Search
-
Renown Neuro-Diagnostic Laboratory Nationally Recognized
Earning its third five-year accreditation, Renown's neuro-diagnostic lab remains Nevada's only accredited ABRET facility. The Renown Institute for Neurosciences is pleased to announce that the neuro-diagnostic lab at Renown Regional Medical Center has been re-accredited by the American Board of Registration of Electroencephalographic and Evoked Potential Technologists (ABRET). ABRET’s lab accreditation process evaluates technical standards, the quality of a laboratory’s output, and lab management. “Renown Health is a leader and a destination for health in treating neurological disorders and advancing innovations in neurology. The specialists at the Renown Institute for Neurosciences provide comprehensive brain, nerve and surgical support along with a full range of diagnostic and additional procedures and a disease-specific, patient-focused approach to care,” says Tony Slonim, MD, DrPH, FACHE, President and CEO, Renown Health. “This prestigious honor from ABRET means Renown’s Electroencephalogram (EEG) Laboratory has met strict standards and is recognized as a place where patients and physicians can confidently receive quality diagnostics.” “In addition to re-accreditation from ABRET, the Institute for Neurosciences has earned a Gold Seal of Approval by the Joint Commission and offers advanced treatment options including t-PA (Tissue Plasminogen Activator) and biplane angiography. The Level III accredited Epilepsy laboratory implements some of the newest treatments available,” said Renown’s Chief Medical Officer, Paul Sierzenski, MD, MSHQS, CPE, FACEP. “Renown patients also have access to the most promising new therapies through national clinical trials, which have been shown to significantly improve patients’ health and well-being.” “I am proud to recognize our dedicated team of caregivers for their continued passion and excellence in maintaining the highest standards in patient care,” said Renown Institute for Neurosciences’ Division Chief, Dr. Rolando Ania. “It is all thanks to their tremendous efforts that we remain the only ABRET accredited laboratory, as well as the only nationally accredited epilepsy center (NAEC Level III), in the state of Nevada.” Using a collaborative approach, specialists at the Renown Institute for Neurosciences use leading-edge diagnostic tools to identify neurological conditions and treat patients with the most effective techniques available. What is a Neuro-diagnostic Lab? A neuro-diagnostic lab allows care teams the technology to evaluate how a patient’s peripheral, autonomic, and central nervous systems function, and aid in diagnosing and treating conditions such as epilepsy, multiple sclerosis, Parkinson’s disease, stroke, and other diseases of the nervous system. What is an Electroencephalogram (EEG)? An Electroencephalogram (EEG) is a test that measures and records the electrical activity of the brain. During the test, special sensors called electrodes are attached to the patient’s head and hooked by wires to a computer. The computer then records the brain’s electrical activity on the screen. Using a collaborative approach, specialists at the Renown Institute for Neurosciences use leading-edge diagnostic tools to identify neurological conditions and treat patients with the most effective techniques available. Renown Health hospitals are ranked as Nevada’s top hospitals by U.S. News & World Report. About Renown Health Renown Health is the region’s largest, locally owned and governed, not-for-profit integrated healthcare network serving Nevada, Lake Tahoe and northeast California. With a diverse workforce of more than 7,000 employees, Renown has fostered a longstanding culture of excellence, determination and innovation. The organization comprises a trauma center, two acute care hospitals, a children’s hospital, a rehabilitation hospital, a medical group and urgent care network, and the region’s largest, locally owned not-for-profit insurance company, Hometown Health. Renown’s institute model addresses social determinants of health and includes: Child Health, Behavioral Health & Addiction, Healthy Aging and Health Innovation. Clinical institutes include: Cancer, Heart and Vascular Heath, Neurosciences and Robotic Surgery. Renown is currently enrolling participants in the world’s largest community-based genetic population health study, the Healthy Nevada Project®. About ABRET The American Board of Registration of Electroencephalographic and Evoked Potential Technologists (ABRET) is the credentialing board for EEG, Evoked Potential, Long Term Monitoring, and Neurophysiologic Intraoperative Monitoring Technologists. ABRET was organized in 1964 through a joint effort by the American Society of Electroencephalographic Technologists (ASET) and the American EEG Society (AEEGS) (now the American Clinical Neurophysiology Society). The Laboratory Accreditation Board was founded in 2004.
