. The cold, dry air can also affect the respiratory system, making it more susceptible to germs. According to the CDC, flu activity in the U.S. often begins to increase in October and peaks between December and February. “Flu season” can last as late as May. When it comes to the cold and flu, prevention and preparation are key. Getting the flu shot and a COVID-19 vaccine is the first and most crucial step in protecting against these two respiratory illnesses. Preventative actions, such as washing your hands, covering your mouth and nose when coughing or sneezing and getting enough sleep can also help you avoid getting sick. However, despite your best prevention efforts, the time may come this winter when you start to feel a little scratch in your throat or a fever coming on. By taking steps ahead of time to assemble a cold and flu survival kit, you’ll be more prepared for whenever illness strikes, allowing you to stay home, rest and avoid spreading germs. Tips for Managing Symptoms Keep these tips in mind to ease your cold or flu symptoms: Stay home and rest Drink plenty of fluids Treat aches and fever with over-the-counter medication such as ibuprofen or acetaminophen Manage a cough with over-the-counter expectorants or suppressants Run a humidifier or sit in a steamy bathroom to ease congestion What to Stock in Your Flu Survival Kit Be ready when a cold or the flu strikes by having a flu survival kit filled with these get-well essentials stocked in your pantry, fridge and medicine cabinet: Over-the-Counter Medications: Take advantage of over-the-counter medications to make yourself feel better and ease most common flu symptoms of fever, headache, cough, muscle aches, sore throat, and runny or stuffy nose Pain relievers - Ibuprofen (Motrin and Advil) or Acetaminophen (Tylenol): for fever and aches Decongestants: for sniffles and congestion Cough expectorant (guaifenesin): for a “wet” cough to help clear secretions from the lungs Cough suppressant (dextromethorphan/DM): for a severe “dry” cough to block the cough reflex Cough syrups and drops Drinks: Water Herbal tea Low-sugar sports drinks Pedialyte Foods: Chicken soup Broth Vitamin C-containing fruits and vegetables Oatmeal Toast (add some avocado, honey or egg) Miscellaneous items: Tissues Lozenges Protective mask Thermometer Humidifier When to Seek Care and Where to Go Most healthy adults who have a cold, the flu, or other mild respiratory illnesses don’t need to see a care provider and will recover at home with self-care measures. Because these are viral illnesses, antibiotics won’t work against treating them. Your care provider may be able to prescribe an antiviral medication that can relieve your symptoms and shorten the duration and severity of your illness; however, this needs to be started within 48 hours of symptom onset and is often only prescribed to individuals at high risk for developing complications from the flu or those experience severe symptoms. Primary Care or Urgent Care Contact your primary care provider or visit an Urgent Care if you are at an increased risk, including those who: Are 65 years of age or older Have chronic medical conditions Are pregnant or recently gave birth Have a weakened immune system Find a primary care provider If you are otherwise healthy and not at increased risk of complications, seek medical advice if your flu symptoms are unusually severe, such as mild difficulty breathing, a severe sore throat, coughing that produces a lot of green or yellow mucus, or feeling faint. Emergency Care Go to the Emergency Department if you are experiencing emergency warning signs such as severe pain (chest, abdomen), concern for heart attack or stroke (slurred speech, new localized weakness), severe dehydration (needing IV fluids) or severe shortness of breath.