Read More About Renown Neuro-Diagnostic Laboratory Nationally Recognized
-
Leading Experts Convene in Tahoe To Focus On Scientific Advancements And The Prevention Of Cardiovascular Disease, The #1 Cause Of Death Globally
Three-day medical education conference advances research, education, prevention and treatment. Physicians and medical professionals from across the country will convene in Lake Tahoe from Friday, Nov. 4 to Sunday, Nov. 6 to explore the most recent advances and established guidelines for the diagnosis, treatment and prevention of cardiovascular disease, diabetes mellitus, stroke and diseases or problems associated with heart disease. Hosted by Renown's Institute for Heart & Vascular Health and the Nevada Academy of Family Physicians, the 32nd annual three-day Trends in Cardiovascular Medicine conference will bring together national experts to explore challenges and solutions to cardiovascular diseases, the leading cause of death globally, taking an estimated 17.9 million lives each year. "The driving force behind this collaborative event is the shared missions of all our organizations, across the country, to advance progress in cardiovascular research, education, prevention and treatment," says Jayson Morgan, MD, FACC, Director of Cardiovascular Services at Renown. "We will be joined by colleagues from across the country including Mayo Clinic College of Medicine and Science in Rochester, UC San Francisco School of Medicine, David Geffen School of Medicine at UCLA, University of Washington Medical Center, University of Chicago Medicine and locally- with experts from Renown's Institute for Heart & Vascular Health/UNR Med and Northern Surgical Associates - to discuss contemporary trends in providing excellent cardiovascular care and prevention." New research will be presented each day from experts across the country, including the following topics: “What the Fentanyl? Making Sense of a Deadly Epidemic” “COVID-19: Return to Sport or Strenuous Activity Following Infection” “Management of Type 2 Diabetes: Evolving Data, Evolving Guidelines, Evolving Practice” “Coronary Microvascular Disease in Women: Signs, Symptoms, Evaluation and Treatment” “Lipoprotein (a): A Risk Factor for Atherosclerosis and an Emerging Therapeutic Target” “Gut Feeling: The Increased Importance of GLP-1 Therapies for Personalized Obesity Management” "Primary Care Perspectives: Peripheral Vascular Disease” “Prevention of Atrial Fibrillation and Sudden Cardiac Death in Women” “Clinical Practice Guidelines for the Management of Heart Failure in 2022: What Do I as a Primary Care Provider Need to Know?” “Can a Patient be Low Risk without a Calcium Score?” “Obesity & Cardiovascular Disease Risk Reduction: How Does Bariatric Surgery Change the Landscape?” To make an appointment with a provider at Renown's Institute for Heart and Vascular Health, request that your primary care provider make a referral. For more information on Renown's Institute for Heart and Vascular Health, visit renown.org/Health-Services/Heart-Care. About Renown Health Renown Health is Nevada’s largest, locally governed, not-for-profit integrated healthcare network serving Nevada, Lake Tahoe and northeast California. With a diverse workforce of more than 7,000 employees, Renown has fostered a longstanding culture of excellence, determination and innovation. The organization comprises a trauma center, two acute care hospitals, a children’s hospital, a rehabilitation hospital, a medical group and urgent care network, and the locally owned not-for-profit insurance company, Hometown Health. Renown is currently enrolling participants in the world’s largest community-based genetic population health study, the Healthy Nevada Project®.
-
Palliative and Supportive Care
Compassionate Care Palliative and Supportive Care provides specialized medical care for serious illnesses and diseases, including advanced kidney failure or heart disease. Palliative Care helps to: Prevent and relieve suffering to help build the best possible quality of life. Add value to standard therapies by assisting with advanced illness planning and symptom management. Palliative & Supportive Care may be needed if: You've had multiple hospital admissions for severe illness. Severe pain, nausea, fatigue or other symptoms impacting quality of life and you are reconsidering treatment plans. Treatments are no longer working. You're feeling hapless or discouraged about the future due to your serious illness. Talk to your doctor to find out if palliative care is the right choice for you or your family member. Your Care Team Your palliative care support team comprises doctors, nurses, chaplains, social workers and other specialists who work together with you to provide extra support. Your care team can help: Facilitate close communication between you and your physician team, as well as nurses and specialists. Offer medical assessments and symptom management to help reduce pain, nausea, fatigue, shortness of breath and anxiety. Improve the ability to tolerate medical treatments and fain the strength to live a productive daily life. Explain treatment options and the decision making process regarding care. Navigate the healthcare process. Lend emotional and spiritual support.
-
Hospice Care
Our Team is Available 24/7 If you or a loved one is interested in Hospice Care, please call us at 775-982-2828. We accept self-referrals at any time, and a member of our team is available 24/7. Hospice Care from Renown Health When medical treatments no longer offer a cure, Hospice Care offers a special way to care for you and your family who are faced with a life-limiting illness. Serving Washoe, Lyon, Storey and Carson Counties, our team is available 24 hours a day, seven days a week. Hospice staff receive special training to care for all types of physical and emotional symptoms that cause pain, discomfort and distress. When considering your options for end-of-life transition, our team is available to answer questions and discuss if Renown Hospice Care will meet your needs. Your hospice care team includes Medical Director Registered Nurses Certified Nursing Aides Medical Social Workers Chaplains Registered Dietitians Trained Volunteers
-
Helpful Caregivers Make a Wedding Dream Come True
A wedding is a big day for the wedding couple, but it’s also special for loved ones. A patient at Renown, Ken, got to take part in his daughter’s special day as her wedding plans changed to accommodate his medical condition. Grab some tissues and read how Renown’s team of compassionate caregivers and chaplains planned a wedding in Fianna’s Healing Garden. Ken was hospitalized at Renown Regional Medical Center where he was battling a lung problem – which was unrelated to COVID-19 – and his condition worsened rapidly on Wednesday, Aug. 12. His family made the decision to transition him to palliative care, which helps patients near the end of their lives remain comfortable, while supporting their dignity and quality of life. Ken’s medical condition altered wedding plans for his daughter, Chandra, and her fiancé, Tyler, who were planning to tie the knot later in 2020. Chandra wanted her father there, but knew he could not leave the hospital. That’s why Chandra’s sister, Heather, approached Ken’s care team with a request to have a small wedding ceremony at the hospital. Planning the Wedding A member of Ken’s care team, Amy Heston, registered nurse (RN), began planning how the wedding could be held outdoors in Fianna's Healing Garden in the E. L. Wiegand Pavilion, which was donated by the E. L. Wiegand Foundation. In 24 hours, Amy planned a wedding ceremony with the help of her colleague, Breyanna Aufiero, RN; the Renown Spiritual Care team; and nursing leaders on the coronary intensive care unit (ICU). Together, they decorated the aisle in the garden with flowers and battery-operated candles. They also made a sign for Ken’s hospital bed, which read, “Father of the Bride,” and crafted a bow tie for him to wear for the special occasion. With visitor restrictions in place at the hospital due to coronavirus (COVID-19), having the wedding outside in the Healing Garden allowed for more members of Ken’s family to attend including his wife, Charlotte, and his dog, Bella. Every step in planning the wedding required thoughtful and thorough care coordination so Ken could participate. His breathing was supported by oxygen and special arrangements were made to transport the oxygen tanks he needed to take part in his daughter’s wedding. Amy worked with respiratory technician, Kasey Benfield, and critical care technician, Ruben Duckworth, to ensure Ken’s oxygen needs were met using portable machines. Celebrating Love and Life Together Ken’s team of caregivers bathed him and shaved his face so he could look and feel his best for the ceremony. They put on his bow tie, covered his bed in decorations and his favorite blue, flannel blanket, and wheeled his bed outside for the ceremony. Renown associate chaplains Terri Domitrovich and Susan Palwick coordinated music and performed the ceremony for Chandra and Tyler on Thursday, Aug. 13, 2020. The bride and groom shared their first dance in the garden and Ken’s care team provided water and treats to give the family a full wedding experience. Shortly after the ceremony, Ken passed away. This wedding provided Ken and his family meaningful memories for their big life-changing moments as they celebrated and said goodbye. “Seeing Ken surrounded by family he never would have gotten to see again while in the hospital, watching him get to share a father-daughter dance with Chandra on her wedding day, and having him tell me that this day meant more to them than we would ever know were some of the most moving moments I’ve witnessed as a nurse,” Amy said. “I am so thankful for the team we have here. I know that this beautiful day wouldn’t have happened without the help of every single person who gave their time, money, creativity and passion to make it a day to remember.”