-
Two Years We Won't Forget: COVID-19 at Renown Health
On March 19, 2020, Renown Regional admitted the first patient in need of care while sick with COVID-19. Our providers navigated two years of a pandemic and overcame many challenges while providing the best care for our patients and the community. Anicia Beckwith’s series “The Art of Healing” captured Renown Health during this time. Let's take a look back on the last two years. February 2020: Standing Up the Hospital Incident Command System (HICS) On February 25, 2020, leaders at Renown Health stood up Renown’s Hospital Incident Command System (HICS), a standardized system used to organize response personnel and resources and manage response operations during emergencies and crises. March 2020: Temporary Deployable Medical Structure Placed Outside Renown Regional Emergency Department On March 12, 2020, Renown set up a deployable medical facility to serve as a respiratory illness screening center for emergency room patients at Renown Regional. A similar tent was also set up outside the emergency room at South Meadows Medical Center. This proactive measure helped our teams care for community members with respiratory illness symptoms while protecting patients and staff in the emergency department and other areas of the hospital. Check out photos of the tent here. Read the Reno Gazette Journal Article about the tent here. April 2020: Alternate Care Site at Mill Street Parking Structure at Renown Regional Renown’s HICS team decided to create an Alternate Care Site (ACS) in the Renown Regional Medical Center Mill Street parking structure. The ACS served additional hospitalized patients and allowed caregivers to remain on campus and still have access to existing hospital infrastructure such as lab, pharmacy, imaging, food services and other critical services. After just 10 days of construction, the ACS was completed on April 3, 2020 with space to hold up to 1,400 patients. Check out photos of the ACS under construction here. On Nov. 12, 2020, Renown opened the ACS to serve additional hospitalized patients diagnosed with COVID-19 who were clinically stable or improving. Healthcare workers at Renown cared for hundreds of patients at this site. In early Jan. 2021, the remaining patients returned home. Check out the video of Connie, a patient who received care in the ACS. April and July 2020: The LOVE Sculpture Placed at Renown Regional On April 16, 2020, during a time of darkness and uncertainty, Artown loaned Renown the LOVE sculpture, a one-ton aluminum piece of art created by artist Laura Kimpton and fabricated by Jeff Schomberg. The structure, which originally debuted at Burning Man, was lit up Renown Regional's main entrance on Mill St. Watch a video about the LOVE sculpture’s debut at Renown Regional. On July 13, 2020, thanks to the support of former board chair and community supporter Blake Smith and the Keyser Foundation, the LOVE sculpture is now a permanent fixture at Renown Health. Throughout the pandemic, it has served as a source of inspiration, hope and positivity for our community and care providers. Check out a video of the LOVE is Here to Stay celebration. June 2020: Renown Offers In-House COVID Testing In June 2020, the Renown laboratory team sprang into action to help meet the growing demand for COVID-19 testing amongst Washoe County residents and businesses. Renown invested in expanded staffing and in-house testing capabilities that ensured our teams could swab and process up to 1,000 COVID-19 tests for patients each day. All with results returning within hours. November 2020: Renown Introduces “Hospital At Home” Remote Monitoring In November 2020, six patients at Renown Regional Medical Center and Renown South Meadows Medical Center diagnosed with COVID-19 were outfitted with a remote Hospital at Home monitoring system. Renown clinicians plan to continue using this system to monitor upwards of 1,000 hospitalized patients and lower acuity patients from their homes. December 2020: Renown Administers COVID-19 Vaccines to Health Care Employees On Dec. 17, 2020, Renown began to vaccinate its healthcare workers. Among those receiving the first vaccines was Luis Martinez, a technician on Renown’s Clinical Decision Unit who cared for patients recovering from COVID-19 in the Alternate Care Site field hospital. Read the Reno Gazette Journal article about the COVID-19 vaccine rollout at Renown. January 2021: Renown Administers COVID-19 Vaccines to Community After several weeks of successful employee and volunteer drive-thru vaccination events, Renown supported the Washoe County Health District and the state in vaccinating Washoe County community members. Click here for a playlist of videos featuring Renown Health employees and patients talking about the importance of the COVID-19 vaccine. February 2021: Local Widow Inspires Renown to Change Visitor Supporter Policy Darlene Randolph’s husband Dave spent 17 days hospitalized at Renown Regional Medical Center before losing his battle with COVID-19 on December 13, 2020. Darlene wrote a passionate letter to Renown Health asking for the visitor policy that allowed patients with COVID-19 to receive visitors. In February 2021, Renown hospitals were among the first in the country to lift visitor restrictions for patients with COVID-19 to encourage families to be at the patient's bedside. Read Darlene’s full story here. May 2021: Renown Celebrates Volunteers, Partners and Community Who Aided in Vaccine Efforts In May 2021, Renown administered the last dose of COVID-19 vaccines to community members in Renown’s drive-thru clinic. Between January and May 2021, over 80,000 doses were administered at the drive-thru. View drone footage of this effort here. Click here to see pictures of vaccine volunteers and employees. November 2021: Renown Offers Vaccine for Children Ages 5+ In November 2021, Renown vaccinated children in the Reno-Sparks community with the 2-dose series in a limited round of weekend clinics. The vaccine clinics featured therapy dogs, local mascots and donuts donated by Doughboy’s Donuts. Click here to see pictures of the children’s vaccine clinics and watch a video about the clinics here.
Read More About Two Years We Won't Forget: COVID-19 at Renown Health
-
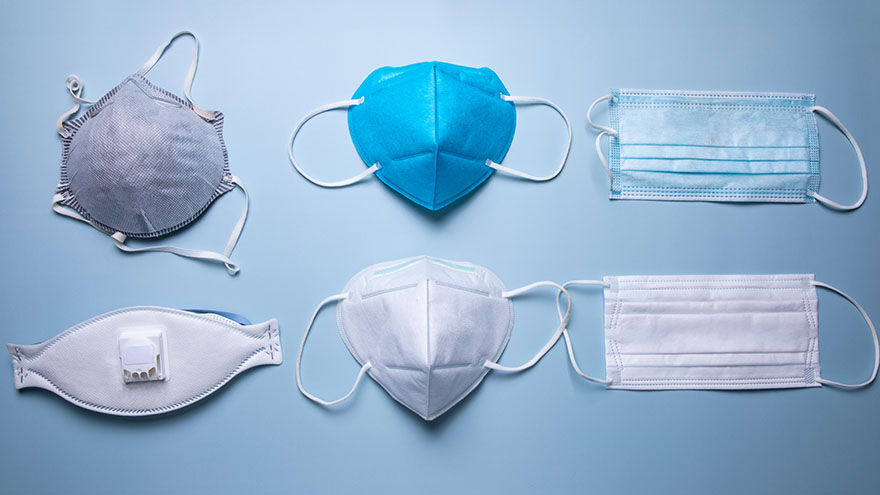
Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide
To better protect our patients, visitors and employees, cloth masks are no longer allowed at Renown facilities. Surgical masks, KN95 and N95 masks are allowed at Renown facilities. Appropriate face masks will be provided for visitors and patients who need one. With recent surges in the infectious COVID-19 omicron variant, many have sought to upgrade their face masks. But, let’s face it, shopping for face masks with adequate protection can be a challenge, especially considering the countless variations and the rise of counterfeit masks. Follow our straightforward guide below which includes some common red flags to help you discern between a high-quality face mask that provides proper protection and those that may be counterfeit. Types of Masks Qualities of a Real N95 Respirator Mask According to the National Institute for Occupational Safety and Health (NIOSH), N95 approved masks form a tight seal around your face and include a disposable respirator that removes particles including bacteria, viruses and dust as you breathe. N95 masks that are NIOSH approved undergo strict quality assurance and performance requirements to ensure mask respirators filter out up to 95% of hazardous particles. As a rule of thumb, N95 masks will not have ear loops, commonly used in cloth or surgical face masks. N95 respirators will contain two elastic bands or head straps that fasten behind the head, one securing the crown of the head and the other resting at the base of the neck, providing a snug fit and seal. Some other common signs that an N95 might be counterfeit include lack of all proper labeling, misspellings of NIOSH, decorative fabric and claiming to be approved for children. Currently, masks in adult sizes are the only masks to undergo NIOSH’s quality assurance and testing process. Respirators approved by NIOSH will include a testing certification (TC) approval number and will contain specific labeling on the facepiece of your mask. Find a full list of Center for Disease Control (CDC) and NIOSH requirements here. Identifying Real KN95 Respirator Masks Often preferred due to comfortability, the KN95 respirators were initially designed to meet Chinese standards for medical masks. Firstly, if a KN95 mask claims to be approved by the CDC, it is counterfeit as the CDC and NIOSH do not support any respiratory protective devices according to international standards. However, when KN95 masks are fitted and worn appropriately they do provide more protection than disposable masks. Legitimate KN95 masks will display a manufacturer number, GB2626-2019, ensuring accordance with current Chinese respirator standards for all masks made after July 1, 2021. Unlike N95 masks, it is important to note that KN95 masks are available in children's sizes. You might run into KN95 masks claiming to be “FDA (Food and Drug Administration) approved” or “FDA-registered,” but be aware that this does not mean much and is a misleading statement. What this indicates is that a mask maker has submitted paperwork to the FDA, but the product has not been thoroughly tested for proper filtration and protection. Surgical Masks Medical procedure masks often referred to as surgical or disposable masks vary in their protection according to a variety of factors including fit and filtration. The CDC defines medical procedure masks as “variably shaped, including flat pleated, cone-shaped, or duck-bill. Medical procedure masks are loose and are not expected to provide a reliable level of protection against airborne or aerosolized particles as N95 respirators regulated by the National Institute of for Occupational Safety and Health.” However, these types of masks provide more protection than cloth masks and are certainly better than wearing no mask at all. Often popular due to their level of comfort and cost-effectiveness, surgical masks can be knotted in the ear loop areas to provide a tighter seal and can be layered for additional filtration. Depending upon your budget and level of comfortability and protection, one variation of mask may suit you over another. Please remember to do your part in limiting the spread of COVID-19 and wear a surgical mask, KN95 or N95 mask when visiting Renown facilities.