Read More About Helpful Caregivers Make a Wedding Dream Come True
-
Alzheimer’s Disease – How to Spot the Signs
Alzheimer’s disease is not normal forgetfulness as we age. Instead, it is a specific form of mental decline. And according to the Alzheimer’s Association it accounts for nearly 80 percent all dementia cases. Natasa Dragicevic, MD, PhD., behavioral neurologist and Alzheimer’s disease specialist with Renown Institute for Neurosciences, weighs in on diagnosing it and the importance of early medical action. How to Diagnose Alzheimer’s Disease In general, the signs of Alzheimer’s disease occur slowly, getting worse over time. For example, forgetfulness is a daily search – for shoes, keys and other misplaced items. Not only is memory affected, but also speech patterns and behavior. There is no single test for Alzheimer’s disease. “Specifically, a neurologist should be the one to diagnose Alzheimer’s disease given differences in presentation,” clarifies Dr. Dragicevic. “And ideally a behavioral neurologist (Alzheimer’s sub-specialist) will be managing the treatment,” she adds. Brain Imaging Diagnosing Alzheimer’s disease involves multiple approaches and medical providers. In short, medical history is reviewed along with a physical exam, lab tests and other diagnostic testing. “A medical workup includes a variety of tests. These include MRI and other brain imaging, as well as neurological and psychological testing. Furthermore, a lumbar puncture is performed to look for markers of the disease,” she states. What Causes Alzheimer’s disease? Although no one knows the cause, researchers think many factors play a role. Uncontrollable risk factors include your genetics and having a family member with the disease. However, the controllable risk factors include: reducing the risk of head injury and keeping your heart healthy. It’s important to realize that high blood pressure, high cholesterol, stroke and diabetes play a role in brain health. Blood loss to the brain causes vascular dementia, leading to long-term blood vessel damage. Symptoms of Alzheimer’s disease Generally speaking, the signs of this disease differ in each person. Yet noticeable behaviors include: • Losing the way to familiar places • Forgetting to pay bills • Trouble finding the right words when talking • Repeating questions • General confusion • Social withdrawal Alzheimer’s Disease – Benefits of Early Diagnosis Equally important, spotting Alzheimer’s disease early allows more time to benefit from medications and possible clinical trials. Likewise, nutrition and exercise changes can be made, increasing blood flow to the body, and perhaps delaying symptoms. Early diagnosis also allows for personal health decisions and quality-of-life conversations to take place. According to the Alzheimer’s Association, these benefits include: 1. Medical advantage 2. Emotional and social comfort 3. Time to plan ahead 4. Cost savings A Brain Supporting Lifestyle “At the present time, treatment is limited,” explains Dr. Dragicevic. “Usually Alzheimer’s is a progressive ongoing disease – any management at this time is purely symptomatic.” However, she states the following lifestyle changes can help support brain health: • New hobbies such as painting, pottery, music classes or learning a new language • Crosswords, puzzles and playing games, such as Scrabble • Brain challenging mobile apps, such as Luminosity • 30-45 minutes of mild to moderate physical activity per day, such as walking • Eating a Mediterranean diet (primarily plant based foods)
-
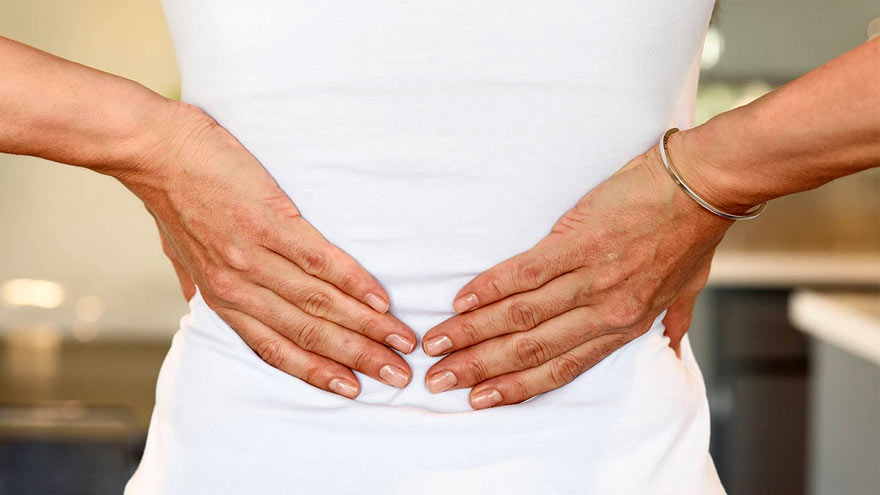
Low Back Pain – How to Stop the Ache
Low back pain is not only a problem most people have at some point in life, but also the leading cause of disability in the U.S. Whether it is a sharp spasm from lifting something heavy or a daily constant ache, there are various treatments available to relieve your pain. Jessica Ryder PT, DPT, cert VRS, with Renown Health Outpatient Therapy, explains some common causes of this pain, how to treat it and ways to prevent pain flare-ups. It’s important to realize most cases of low back pain are short term. Frequently lasting only a few days or weeks. In general these cases leave no long-term damage to the spine, muscles, discs or nerves. “However, it can become episodic or chronic (lasting longer than 12 weeks) if it is not properly understood or managed by the individual, ” cautions Ryder. Causes of Pain Specifically back discomfort can be related to: Wear and tear on the spine due to age or poor movement patterns Injury to spinal discs Sprains (overstretching or tearing of ligaments) and strains (tears in tendons or muscles) Trauma Irregularities of the spine present at birth (example: scoliosis)Notably the above issues may result in a “pinched nerve” or sciatica, causing pain to extend down the leg. Risk Factors for Pain In particular, your chance of developing low back pain increases with the risk factors below: Age Being overweight Low fitness level or occasional physical activity (“weekend warrior”) Family history Pregnancy Poor posture Jobs requiring heavy physical work (landscaping, plumbers, construction, etc.)
-
The Salty Six: Are High-Sodium Foods Increasing Your Stroke Risk?
Excess amounts of sodium doesn’t just increase your risk of a heart attack, it can also increase your risk of a stroke. Unfortunately, avoiding that saltshaker may not be enough. Did you know that the average American consumes 3,400 milligrams of sodium each day? That’s a dangerous number considering that the American Heart Association recommends limiting daily sodium intake to 1,500 milligrams (about half the weight of a penny) to reduce the risk of heart disease and stroke. The problem is not necessarily that you’re putting too much salt on your food, it’s that salt is already in the foods you’re regularly eating. To help keep your sodium intake at a healthy level, make sure you’re aware of “The Salty Six,” six sneaky foods that are surprisingly high in sodium. Breads, Rolls and Tortillas: Although breads and tortillas may not initially appear to be high in sodium, we often consume several servings. Make sure to keep track of your total servings to see how they add up. Deli Meat, Cured Meats and Poultry: It may surprise you that six thin slices of deli meat can add up to more than half of your daily limit, so be mindful when building those sandwiches. Also, do your best to avoid cured meats, which often means the meat has been salted. Substitute uncured, skinless meats instead. Cheese: Salt is an important addition in the cheese-making process, as it prevents bacterial growth. Unfortunately, that added salt can increase your health risks. Limit the amount of cheese you add to meals to keep your sodium content down. Pizza: Take a quick look at the first three items above and it should be no surprise as to why pizza made the list. One slice and you’ve met at least half of your daily limit. Go easy on the cheese and try adding more veggies instead of meat. Canned Soup: One cup of canned soup can be as high as nearly 1,000 milligrams of sodium. When shopping for canned soup it’s important to check the label – not just on sodium content but serving size as well. Always select low-sodium options when possible or cook your own soup at home. Sandwiches and Burgers: A sandwich or burger from your favorite restaurant can contain more than 100 percent of your daily sodium limit. When dining out, it is best to select low-sodium options or eat a half portion to limit the amount of salt. If some of your favorite foods are on this Salty Six list, don’t panic. Although these foods can be high in sodium, it isn’t necessary to cut these foods out of your diet completely. It’s just important to eat them in moderation and be mindful of your daily sodium intake. Look for low-sodium options, use herbs and spices instead of table salt and do your best to stay under the recommended daily limit of 1,500 milligrams.”