Read More About Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide
-
COVID-19 Booster Shots, What You Need to Know
Getting the COVID-19 booster is the best way to protect yourself from severe illness or death due to COVID-19, and both the CDC and the FDA have approved booster shots for people ages 18 and older. So, with the holidays right around the corner and infection rates on the rise both in Nevada and nationally, the best thing you can do to prevent the continued spread of this deadly virus is to get boosted today. The Basics: Who: It is recommended that everyone 18 years or older get a COVID-19 booster shot. When: At least 6 months after completing your primary COVID-19 vaccination series. What: Any of the COVID-19 vaccines authorized in the United States. The CDC allows for mix and match dosing for booster shots. How: To make an appointment for your COVID-19 vaccine booster, please visit vaccines.gov today. Appointment Reminders: Don’t forget to bring your CDC vaccination record card to your appointment. Refresh yourself on the potential side effects and remember that these are normal signs your body is building up protection. Commonly Asked Questions: Q: Does anything change if I received the Johnson & Johnson as my first COVID-19 vaccine? A: If you received the Johnson & Johnson COVID-19 vaccine, you are elidable for a booster two months after completing your primary vaccine. Q: Is the formula the same for the boosters as it was for the primary vaccine? A: COVID-19 booster shots are the same formulation as the current COVID-19 vaccines. However, in the case of the Moderna COVID-19 vaccine booster shot, it is half the dose of the vaccine people get for their primary series. Q: Am I still considered “fully vaccinated” if I don’t receive a COVID-19 booster shot. A: Yes, everyone is still considered fully vaccinated two weeks after their second dose in a two-shot series, such as the Pfizer-BioNTech or Moderna vaccines, or two weeks after a single-dose vaccine, such as the J&J/Janssen vaccine. All information courtesy of the Center for Disease Control and Prevention. All information courtesy of the Center for Disease Control and Prevention
Read More About COVID-19 Booster Shots, What You Need to Know
-
How to Ease Your Child's Fear of Vaccines
Getting a shot can be scary for kids and anxiety-inducing for parents and caregivers. With flu shot season well underway and children's COVID-19 vaccine clinics in full swing, we wanted to share ways to reduce the stress for you and your child. Plan Ahead and Be Honest A few days before the scheduled appointment, casually mention to your child that you’re both going to the doctor’s office (or vaccine clinic, or pharmacy) soon for their vaccine. Explain to them that this will help protect them and will only take a second. Being honest is important, telling your child that it will hurt for a moment. If possible, try and schedule the vaccine at a kid-specific vaccine clinic, your pediatrician's office or a school-based site. Remember that words are powerful. Take notice if you are using a word that might make them more upset, such as prick, jab, needle or shot. You can interchange words such as vaccine, immunization or injection. Bring Toys Don’t be afraid to let your child bring one of their favorite toys or stuffed animals to the appointment. This can make them feel more comfortable and provide distraction. Ask for Pain Reliever/Numbing Agent If you know from past experience (or suspect) that your child has a needle phobia, talk to the vaccination location ahead of time and ask if they can use a pain reliever or numbing agent before administering the vaccine. Distract. Distract. Distract. Sing a song, tell them a joke, make a funny face. If you can pull your child’s attention away from the needle and make them laugh, they won’t focus all their energy on worrying about the shot. Lead By Example If you haven't gotten your flu shot, COVID shot or COVID-19 booster yet, ask the facility ahead of time if you can also get a shot before your child. Show them that the shot is no big deal and that they will have no problem getting it themselves. Celebrate Don’t be afraid to celebrate this victory with your child once it is over – bring them to the park, go out for an ice cream cone, let them pick what’s for dinner. This reward will show that you’re proud of them for being brave and may also make the next time your child is due for a shot easier.
-
Reliable Care From Home
Renown Health has always been on the frontlines of technological advancement, and that innovation remained unwavering during the COVID-19 pandemic. Our telehealth teams heeded the call to provide home monitoring for our patients, transforming how we provide care. The care providers at Renown successfully monitored lower acuity COVID-19 patients from the comfort of their own homes. Bernard Lee was diagnosed with COVID-19 and pneumonia, and was able to return home to continue his recovery with a home monitoring system. While at home, Bernard’s health took a turn for the worse while he was sleeping, but thanks to the continuous monitoring of Health at Home, his worsening vitals did not go unnoticed. “This monitoring system really saved my life,” Bernard said. “It was telling me that my sats were low, but I didn’t even feel the common COVID symptoms; I just felt tired.” Because of his low oxygen saturation (sats) and the continuous monitoring, he woke up to providers calling to check on him in the early morning. He was immediately transferred to the Renown Intensive Care Unit to be cared for and monitored by our expert care teams. Today Bernard is recovering, feeling great and continuously refers to the team and the home monitoring system as his guardian angels.
-
How to Talk to Your Vaccine-Hesitant Friends About Getting Vaccinated Against COVID-19
Roughly 59% of eligible Nevadans are fully vaccinated against COVID-19 as of mid-September. That number is up 9% from only a month ago, but our work is far from done! One of the most powerful ways to convince someone to get vaccinated is for a person they trust and respect to take the time and have that complicated conversation with them. We know these conversations can be daunting, so we consulted Marie McCormack, MD, Primary Care Division Chief at Renown, about the six best ways to approach and frame these conversations to be productive and effective. 1. Be firm, but not aggressive. 2. Listen to what they have to say, and don’t assume you know why they haven't gotten the vaccine yet. 3. Cater your responses to their concerns. The CDC even has a helpful reference table identifying main reasons people are not getting vaccinated. If they are scared, offer to go with them. If they are not worried about getting sick, explain that they are more at risk of infecting those around them who are more likely to have a severe reaction to the virus. If they don’t know how to make an appointment, help them find the most convenient time and place for their schedule. If they are worried about how fast the vaccine was developed, remind them that the mRNA technology used in these vaccines has been studied for years. If they are worried the vaccine will affect fertility, tell them that in August the CDC officially recommended that pregnant people can get vaccinated. 4. When in doubt, hit them with the stats! 1 in 500 Americans has died from COVID-19. Vaccinated people are nearly five times less likely to get infected, according to the CDC. Vaccinated people are 10 times less likely to get so sick they ended up in the hospital, according to the CDC. 5. Remind them of all the things they might not be able to do if they aren't vaccinated. Attend concerts or sporting events Travel Potentially even keep their job 6. When all else fails, use the tough love approach. Tell these people you don’t feel comfortable meeting with them in person until they are vaccinated.