Read More About The Salty Six: Are High-Sodium Foods Increasing Your Stroke Risk?
-
Alzheimer's Safety Tips for Caregivers to Know
November is National Alzheimer’s Disease Awareness Month. At Renown Health, we know that Alzheimer's safety for your loved one is a priority, as the symptoms can sometimes lead to unsafe situations. We asked Dr. Jonathan Artz – a neurology physician with Renown Health and an assistant professor of clinical neurology at the University of Nevada, Reno School of Medicine – for tips on keeping loved ones safe and secure. According to the Alzheimer’s Association, Alzheimer’s disease affects safety in various ways, specifically due to body and brain adjustments. These changes can include: Judgment, including forgetfulness Sense of place – getting lost on the way home Behavior – being suspicious or fearful Body difficulty – losing balance Sensing ability – noticeable sensitivity in hearing, seeing or temperature Dr. Artz gives us four major tips to ensure your loved one’s safety as you both navigate this disease together. Watch for Wandering Those experiencing Alzheimer’s disease tend to wander and get lost. Try the following tips to reduce the risk of wandering: Get your loved one an ID bracelet and have them wear it at all times. You can also enroll your loved one in “Wandering Support.” Install door chimes so you know when exterior doors are open. Ask neighbors to call you if they see your loved one out alone. Go with your loved one when they insist on leaving the house. Don’t argue or yell. Instead, use distraction or gentle hints to get them to return home. Discourage Driving Driving can be unsafe for someone with this disease. With this in mind, ask a doctor whether it’s safe for your loved one to drive. For example, on a case-by-case basis, there are certain situations where doctors are required to report individuals with particular cognitive impairments, wherein a form of a driving assessment will be recommended. Limit access to the car. Keep the keys with you or lock them away. Ask an authority figure, such as an insurance agent or a doctor, to tell them not to drive. Adult-Proof Your Abode A simple living space is a safe living space. This means reducing clutter and removing any issues that may pose a safety concern. You may also want to get advice from an occupational therapist (home safety expert). Keep in mind that some changes may not be needed right away. Focus on major safety concerns first. Try the following tips: Add lighting (or glow-in-the-dark tape) to brighten dark areas, including stairways and halls. Use color contrast or texture indicators for dials, knobs and appliance controls. Remind your loved one not to carry items while walking to avoid a fall. Remove sharp objects from drawers and countertops. Avoid using small throw rugs or doormats, as they are easy to trip on. Move frequently used items so that they are easy to reach. Lock away alcohol and tobacco products, as they are not recommended for dementia patients. Install handrails in the shower, tub and near the toilet. Bathroom falls are especially common. Adjust the setting on your hot water heater so water does not scald. Those with Alzheimer’s can lose their sensitivity to temperature. Move and lock up hazardous chemicals and cleaning supplies, such as bleach and insecticides. Disable and remove guns or any weapons. Supervise any medication taken by your loved one. Promote a Positive & Healthy Lifestyle Continually emphasize the strengths of your loved one by promoting participation in meaningful activities, wellness visits and healthy habits to help them improve their well-being. Here are some ways to keep them physically and mentally active: Maintain regular vision and hearing screenings and make necessary adaptations. Establish a routine for daily activities. Encourage participation in self-care and leisure activities. Work with your loved one’s doctor to establish a healthy diet. Ensure proper hydration. It may help to set reminders for your loved one to drink fluids. Encourage regular exercise. Exercise delivers oxygen to the brain, improving brain health. Promote good sleep habits. Good quality sleep can increase overall brain health and has been associated with improving memory, attention and concentration. Resources and support are available with the Renown Memory Disorders Program. Providers within this program are specifically dedicated to treating several different memory-related disorders. Memory Disorders Resources & Support.
Read More About Alzheimer's Safety Tips for Caregivers to Know