-
Breast Feeding Doesn't Have To Mean Sore Nipples
If you think sore nipples are just a normal part of breastfeeding, think again. Robin Hollen, APRN, and Breastfeeding Medicine Specialist, says that nursing can be an enjoyable experience for mom and baby without pain and discomfort. A top concern of nursing moms within the first week after delivery is how to prevent sore nipples. Even moms who’ve nursed before struggle with this common issue. While many women think it is a regular part of the nursing experience, it is actually a sign that something isn’t quite right. “Nursing your baby should be enjoyable,” says Robin Hollen, Breastfeeding Medicine Specialist with Renown Health. For over 30 years Robin has been supporting moms to breastfeed. Below she shares some valuable information and tips, helping you create a happy and healthy breastfeeding experience for you and your baby. What causes sore nipples? The most common cause of sore nipples involves incorrect latching. For a proper latch, a baby’s mouth takes in the entire nipple and some of the breast, so that the nipple rests at the back of the mouth where the palate is soft. With an improper latch, the mouth may slip down to the tip of the nipple while the baby nurses. This constant pressure on your sensitive skin may cause discomfort and pain. A board-certified lactation consultant can help assess if your baby is latched correctly and troubleshoot your breastfeeding concerns. Less common causes of sore nipples include: • Improper tongue placement of baby • Clenching • Incorrect breast pump use How can a mother prevent sore nipples from an improper latch? Breastfeeding is a learning experience for both mom and baby. Ask for help with the latch so your baby learns it correctly and maintains its depth. In the past, new mothers were surrounded by a community of women — their own mothers, grandmothers, or other family and friends — to provide assistance and guidance with every latch at the beginning of an infant’s life. In today’s culture, new moms can find themselves on their own with no extended family to lend their knowledge. Nurses, pediatricians and lactation consultants now fill that role; they are the eyes and hands along with the much-needed experience to guide new mothers. Our Breastfeeding Medicine experts assist nursing moms with latch every day. Even a single visit with a lactation consultant observing your breastfeeding baby can provide valuable insight on achieving, and maintaining, the proper latch - preventing future nipple soreness and discomfort. How to heal sore nipples from breastfeeding To heal sore nipples, you must first fix the cause, and correcting the latch prevents further damage. A lactation consultant can also help you address the pain. Below are some breast healing tips: • Your own expressed breast milk is excellent to rub into the nipple for anti-bacterial protection. • For those moms who need more lubricant or fat than breast milk offers, use a lanolin or a cream that is labeled safe for the baby. • Soothies are a gel pads providing comfort in between feedings, but should not be used with lanolin products. • Breast shells, not to be confused with shields, can guard the nipples from irritation or pressure in between feedings. If you have more questions about preventing and healing sore nipples or general breastfeeding concerns, talk to your pediatrician or a Renown Health Breastfeeding Medicine specialist at 775-982-6365.
Read More About Breast Feeding Doesn't Have To Mean Sore Nipples
-
4 Breastfeeding Tips for New Moms
While breastfeeding is natural, it's not always easy. We asked Certified Lactation Counselor Sarah Mitchell for some tips to help make the process easier for mom and baby. From increased infant immunity to improved maternal health and well-being, the benefits of breastfeeding are many. Still, only 60 percent of U.S. moms in the United States continue to breastfeed past their baby's first six months. There are for many reasons for why moms stop, including the mother's their need to return to work. We reached out spoke to Sarah Mitchell, a certified lactation counselor at The Lactation Connection at Renown, for some expert advice. Tip 1 At first, it's normal to expect obstacles. Even in cultures where close to 100 percent of moms breastfeed, they can experience issues, including getting the baby to "latch on," sore nipples, and milk production. In addition, it sometimes can take several weeks for mom and baby to get comfortable. Tip 2 Line up a coach, even before the baby is born. This can be a professional lactation coach, family member, or friend who is experienced and encouraging. While online videos can be helpful, most new moms need the one-on-one guidance that a coach can provide. Renown offers outstanding resources in its Lactation Connection center, including expert consultants, products, and support. Tip 3 Well ahead of the due date, set up a support network of friends, family members, or community groups such as La Leche League. Women historically have relied on extended support systems to help them with raising children, and breastfeeding is one of those areas that, while natural, still needs encouragement from the women who’ve been there. Tip 4 Don’t get discouraged if you need to supplement at times with formula. This, too, as it turns out, is not uncommon in other cultures. In other parts of the world, babies are given beverages and foods such as tea, broth, soup, juice, mashed bananas, and papaya. The American Academy of Pediatrics recommends supplementation only with approved formula -- but the point is, it’s ok to supplement if you need to. Finally, don’t forget the importance of breastfeeding for connecting with your baby. It’s essential to maintain breastfeeding over the weekends, preferably “on-demand,.” and will keep that special bond strong after you have returned to your job.